Abstract
Purpose
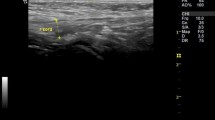
Laparoscopic percutaneous extraperitoneal closure (LPEC) is known to reduce the incidence of metachronous contralateral hernia (MCH) compared to conventional hernia repair. We herein describe the effects of insistent screening for an irregular orifice of the contralateral patent processus vaginalis (CPPV).
Methods
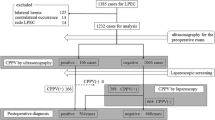
All patients who underwent LPEC between 2003 and 2013 were reviewed. We started insistent screening for a CPPV in July 2010. The surgically treated cases before June 2010 were assigned to the former group, while those treated after July 2010 were in the latter group. The data were retrospectively collected from medical records. The statistical analysis was performed using the Mann–Whitney U test or Chi square test. A value of P < 0.05 was considered to be significant.
Result
A total of 1113 patients (514 males and 599 females) ranging in age from 3 months old to 15 years old (median 4.6 years old), were reviewed. Of the 626 patients in the former group, a CPPV was detected in 227 patients. Of the 487 patients in the latter group, a CPPV was detected in 271 patients. The incidence of a CPPV significantly increased over time (P < 0.001). We encountered five cases of MCH, all of which belonged to the former group (P = 0.048).
Conclusions
The increased detection of a CPPV by insistent screening seemed to cause a decrease in the incidence of MCH.


Similar content being viewed by others
References
Takehara H, Yakabe S, Kameoka K. Laparoscopic percutaneous extraperitoneal closure for inguinal hernia in children: clinical outcome of 972 repairs done in 3 pediatric surgical institutions. J Pediatr Surg. 2006;41(12):1999–2003.
Hayashi Y, Miyata K, Yuasa N, Takeuchi E, Goto Y, Miyake H, et al. Short- and long-term outcomes of open inguinal hernia repair: comparison of the Prolene Hernia System and the Mesh Plug method. Surg Today. 2014;44(12):2255–62.
Okus A. Is Tachosil mesh better than polypropylene mesh for inguinal hernia repair? Surg Today. 2014;44(6):1188.
Tam YH, Wong YS, Pang KK, Tsui SY, Mou JW, Houben CH, et al. Unexpected metachronous hernia development in children following laparoscopic unilateral hernia repair with negative evaluation for contralateral patent processus vaginalis. J Laparoendosc Adv Surg Tech A. 2013;23(3):287–90.
Watanabe T, Nakano M, Endo M. An investigation on the mechanism of contralateral manifestations after unilateral herniorrhaphy in children based on laparoscopic evaluation. J Pediatr Surg. 2008;43(8):1543–7.
Sparkman RS. Bilateral exploration in inguinal hernia in juvenile patients. Review and appraisal. Surgery. 1962;51:393–406.
Kiesewetter WB, Oh KS. Unilateral inguinal hernias in children: what about the opposite side? Arch Surg. 1980;115(12):1443–5.
Timberlake GA, Ochsner MG, Powell RW. Diagnostic pneumoperitoneum in the pediatric patient with a unilateral inguinal hernia. Arch Surg. 1989;124(6):721–3.
Kokorowski PJ, Wang HH, Routh JC, Hubert KC, Nelson CP. Evaluation of the contralateral inguinal ring in clinically unilateral inguinal hernia: a systematic review and meta-analysis. Hernia. 2014;18(3):311–24.
Zhong H, Wang F. Contralateral metachronous hernia following negative laparoscopic evaluation for contralateral patent processus vaginalis: a meta-analysis. J Laparoendosc Adv Surg Tech A. 2014;24(2):111–6.
Hall NJ, Choi W, Pierro A, Eaton S. Age-related probability of contralateral processus vaginalis patency in children with unilateral inguinal hernia. Pediatr Surg Int. 2012;28(11):1085–8.
Maddox MM, Smith DP. A long-term prospective analysis of pediatric unilateral inguinal hernias: should laparoscopy or anything else influence the management of the contralateral side? J Pediatr Urol. 2008;4(2):141–5.
Ron O, Eaton S, Pierro A. Systematic review of the risk of developing a metachronous contralateral inguinal hernia in children. Br J Surg. 2007;94(7):804–11.
Niyogi A, Tahim AS, Sherwood WJ, De Caluwe D, Madden NP, Abel RM, et al. A comparative study examining open inguinal herniotomy with and without hernioscopy to laparoscopic inguinal hernia repair in a pediatric population. Pediatr Surg Int. 2010;26(4):387–92.
Saka R, Okuyama H, Sasaki T, Nose S, Yoneyama C. Safety and efficacy of laparoscopic percutaneous extraperitoneal closure for inguinal hernias and hydroceles in children: a comparison with traditional open repair. J Laparoendosc Adv Surg Tech A. 2014;24(1):55–8.
Yoshizawa J, Ashizuka S, Kuwashima N, Kurobe M, Tanaka K, Ohashi S, et al. Laparoscopic percutaneous extraperitoneal closure for inguinal hernia: learning curve for attending surgeons and residents. Pediatr Surg Int. 2013;29(12):1281–5.
Zamakhshardy M, Ein A, Ein SH, Wales PW. Predictors of metachronous inguinal hernias in children. Pediatr Surg Int. 2009;25(1):69–71.
Conflict of interest
The authors have no conflicts of interest to declare in association with this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sumida, W., Watanabe, Y., Takasu, H. et al. Effects of insistent screening for contralateral patent processus vaginalis in laparoscopic percutaneous extraperitoneal closure to prevent metachronous contralateral onset of pediatric inguinal hernia. Surg Today 46, 569–574 (2016). https://doi.org/10.1007/s00595-015-1199-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-015-1199-y