Abstract
Purpose
Spinopelvic parameters can be useful in identifying risk factors for lumbar degenerative disc disease, but few studies assess patients with single-level disc herniation and most do not evaluate symptoms. This comparative retrospective study was aimed to analyse spinopelvic parameters, symptoms and MRI changes in patients with single-level lumbar disc herniation undergoing conservative or surgical treatment.
Methods
Patients with clinical and radiological assessment (Japanese Orthopaedic Association Score) and an MRI evaluation of the lumbar spine were identified and divided into two groups: surgically treated (group A) and not requiring surgery (group B). Spinopelvic parameters were determined on standing profile radiographs of the lumbar spine and pelvis, and mean values were compared to those reported in the literature for normal subjects. MRI findings were graded according to the system described by Pfirrmann et al.
Results
The study included 71 patients with single-level lumbar disc herniation: 26 in group A (39.4 ± 12.1 years) and 45 in group B (51.4 ± 17.2 years). The notable differences in spinopelvic parameter means between the two groups did not reach statistical significance. A positive correlations of age with pelvic tilt and Pfirrmann changes with pelvic incidence was only found in group A, while both groups showed highly significant positive correlations of pelvic incidence with the spine’s conformational type (p = 0.001).
Conclusions
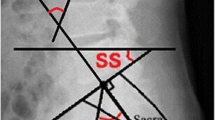
Characteristic changes in spinopelvic parameters identified in patients with lumbar degenerative disc disease were a reduction in pelvic incidence, sacral slope and lumbar lordosis, with an increased pelvic tilt. These were found to correlate with MRI changes in surgically treated patients.




Similar content being viewed by others
References
Katz JN (2006) Lumbar disc disorders and low-back pain: socioeconomic factors and consequences. J Bone Joint Surg Am 88(Suppl 2):21–24. doi:10.2106/JBJS.E.01273
Hoy D, Bain C, Williams G, March L, Brooks P, Blyth F, Woolf A, Vos T, Buchbinder R (2012) A systematic review of the global prevalence of low back pain. Arthritis Rheum 64(6):2028–2037. doi:10.1002/art.34347
Hoy D, Brooks P, Blyth F, Buchbinder R (2010) The Epidemiology of low back pain. Best Pract Res Clin Rheumatol 24(6):769–781. doi:10.1016/j.berh.2010.10.002
Schmidt CO, Raspe H, Pfingsten M, Hasenbring M, Basler HD, Eich W, Kohlmann T (2007) Back pain in the German adult population: prevalence, severity, and sociodemographic correlates in a multiregional survey. Spine (Phila Pa 1976) 32(18):2005–2011. doi:10.1097/BRS.0b013e318133fad8
Taher F, Essig D, Lebl DR, Hughes AP, Sama AA, Cammisa FP, Girardi FP (2012) Lumbar degenerative disc disease: current and future concepts of diagnosis and management. Adv Orthop 2012:970752. doi:10.1155/2012/970752
Oprea M, Popa I, Cimpean AM, Raica M, Poenaru DV (2015) Microscopic assessment of degenerated intervertebral disc: clinical implications and possible therapeutic challenge. Vivo 29(1):95–102
Vaz G, Roussouly P, Berthonnaud E, Dimnet J (2002) Sagittal morphology and equilibrium of pelvis and spine. Eur Spine J 11(1):80–87
Barrey C, Roussouly P, Le Huec JC, D’Acunzi G, Perrin G (2013) Compensatory mechanisms contributing to keep the sagittal balance of the spine. Eur Spine J 22(Suppl 6):S834–S841. doi:10.1007/s00586-013-3030-z
Gelb DE, Lenke LG, Bridwell KH, Blanke K, McEnery KW (1995) An analysis of sagittal spinal alignment in 100 asymptomatic middle and older aged volunteers. Spine (Phila Pa 1976) 20(12):1351–1358
During J, Goudfrooij H, Keessen W, Beeker TW, Crowe A (1985) Toward standards for posture. Postural characteristics of the lower back system in normal and pathologic conditions. Spine (Phila Pa 1976) 10(1):83–87
Duval-Beaupère G, Legaye J (2004) Composante sagittale de la statique rachidienne (in French). Rev Rhum 71:105–119. doi:10.1016/j.rhum.2003.09.018
Le Huec JC, Faundez A, Dominguez D, Hoffmeyer P, Aunoble S (2015) Evidence showing the relationship between sagittal balance and clinical outcomes in surgical treatment of degenerative spinal diseases: a literature review. Int Orthop 39(1):87–95. doi:10.1007/s00264-014-2516-6
Mehta VA, Amin A, Omeis I, Gokaslan ZL, Gottfried ON (2015) Implications of spinopelvic alignment for the spine surgeon. Neurosurgery 76(Suppl 1):S42–S56; discussion S56. doi:10.1227/01.neu.0000462077.50830.1a
Lazennec JY, Ramare S, Arafati N, Laudet CG, Gorin M, Roger B, Hansen S, Saillant G, Maurs L, Trabelsi R (2000) Sagittal alignment in lumbosacral fusion: relations between radiological parameters and pain. Eur Spine J 9(1):47–55
Ferrero E, Ould-Slimane M, Gille O, Guigui P, French Spine S (2015) Sagittal spinopelvic alignment in 654 degenerative spondylolisthesis. Eur Spine J 24(6):1219–1227. doi:10.1007/s00586-015-3778-4
Dai J, Yu X, Huang S, Fan L, Zhu G, Sun H, Tang X (2015) Relationship between sagittal spinal alignment and the incidence of vertebral fracture in menopausal women with osteoporosis: a multicenter longitudinal follow-up study. Eur Spine J 24(4):737–743. doi:10.1007/s00586-014-3637-8
Roussouly P, Gollogly S, Berthonnaud E, Dimnet J (2005) Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine (Phila Pa 1976) 30(3):346–353
Aykac B, Ayhan S, Yuksel S, Guler UO, Pellise F, Alanay A, Perez-Grueso FJ, Acaroglu E, Group EESS (2015) Sagittal alignment of cervical spine in adult idiopathic scoliosis. Eur Spine J 24(6):1175–1182. doi:10.1007/s00586-015-3868-3
Chaleat-Valayer E, Mac-Thiong JM, Paquet J, Berthonnaud E, Siani F, Roussouly P (2011) Sagittal spino-pelvic alignment in chronic low back pain. Eur Spine J 20(Suppl 5):634–640. doi:10.1007/s00586-011-1931-2
Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 26(17):1873–1878
Vrtovec T, Pernus F, Likar B (2009) A review of methods for quantitative evaluation of spinal curvature. Eur Spine J 18(5):593–607. doi:10.1007/s00586-009-0913-0
Barrey C, Jund J, Noseda O, Roussouly P (2007) Sagittal balance of the pelvis-spine complex and lumbar degenerative diseases. A comparative study about 85 cases. Eur Spine J 16(9):1459–1467. doi:10.1007/s00586-006-0294-6
Legaye J, Duval-Beaupere G, Hecquet J, Marty C (1998) Pelvic incidence: a fundamental pelvic parameter for three-dimensional regulation of spinal sagittal curves. Eur Spine J 7(2):99–103
Johnson RD, Valore A, Villaminar A, Comisso M, Balsano M (2013) Sagittal balance and pelvic parameters–a paradigm shift in spinal surgery. J Clin Neurosci 20(2):191–196. doi:10.1016/j.jocn.2012.05.023
Le Huec JC, Charosky S, Barrey C, Rigal J, Aunoble S (2011) Sagittal imbalance cascade for simple degenerative spine and consequences: algorithm of decision for appropriate treatment. Eur Spine J 20(Suppl 5):699–703. doi:10.1007/s00586-011-1938-8
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Mardare, M., Oprea, M., Popa, I. et al. Sagittal balance parameters correlate with spinal conformational type and MRI changes in lumbar degenerative disc disease: results of a retrospective study. Eur J Orthop Surg Traumatol 26, 735–743 (2016). https://doi.org/10.1007/s00590-016-1842-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-016-1842-3