Abstract
Background
The use of absorbable sutures in wound closure has been shown to reduce the incidence of surgical site infection (SSI); however, there is no evidence that the intra-abdominal use of absorbable rather than silk sutures reduces the incidence of SSI after gastrointestinal surgery. We report the findings of a phase II trial, designed to evaluate the impact of the intra-abdominal use of absorbable sutures on the incidence of SSI.
Methods
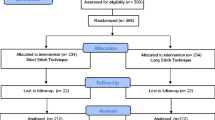
At 19 Japanese hospitals, 1147 patients undergoing elective gastrectomy, colorectal surgery, hepatectomy, or pancreaticoduodenectomy (PD) were randomly assigned to absorbable or silk intra-abdominal suture groups. The primary efficacy endpoint was the incidence of SSI. The secondary efficacy endpoints were the locations of SSI, time to resolution of SSI, length of hospital stay, and the incidence of bile leakage in hepatectomy and pancreatic fistula.
Results
The incidence of SSI was 11.3%, 15.5%, 11.3%, and 36.9% after gastrectomy, colorectal surgery, hepatectomy, and PD, respectively. The incidence of SSI was higher in the absorbable suture group than in the silk suture group for all the surgical procedures, but the difference was not significant.
Conclusion
The intra-abdominal use of absorbable sutures did not have enough of an effect on the reduction of SSI in this phase II trial to justify the planning of a large-scale phase III trial.




Similar content being viewed by others
Change history
27 September 2017
In the original publication, the article category was published as “Review Article”. The correct category should read as “Original Article”.
References
Katayama H, Kurokawa Y, Nakamura K, Ito H, Kanemitsu Y, Masuda N, et al. Extended Clavien-Dindo classification of surgical complications: Japan Clinical Oncology Group postoperative complications criteria. Surg Today. 2016;46:668–85.
Smith RL, Bohl JK, McElearney ST, Friel CM, Barclay MM, Sawyer RG, et al. Wound infection after elective colorectal resection. Ann Surg. 2004;239:599–607.
Sørensen LT, Hemmingsen U, Kallehave F, Wille-Jørgensen P, Kjaergaard J, Møller LN, et al. Risk factors for tissue and wound complications in gastrointestinal surgery. Ann Surg. 2005;241:654–8.
Emori TG, Culver RDH, Horan TC, Jarvis WR, White JW, Olson DR, et al. National nosocomial infection surveillance system (NNISS) description of surveillance methods. Am J Infect Control. 1991;19:19–35.
Cruse PJ, Foord R. The epidemiology of wound infection: A 10-year prospective study of 62,939 wounds. Surg Clin North Am. 1980;60:27–40.
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR. Guideline for prevention of surgical site infection, 1999. Infect Control Hosp Epidemiol. 1999;20:247–78.
Culver DH, Horan TC, Gaynes RP, Martone WJ, Jarvis WR, Emori TG, et al. Surgical wound infection rates by wound class, operative procedure, and patient risk index. National Nosocominal Infections Surveillance System. Am J Med. 1991;91:1525–7S.
Gayne RP, Culver DH, Horan TC, Edwards JR, Richards C, Tolson JS. Surgical site infection (SSI) rates in the United States, 1992–1998: the National Nosocomial Infections Surveillance System basic SSI risk index. Clin Infect Dis. 2001;33(Suppl 2):S69–77.
Roy MC, Herwaldt LA, Embrey R, Kuhns K, Wenzel RP, Perl TM. Does the center for disease control’s NNIS system risk index stratify patients undergoing cardiothoracic operations by their risk of surgical-site infection? Infect Control Hosp Epidermiol. 2000;21:1865–90.
Melton GB, Vogel JD, Swenson BR, Remzi FH, Rothenberger DA, Wick EC. Continuous intraoperative temperature measurement and surgical site infection risk: analysis of anesthesia information system data in 1008 colorectal procedures. Ann Surg. 2013;258:606–12.
Sørensen LT, Karlsmark T, Gottrup F. Abstinence from smoking reduces incisional wound infection: a randomized controlled trial. Ann Surg. 2003;238:1–5.
Lizan-Garcia M, Garcia-Caballero J, Assensio Vegas A. Risk factors for surgical-wound infection in general surgery:a prospective study. Infect Control Hosp Epidemiol. 1997;18:310–5.
Zerr KJ, Furnary AP, Grunkenmeier GL, Bookin S, Kanhere V, Starr A. Glucose control lowers the risk of wound infection in diabetics after open heart operation. Ann Thro Surg. 1997;63(2):356–61.
Greif R, Akca O, Horn EP, Kurz A, Sessler DI. Supplemental perioperative oxygen to reduce the incidence of surgical-wound infection. N Engl J Med. 2000;342:161–7.
Merritt K, Hitchins VM, Neale AR. Tissue colonization from implantable biomaterials with low numbers of bacteria. J Biomed Mater Res. 1999;44:261–5.
Otten J-E, Wiedmann-Al-Ahmad M, Jahnke H, Pelz K. Bacterial colonization on different suture materials-a potential risk for introral dentoalveolar surgery. J Biomed Mater Res B Appl Biomater. 2005;74:627–35.
Kronborg O. Polyglycolic acid (DEXON) versus silk for fascial closure of abdominal incisions. Acta Chir Scand. 1976;142:9–12.
Blomstedt GC. Infection in Neurosurgery: A randomized comparison between silk and Plyglycolic acid. Acta Neurochir. 1985;76:90–3.
Iwase K, Higaki J, Tanaka Y, Kondoh, M, Yoshikawa M, Kamiike W. Running closure of clean and contaminated abdominal wounds using a synthetic monofilament absorbable looped suture. Surg Today. 1999;29:874–9.
Sortino F, Lombardo C, Sciacca A. Silk and polyglycolic acid in oral surgery: a comparative study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;105:e15–8.
Adams IW, Bell MS, Driver RM, Fry WG. A comparative trail of polyglycolic acid and silk suture materials for accidental wounds. Lancet. 1977;2(8050):1216–7.
Willatt DJ, Durham L, Ramadan MF, Bark-Jones N. A prospective randomized trial of suture material in aural wound closure. J Laryngol Otol. 1988;102:788–90.
Hodgson NC, Malthaner RA, Østbye T. The search for an ideal method of abdominal fascial closure, a meta-analysis. Ann Surg. 2000;231:436–42.
van’t Riet M, Steyerberg EW, Nellensteyn J, Bonjer HJ, Jeekel J. Meta-analysis of techniques for closure of midline abdominal incisions. Br J Surg. 2002;89:1350–6.
Watanabe A, Kohnoe S, Shimabukuro R, Yamanaka T, Iso Y, Baba H, et al. Risk factors associated with surgical site infection in upper and lower gastro- intestinal surgery. Surg Today. 2008;38:404–12.
Okabayashi T, Nishimori I, Yamashita K, Sugimoto T, Yatabe T, Maeda H, et al. Risk factors and predictors for surgical site infection after hepatectomy. J Hosp Infect. 2009;73:47–53.
Togo S, Matsuo K, Tanaka K, Matsumoto C, Shimizu T, Ueda M, et al. Perioperative infection control and its effectiveness in hepatectomy patients. J Gastroenterol Hepatol. 2007;22:1942–8.
Ueno T, Yamamoto K, Kawaoka T, Takashima M, Oka M. Current antibiotics prophylaxis in pancreatoduodenectomy in Japan. J Hepatobiliary Pancreat Surg. 2005;12:304–9.
Yamashita Y, Hamatsu T, Rikimaru T, Tanaka S, Shirabe K, Shimada M, et al. Bile leakage after hepatic resection. Ann Surg. 2001;233:45–50.
Bassi C, Butturini G, Molinari E, Mascetta G, Salvia R, Falconi M, et al. Pancreatic fistula after pancreatic resection. The importance of definitions. Dig Surg. 2004;21:54–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by a grant from the Japan Surgical Society Clinical Investigation Project Award and a Health Labour Science Research Grant (Rinsho-Ippan-006).
Conflict of interest
We declare that we have no conflicts of interest.
Additional information
An erratum to this article is available at https://doi.org/10.1007/s00595-017-1589-4.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Maehara, Y., Shirabe, K., Kohnoe, S. et al. Impact of intra-abdominal absorbable sutures on surgical site infection in gastrointestinal and hepato-biliary-pancreatic surgery: results of a multicenter, randomized, prospective, phase II clinical trial. Surg Today 47, 1060–1071 (2017). https://doi.org/10.1007/s00595-017-1480-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-017-1480-3