Abstract
Aims
Although Catholic priests have a life of discipline with many responsibilities, there has been little research on the health effects of their lifestyle. Analysis of disease prevalence in priests will help elucidate the influence of religious life and occupational characteristics on the occurrence of diabetes. This retrospective study was performed to examine the differences in the prevalence of diabetes and prediabetes between Catholic priests and the general population.
Methods
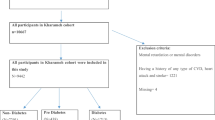
The study population comprised 1845 Catholic priests aged 31–80 years who visited the health promotion centers of three university hospitals in Korea between 2010 and 2019. Controls consisted of 1801 adult non-clerics aged 31–80 years who underwent health checkups at the screening center during the same period. Logistic regression analysis was performed to compare the differences in the rates of diabetes and prediabetes between the priest and control groups.
Result
Priests were younger and had lower rates of smoking, drinking alcohol, and hypertension compared with the control group. However, metabolic markers, such as BMI, waist circumference, body fat mass, insulin, HbA1c, and lipid profiles, were significantly higher in the priest group than the control group (all p < 0.05). After adjusting for covariates, the priest group had a significantly higher likelihood of having diabetes (OR = 1.651, 95% CI 1.146–2.379) or prediabetes (OR = 3.270, 95% CI 2.471–4.327) compared with the controls.
Conclusions
This study showed that Catholic priests have higher risks of diabetes and prediabetes compared with the general population, and these risks increase with age. Further large-scale prospective studies are required to confirm these relationships.

Similar content being viewed by others
Data availability and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Zimmer Z, Jagger C, Chiu C-T, Ofstedal MB, Rojo F, Saito Y (2016) Spirituality, religiosity, aging and health in global perspective: a review. SSM-Popul Health 2:373–381
Shattuck EC, Muehlenbein MP (2020) Religiosity/spirituality and physiological markers of health. J Relig Health 59(2):1035–1054
Flannelly KJ, Weaver AJ, Larson DB, Koenig HG (2002) A review of mortality research on clergy and other religious professionals. J Relig Health 41(1):57–68
WHO Diabetes
Association AD (2018) Economic costs of diabetes in the US in 2017. Diabetes Care 41(5):917–928
Bae JH, Han K-D, Ko S-H et al (2022) Diabetes fact sheet in Korea 2021. Diabetes Metab J 46(3):417
Agardh E, Allebeck P, Hallqvist J, Moradi T, Sidorchuk A (2011) Type 2 diabetes incidence and socio-economic position: a systematic review and meta-analysis. Int J Epidemiol 40(3):804–818
Rayburn CA, Richmond LJ, Rogers L (1988) Female rabbis, ministers and priests and the religion and stress questionnaire. NA
Koller M, Blanchfield K, Vavra T, Andrusyk J, Altier M (2012) Assessing and meeting the health needs of Roman Catholic priests in the archdiocese of Chicago. J Prev Interv Community 40(3):219–232
Proeschold-Bell RJ, LeGrand SH (2010) High rates of obesity and chronic disease among United Methodist clergy. Obesity 18(9):1867–1870
Halaas GW (2002) Ministerial Health and Wellness: 2002 Evangelical Lutheran Church in America. Evangelical Lutheran Church in America
Kaplan SD (1988) Retrospective cohort mortality study of Roman Catholic priests. Prev Med 17(3):335–343
Roncero-Ramos I, Alcala-Diaz JF, Rangel-Zuñiga OA et al (2020) Prediabetes diagnosis criteria, type 2 diabetes risk and dietary modulation: The CORDIOPREV study. Clin Nutr 39(2):492–500
Bonora E, Formentini G, Calcaterra F et al (2002) HOMA-estimated insulin resistance is an independent predictor of cardiovascular disease in type 2 diabetic subjects: prospective data from the Verona Diabetes Complications Study. Diabetes Care 25(7):1135–1141
Grundy SM, Cleeman JI, Daniels SR et al (2005) Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute scientific statement. Circulation 112(17):2735–2752
Shockey TM, Tsai RJ, Cho P (2021) Prevalence of Diagnosed Diabetes Among Employed US Adults by Demographic Characteristics and Occupation, 36 States, 2014 to 2018. J Occup Environ Med 63(4):302–310
Kuramasuwan B, Howteerakul N, Suwannapong N, Rawdaree P (2013) Diabetes, impaired fasting glucose, daily life activities, food and beverage consumption among Buddhist monks in Chanthaburi Province. Thailand Int J Diabetes Dev Ctries 33(1):23–28
Sridhar G (2013) Diabetes, religion and spirituality. Springer
Chiarlitti NA, Kolen AM (2020) Exploring supports and barriers to physical activity in catholic priests. J Prim Prev 41(4):317–329
Bopp M, Baruth M, Peterson JA, Webb BL (2013) Leading their flocks to health? Clergy health and the role of clergy in faith-based health promotion interventions. Fam Community Health 36(3):182–192
Feinstein M, Liu K, Ning H, Fitchett G, Lloyd-Jones DM (2012) Incident obesity and cardiovascular risk factors between young adulthood and middle age by religious involvement: the Coronary Artery Risk Development in Young Adults (CARDIA) study. Prev Med 54(2):117–121
Newlin K, Melkus GD, Tappen R, Chyun D, Koenig HG (2008) Relationships of religion and spirituality to glycemic control in Black women with type 2 diabetes. Nurs Res 57(5):331–339
Lynch CP, Hernandez-Tejada MA, Strom JL, Egede LE (2012) Association between spirituality and depression in adults with type 2 diabetes. Diabetes Educ 38(3):427–435
Ironson G, Lucette A, Hylton E, Pargament KI, Krause N (2018) The relationship between religious and psychospiritual measures and an inflammation marker (CRP) in older adults experiencing life event stress. J Relig Health 57(4):1554–1566
Sephton SE, Koopman C, Schaal M, Thoresen C, Spiegel D (2001) Spiritual expression and immune status in women with metastatic breast cancer: an exploratory study. Breast J 7(5):345–353
Lou M, Luo P, Tang R et al (2015) Relationship between neutrophil-lymphocyte ratio and insulin resistance in newly diagnosed type 2 diabetes mellitus patients. BMC Endocr Disord 15(1):1–6
Femlak M, Gluba-Brzózka A, Ciałkowska-Rysz A, Rysz J (2017) The role and function of HDL in patients with diabetes mellitus and the related cardiovascular risk. Lipids Health Dis 16(1):1–9
Xiong Q, Liu J, Xu Y (2019) Effects of uric acid on diabetes mellitus and its chronic complications. Int J Endocrinol. https://doi.org/10.1155/2019/9691345
Kobayashi D, Shimbo T, Takahashi O, Davis RB, Wee CC (2015) The relationship between religiosity and cardiovascular risk factors in Japan: a large–scale cohort study. J Am Soc Hypertens 9(7):553–562
Funding
This research was supported by grant of the Institute of Clinical Medicine Research in the Yeouido St. Mary’s hospital, Catholic University of Korea.
Author information
Authors and Affiliations
Contributions
SMO, SHK, KDH and YME participated in the design of the study, data collection, performed the statistical analysis and drafted the manuscript. JHC, CMK, SJP and MKI supervising the study and participated in draft review. All authors have read and approved the final version of the manuscript and agree with the order of presentation of the authors.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no competing interests.
Ethical approval
The study protocol was approved by the Clinical Research Review Board of the Catholic medical center of Korea (IRB No: XC20RIDI0058) and conducted in accordance with the Declaration of Helsinki. Since data were anonymous and used in aggregated form, no subjects’ informed consent was needed according to local ethic committee indications.
Informed consent
The study protocol was approved by the Clinical Research Review Board of the Catholic medical center of Korea (IRB No: XC20RIDI0058) and conducted in accordance with the Declaration of Helsinki. Since data were anonymous and used in aggregated form, no subjects’ informed consent was needed according to local ethic committee indications.
Additional information
Managed by Massimo Porta.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Eun, Y., Ock, S.M., Kim, SH. et al. Risk of type 2 diabetes mellitus in catholic priests compared with general public. Acta Diabetol 60, 655–661 (2023). https://doi.org/10.1007/s00592-023-02041-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-023-02041-y