Abstract
Aims
Alterations of the exocrine pancreas have been reported in type 1 diabetes, but their contribution to the pathogenesis of the disease is poorly understood. Here, we investigated markers of exocrine pancreas dysfunction in individuals at-risk of developing type 1 diabetes.
Methods
Serum P-amylase and lipase levels were assessed in samples obtained from healthy controls, patients with new onset type 1 diabetes, relatives participating to the TrialNet Pathway to Prevention who were, at blood collection, autoantibody negative or positive for a single autoantibody (low-risk individuals), and positive for multiple autoantibodies (high-risk individuals). Linear mixed models were adopted to estimate variation of pancreatic enzymes among the groups and to evaluate the influence of high-risk HLA genotypes and residual beta cell function on exocrine pancreas function.
Results
In adults, but not children, reduced levels of P-amylase and lipase were shown in at-risk individuals, including (for P-amylase levels only) those at low-risk, and in T1Dnew. Furthermore, while high-risk HLA genotypes negatively affected P-amylase levels in autoantibody negative adult individuals, fasting C-peptide levels did not correlate with pancreatic enzyme levels.
Conclusions
Exocrine pancreas dysfunction precedes the onset of type 1 diabetes in adult at-risk individuals and may be unrelated to fasting C-peptide levels.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 1 diabetes (T1D) has been recently reconsidered as a disease of the whole pancreas, rather than exclusively characterized by self-reactive T cell-mediated beta cell destruction. In fact, consistent evidence now suggests that the exocrine component of the pancreas, mainly composed of acinar cells that produce digestive enzymes, is also involved in the disease process leading to beta cell loss.
Data corroborating this hypothesis are structural, immunopathological and functional. Pancreas weight and volume are reduced in patients with overt type 1 diabetes as well as at-risk individuals, including relatives with and without islet autoantibodies, suggesting that pancreas remodeling occurs before and after seroconversion and may be genetically determined [1,2,3,4,5,6,7]. Immune cells are abundant both in the islets and the exocrine compartment [8,9,10,11,12,13], and autoantibodies targeting exocrine pancreas-derived proteins were described in at-risk individuals as well as in patients with type 1 diabetes [14]. The reduced pancreatic mass, accompanied by immune cell infiltration, results in a subclinical exocrine functional impairment, characterized by an overall reduction of exocrine pancreatic enzymes, with trypsinogen, lipase and fecal elastase (FE-1) levels already decreased in at-risk individuals [15,16,17,18].
The heterogeneous clinical phenotype observed in patients with type 1 diabetes led investigators to propose the use of the ‘endotype model’, originally applied to the asthma field [19], also in type 1 diabetes. This model is based on the assumption that different mechanisms underlie the pathogenesis of the disease and can explain, at least to some extent, the variety of clinical phenotypes [20]. Here, we hypothesized that exocrine pancreas dysfunction contributes to type 1 diabetes heterogeneity; therefore, in this study, we attempted to clarify how pancreatic enzyme abnormalities associate with age, sex, high-risk HLA genotypes, islet autoantibodies status and fasting C-peptide in individuals at various stages (low-risk, high-risk, clinical onset) of progression to type 1 diabetes.
Understanding the patterns of exocrine pancreas pathophysiology in at-risk, pre-symptomatic individuals can contribute to the understanding of type 1 diabetes heterogeneity and underlying endotypes.
Methods
Subjects
Subjects participating in this study were enrolled at Ospedale San Raffaele (OSR), Milan (Italy) from December 2010 to February 2019. In this study, 3 groups of subjects were enrolled. Group 1: relatives of patients with T1D were participants to the TN01 TrialNet Pathway to Prevention Study (formerly Natural History Study) [21]. Based on their islet autoantibody profile at study entry, relatives were recruited as follows: autoantibody negative (AAb−, n = 276), subjects positive for single (AAb1 + , n = 74) or multiple (2 or more) autoantibodies (AAb ≥ 2 + , n = 50). The risk of progression to clinical type 1 diabetes is negligible in those negative, around 15% in those with a single autoantibody (low-risk), and more than 80% in those with multiple autoantibodies (high-risk) in the following 15 years [22, 23]. A fraction of at-risk subjects, equal to 14.6% (107 subjects out of 732), was followed longitudinally in the TN01, and multiple samples obtained from these individuals were used in this study (referred to as repeated measures). The total number of samples was 1092 from 732 subjects within 598 families. Group 2: patients with new onset type 1 diabetes (T1Dnew, n = 86) according to the American Diabetes Association criteria [24] were enrolled either at the Pediatric or General Medicine, Diabetes and Endocrinology Departments of the Ospedale San Raffaele, Milan, Italy. Blood samples were withdrawn within 3 months from diagnosis. In patients presenting with diabetic ketoacidosis (DKA), blood samples were collected at least five days after hospital admission to rule out potential confounding factors affecting pancreatic enzyme levels [25]. Group 3: healthy non-diabetic controls (HC, n = 246) with no family history for type 1 diabetes undergoing surgery for congenital diseases (i.e., flatfeet or hallux valgus) at the OSR Orthopedic Department. Subjects with current infection or missing data were excluded from the study. Detailed characteristics of participants are shown in Table 1.
Study approval
The study was approved by the Ospedale San Raffaele (OSR) Ethics Committee (IRB#TIGET004-DRI003). First-degree relatives of T1D patients were enrolled in the T1D TrialNet Pathway to Prevention Trial (TN01) at OSR (IRB# NHPROT32803-TN01). Peripheral blood was collected for mechanistic studies (approved by the TrialNet Ancillary Studies Subcommittee). All participants (or parents for pediatric individuals) provided written informed consent. Participants over the age of 12 signed an additional study assent form.
Blood tests
Serum P-amylase, lipase and C-peptide concentrations were measured in the Ospedale San Raffaele central laboratory by automated methods, as follows. Serum P-amylase levels were measured using the enzymatic colorimetric method after inhibition of human salivary α-amylase (Cobas C, Roche/Hitachi, Roche Diagnostics GmbH, Mannheim, Germany); serum lipase levels using the enzymatic colorimetric method (Cobas C, Roche/Hitachi, Roche Diagnostics GmbH, Mannheim, Germany); fasting serum C-peptide levels using Electrochemiluminescent Assay, CLIA, on automatic Instrumentation Cobas 8000 (Roche Diagnostics GmbH, Mannheim, Germany). Reference ranges for the above enzymes are: P-amylase, 0–20 U/L (0–24 months), 9–35 U/L (2–18 years) subjects, 13–53 U/L (> 18 years); lipase: 0–60 U/L. The following islet autoantibodies were measured in all enrolled participants except HC: islet cell antibodies (ICA), anti-IA2, anti-GAD, anti-insulin (IAA) and anti-ZnT8. Measurements were performed according to study protocol [21]. ICA were not routinely measured in T1Dnew. HLA genotypes were performed in an European Federation for Immunogenetics (EFI) accredited laboratory using the HISTO SPOT SSO System (BAG Health Care GmbH, Germany). DRB1*03 (DR3) and DRB1*04 (DR4) alleles are considered high-risk HLA genotypes for the development of type 1 diabetes [26].
Statistical analysis
Linear mixed-effects models (LME) were employed to estimate the longitudinal trend of the amylase and the lipase and evaluate the differences among groups, since the data consist of repeated measurements of the same subjects with some subjects belonging to the same family. Random effects were accordingly defined, nested by family and by subject. In order to meet the assumptions of normality of the model, the square root transformation was applied to the amylase and the logarithmic transformation was applied to the lipase. Both linear and quadratic terms for age at sample collection were included in the model to account for the nonlinear trajectories of amylase and lipase over time. In the models, we also accounted for the possible effect of sex and the disease-groups (HC, AAb−, AAb1 + or AAb ≥ 2 + and T1Dnew) at sample collection, for the interaction effect between the sex and the disease-groups and for the interaction effect between the age and the disease-groups. Backward selection procedures were applied to select the most parsimonious model. Post-hoc analysis after LME was performed, considering all the pairwise comparisons of disease-groups at a fixed age. p-values were adjusted using Bonferroni’s correction. LME models were also employed to evaluate the effect of high-risk HLA genotypes and fasting C-peptide on amylase and lipase. These effects were evaluated separately and accounting for the possible effects of age, sex and disease-groups and the interactions with these variables. All statistical analyses were performed using R 3.6.3 (http://www.R-project.org/) and the significance threshold was set at 0.05.
Results
Serum levels of P-amylase and lipase are decreased in adult relatives of patients with type 1 diabetes, but not in children
Serum P-amylase and lipase levels were evaluated in relation to age and sex in HC, relatives of patients with type 1 diabetes (i.e., AAb−, AAb1 + or AAb ≥ 2 +) and T1Dnew. Table 1 shows characteristics of participants including all 1092 observations from 732 subjects. The linear mixed-effects model showed that P-amylase levels increase with age in all groups although with different trends (Fig. 1a and Table S1). In HC, a significant positive linear effect of age is evident. Low-risk relatives (i.e., AAb− and AAb1 + individuals), although presenting a lower slope than HC, also showed increased P-amylase levels with age. In T1Dnew, P-amylase levels decreased during childhood and early adolescence, starting to rise only after the age of 15. Of note, high-risk individuals (AAb ≥ 2 +) showed a relatively flat curve until their 20 s, with an intermediate pattern between low-risk relatives and T1Dnew. Although within the normal range, in adults (Fig. 1b showing the status at age 30) estimated serum P-amylase levels were significantly reduced in at-risk individuals, already before seroconversion, and in T1Dnew patients. This was not observed in children, where the significant reduction was evident only in T1Dnew (Fig. 1c showing the status at age 10).
Reduction of serum amylase and lipase occurs in adult relatives of type 1 diabetes but not in children. a Final linear mixed-effects model for predicting serum P-amylase levels based on disease-groups, age and sex as well as interactions among variables are shown. b–c Pairwise post-hoc comparisons among groups at fixed age for estimated level of P-amylase in female subjects. d Final linear mixed-effects model for predicting serum lipase levels on the basis of the disease-groups, age and sex as well as interactions with them are shown. e–f Pairwise post-hoc comparisons among groups at fixed age for estimated level of lipase in female subjects. Only significative comparisons p-values are shown in the graph
Age-dependent levels of lipase showed a similar trend compared to P-amylase, but differed in that HC have a less steep curve and subjects with multiple autoantibodies overlap with T1Dnew patients (Fig. 1d and Table S2). Serum lipase levels in adults (30 years; Fig. 1e and Figure S1b left panel), but not in children (10 years; Fig. 1f and Fig. S1b right panel), were found significantly reduced in relatives with multiple autoantibodies and in T1Dnew patients compared to HCs. No statistical differences were evident between adult low-risk relatives and HCs (AAb− vs. HC, p = 0.090; AAb1 + vs. HC, p = 0.209) (Fig. 1e). Unexpectedly, lipase levels were increased in AAb− pediatric individuals compared to HCs, but declined in AAb ≥ 2 + subjects.
With regard to sex, males showed significantly lower levels of both P-amylase and lipase compared to females within all groups (Fig. S1).
Overall, these data indicate that exocrine pancreas function is impaired in adults, but not in children, already during pre-symptomatic stages of type 1 diabetes. Moreover, in the case of P-amylase, function impairment is detectable already prior to islet autoantibody seroconversion, suggesting a possible genetic predisposition to exocrine dysfunction.
High-risk HLA genotypes negatively affect P-amylase levels of AAb1+ adult individuals
The effect of high-risk HLA genotypes DR3 and/or DR4 on the exocrine pancreas function was tested in at-risk individuals. The presence of high-risk HLA genotypes has a negative effect on P-amylase (Table 2) in AAb1+ individuals only (AAb1+ × Age x HLA, p-value = 0.024), with a trend observed in AAb ≥ 2+ subjects (Ab POS ≥ 2+ × Age x HLA, p-value = 0.099), and no effect in AAb− (Ab POS ≥ 2+ × Age x HLA, p-value = 0.773). Notably, the effect of high-risk HLA in AAb1+ relatives was greater with increasing age (AAb1+ × Age, Ab POS ≥ 2+ × Age, p-value < 0.001), suggesting that the high-risk HLA genotypes are associated with lower P-amylase levels in adults more than in children. No effect of high-risk HLA genotypes was observed on lipase levels (data not shown).
Fasting C-peptide levels do not correlate with pancreatic enzymes reduction
To test the hypothesis that exocrine pancreas dysfunction is influenced by the loss of insulin secretion during the pre-symptomatic stage of type 1 diabetes, we evaluated the effect of fasting C-peptide on P-amylase and lipase levels, accounting for the possible effects of age, sex and disease-groups and the interactions with these variables. After backward selection, the final models did not include fasting C-peptide levels (data not shown) indicating lack of relationship between the two variables.
Discussion
Exocrine pancreas dysfunction is commonly accepted as a feature of type 1 diabetes, as evidence from multiple independent studies have shown decreased levels of pancreatic enzymes [15,16,17,18, 27,28,29,30]. In this study, we demonstrate that impaired exocrine function, resulting in lower levels of circulating P-amylase and lipase, can be detected long before the onset of clinical symptoms in at-risk adult individuals, but not in children. It can be postulated that the exocrine pancreas is able to better counteract type 1 diabetes-associated pathogenetic destruction during infancy and early adolescence than in adult age, possibly thanks to the development and regeneration ability of the pancreas in childhood [31]. This would lead to stable P-amylase levels during the pre-symptomatic stages of type 1 diabetes as observed at the age of 10, while declining thereafter as shown at the age of 30. Since the study population was not randomly selected as it is part of a large T1D prevention trial, it cannot be excluded that, when subjects were aware of their autoantibody status, their lifestyle habits changed in such a way as to affect P-amylase and lipase levels. Furthermore, although this is an observational study in which subjects were selected retrospectively, with a non-negligible selection bias, our analysis allowed to control for a number of confounding factors. To strengthen these results, a validation cohort would be needed.
Reduced levels of FE-1 [16], serum trypsinogen [17] and lipase [18] have been reported in children at-risk of developing type 1 diabetes. In our analysis, we have taken into account the effect of multiple parameters (such as age, sex and number of autoantibodies) on P-amylase and lipase levels. The different pattern of exocrine pancreas dysfunction observed between children and adults may explain why, in another study [18], pancreatic enzymes were not found reduced in individuals with low-risk of developing type 1 diabetes. However, it should be noted that a limitation of our study is the lack of body mass index (BMI) and pubertal status data, which may affect pancreatic enzyme levels [32]. Although serum P-amylase and lipase levels are not considered sensitive biomarkers of exocrine pancreas function [33], our data are consistent with previous reports showing that exocrine pancreatic enzymes are a serological biomarker for T1D staging.
The lack of relationship between P-amylase with fasting C-peptide levels suggests that the counterregulatory mechanisms against the progression of type 1 diabetes in younger age are more effective for the exocrine, as reflected by stable P-amylase, than the endocrine pancreas, as reflected by declining C-peptide. On the other hand, this divergence is unlikely to persist with advancing age and disease progression, as indicated by the recently reported correlation between P-amylase and C-peptide in adult new onset and long-standing type 1 diabetes [29]. However, it should be considered that fasting C-peptide, although considered a reasonably good indicator of endogenous insulin secretion [34], it is not the best way to estimate residual beta cell function, thus leaving still uncertain whether exocrine and endocrine compartments of the pancreas are interdependent in the natural history of type 1 diabetes.
The evidence that low-risk adult relatives display reduced P-amylase levels suggests that the genetic background may influence the impairment of exocrine pancreas function. However, with regard to HLA, we show that high-risk genotypes impact exocrine dysfunction only in adult single autoantibody-positive individuals. It is possible that increasing sample size may help clarify the effect of HLA genotypes in multiple autoantibody-positive subjects. However, since other non-HLA genes may be equally involved in exocrine pancreas dysfunction, additional studies are needed to more comprehensively address the role of the genetics.
There is growing evidence that, behind the clinical phenotype, there are different mechanisms contributing to the pathogenesis of type 1 diabetes, thus highlighting the need to unveil disease endotypes [20]. Besides the heterogeneity of type 1 diabetes in terms of age at disease onset, genetic susceptibility, decline of residual beta cell function and pancreas-specific immune cell infiltrate, here we provide evidence that exocrine pancreas dysfunction occurs in at-risk adult individuals, possibly reflecting an endotype with a low progression rate. So far, the abnormalities of exocrine pancreatic function have been considered subclinical; however, in the perspective of a new trait of endotype heterogeneity, the possible clinical impact of exocrine pancreatic dysfunction in type 1 diabetes should be studied more in depth in the future.
Conclusion
In conclusion, our findings provide evidence that the exocrine pancreas dysfunction detected during the pre-symptomatic stages of type 1 diabetes show different patterns of progression according to age, possibly reflecting a further trait of endotype heterogeneity.
Availability of data and material
The data supporting the findings of this study are available within the article [and/or] its supplementary materials.
Abbreviations
- AAb−:
-
Autoantibody negative
- AAb1 + :
-
Positive for 1 islet autoantibody
- AAb ≥ 2 + :
-
Positive for 2 or more islet autoantibodies
- BMI:
-
Body Mass Index
- DKA:
-
Diabetic ketoacidosis
- DR3:
-
DRB1*03
- DR4:
-
DRB1*04
- FE-1:
-
Fecal elastase-1
- GAD:
-
Glutamic acid decarboxylase
- HC:
-
Healthy controls
- HLA:
-
Human Leukocyte Antigens
- IA2:
-
IA‐2 molecule (IA‐2A)
- IAA:
-
Insulin autoantibodies
- ICA:
-
Cytoplasmic islet cell antibodies
- LME:
-
Linear mixed model
- OSR:
-
Ospedale San Raffaele
- P-amylase:
-
Pancreatic amylase
- T1D:
-
Type 1 diabetes
- T1Dnew:
-
New onset type 1 diabetes patients
- TN01:
-
TrialNet Pathway to Prevention Study
- ZnT8:
-
Zinc transporter isoform 8
References
Campbell-Thompson ML et al. (2016) The influence of type 1 diabetes on pancreatic weight. Diabetologia 59(1):217–221
Campbell-Thompson ML et al. (2019) Relative pancreas volume is reduced in first-degree relatives of patients with Type 1 Diabetes. Diabetes Care 42(2):281–287
Virostko J et al. (2019) Pancreas volume declines during the first year after diagnosis of type 1 diabetes and exhibits altered diffusion at disease onset. Diabetes Care 42(2):248–257
Augustine P et al. (2020) Pancreas size and exocrine function is decreased in young children with recent-onset Type 1 diabetes. Diabet Med 37(8):1340–1343
Gaglia JL et al. (2011) Noninvasive imaging of pancreatic islet inflammation in type 1A diabetes patients. J Clin Invest 121(1):442–445
Williams AJ et al. (2012) Pancreatic volume is reduced in adult patients with recently diagnosed type 1 diabetes. J Clin Endocrinol Metab 97(11):E2109–E2113
Campbell-Thompson M et al. (2012) Pancreas organ weight in individuals with disease-associated autoantibodies at risk for type 1 diabetes. JAMA 308(22):2337–2339
Valle A et al. (2013) Reduction of circulating neutrophils precedes and accompanies type 1 diabetes. Diabetes 62(6):2072–2077
Rodriguez-Calvo T et al. (2014) Increased immune cell infiltration of the exocrine pancreas: a possible contribution to the pathogenesis of type 1 diabetes. Diabetes 63(11):3880–3890
de Boer P et al. (2020) Large-scale electron microscopy database for human type 1 diabetes. Nat Commun 11(1):2475
Damond N et al. (2019) A Map of Human Type 1 Diabetes Progression by Imaging Mass Cytometry. Cell Metab 29(3):755-768.e5
Korsgren S et al. (2012) On the etiology of type 1 diabetes: a new animal model signifying a decisive role for bacteria eliciting an adverse innate immunity response. Am J Pathol 181(5):1735–1748
Bender C et al. (2020) The healthy exocrine pancreas contains preproinsulin-specific CD8 T cells that attack islets in type 1 diabetes. Sci Adv 6(42).
Panicot L et al. (1999) Circulating antibodies against an exocrine pancreatic enzyme in type 1 diabetes. Diabetes 48(12):2316–2323
Kondrashova A et al. (2018) Exocrine pancreas function decreases during the progression of the beta-cell damaging process in young prediabetic children. Pediatr Diabetes 19(3):398–402
Penno MAS et al. (2020) Changes in pancreatic exocrine function in young at-risk children followed to islet autoimmunity and type 1 diabetes in the ENDIA study. Pediatr Diabetes.
Li X et al. (2017) Serum trypsinogen levels in Type 1 diabetes. Diabetes Care 40(4):577–582
Ross JJ et al. (2021) Exocrine pancreatic enzymes are a serological biomarker for Type 1 diabetes staging and pancreas size. Diabetes 70(4):944–954
Lötvall J et al. (2011) Asthma endotypes: a new approach to classification of disease entities within the asthma syndrome. J Allergy Clin Immunol 127(2):355–360
Battaglia M et al. (2020) Introducing the endotype concept to address the challenge of disease heterogeneity in Type 1 diabetes. Diabetes Care 43(1):5–12
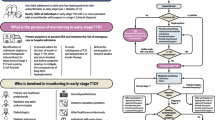
Sims EK et al. (2019) Who is enrolling? The path to monitoring in Type 1 diabetes TrialNet’s Pathway to prevention. Diabetes Care 42(12):2228–2236
Ziegler AG et al. (2013) Seroconversion to multiple islet autoantibodies and risk of progression to diabetes in children. JAMA 309(23):2473–2479
Orban T et al. (2009) Pancreatic islet autoantibodies as predictors of type 1 diabetes in the Diabetes Prevention Trial-Type 1. Diabetes Care 32(12):2269–2274
(2021) Classification and diagnosis of diabetes: standards of medical care in diabetes-2021. Diabetes Care 44(Suppl 1):S15–S33
Haddad NG, Croffie JM, Eugster EA (2004) Pancreatic enzyme elevations in children with diabetic ketoacidosis. J Pediatr 145(1):122–124
Concannon P et al. (2005) Type 1 diabetes: evidence for susceptibility loci from four genome-wide linkage scans in 1,435 multiplex families. Diabetes 54(10):2995–3001
Madole MB et al. (2016) Evaluation of biochemical markers serum amylase and serum lipase for the assessment of pancreatic exocrine function in diabetes mellitus. J Clin Diagn Res 10(11):BC01–BC04.
Ludvigsson J (2019) No acute pancreatitis but reduced exocrine pancreatic function at diagnosis of type 1 diabetes in children. Pediatr Diabetes 20(7):915–919
Dozio N et al. (2021) Impaired exocrine pancreatic function in different stages of type 1 diabetes. BMJ Open Diabetes Res Care 9(1).
Icks A et al. (2001) Low fecal elastase-1 in type I diabetes mellitus. Z Gastroenterol 39(10):823–830
Watanabe H et al. (2005) Aging is associated with decreased pancreatic acinar cell regeneration and phosphatidylinositol 3-kinase/Akt activation. Gastroenterology 128(5):1391–1404
Kondo T et al. (1988) Serum levels of pancreatic enzymes in lean and obese subjects. Int J Pancreatol 3(4):241–248
Laterza L et al. (2013) Pancreatic function assessment. Eur Rev Med Pharmacol Sci 17(Suppl 2):65–71
Besser RE et al. (2013) Lessons from the mixed-meal tolerance test: use of 90-minute and fasting C-peptide in pediatric diabetes. Diabetes Care 36(2):195–201
Funding
Dr. Petrelli is supported by the Juvenile Diabetes Research Foundation JDRF (no. 3-APF-2019-744-AN). All authors have read and approved the final version of the manuscript.
Author information
Authors and Affiliations
Contributions
AG and FV planned the analyses, contributed to data interpretation and discussion, drafted, revised and approved the final version of the article. AS and AM provided biological samples, performed data acquisition, patient selections, contributed to data interpretation, revised and approved the final version of the article. BAM performed data acquisition and contributed to data interpretation, revised and approved the final version of the article. FC and AN performed statistical analysis and contributed to data interpretation, revised and approved the final version of the article. MDP, AL and RB contributed to patient selection, provided biological samples, contributed to data interpretation, revised and approved the final version of the article. MB designed the study, contributed to the discussion, revised and approved the final version of the article. EB coordinated the study, interpretated the data, contributed to the discussion, revised and approved the final version of the article. AP coordinated the study, interpretated the data, contributed to the discussion, drafted, revised and approved the final version of the article.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Ospedale San Raffaele IRB#TIGET004-DRI003 and IRB# NHPROT32803-TN01).
Consent to participate
Informed consent to participate in the study was obtained from participants or their parent or legal guardian in the case of children under 18.
Consent to publish
Not applicable.
Additional information
Managed by Antonio Secchi.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Manuela Battaglia, Emanuele Bosi, and Alessandra Petrelli jointly directed this work.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Giovenzana, A., Vecchio, F., Cugnata, F. et al. Exocrine pancreas function is impaired in adult relatives of patients with type 1 diabetes. Acta Diabetol 59, 473–479 (2022). https://doi.org/10.1007/s00592-021-01819-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-021-01819-2