Abstract
Introduction
Sacroiliac (SI) screws are used for osteosynthesis in unstable posterior pelvic ring injuries. In the cases of “sacral dysplasia”, in which the elevated upper sacrum does not allow a secure SI screw insertion into the S1 level, the S2 segment must be used to achieve stable fixation. The bone quality of the S2 segment is thinner compared to that of the S1 vertebra and may cause biomechanical weakness. An additional SI screw insertion into the S3 level may improve stability. With respect to the anatomical conditions of the posterior pelvic ring, there have been no anatomical investigations to date regarding SI screw placement into the third sacral segment.
Materials and methods
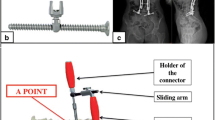
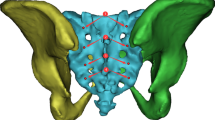
CT raw datasets from 125 patients (ø59 years, ø172 cm, ø76 kg) were post-processed using Amira 5.2 software to generate 3D pelvic models. A program code implemented in C++ computed a transverse bone corridor for the first, second and third sacral segments for a typical SI screw diameter of 7.3 mm. Volume, sagittal cross-section, iliac entrance area and length of the determined screw corridors were measured. A confidence interval of 95 % was assumed (p < 0.05).
Results
The fully automatic computation revealed a possible transverse insertion for one 7.3-mm screw in the third sacral segment in 30 cases (24 %). The rate (60 %) of feasible S3 screw placements in the cases of sacral dysplasia (n = 25) is significantly higher compared to that (15 %) of “normal” sacra (n = 100). With regard to the existence of transverse iliosacroiliac corridors as a function of sacral position in between the adjacent iliac bone bilaterally, a new classification of three different shape conditions can be made: caudad, intermediate minor, intermediate major, and cephalad sacrum. Gender, age, body height and body weight had no statistically significant influence on either possible screw insertion or on the calculated data of the corridors (p > 0.05).
Conclusion
SI screw insertion into the third sacral level deserves discussion in the cases of sacral dysplasia. Biomechanical and practical utility must be verified.



Similar content being viewed by others
References
Carlson DA, Scheid DK, Maar DC, Baele JR, Kaehr DM (2000) Safe placement of S1 and S2 iliosacral screws: the “vestibule” concept. J Orthop Trauma 14(4):264–269
Culemann U, Scola A, Tosounidis G, Pohlemann T, Gebhard F (2010) Concept for treatment of pelvic ring injuries in elderly patients. A challenge. Unfallchirurg 113(4):258–271
Day CS, Prayson MJ, Shuler TE, Towers J, Gruen GS (2000) Transsacral versus modified pelvic landmarks for percutaneous iliosacral screw placement—a computed tomographic analysis and cadaveric study. Am J Orthop 29(9 Suppl):16–21
Ebraheim N, Sabry FF, Nadim Y, Xu R, Yeasting RA (2000) Internal architecture of the sacrum in the elderly. An anatomic and radiographic study. Spine (Phila Pa 1976) 25(3):292–297
Ebraheim NA, Lin D, Xu R, Stanescu S, Yeasting RA (1999) Computed tomographic evaluation of the internal structure of the lateral mass in the upper sacra. Orthopedics 22(12):1137–1140
Griffin DR, Starr AJ, Reinert CM, Jones AL, Whitlock S (2006) Vertically unstable pelvic fractures fixed with percutaneous iliosacral screws: does posterior injury pattern predict fixation failure? J Orthop Trauma 20(1 Suppl):S30–S36
Hinsche AF, Giannoudis PV, Smith RM (2002) Fluoroscopy-based multiplanar image guidance for insertion of sacroiliac screws. Clin Orthop Relat Res 395:135–144
Kim JJ, Jung CY, Oh HK, Chang JS (2007) Measurement of optimal pelvic tilt angle for iliosacral screw fixation using 3-D CT scan. 8th EFORT Congress, Florence, Italy
Mehling I, Hessmann MH, Rommens PM (2012) Stabilization of fatigue fractures of the dorsal pelvis with a trans-sacral bar. Operative technique and outcome. Injury 43(4):446–451
Mendel T, Noser H, Kuervers J, Goehre F, Hofmann GO, Radetzki F (2013) The influence of sacral morphology on the existence of secure S1 and S2 transverse bone corridors for iliosacroiliac screw fixation. Injury 44(12):1773–1779
Mendel T, Noser H, Wohlrab D, Stock K, Radetzki F (2011) The lateral sacral triangle—a decision support for secure transverse sacroiliac screw insertion. Injury 42(10):1164–1170
Mendel T, Radetzki F, Wohlrab D, Stock K, Hofmann GO, Noser H (2013) CT-based 3-D visualisation of secure bone corridors and optimal trajectories for sacroiliac screws. Injury 44(7):957–963
Moed BR, Geer BL (2006) S2 iliosacral screw fixation for disruptions of the posterior pelvic ring: a report of 49 cases. J Orthop Trauma 20(6):378–383
Noser H, Radetzki F, Stock K, Mendel T (2011) A method for computing general sacroiliac screw corridors based on CT scans of the pelvis. J Digit Imaging 24(4):665–671
Peretz AM, Hipp JA, Heggeness MH (1998) The internal bony architecture of the sacrum. Spine (Phila Pa 1976) 23(9):971–974
Radetzki F, Mendel T, Noser H, Stoevesandt D, Rollinghoff M, Gutteck N et al (2013) Potentialities and limitations of a database constructing three-dimensional virtual bone models. Surg Radiol Anat 35(10):963–968
Reilly MC, Bono CM, Litkouhi B, Sirkin M, Behrens FF (2003) The effect of sacral fracture malreduction on the safe placement of iliosacral screws. J Orthop Trauma 17(2):88–94
Rommens PM (2007) Is there a role for percutaneous pelvic and acetabular reconstruction? Injury 38(4):463–477
Rommens PM, Hofmann A (2013) Comprehensive classification of fragility fractures of the pelvic ring: recommendations for surgical treatment. Injury 44(12):1733–1744
Routt ML Jr, Simonian PT, Agnew SG, Mann FA (1996) Radiographic recognition of the sacral alar slope for optimal placement of iliosacral screws: a cadaveric and clinical study. J Orthop Trauma 10(3):171–177
van Zwienen CM, van den Bosch EW, Snijders CJ, Kleinrensink GJ, van Vugt AB (2004) Biomechanical comparison of sacroiliac screw techniques for unstable pelvic ring fractures. J Orthop Trauma 18(9):589–595
Vanderschot P (2007) Treatment options of pelvic and acetabular fractures in patients with osteoporotic bone. Injury 38(4):497–508
Vanderschot P, Kuppers M, Sermon A, Lateur L (2009) Trans-iliac-sacral-iliac-bar procedure to treat insufficiency fractures of the sacrum. Indian J Orthop 43(3):245–252
Acknowledgments
The authors would like to thank the AO Research Institute Davos/Switzerland for supporting this project and Prof. Dr. Andreas Wienke, PhD for assistance of the statistical analysis.
Conflict of interest
The authors confirm that there are no financial and personal relationships with any other people or organisations that could inappropriately influence the content or the statements of the submitted article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Radetzki, F., Wohlrab, D., Goehre, F. et al. Anatomical conditions of the posterior pelvic ring regarding bisegmental transverse sacroiliac screw fixation: a 3D morphometric study of 125 pelvic CT datasets. Arch Orthop Trauma Surg 134, 1115–1120 (2014). https://doi.org/10.1007/s00402-014-2022-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-014-2022-8