Abstract
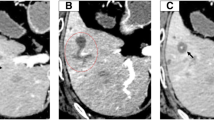
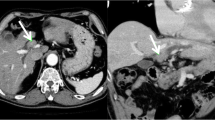
Morphologically, liver metastases from colorectal carcinoma usually form as nodular tumor masses, whereas intraductal papillary growth in the bile duct is rare. A 65-year-old man underwent right hemicolectomy for advanced colon carcinoma, and histology of the primary carcinoma confirmed moderately differentiated adenocarcinoma with subserosal invasion, no vascular infiltration, and no lymph node metastasis. A liver tumor was found in the right paramedian Glisson pedicle and intraductal growth of cholangiocarcinoma was seen on imaging. We performed right hepatectomy and macroscopically, the resected specimen contained a growth in the bile duct lumen similar to cholangiocarcinoma. Histological examination revealed intraductal papillary proliferation of well-differentiated adenocarcinoma without vascular infiltration or lymph node metastasis in the hepatic hilum. Immunohistochemical staining revealed that the tumor cells were negative for cytokeratin-7 and positive for cytokeratin-20. Based on these findings, liver metastasis from colon carcinoma was diagnosed. Liver metastasis from colorectal carcinoma rarely arises as intraductal papillary growth in the bile duct, but the possibility of liver metastases with unusual morphology must be borne in mind for patients with a history of carcinoma in the digestive tract.
Similar content being viewed by others
References
Sharma S, Camci C, Jabbour N. Management of hepatic metastasis from colorectal cancers: an update. J Hepatobiliary Pancreat Surg 2008;15:570–580.
Yasui K, Hirai T, Kato T, Torii A, Uesaka K, Morimoto T, et al. A new macroscopic classification predicts prognosis for patient with liver metastases from colorectal cancer. Ann Surg 1997;226:582–586.
Riopel MA, Klimstra DS, Godellas CV, Blumgart LH, Westra WH. Intrabiliary growth of metastatic colonic adenocarcinoma. A pattern of intrahepatic spread easily confused with primary neoplasia of the biliary tract. Am J Surg Pathol 1997;21:1030–1036.
Okano K, Yamamoto J, Moriya Y, Akasu T, Kosuge T, Sakamoto M, et al. Macroscopic intrabiliary growth of liver metastases from colorectal cancer. Surgery 1999;126:829–834.
Sugiura T, Nagino M, Oda K, Ebata T, Nishio H, Arai T, et al. Hepatectomy for colorectal liver metastases with macroscopic intrabiliary tumor growth. World J Surg 2006;30:1902–1908.
Kayashima H, Taketomi A, Yamashita Y, Kuroda Y, Kitagawa D, Harimoto N, et al. Liver metastasis with intraductal invasion originating from rectal cancer: Report of a case. Surg Today 2008;38:765–768.
Takamatsu S, Teramoto K, Kawamura T, Kudo A, Noguchi N, Irie T, et al. Liver metastasis from rectal cancer with prominent intrabile duct growth. Pathology Int 2004;54:440–445.
Tokai H, Kawashita Y, Eguchi S, Kamohara Y, Takatsuki M, Okudaira S, et al. A case of mucin producing liver metastases with intrabiliary extension. World J Gastroenterol 2006;12:4918–4921.
Uehara K, Hasegawa H, Ogise S, Sakamoto E, Igami T, Ohira S, et al. Intrabiliary polypoid growth of liver metastasis from colonic adenocarcinoma with minimal invasion of the liver parenchyma. J Gastroenterol 2004;39:72–75.
Rullier A, Bail BL, Famaz R, Blanc JF, Saric J, Bioulac-Sage P. Cytokeratin 7 and 20 expression in cholangiocarcinomas varies along the biliary tract but still differs from that in colorectal carcinoma metastasis. Am J Surg Pathol 2000;24:870–876.
Chen TC, Nakanuma Y, Zen Y, Chen MF, Jan YY, Yeh TS, et al. Intraductal papillary neoplasia of the liver associated with hepatolithiasis. Hepatology 2001;34:651–658.
Nakanuma Y, Sasaki M, Ishikawa A, Tsui W, Chen TC, Huang SF. Biliary papillary neoplasm of the liver. Histol Histopathol 2002;17:851–861.
Nanashima A, Sumida Y, Tamaru N, Nakanuma Y, Abo T, Tanaka K, et al. Intraductal papillary neoplasm of the bile duct extending superficially from the intrahepatic to extrahepatic bile duct. J Gastroenterol 2006;41:495–499.
Nanashima A, Kinoshita N, Nakanuma Y, Zen Y, Sumida Y, Abo T, et al. Clinicopathological features of “intraductal papillary neoplasm of the bile duct” and patient outcome after surgical resection. Hepatogastroenterology 2008;55:1167–1173
Okano K, Yamamoto J, Okabayashi T, Sugawara Y, Shimada K, Kosuge T, et al. CT imaging of intrabiliary growth of colorectal liver metastases: a comparison of pathological findings of resected specimens. Br J Radiol 2002;75:497–501.
Itatsu K, Fujii T, Sasaki M, Zen Y, Nakanuma Y. Intraductal papillary cholangiocarcinoma and atypical biliary epithelial lesions confused with intrabiliary extension of metastatic colorectal carcinoma. Hepatogastroenterology 2007;54:677–680.
Hiramatsu K, Sano T, Nagino M, Nimura Y. Repeat hepatectomy for colonic liver metastasis presenting intrabiliary growth — application of percutaneous transhepatic portal vein embolization for impaired liver. Hepatogastroenterology 2007;54:1554–1556.
Fong Y. Surgical therapy of hepatic colorectal metastasis. CA Cancer J Clin 1999;49:231–255.
Ambiru S, Miyazaki M, Ito H, Nakagawa K, Shimizu H, Kato A, et al. Resection of hepatic and pulmonary metastases in patients with colorectal carcinoma. Cancer 1998;82:274–278.
Hotokezaka M, Jimi S, Hidaka H, Ikeda T, Uchiyama S, Nakashima S, et al. Factors influencing outcome after surgery for stage IV colorectal cancer. Surg Today 2008;38:784–789.
Seyama Y, Makuuchi M. Current surgical treatment for bile duct cancer. World J Gastroenterol 2007;13:1505–1515.
Sasaki A, Aramaki M, Kawano K, Yasuda K, Inomata M, Kitano S. Prognostic significance of intrahepatic lymphatic invasion in patients with hepatic resection due to metastases from colorectal carcinoma. Cancer 2002;95:105–111.
Hotta T, Takifuji K, Arii K, Yokoyama S, Matsuda K, Higashiguchi T, et al. Potential predictors of long-term survival after surgery for patients with stage IV colorectal cancer. Anticancer Res 2006;26:1377–1383.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Nanashima, A., Tobinaga, S., Araki, M. et al. Intraductal papillary growth of liver metastasis originating from colon carcinoma in the bile duct: Report of a case. Surg Today 41, 276–280 (2011). https://doi.org/10.1007/s00595-009-4235-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-009-4235-y