Abstract
Purpose
Tension-free mesh repair of adult inguinal hernias has become a standard procedure, but there have been few comparisons of the postoperative outcome after hernia repair using the Prolene Hernia System (PHS) vs. the Mesh Plug (MP) method in a large number of patients from a single institution.
Methods
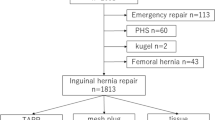
We reviewed the medical records of patients to investigate the short- and long-term outcomes of the different types of hernia repair. Late symptoms were evaluated by questionnaire. A total of 1,141 repairs performed from 1999 to 2008 (PHS in 957 and MP in 184 repairs) were evaluated.
Results
There were 93 early postoperative complications (8.2 %). A subcutaneous hematoma was found more frequently after MP repair compared with after PHS repair (3.8 vs. 1.3 %, P = 0.013). Seven hundred and ten patients (62.2 %) could be followed up for more than 2 years. Recurrence was detected in 14 patients with PHS repair and two patients with MP repair (1.5 vs. 1.1 %, P = 0.956). Wound infections occurred in three patients (0.3 %) with PHS repair vs. none with MP repair (P > 0.999). Patients with PHS and MP repair showed no significant differences in the long-term wound pain.
Conclusions
The recurrence and wound infection rates were similar after hernia repair using the PHS and MP methods. Patients undergoing PHS repair developed fewer subcutaneous hematomas. An older age (≥65 years) was a significant independent risk factor for recurrence.


Similar content being viewed by others
References
Lichtenstein IL, Shuluman AG. Ambulatory outpatient hernia surgery: including a new concept, introducing tension-free repair. Int Surg. 1986;71:1–4.
Kingsnorth AN, Wright D, Porter CS, Robertson G. Prolene Hernia System compared with Lichtenstein patch: a randomized double blind study of short-term and medium-term outcomes in primary inguinal hernia repair. Hernia. 2002;6:113–9.
Dalenback J, Andersson C, Anesten B, Björck S, Eklund S, Magnusson O, et al. Prolene Hernia System, Lichtenstein mesh and plug-mesh-patch for primary inguinal hernia repair: 3-year outcome of a prospective randomized controlled trial. Hernia. 2009;13:121–9.
Faraj D, Ruurda JP, Olsman JG, van Geffen HJ. Five-year results of inguinal hernia treatment with the Prolene Hernia System in a regional training hospital. Hernia. 2010;14:155–8.
Gilbert AI, Graham MF. Symposium on the management of inguinal hernia 5. Sutureless technique: second version. Can J Surg. 1997;40:209–12.
Kugel RD. Minimally invasive, nonlaparoscopic, preperitoneal, and sutureless inguinal herniorrhaphy. Am J Surg. 1999;178:298–302.
Gilbert AI, Graham MF, Voigt WJ. A bilayer patch device for inguinal hernia repair. Hernia. 1993;3:161–6.
Hasegawa S, Yoshikawa T, Yamamoto Y, Ishiwa N, Morinaga S, Noguchi Y, et al. Long-term outcome after hernia repair with the Prolene Hernia System. Surg Today. 2006;36:1058–62.
Mesci A, Korkmaz B, Dinckan A, Colak T, Balci N, Ogunc G. Digital evaluation of the muscle functions of the lower extremities among inguinal hernia patients treated using there different surgical techniques: a prospective randomized study. Surg Today. 2012;42:157–63.
Huang CS, Huang CC, Lien HH. Prolene Hernia System compared with mesh plug technique: a prospective study of short- to mid-term outcomes in primary groin hernia repair. Hernia. 2005;9:167–71.
Zhao G, Gao P, Ma B, Tian J, Yang K. Open mesh techniques for inguinal hernia repair: a meta-analysis of randomized controlled trials. Ann Surg. 2009;250:35–42.
Mayagoitia JC. Inguinal hernioplasty with the Prolene Hernia System. Hernia. 2004;8:64–6.
Gilbert AI, Young J, Graham MF, Divilio LT, Patel B. Combined anterior and posterior inguinal hernia repair: intermediate recurrence rates with three groups of surgeons. Hernia. 2004;8:203–7.
Mayagoitia JC, Prieto-Diaz Chavez E, Suarez D, Cisneros HA, Tene CE. Predictive factors comparison of complications and recurrences in three tension-free herniorrhaphy techniques. Hernia. 2006;10:147–51.
Berende CA, Ruurda JP, Hazenberg CE, Olsman JG, van Geffen HJ. Inguinal hernia treatment with the Prolene Hernia System in a Dutch regional training hospital. Hernia. 2007;11:303–6.
Awad SS, Yallampalli S, Srour AM, Bellows CF, Albo D, Berger DH. Improved outcomes with the Prolene Hernia System mesh compared with the time-honored Lichtenstein onlay mesh repair for inguinal hernia repair. Am J Surg. 2007;193:697–701.
Just E, Botet X, Martinez S, Escolà D, Moreno I, Duque E. Reduction of the complication rate in Lichtenstein hernia repair. Int J Surg. 2010;8:462–5.
Rosemar A, Angerås U, Rosengren A, Nordin P. Effect of body mass index on groin hernia surgery. Ann Surg. 2010;252:397–401.
Jansen PL, Klinge U, Jansen M, Junge K. Risk factors for early recurrence after inguinal hernia repair. BMC Surg. 2009;9:18.
Kald A, Nilsson E, Anderberg B, Bragmark M, Engström P, Gunnarsson U, et al. Reoperation as surrogate endpoint in hernia surgery. A three year follow-up of 1565 herniorrhaphies. Eur J Surg. 1998;164:45–50.
Kehlet H, Bay-Nielsen M. Local anesthesia as a risk factor for recurrence after groin hernia repair. Hernia. 2008;12:507–9.
Sorensen LT, Friis E, Jorgensen T, Vennits B, Andersen BR, Rasmussen GI, et al. Smoking is a risk factor for recurrence of groin hernia. World J Surg. 2002;26:397–400.
Junge K, Rosch R, Klinge U, Schwab R, Peiper Ch, Binnebösel M, et al. Risk factors related to recurrence in inguinal hernia repair: a retrospective analysis. Hernia. 2006;10:309–15.
Arvidsson D, Berndsen FH, Larsson LG, Leijonmarck CE, Rimbäck G, Rudberg C, et al. Randomized clinical trial comparing 5-year recurrence rate after laparoscopic versus Shouldice repair of primary inguinal hernia. Br J Surg. 2005;92:1085–91.
Esposito S, Leone S, Noviello S, Ianniello F, Marvaso A, Cuniato V, et al. Antibiotic prophylaxis in hernia repair and breast surgery: a prospective randomized study comparing piperacillin/tazobactam versus placebo. J Chemother. 2006;18:278–84.
Pessaux P, Lermite E, Blezel E, Msika S, Hay JM, Flamant Y, et al. Predictive risk score for infection after inguinal hernia repair. Am J Surg. 2006;192:165–71.
Praveen S, Rohaizak M. Local antibiotics are equivalent to intravenous antibiotics in the prevention of superficial wound infection in inguinal hernioplasty. Asian J Surg. 2009;32:59–63.
van der Linden W, Warg A, Nordin P. National register study of operating time and outcome in hernia repair. Arch Surg. 2011;146:1198–203.
Taylor EW, Duffy K, Lee K, Hill R, Noone A, Macintyre I, et al. Surgical site infection after groin hernia repair. Br J Surg. 2004;91:105–11.
Bay-Nielsen M, Perkins FM, Kehlet H, Danish Hernia Database. Pain and functional impairment 1 year after inguinal herniorrhaphy: a nationwide questionnaire study. Ann Surg. 2001;233:1–7.
Chen J, Li N, Ma SZ, Song JK. Randomized clinical trial of mesh plug versus Prolene Hernia System for inguinal hernia repair. Chin J Gen Surg. 2003;18:543–5.
Nienhuijs SW, van Oort I, Keemers-Gels ME, Strobbe LJ, Rosman C. Randomized trial comparing the Prolene Hernia System, mesh plug repair and Lichtenstein method for open inguinal hernia repair. Br J Surg. 2005;92:33–8.
Conflict of interest
The authors have no conflicts of interest with regard to the contents of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hayashi, Y., Miyata, K., Yuasa, N. et al. Short- and long-term outcomes of open inguinal hernia repair: comparison of the Prolene Hernia System and the Mesh Plug method. Surg Today 44, 2255–2262 (2014). https://doi.org/10.1007/s00595-014-0867-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-014-0867-7