Abstract
Purpose
To propose a novel Modic grading scoring system and explore the relationship between the Modic grading score and disc degeneration, disc herniation, disc height, and clinical symptom scores.
Method
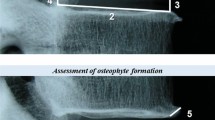
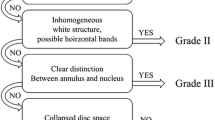
In total, 194 patients were included in the study. The new Modic grading scoring system included four indicators: invaded vertebral height, invaded endplate length, endplate morphology, and grade of endplate defects. The severity of Modic changes was visually quantified by numerical scores, and the kappa value was used to verify the interobserver and intraobserver reliability. Spearman correlation analysis was used to explore the relationship between the Modic grading score and intervertebral disc degeneration, disc herniation, disc height, and clinical symptom scores.
Results
The interobserver and intraobserver reliability showed substantial to almost perfect agreement in the new Modic grading scoring system. The Modic grading score was positively correlated with intervertebral disc degeneration (r = 0.757, p < 0.001) and negatively correlated with the intervertebral disc height index (r = − 0.231, p < 0.001). There was no significant correlation between the Modic grading scoring system and disc herniation (r = 0.369, p = 0.249). Additionally, there was no significant correlation between the Modic grading score and the Japanese Orthopaedic Association score (r = − 0.349, p = 0.25), Oswestry Disability Index score (r = 0.246, p = 0.11), or visual analogue scale score (r = 0.315, p = 0.35).
Conclusion
The new Modic grading scoring system had good interobserver and intraobserver reliability. The Modic grading score was positively correlated with intervertebral disc degeneration and negatively correlated with the intervertebral disc height.




Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Modic MT, Masaryk TJ, Ross JS et al (1988) Imaging of degenerative disk disease. Radiology 168:177–186. https://doi.org/10.1148/radiology.168.1.3289089
Modic MT, Steinberg PM, Ross JS et al (1988) Degenerative disk disease: assessment of changes in vertebral body marrow with MR imaging. Radiology 166:193–199. https://doi.org/10.1148/radiology.166.1.3336678
Jensen TS, Karppinen J, Sorensen JS et al (2008) Vertebral endplate signal changes (Modic change): a systematic literature review of prevalence and association with non-specific low back pain. Eur Spine J 17:1407–1422. https://doi.org/10.1007/s00586-008-0770-2. (Official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society)
Määttä JH, Wadge S, MacGregor A et al (2015) ISSLS prize winner: vertebral endplate (Modic) change is an independent risk factor for episodes of severe and disabling low back pain. Spine 40:1187–1193. https://doi.org/10.1097/brs.0000000000000937
Albert HB, Kjaer P, Jensen TS et al (2008) Modic changes, possible causes and relation to low back pain. Med Hypotheses 70:361–368. https://doi.org/10.1016/j.mehy.2007.05.014
Arana E, Kovacs FM, Royuela A et al (2011) Modic changes and associated features in Southern European chronic low back pain patients. Spine J 11:402–411. https://doi.org/10.1016/j.spinee.2011.03.019. (Official journal of the North American Spine Society)
Özcan-Ekşi EE, Yayla A, Orhun Ö et al (2021) Is the distribution pattern of Modic changes in vertebral end-plates associated with the severity of intervertebral disc degeneration?: A cross-sectional analysis of 527 Caucasians. World Neurosurg 150:e298–e304. https://doi.org/10.1016/j.wneu.2021.02.128
Albert HB, Briggs AM, Kent P et al (2011) The prevalence of MRI-defined spinal pathoanatomies and their association with modic changes in individuals seeking care for low back pain. Eur Spine J 20:1355–1362. https://doi.org/10.1007/s00586-011-1794-6. (Official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society)
Li Y, Wang B, Li H et al (2021) Adjuvant surgical decision-making system for lumbar intervertebral disc herniation after percutaneous endoscopic lumber discectomy: a retrospective nonlinear multiple logistic regression prediction model based on a large sample. Spine J 21:2035–2048. https://doi.org/10.1016/j.spinee.2021.07.012. (Official journal of the North American Spine Society)
Hao L, Li S, Liu J et al (2020) Recurrent disc herniation following percutaneous endoscopic lumbar discectomy preferentially occurs when Modic changes are present. J Orthop Surg Res 15:176. https://doi.org/10.1186/s13018-020-01695-6
Weishaupt D, Zanetti M, Hodler J et al (2001) Painful lumbar disk derangement: relevance of endplate abnormalities at MR imaging. Radiology 218:420–427. https://doi.org/10.1148/radiology.218.2.r01fe15420
Määttä JH, Karppinen JI, Luk KD et al (2015) Phenotype profiling of Modic changes of the lumbar spine and its association with other MRI phenotypes: a large-scale population-based study. Spine J 15:1933–1942. https://doi.org/10.1016/j.spinee.2015.06.056. (Official journal of the North American Spine Society)
Saukkonen J, Määttä J, Oura P et al (2020) Association between modic changes and low back pain in middle age: a northern finland birth cohort study. Spine 45:1360–1367. https://doi.org/10.1097/brs.0000000000003529
Udby PM, Samartzis D, Carreon LY et al (2022) A definition and clinical grading of Modic changes. J Orthop Res 40:301–307. https://doi.org/10.1002/jor.25240. (Official publication of the Orthopaedic Research Society)
Rajasekaran S, Venkatadass K, Naresh Babu J et al (2008) Pharmacological enhancement of disc diffusion and differentiation of healthy, ageing and degenerated discs: results from in-vivo serial post-contrast MRI studies in 365 human lumbar discs. Eur Spine J 17:626–643. https://doi.org/10.1007/s00586-008-0645-6. (Official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society)
Määttä JH, Rade M, Freidin MB et al (2018) Strong association between vertebral endplate defect and Modic change in the general population. Sci Rep 8:16630. https://doi.org/10.1038/s41598-018-34933-3
Sinha IP, Smyth RL, Williamson PR (2011) Using the Delphi technique to determine which outcomes to measure in clinical trials: recommendations for the future based on a systematic review of existing studies. PLoS Med 8:e1000393. https://doi.org/10.1371/journal.pmed.1000393
Pfirrmann CW, Metzdorf A, Zanetti M et al (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine 26:1873–1878. https://doi.org/10.1097/00007632-200109010-00011
Mysliwiec LW, Cholewicki J, Winkelpleck MD et al (2010) MSU classification for herniated lumbar discs on MRI: toward developing objective criteria for surgical selection. Eur Spine J 19:1087–1093. https://doi.org/10.1007/s00586-009-1274-4. (Official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society)
Kim KT, Park SW, Kim YB (2009) Disc height and segmental motion as risk factors for recurrent lumbar disc herniation. Spine 34:2674–2678. https://doi.org/10.1097/BRS.0b013e3181b4aaac
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Udby PM, Modic M, Elmose S et al (2022) The clinical significance of the Modic changes grading score. Glob Spine J. https://doi.org/10.1177/21925682221123012
Jensen TS, Sorensen JS, Kjaer P (2007) Intra- and interobserver reproducibility of vertebral endplate signal (Modic) changes in the lumbar spine: the Nordic Modic Consensus Group classification. Acta Radiol 48:748–754. https://doi.org/10.1080/02841850701422112
Jensen TS, Kjaer P, Korsholm L et al (2010) Predictors of new vertebral endplate signal (Modic) changes in the general population. Eur Spine J 19:129–135. https://doi.org/10.1007/s00586-009-1184-5. (Official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society)
Yang X, Karis DSA, Vleggeert-Lankamp CLA (2020) Association between Modic changes, disc degeneration, and neck pain in the cervical spine: a systematic review of literature. Spine J 20:754–764. https://doi.org/10.1016/j.spinee.2019.11.002. (Official journal of the North American Spine Society)
Salo J, Mackiewicz Z, Indahl A et al (2008) Plasmin-matrix metalloproteinase cascades in spinal response to an experimental disc lesion in pig. Spine 33:839–844. https://doi.org/10.1097/BRS.0b013e31816b1f1d
Adams MA, Freeman BJ, Morrison HP et al (2000) Mechanical initiation of intervertebral disc degeneration. Spine 25:1625–1636. https://doi.org/10.1097/00007632-200007010-00005
Wang Z, Tian Y, Li C et al (2022) Radiographic risk factors for degenerative lumbar spondylolisthesis: a comparison with healthy control subjects. Front Surg 9:956696. https://doi.org/10.3389/fsurg.2022.956696
Chen X, Sima S, Sandhu HS et al (2022) Radiographic evaluation of lumbar intervertebral disc height index: An intra and inter-rater agreement and reliability study. J Clin Neurosci 103:153–162. https://doi.org/10.1016/j.jocn.2022.07.018. (Official journal of the Neurosurgical Society of Australasia)
Teichtahl AJ, Urquhart DM, Wang Y et al (2016) Modic changes in the lumbar spine and their association with body composition, fat distribution and intervertebral disc height—a 3.0 T-MRI study. BMC Musculoskelet Disord 17:92. https://doi.org/10.1186/s12891-016-0934-x
Luoma K, Vehmas T, Kerttula L et al (2016) Chronic low back pain in relation to Modic changes, bony endplate lesions, and disc degeneration in a prospective MRI study. Eur Spine J 25:2873–2881. https://doi.org/10.1007/s00586-016-4715-x. (Official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society)
Brinjikji W, Diehn FE, Jarvik JG et al (2015) MRI findings of disc degeneration are more prevalent in adults with low back pain than in asymptomatic controls: a systematic review and meta-analysis. AJNR Am J Neuroradiol 36:2394–2399. https://doi.org/10.3174/ajnr.A4498
Lambrechts MJ, Brush P, Issa TZ et al (2022) Evaluating the Impact of Modic changes on operative treatment in the cervical and lumbar spine: a systematic review and meta-analysis. Int J Environ Res Public Health 19:10158. https://doi.org/10.3390/ijerph191610158
Modic MT (2007) Modic type 1 and type 2 changes. J Neurosurg Spine 6:150–151. https://doi.org/10.3171/spi.2007.6.2.150. (Discussion 151)
Hanımoğlu H, Çevik S, Yılmaz H et al (2019) Effects of Modic Type 1 changes in the vertebrae on low back pain. World Neurosurg 121:e426–e432. https://doi.org/10.1016/j.wneu.2018.09.132
Acknowledgements
Not applicable.
Funding
This work was supported in part by the National Nature Science Foundation (81874022 and 82172483 to Xinyu Liu; 82102522 to Lianlei Wang), Key R & D Project of Shandong Province (2022CXGC010503 to Xinyu Liu), Shandong Natural Science Foundation (ZR202102210113 to Lianlei Wang) and Shandong Province Taishan Scholar Project (tsqn202211317 to Lianlei Wang).
Author information
Authors and Affiliations
Contributions
HL, LYY, XLG is responsible for data collection, statistical analysis and writing the main manuscript text. LLW, SMY and YHT is responsible for statistical analysis and revising article. XYL proposed the concept and revised article finally. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Consent for publication
Not applicable.
Ethical approval
This study was approved by the ethics committee of Qilu Hospital of Shandong University [KYLL-2021(KS)-055]. All methods were carried out in accordance with relevant guidelines and regulations.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, H., Yu, L., Gao, X. et al. Novel Modic grading scoring system and its clinical validation: a preliminary investigation. Eur Spine J 33, 84–92 (2024). https://doi.org/10.1007/s00586-023-08003-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-08003-w