Abstract
Objectives
Iliosacral (IS) and transsacral (TS) screws are commonly used to stabilize pelvic ring injuries. The course of the superior gluteal artery (SGA) can be close to implant insertion paths. The third sacral segment (S3) has been described as a viable osseous fixation pathway (OFP) but the proximity of the SGA to the S3 screw path is unknown.
Methods
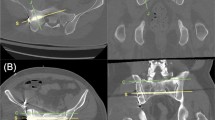
Fifty uninjured patients with contrasted pelvic computed tomograms (CTA) were identified with an S3 path large enough for a 7.0 mm TS screw. Starting sites for S1 IS or TS, S2 and S3 TS screws were located on the volume rendered lateral CTA image and transferred onto the surface rendered 3D CTA with the SGA clearly visible. The distance from screw start sites to the SGA was measured. A distance less than 3.5 mm was considered likely for injury.
Results
The average distances from screw start sites to the SGA were 23.0 ± 7.9 mm for S1 IS screws, 14.3 ± 6.4 mm for S2 TS screws and 25.9 ± 6.5 mm for S3 TS screws. No S1 IS screws, 5 S2 TS screws (10%), and no S3 TS screws were projected to cause injury to the SGA.
Conclusions
The osseous start site and soft tissue path for an S3 TS screw is remote from the SGA. The S1 IS and S3 TS pathways are further away from the SGA while the S2 TS pathway is closer and may theoretically pose a higher injury risk in patients with an available S3 OFP.




Similar content being viewed by others
References
Routt ML Jr, Kregor PJ, Simonian PT et al (1995) Early results of percutaneous iliosacral screws placed with the patient in the supine position. J Orthop Trauma 9:207–214
Routt ML Jr, Simonian PT (1996) Closed reduction and percutaneous skeletal fixation of sacral fractures. Clin Orthop Relat Res 329:121–128
Keating JF, Werier J, Blachut P et al (1999) Early fixation of the vertically unstable pelvis: the role of iliosacral screw fixation of the posterior lesion. J Orthop Trauma 13:107–113
Routt ML Jr, Nork SE, Mills WJ (2000) Percutaneous fixation of pelvic ring disruptions. Clin Orthop Relat Res 375:15–29
Nork SE, Jones CB, Harding SP et al (2001) Percutaneous stabilization of U-shaped sacral fractures using iliosacral screws: technique and early results. J Orthop Trauma 15:238–246
Moed BR, Geer BL (2006) S2 iliosacral screw fixation for disruptions of the posterior pelvic ring: a report of 49 cases. J Orthop Trauma 20:378–383
Gardner MJ, Routt ML Jr (2011) Transiliac-transsacral screws for posterior pelvic stabilization. J Orthop Trauma 25:378–384
Altman DT, Jones CB, Routt ML (1999) Superior gluteal artery injury during iliosacral screw placement. J Orthop Trauma. 13:220–222
Gansslen A, Hufner T, Krettek C (2006) Percutaneous iliosacral screw fixation of unstable pelvic injuries by conventional fluoroscopy. Oper Orthop Traumatol. 18:225–244
Collinge CA, Coons DA, Aschenbrenner J (2005) Risks to the superior gluteal neurovascular bundle during percutaneous iliosacral screw insertion: an anatomical cadaver study. J Orthop Trauma 19:96–101
Marmor M, Lynch T, Matityahu A (2010) Superior gluteal artery injury during iliosacral screw placement due to aberrant anatomy. Orthopedics 33:117–120
Maled I, Velez R, Lopez R et al (2007) Pseudoaneurysm of the superior gluteal artery during iliosacral screw fixation. Acta Orthop Belg 73(4):544–547
Stephen DJ (1997) Pseudoaneurysm of the superior gluteal arterial system: an unusual cause of pain after a pelvic fracture. J Trauma 43(1):146–149
Ebraheim NA, Olexa TA, Xu R et al (1998) The quantitative anatomy of the superior gluteal artery and its location. Am J Orthop 27:427–431
Jacobs L, Buxton RA (1989) The course of the superior gluteal nerve in the lateral approach to the hip. J Bone Joint Surg Am 71:1239–1243
Smith A, Chitre V, Deo H (2012) Acute gluteal compartment syndrome: superior gluteal artery rupture following a low energy injury. BMJ Case Rep. https://doi.org/10.1136/bcr-2012-007710
Schweitzer D, Zylberberg A, Cordova M et al (2008) Closed reduction and iliosacral percutaneous fixation of unstable pelvic ring fractures. Injury 29:869–874
Sullivan MP, Scolaro JA, Milby AH et al (2015) Isolated pelvic ring injuries: functional outcomes following percutaneous posterior fixation. Eur J Orthop Surg Traumatol 25:1025–1030
Iorio JA, Jakoi AM, Rehman S (2015) Percutaneous screw fixation of posterior pelvic ring. Orthop Clin North Am 46:511–521
Maslow J, Collinge CA (2017) Risks to the superior gluteal neurovascular bundle during iliosacral and transsacral screw fixation: a computed tomogram arteriography study. J Ortho Trauma 31(12):640–643
Zhao Y, You L, Lian W et al (2018) Anatomical relation between S1 sacroiliac screws’ entrance points and superior gluteal artery. J Orthop Surg Res 13(1):15
Eastman JG, Adams MR, Frisoli K et al (2018) Is S3 a viable osseous fixation pathway. J Orthop Trauma 32(2):93–99
Hwang JS, Reilly MC, Shaath MK et al (2018) Safe zone quantification of the third sacral segment in normal and dysmorphic sacra. J Orthop Trauma 32(4):178–182
Radetzki F, Wohlrab D, Goehre F et al (2014) Anatomical conditions of the posterior pelvic ring regarding bisegmental transverse sacroiliac screw fixation: a 3D morphometric study of 125 pelvic CT datasets. Arch Orthop Trauma Surg 134:1115–1120
Lucas JF, Routt ML Jr, Eastman JG (2017) A useful preoperative planning technique for transiliac-transsacral screws. J Orthop Trauma 31:e25–e31
Kaiser SP, Gardner MJ, Liu J et al (2014) Anatomic determinants of sacral dysmorphism and implications for safe iliosacral screw placement. J Bone Jt Surg Am 96:e120
Miller AN, Routt ML Jr (2012) Variations in sacral morphology and implications for iliosacral screw fixation. J Am Acad Orthop Surg 20:8–16
Routt ML Jr, Simonian PT, Agnew SG et al (1996) Radiographic recognition of the sacral alar slope for optimal placement of iliosacral screws: a cadaveric and clinical study. J Orthop Trauma 10:171–177
Gardner MJ, Morshed S, Nork SE et al (2010) Quantification of the upper and second sacral segment safe zones in normal and dysmorphic sacra. J Orthop Trauma 24:622–629
Zhao Y, Li J, Wang D et al (2012) Comparison of stability of two kinds of sacro-iliac screws in the fixation of bilateral sacral fractures in a finite element model. Injury 43:490–494
Acknowledgements
All of the authors listed above did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All of the authors listed above have no relevant financial or non-financial interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Eastman, J.G., Kuse, Q.A., Routt, M.L.C. et al. Superior gluteal artery injury risk from third sacral segment transsacral screw insertion. Eur J Orthop Surg Traumatol 32, 965–971 (2022). https://doi.org/10.1007/s00590-021-03073-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-021-03073-2