Abstract
Purpose
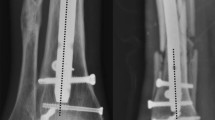
In treating distal third tibial fractures, restoration of the axial alignment and therefore accurate reduction of the distal fragment minimise the risk of tibiotalar joint malalignment. The aim of this study is to investigate whether there was a difference in accuracy of reduction and axial alignment, when nailing distal third tibial fractures using either the suprapatellar or the infrapatellar tibial nailing entry technique.
Methods
This retrospective cohort study compared alignment of intramedullary nails performed for distal third tibial fractures between 2015 and 2018 through the suprapatellar and infrapatellar approach at a UK Level 1 trauma centre. It compared a consecutive series of 74 suprapatellar nails and 51 infrapatellar nails, with radiographic assessment of tibial alignment in the antero-posterior and sagittal planes. It included inter- and intra-observer analyses of radiographic measurements.
Results
In the coronal plane, mean malalignment in the suprapatellar technique group was 2.8 ± 0.7° and 4.7 ± 0.9° in the infrapatellar technique group (P < 0.01). In the sagittal plane, mean malalignment in the suprapatellar technique group was 4.0 ± 0.8° and 3.5 ± 0.9° in the infrapatellar technique group (P = 0.42). Intra- and inter-observer analysis showed strongly positive correlations between observers.
Conclusions
We suggest that the suprapatellar technique may improve coronal plane alignment when intramedullary nailing distal tibial fractures. There was no significant difference in alignment in the sagittal plane. We conclude that the suprapatellar technique may be superior in preventing malalignment when treating distal third tibial fractures, potentially improving clinical outcome.





Similar content being viewed by others
References
Costa ML, Achten J, Hennings S et al (2018) Intramedullary nail fixation versus locking plate fixation for adults with a fracture of the distal tibia: the UK fixDT RCT. Health Technol Assess (Rockv) 22(25):1–147. https://doi.org/10.3310/hta22250
Vallier HA, Cureton BA, Patterson BM (2011) Randomized, prospective comparison of plate versus intramedullary nail fixation for distal tibia shaft fractures. J Orthop Trauma 25(12):736–741. https://doi.org/10.1097/BOT.0b013e318213f709
Il IG, Tae SK (2005) Distal metaphyseal fractures of tibia: A prospective randomized trial of closed reduction and intramedullary nail versus open reduction and plate and screws fixation. J Trauma - Inj Infect Crit Care 59(5):1219–1223. https://doi.org/10.1097/01.ta.0000188936.79798.4e
Hu L, Xiong Y, Mi B et al (2019) Comparison of intramedullary nailing and plate fixation in distal tibial fractures with metaphyseal damage: a meta-analysis of randomized controlled trials. J Orthop Surg Res 14(1):1–11. https://doi.org/10.1186/S13018-018-1037-1
Vallier HA, Le TT, Bedi A (2008) Radiographic and clinical comparisons of distal tibia shaft fractures (4 to 11 cm proximal to the plafond): Plating versus intramedullary nailing. J Orthop Trauma 22(5):307–311. https://doi.org/10.1097/BOT.0b013e31816ed974
Tarr RR, Resnick CT, Wagner KS, Sarmiento A (1985) Changes in tibiotalar joint contact areas following experimentally induced tibial angular deformities. Clin Orthop Relat Res 199:72–80. https://doi.org/10.1097/00003086-198510000-00011
Vallier HA, Cureton BA, Patterson BM (2012) Factors influencing functional outcomes after distal tibia shaft fractures. J Orthop Trauma 26(3):178–183. https://doi.org/10.1097/BOT.0b013e31823924df
Milner SA, Davis TRC, Muir KR, Greenwood DC, Doherty M (2002) Long-term outcome after tibial shaft fracture: is malunion important? J Bone Jt Surg 84A(6):971–980
Hiesterman TG, Shafiq BX, Cole PA (2011) Intramedullary nailing of extra-articular proximal tibia fractures. J Am Acad Orthop Surg 19(11):690–700. https://doi.org/10.5435/00124635-201111000-00005
Cole JD (2006) OPINION: Intramedullary nailing. J Orthop Trauma 20(1):73–74. https://doi.org/10.1097/01.bot.0000196658.55293.e6
Franke J, Hohendorff B, Alt V, Thormann U, Schnettler R (2016) Suprapatellar nailing of tibial fractures-Indications and technique. Injury 47(2):495–501. https://doi.org/10.1016/j.injury.2015.10.023
Jones M, Parry M, Whitehouse M, Mitchell S (2014) Radiologic outcome and patient-reported function after intramedullary nailing. J Orthop Trauma 28(5):256–262. https://doi.org/10.1097/BOT.0000000000000070
Avilucea FR, Triantafillou K, Whiting PS, Perez EA, Mir HR (2016) Suprapatellar intramedullary nail technique lowers rate of malalignment of distal tibia fractures. J Orthop Trauma 30(10):557–560. https://doi.org/10.1097/BOT.0000000000000631
Meinberg E, Agel J, Roberts C, Karam M, Kellam J (2018) Fracture and dislocation classification compendium—2018. J Orthop Trauma 32:S1–S10. https://doi.org/10.1097/BOT.0000000000001063
Paley D, Herzenberg JE, Tetsworth K, McKie J, Bhave A (1994) Deformity planning for frontal and sagittal plane corrective osteotomies. Orthop Clin North Am 25(3):425–465
Stryker Orthopaedics (325 Corporate Dr. Mahwah NJ 07110) (2013) T2 Tibial Nailing System Operative Technique. https://www.strykermeded.com/media/1315/t2-tibial-nailing-system-operative-technique.pdf
Wang C, Chen E, Ye C, Pan Z (2018) Suprapatellar versus infrapatellar approach for tibia intramedullary nailing: A meta-analysis. Int J Surg 51:133–139. https://doi.org/10.1016/j.ijsu.2018.01.026
Williamson M, Iliopoulos E, Williams R, Trompeter A (2018) Intra-operative fluoroscopy time and radiation dose during suprapatellar tibial nailing versus infrapatellar tibial nailing. Injury 49(10):1891–1894. https://doi.org/10.1016/j.injury.2018.07.004
Franke J, Homeier A, Metz L et al (2018) Infrapatellar vs suprapatellar approach to obtain an optimal insertion angle for intramedullary nailing of tibial fractures. Eur J Trauma Emerg Surg. 44(6):927–938. https://doi.org/10.1007/s00068-017-0881-8
Anderson TRE, Beak PA, Trompeter AJ (2019) Intra-medullary nail insertion accuracy: a comparison of the infra-patellar and supra-patellar approach. Injury 50(2):484–488. https://doi.org/10.1016/j.injury.2018.12.024
Sun Q, Nie XY, Gong JP et al (2016) The outcome comparison of the suprapatellar approach and infrapatellar approach for tibia intramedullary nailing. Int Orthop 40(12):2611–2617. https://doi.org/10.1007/s00264-016-3187-2
Prasad M, Yadav S, Sud A, Arora NC, Kumar N, Singh S (2013) Assessment of the role of fibular fixation in distal-third tibia-fibula fractures and its significance in decreasing malrotation and malalignment. Injury 44(12):1885–1891. https://doi.org/10.1016/j.injury.2013.08.028
Egol KA, Weisz R, Hiebert R, Tejwani NC, Koval KJ, Sanders RW (2006) Does fibular plating improve alignment after intramedullary nailing of distal metaphyseal tibia fractures? J Orthop Trauma 20(2):94–103. https://doi.org/10.1097/01.bot.0000199118.61229.70
Morin PM, Reindl R, Harvey EJ, Beckman L, Steffen T (2008) Fibular fixation as an adjuvant to tibial intramedullary nailing in the treatment of combined distal third tibia and fibula fractures: A biomechanical investigation. Can J Surg 51(1):45–50. https://doi.org/10.1016/S0008-428X(08)50009-9
Funding
No funding was received to support the study.
Author information
Authors and Affiliations
Contributions
I can confirm all authors have made substantial contributions to all the following: (1) The conception and design of the study, or acquisition of data, or analysis and interpretation of data, (2) Drafting the article or revising it critically for important intellectual content, (3) Final approval of the version to be submitted.
Corresponding author
Ethics declarations
Conflict of interest
A. Trompeter receives payment for educational activities related to Smith and Nephew, Styker and Orthofix Products. A Trompeter is a paid consultant of Stryker Trauma in relation to research and Development. The other authors report no conflict of interest.
Ethical approval
Institutional ethical approval was not required. Consent for use of patient imaging for research purposes was gained as part of the normal consent process for operative procedures in the authors’ institution.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hague, M., Texeira, D., Anderson, T. et al. Nailing distal tibial fractures: does entry technique affect distal alignment?. Eur J Orthop Surg Traumatol 33, 61–66 (2023). https://doi.org/10.1007/s00590-021-03148-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-021-03148-0