Abstract
Background context
Patients with multiple myeloma (MM) are at increased risk of infections and suffer from poor bone quality due to their disseminated malignant bone disease. Therefore, postoperative complications may occur following surgical treatment of MM lesions.
Purpose
In this study, we aimed to determine the incidence of postoperative complications and retreatments after spinal surgery in MM patients. Additionally, we sought to identify risk factors associated with complications and retreatments.
Study design
Retrospective cohort study.
Patient sample.
In total, 270 patients with MM who received surgical treatment for spinal involvement between 2008 and 2021 were included.
Outcome measures.
The incidence of perioperative complications within 6 weeks and reoperations within 2.5 years and individual odds ratios for factors associated with these complications and reoperations.
Methods
Data were collected through manual chart review. Hosmer and Lemeshow’s purposeful regression method was used to identify risk factors for complications and reoperations.
Results
The median age of our cohort was 65 years (SD = 10.8), and 58% were male (n = 57). Intraoperative complications were present in 24 patients (8.9%). The overall 6-week complication rate after surgery was 35% (n = 95). The following variables were independently associated with 6-week complications: higher Genant grading of a present vertebral fracture (OR 1.41; 95% CI 1.04–1.95; p = .031), receiving intramuscular or intravenous steroids within a week prior to surgery (OR 3.97; 95% CI 1.79–9.06; p = .001), decompression surgery without fusion (OR 6.53; 95% CI 1.30–36.86; p = .026), higher creatinine levels (OR 2.18; 95% CI 1.19–5.60; p = .014), and lower calcium levels (OR 0.58; 95% CI 0.37–0.88; p = .013). A secondary surgery was indicated for 53 patients (20%), of which 13 (4.8%) took place within two weeks after the initial surgery. We additionally discovered factors associated with retreatments, which are elucidated within the manuscript.
Conclusion
The goal of surgical treatment for MM bone disease is to enhance patient quality of life and reduce symptom burden. However, postoperative complication rates remain relatively high after spine surgery in patients with MM, likely attributable to both inherent characteristics of the disease and patient comorbidities. The risk for complications and secondary surgeries should be explored and a multidisciplinary approach is crucial.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multiple myeloma (MM) is the second most common hematological malignancy and arises from the antibody-producing plasma cells inside the bone marrow [1]. MM can occur in any part of the skeleton but typically affects the spine, ribs, skull, and pelvis. Pathological vertebral compression fractures (VCFs) are common in MM [2]. Approximately 30–60% of patients present with a VCF at the time of diagnosis, and over 60% of patients develop new VCFs later on [3]. VCFs can cause intractable back pain, reduced mobility, and spinal cord compression, potentially leading to rapid neurologic decline, thereby severely increasing the burden of disease [4].
MM patients are primarily treated with chemotherapy, stem cell transplantation, and immunomodulatory drugs under the supervision of a (hemato)oncologist. For some patients however, surgical intervention may be warranted [5]. Indications for surgery include gross spinal instability, compression of neural elements, and mechanical or neuropathic pain caused by an (impending) fracture or epidural tumor extension [6, 7]. Previous studies have shown that surgical intervention can improve patients’ neurologic function and quality of life [7, 8]. However, MM patients are at an increased risk of (postoperative) infections due to a multifactorial immunodeficiency caused by the disease itself and due to the treatment regimens [9]. Furthermore, they suffer from overall poor bone quality due to disseminated malignant bone disease. Specifically, the osteoclast differentiation promoted by monoclonal immunoglobulins can lead to weakening of bones and consequently a higher rate of pseudoarthrosis and hardware failure [10]. Therefore, it is critical to ensure that the benefits of surgical management outweigh the associated risks.
To date, little is known about the incidence of and predisposing factors for postoperative complications and retreatments after spinal surgery in MM. Therefore, in this study, we aimed to determine the incidence of postoperative complications within 6 weeks and the incidence of retreatments within 2.5 years after spinal surgery in MM patients. Additionally, we sought to identify factors associated with such complications and retreatments.
Method
Study design
This retrospective cohort study was approved by our institutional review board (registration number 2018P000688). The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines were used for adequate reporting [11].
Patient selection
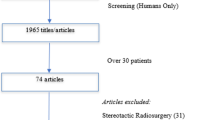
We identified 1,850 potentially eligible patients through the ICD-9 and ICD-10 codes for ‘Multiple Myeloma’ (203.0 and C90), and ‘Secondary malignant neoplasm of bone and bone marrow’ (198.5 and C79.5) or ‘Fracture of vertebrae’ (733.13, 805.0, 805.1, 805.2, M48.5, M84.5, S12.0, S22.0, and S32.0). We manually screened medical records on surgical treatment. The following inclusion criteria were applied: (1) adult patients with MM or plasmacytoma, (2) received spinal surgery for spinal MM-lesions between January 2010 and June 2021 in one of two tertiary academic medical centers that operate under a single umbrella institution. Patients were excluded if (1) no information was available, (2) if they had a history of another (major) malignant or neurologic disease for which they were treated, or (3) if they had prior surgery in the same area. Two-hundred-seventy patients met these criteria. A flowchart of selection can be found in the Appendix, Fig. 1.
Variables
Our outcome measures were (1) postoperative complication within 6 weeks after surgery, (2) retreatments within 2.5 years, and (3) risk factors associated with complications and retreatments expressed in individual odds ratios and subdistribution hazard ratios, respectively. The following baseline characteristics from patients’ medical records were extracted: age, gender, body mass index (BMI, in kg/m2), International Staging System (ISS) disease stage [12], age-adjusted Charlson comorbidity index (ACCI) [13], Eastern Cooperative Oncology Group (ECOG) performance status [14], back pain (yes/no), chemotherapy regimen, administration of perioperative steroids (minimum 6-10mg every 6–8 h intramuscular or intravenous within a week from surgery), treated area (cervical, thoracic, lumbar, sacral, or combined), and discharge disposition. Radiological variables were spread of myeloma disease (local: 1 affected vertebrae, multiple: 2–5 affected vertebrae, disseminated: widespread disease), Epidural Spinal Cord Compression (ESCC) scale [15], number of vertebral levels affected by the ESCC (≤ 2 or ≥ 3), highest Spinal Instability Neoplastic Score (SINS) score of treated area [16], number of vertebral fractures in the treated area, highest Genant fracture grading [17]. Surgical variables were type of surgery, estimated blood loss during surgery, duration of surgery, and intraoperative complications. Date of death was extracted from the charts (linked to the National Death Index), and for non-deceased patients, the last follow-up date was set on the date of their last hospital visit.
Surgical complications and retreatments
Postoperative complications were graded according to the Clavien-Dindo classification, which is based on the therapy used to treat or correct a specific complication [18]. Grade I complications were defined as any deviation from the normal postoperative course without the need for pharmacological treatment (with the exception of analgesics, antipyretics, diuretics, antiemetics, and electrolytes). Grade II complications were defined as postoperative deviations requiring any pharmacological treatment other than those allowed for grade I complications. Blood transfusions are also included in this grade. Grade III complications were defined as postoperative deviations requiring either surgical, endoscopic or radiological intervention. Grade IV complications were defined as life-threatening postoperative deviations warranting admission to the Intensive Care Unit. Grade V complications were defined as any postoperative deviations that led to the death of a patient [18]. We recorded all postoperative complications separately and additionally dichotomized complications into minor complications (Grade I or II) and major complications (Grade III, IV, or V). Intraoperative complications were also recorded but were not graded according to the Clavien-Dindo classification. Retreatments were defined as unplanned surgical interventions directly related to the initial surgery or unplanned radiation treatments to the operated area. Patients who died within 6 weeks from a cause that was unknown or presumably unrelated to the initial surgery or complications were excluded (n = 2).
Statistical analysis
Categorical variables were presented as count (%) and continuous data as median with interquartile ranges (IQR) as they were non-parametric after inspecting histograms. Baseline differences were assessed using Chi‐square tests or Fisher’s exact tests for categorical variables and Mann–Whitney U tests for continuous variables. Independent risk factors associated with postoperative complications were assessed using multivariable regression, and the Fine-Gray competing risk regression method was applied for retreatment analyses to address the situation where there is a competing risk of death within 2.5 years [19]. The purposeful selection approach described by Hosmer and Lemeshow was used to select variables of interest, where covariates are removed from the model if they are non-significant and not a confounder [20]. Factors with a p-value below 0.25 in bivariate analysis are entered in a multivariable regression model. Next, variables with a p-value below 0.10 in the multivariable model are entered into a new model together with variables that are considered clinically important. Then, other covariates are added back to the model one by one, to identify potential confounders that, by themselves, are not significantly related to the outcome but make an important contribution in the presence of other variables. A change in a parameter estimate above 20% indicates that the excluded variable was important in the sense of providing a needed adjustment for one or more of the variables remaining in the model [20]. The steps of this iterative process of deleting, refitting, and verifying are outlined in the Appendix, Tables 8, 9, and 10. Patients with missing values were excluded from the analysis; however, laboratory variables with more than 30% missing data were not included in the multivariable analyses due to the substantial loss of patients when retaining these factors (Alkaline Phosphatase 32.2%; Neutrophils 40.4%; Lymphocytes 33.3%; PTT 41.9%; PT 31.9%; INR 32.6%). Statistical analyses were performed with Python programming language, version 3.9.7 (Python Software Foundation, https://www.python.org/), and R statistical software version 4.1.0 (R Project for Statistical Computing) within RStudio statistical software version 1.4.1717. A two-tailed p-value of < 0.05 was considered significant.
Results
Baseline characteristics
Among 270 included patients, the mean age was 65 years (SD 10.8), and 157 (58%) were male (Table 1). Most patients had an ECOG score of 2 or lower (n = 235, 91%), and an ASIA impairment score E (n = 176, 66%). The median time from diagnosis to surgery was 57 months (IQR 0–438). Prior to surgery, 259 (96%) patients experienced back pain and 106 (41%) had neurologic symptoms. One hundred thirty-nine (57%) patients were started on chemotherapy prior to surgery, and 76 (29%) received perioperative steroids. The thoracic spine was the most commonly treated region (n = 133, 49%) and 88 patients had an ESCC grade of 3 (37%). One hundred seventy-three patients (71%) had a potentially unstable vertebra, and 59 had an unstable vertebra according to the SINS scoring system, warranting surgical consultation [16]. There were 196 fractures in our cohort, of which 133 (52%) were classified as severe. One hundred and thirty patients were treated with a vertebral augmentation (48%), 64 had a decompression with fusion (24%), 55 patients had a corpectomy with fusion (20%), and 21 had a posterior decompression without fusion (8%). Other surgical variables and laboratory data are displayed in the Appendix, Tables 6 and 7, respectively. Patients receiving less invasive surgeries (augmentations and decompression surgery without fusion) were, compared with patients receiving more invasive procedures, generally older at the time of surgery (67 vs 64 years, p = 0.061), in a higher ISS disease stage (30% ISS 3 vs 11% ISS 3, p < 0.001), more patients with ECOG scores 3 and 4 (12% vs 5.5%, p = 0.064) and had their diagnosis of MM for a longer period of time (median 12 vs 137 days, p = 0.006). The 5-year survival was 43.0% (95%CI 36.4%–50.8%).
Surgical complications
Intra-operative complications were present in 25 patients (9.7%), which were mostly related to excessive blood loss of more than 3 L (40% of all intraoperative complications). Ninety-four patients (35%) suffered from at least one postoperative complication within 6 weeks, of which 47 (50%) had a major complication (Table 2). Fifty-four patients (20%) had a single postoperative complication, whereas 41 patients (15%) experienced two or more complications. Most postoperative complications were grade II, which means they required a pharmacological treatment (other than analgesics, antipyretics, diuretics, antiemetics, and electrolytes) or blood transfusion (n = 97, 58%). Twenty-three complications (14%) required a surgical or radiological intervention (grade III), 31 patients (19%) had a life-threatening complication (grade IV) and 5 (3.0%) died as a consequence of their complication (grade V). Postoperative systemic infections (pneumonia, urinary tract infection, or bacteriemia/sepsis) (n = 43, 19%) were the most common complication type. Thromboembolic complications occurred in 10 patients (3.7%). Median survival time was 37 months (95%CI 19–64) for patients who had a postoperative complication and 68 months (95%CI 48–120) for patients without complications. Table 2 shows the differences in complication rates for patients treated with vertebral augmentation versus invasive surgery. Patients treated with vertebral augmentation suffered more from (new or persisting) pain within six weeks (9.2% vs. 2.9%, p = 0.037). Patients treated with invasive surgery suffered more from wound infections (0.8% vs. 7.9%, p = 0.006). There were also more life-threatening complications in the invasive surgery group (6.9% vs. 15.7%, p = 0.024).
In basic comparative analyses, patients with postoperative complications had at baseline, compared to patients without complications, higher age, worse ECOG performance score, worse ASIA impairment score, lower SINS scores, and more often received intravenous or intramuscular steroids prior to surgery (all p < 0.05; Table 1). In multivariable analyses, four variables remained independently associated with postoperative complications after full adjustment for potential confounders: Genant grading of a present vertebral fracture (OR 1.41; 95% CI 1.04–1.95; p = 0.031), receiving steroids prior to surgery (OR 3.97; 95% CI 1.79–9.06; p = 0.001), decompression surgery without fusion (OR 6.53; 95%CI 1.30–36.86; p = 0.026), creatinine levels (OR 2.18; 95%CI 1.19–5.60; p = 0.014), and calcium levels (OR 0.58; 95%CI 0.37–0.88; p = 0.013; Table 4). The following variables were identified as potential confounding factors: age, time from MM diagnosis to surgery, ECOG score, and the number of levels operated.
Retreatments
Fifty-three patients (20%) had at least one reoperation within 2.5 years after the initial surgery (Table 3). The most common indications for reoperation were adjacent-level fractures (ALF) (n = 28, 53%), wound dehiscence and/or infected hardware (n = 10, 19%), and tumor recurrence or spinal cord compression at the operated region (n = 4, 7.5%). The most common types of re-interventions were spinal augmentation (n = 27, 51%), removal and re-implantation of hardware (n = 9, 17%), and interventions to fight infection (n = 8, 15%). Aside from reoperations, 25 patients (9.3%) underwent unplanned radiation treatment after the initial surgery. Most of the radiation treatments were indicated because of severe pain (n = 12, 48%) (Table 4).
Factors independently affecting the rate of revision surgery or unplanned radiation treatments to the operated area within 2.5 years were: ECOG performance score (Subdistribution Hazard Ratio (SHR) 1.39; 95%CI 1.03–1.88, p = 0.031), preoperative radiotherapy (SHR 0.28; 95%CI 0.11–0.71; p = 0.007), corpectomy with fusion surgery (SHR 0.16; 95%CI 0.04–0.72; p = 0.017), decompression with fusion surgery (SHR 0.22, 95%CI 0.05–0.93, p = 0.039), and number of levels operated on (SHR 1.57; 95%CI 1.03–2.38; p = 0.037; Table 5). Variables identified as potential confounding factors were: age and treated spine segment. Surgery type and disease spread were retained because of assumed clinical relevance.
Discussion
Clinical management of MM patients with spinal involvement remains challenging due to a lack of clear treatment guidelines. Patients with MM are more susceptible to postoperative complications as compared to other spinal metastases, due to their immunodeficient state, disseminated bone disease, and diminished bone healing [9, 10]. This study describes a series of spinal procedures in 270 patients with MM and shows that 35% of patients suffered from postoperative complications within 6 weeks after surgery and 20% of patients received unplanned additional surgical/radiotherapy treatment. As expected, due to the inherent characteristics of the disease, this is slightly higher than complication rates found in patients undergoing surgery for spinal metastases originating from solid tumors, where reported rates vary between 17 and 32% [21,22,23]. Furthermore, risk factors were identified for both postoperative complications and retreatments that can assist in improving patient-centered treatment strategies in a multidisciplinary approach.
MM causes hypogammaglobulinemia, T-cell dysfunction, and granulocytopenia, which results in a higher risk of infectious complications [9], [24]. This reflects in our cohort as the most common complication was related to infection (either systemic or wound infection). Additionally, patients with MM are specifically more at risk for thromboembolic complications compared to the general population since MM results in a hypercoagulable state [24]. Our results show that 11% of patients with a complication had a thromboembolic complication. Furthermore, it has been well established that preoperative high-dose steroid therapy is associated with an increased risk of postoperative complications. Patients receiving steroids perioperatively are especially vulnerable to infectious complications such as surgical site infections, wound dehiscence, and pneumonia [25, 26]. It has been shown that patients receiving steroids were more than twice as likely to experience pulmonary embolism [27], and have an almost fourfold higher mortality risk [28]. Our results underscore these findings, as the administration of steroids was strongly associated with postoperative complications. Since steroids play an integral role in the treatment of MM, it is important that patients are counseled preoperatively about the higher likelihood of complications. Consideration of perioperative infection mitigation strategies and/or antithrombotic prophylaxis is essential. Postoperative monitoring of patients should be done with extra vigilance.
In contrast to common expectations, our data showed that more patients treated with vertebral augmentation reported severe pain within the first six weeks postoperatively when compared to those who underwent invasive surgery. One might anticipate that the more invasive procedures would result in more pain. However, this was not reflected in our findings. The explanation for this counterintuitive result may lie in the nature of the procedures themselves. While cement augmentation will often address the fracture pain itself, residual discomfort could persist due to unresolved mechanical stresses and global spinal imbalances [29]. Our findings suggest that the etiology of pain in these patients is complex and likely multifactorial, extending beyond the fracture itself. Therefore, to effectively manage pain, some patients may require a more comprehensive approach that includes spinal instrumentation. Vertebral augmentation plays a vital role in managing MM patients with spinal involvement, but our results highlight the importance of a tailored treatment approach that considers each patient's individual needs and circumstances.
Several laboratory values seemed to play an important role in both complication risk analysis and retreatment risk analysis. Elevated serum creatinine levels before surgery have been associated with increased complication rates and are often attributed to muscle wasting or poor nutritional status [30]. Elevated serum creatinine levels are also indicative of active myeloma disease and renal failure, which is a common complication in MM and has a strong impact on both morbidity and mortality [31, 32]. Also in this study, elevated creatinine levels are strongly associated with postoperative complications. Therefore, it is important to be alert to the increased complication risk when a patient with elevated creatinine levels or advanced disease stage is indicated for surgery.
Adjacent-level fractures were the most common reason for revision surgery. These fractures occurring after augmentation procedures or long spinal segment instrumentation have been discussed in the literature for patients with MM, osteoporosis, or after scoliosis surgery [33,34,35,36]. The procedures fuse the target segments and thereby cause increased stress on the adjacent vertebrae. Specifically, patients with decreased bone density (i.e., patients with MM with widespread bone destruction), have an increased risk of adjacent-level fractures after surgery [36]. Caution is warranted when patients with widespread MM are indicated for surgical intervention. Measures to prevent these fractures, like augmentation of the first mobile vertebra or establishing less rigid constructs can help to prevent these in multilevel fusion surgeries [37], [38], and could be considered in myeloma surgery as well.
Decompression surgery without fusion was found to be a risk factor for postoperative complications. This is in contrast to previous literature, showing that the incidence of complications is lower after decompression surgery when compared to spinal fusion surgery [39, 40]. The use of spinal instrumentation requires more extensive tissue disruption and often results in prolonged surgical time and increased blood loss [26]. Many studies have proven that both surgical time and blood loss are correlated with a higher risk of perioperative complications [41, 42]. We assume that our findings are a result of a selection bias where surgeons deliberately chose not to perform invasive spinal fusions on sicker patients, as they were already at a higher risk of developing complications. It is worth noting that the different types of surgical intervention, be it vertebral augmentation or open surgery, may have different complication profiles. We aimed to account for this in our regression analysis by including the type of surgery as a covariate. While it is plausible that separate analyses for each surgical type might provide more specific insights, such an approach would substantially reduce our sample size for each group, limiting our ability to analyze all variables of interest comprehensively. We aimed to offer a clearer understanding of the unique risks associated with each procedure by separating them in the provided table. The same goes for the seemingly protective effect of doing a corpectomy for retreatment risk. When a patient was in a good condition and therefore selected for a more invasive surgical approach, they may have been less likely to experience problems postoperatively because of their general fitness level before surgery. From the results, we can see that patients who were in a worse disease stage and had their MM diagnosis for a longer period of time were generally treated with less invasive surgeries like augmentations and decompression surgery without fusion. This is also reflected by the effect of elevated calcium levels. Similar to elevated creatinine levels, high calcium levels are an indicator of further disease progression in MM. In later stages of the disease, induction of osteoclasts causes bone destruction which in turn leads to hypercalcemia. Hypercalcemia is a sign of further disease progression and is associated with renal failure, anemia, and poor survival [43]. It is present in 30% of MM patients at the time of diagnosis [44]. It is expected that patients with elevated calcium levels would experience more complications. However in our study, the opposite was true. We interpret this as a reflection of the selection bias for less invasive treatments rather than a reflection of the true effect of elevated calcium levels.
Limitations
Our study had several limitations. Firstly, due to the retrospective nature of the study, complications were assessed by screening discharge summaries and postoperative visit notes. Minor complications (Clavien-Dindo grade 1 and 2) might not have always been reported in such notes. It is also possible that some complications and reoperations were treated in other facilities and did not end up in our institution’s medical records. This might have led to an underestimation of true complication and retreatment rates. Furthermore, because of the retrospective design, when a revision surgery was done 2 years from the initial surgery, it was difficult to distinguish whether this was done because of (instrument) failure or disease progression if there was no evident myelomatous disease in that vertebra initially. Second, the retrospective design of our study might have introduced some selection bias. The choice to operate on a patient and the subsequent type of surgery depended on the surgical indication and on the surgeon and we did not document the indications that led to these decisions. As mentioned before, surgeons may have chosen to only perform highly invasive surgery such as corpectomy on the healthiest patients and refrained from implanting hardware in the sickest patients. Third, certain variables in our analysis were subjective in nature (such as ECOG performance status) and are subject to interobserver variability. Fourth, we decided to exclude patients with missing values from analysis, which might also have introduced selection bias. Additionally, to assess individually associated factors with retreatments, the Fine-Gray model was used. We chose the Fine-Gray model since it refers to the pattern of actually performed retreatments and not to the retreatment risk that could be expected for a patient living long enough. It does not censor deaths but treats death as a competing risk [45]. However, caution should be taken with the interpretation of the documented SHR. The SHR can be interpreted in a similar manner to an HR from a Cox regression, but an SHR accounted for the risk of death. This means that an SHR is often smaller than a Cox HR, since part of the cohort already died before they could have a retreatment [45]. To overcome this, we also provided the Cox Regression HRs for easier interpretation and to allow comparison of results across different studies. Despite the abovementioned limitations, considering the fact that we analyzed one of the biggest surgical MM cohorts, we believe that these results provide valuable knowledge for postoperative risk assessment in patients with MM facing a spinal intervention. Furthermore, we believe that this work will raise surgeons' awareness of the relatively high risk of postoperative complications and retreatments of MM patients. This awareness can help them better plan patient care and co-manage patients with internal medicine specialists for better outcomes.
Conclusion
The goal of surgical treatment for MM bone disease is to enhance patient quality of life, spinal stability, and relieve symptoms. However, postoperative complication rates remain high after spine surgery in patients with MM. We found an overall complication rate of 35% and a retreatment rate of 20% which might still be an underestimation. These relatively high rates are likely attributable to the inherent characteristics of the disease. The risk factors identified that are associated with complication and retreatment can assist future efforts for improving patient-centered treatment strategies in a multidisciplinary approach. Patient risk for complications and subsequent surgery should be explored, and multidisciplinary therapy including other medical disciplines is crucial to mitigate these risks.
References
Rajkumar SV, Palumbo A (2007) Management of newly diagnosed Myeloma. Hematol Oncol Clin North Am 21(6):1141–1156. https://doi.org/10.1016/j.hoc.2007.08.008
Kyle RA, Therneau TM, Rajkumar SV, Larson DR, Plevak MF, Melton LJ (2004) Incidence of multiple myeloma in Olmsted County, Minnesota: Trend over 6 decades. Cancer 101(11):2667–2674. https://doi.org/10.1002/cncr.20652
Zijlstra H, Wolterbeek N, Drost RW et al (2020) Identifying predictive factors for vertebral collapse fractures in multiple myeloma patients. Spine J 20(11):1832–1839. https://doi.org/10.1016/j.spinee.2020.07.004
Kiely F, Cran A, Finnerty D, O’Brien T (2017) Self-reported quality of life and symptom burden in ambulatory patients with multiple myeloma on disease-modifying treatment. Am J Hosp Palliat Med 34(7):671–676. https://doi.org/10.1177/1049909116646337
Terpos E, Zamagni E, Lentzsch S et al (2021) Treatment of multiple myeloma-related bone disease: recommendations from the Bone Working Group of the International Myeloma working group. Lancet Oncol 22(3):e119–e130. https://doi.org/10.1016/S1470-2045(20)30559-3
Rasch S, Lund T, Asmussen JT et al (2020) Multiple myeloma associated bone disease. Cancers (Basel) 12(8):1–19. https://doi.org/10.3390/cancers12082113
Zadnik PL, Goodwin CR, Karami KJ et al (2015) Outcomes following surgical intervention for impending and gross instability caused by multiple myeloma in the spinal column. J Neurosurg Spine 22(3):301–309. https://doi.org/10.3171/2014.9.SPINE14554
Milavec H, Ravikumar N, Syn NL, Soekojo CY, Chng WJ, Kumar N (2020) Surgical management of multiple myeloma with symptomatic involvement of the spine. Int J Spine Surg 14(5):785–794. https://doi.org/10.14444/7112
Schütt P, Brandhorst D, Stellberg W et al (2006) Immune parameters in multiple myeloma patients: influence of treatment and correlation with opportunistic infections. Leuk Lymphoma 47(8):1570–1582. https://doi.org/10.1080/10428190500472503
Guzik G (2017) Oncological and functional results of the surgical treatment of vertebral metastases in patients with multiple myeloma. BMC Surg 17(1):92–100. https://doi.org/10.1186/s12893-017-0288-9
STROBE - Strengthening the reporting of observational studies in epidemiology. Accessed November 21, 2022. https://www.strobe-statement.org/
Greipp PR, Miguel JS, Dune BGM et al (2005) International staging system for multiple myeloma. J Clin Oncol 23(15):3412–3420. https://doi.org/10.1200/JCO.2005.04.242
Qu WF, Zhou PY, Liu WR et al (2020) Age-adjusted Charlson Comorbidity Index predicts survival in intrahepatic cholangiocarcinoma patients after curative resection. Ann Transl Med 8(7):487–487. https://doi.org/10.21037/ATM.2020.03.23
Oken MM, Creech RH, Tormey DC et al (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5(6):649–656
Bilsky MH, Laufer I, Fourney DR et al (2010) Reliability analysis of the epidural spinal cord compression scale: clinical article. J Neurosurg Spine 13(3):324–328. https://doi.org/10.3171/2010.3.SPINE09459
Fisher CG, DiPaola CP, Ryken TC et al (2010) A novel classification system for spinal instability in neoplastic disease: an evidence-based approach and expert consensus from the Spine Oncology Study Group. Spine (Phila Pa 1976) 35(22):E1221–E1229
Genant HK, Wu CY, van Kuijk C, Nevitt MC (1993) Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 8(9):1137–1148. https://doi.org/10.1002/JBMR.5650080915
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213. https://doi.org/10.1097/01.SLA.0000133083.54934.AE
Fine JP, Gray RJ (1999) A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc 94(446):496–509. https://doi.org/10.1080/01621459.1999.10474144
DW. Hosmer, S Lemeshow, RX (2013) Sturdivant. Model-building strategies and methods for logistic regression. In: Applied Logistic Regression. 3rd ed. Wiley
Paulino Pereira NR, Ogink PT, Groot OQ et al (2019) Complications and reoperations after surgery for 647 patients with spine metastatic disease. Spine J 19(1):144–156. https://doi.org/10.1016/j.spinee.2018.05.037
Lee BH, Park JO, Kim HS, Park YC, Lee HM, Moon SH (2014) Perioperative complication and surgical outcome in patients with spine metastases: retrospective 200-case series in a single institute. Clin Neurol Neurosurg 122:80–86. https://doi.org/10.1016/j.clineuro.2014.04.025
Luksanapruksa P, Buchowski JM, Zebala LP, Kepler CK, Singhatanadgige W, Bumpass DB (2017) Perioperative complications of spinal metastases surgery. Clin Spine Surg; 30(1). www.clinicalspinesurgery.com
Fotiou D, Dimopoulos MA, Kastritis E (2022) Approach to contemporary risk assessment, prevention and management of thrombotic complications in multiple Myeloma. Cancers (Basel) 14(24):6216. https://doi.org/10.3390/CANCERS14246216
Kittle H, Ormseth A, Patetta MJ, Sood A, Gonzalez MH (2020) Chronic corticosteroid use as a risk factor for perioperative complications in patients undergoing total joint arthroplasty. J Am Acad Orthop Surg Glob Res Rev. https://doi.org/10.5435/JAAOSGlobal-D-20-00001
Tihista M, Gu A, Wei C, Weinreb JH, Rao RD (2020) The impact of long-term corticosteroid use on acute postoperative complications following lumbar decompression surgery. J Clin Orthop Trauma 11(5):921–927. https://doi.org/10.1016/j.jcot.2020.04.010
Ranson WA, White SJW, Cheung ZB et al (2018) The effects of chronic preoperative steroid therapy on perioperative complications following elective posterior lumbar fusion. Global Spine J 8(8):834–841. https://doi.org/10.1177/2192568218775960
Ismael H, Horst M, Farooq M, Jordon J, Patton JH, Rubinfeld IS (2011) Adverse effects of preoperative steroid use on surgical outcomes. Am J Surg 201(3):305–309. https://doi.org/10.1016/j.amjsurg.2010.09.018
Robinson Y, Heyde CE, Försth P, Olerud C (2011) Kyphoplasty in osteoporotic vertebral compression fractures—guidelines and technical considerations. J Orthop Surg Res 6(1):1–8. https://doi.org/10.1186/1749-799X-6-43/TABLES/2
O’Brien MM, Gonzales R, Shroyer AL et al (2002) Modest serum creatinine elevation affects adverse outcome after general surgery. Kidney Int 62(2):585–592. https://doi.org/10.1046/J.1523-1755.2002.00486.X
Eleutherakis-Papaiakovou V, Bamias A, Gika D et al (2007) Renal failure in multiple myeloma: incidence, correlations, and prognostic significance. Leuk Lymphoma 48(2):337–341. https://doi.org/10.1080/10428190601126602
Corso A, Zappasodi P, Pascutto C et al (2003) Urinary proteins in multiple myeloma: correlation with clinical parameters and diagnostic implications. Ann Hematol 82(8):487–491. https://doi.org/10.1007/S00277-003-0699-9
Aboud N, Eckardt N, Kamp MA, Senft C, Schwarz F (2022) Occurrence of adjacent segment fractures after surgical treatment of an osteoporotic vertebral fracture: a retrospective comparison between two different treatment methods. Arch Orthop Trauma Surg 1:1–7. https://doi.org/10.1007/S00402-022-04434-0/TABLES/1
Astolfi S, Scaramuzzo L, Logroscino CA (2009) A minimally invasive surgical treatment possibility of osteolytic vertebral collapse in multiple myeloma. Eur Spine J 18(Suppl 1):115. https://doi.org/10.1007/S00586-009-0977-X
Granville M, Berti A, Jacobson RE (2017) Vertebral compression fractures after lumbar instrumentation. Cureus. https://doi.org/10.7759/CUREUS.1729
Schwarz F, Burckhart M, McLean AL, Kalff R, Waschke A (2018) Risk factors for adjacent fractures after cement-augmented thoracolumbar pedicle screw instrumentation. Int J Spine Surg 12(5):565. https://doi.org/10.14444/5069
Ghobrial GM, Eichberg DG, Kolcun JPG et al (2017) Prophylactic vertebral cement augmentation at the uppermost instrumented vertebra and rostral adjacent vertebra for the prevention of proximal junctional kyphosis and failure following long-segment fusion for adult spinal deformity. Spine J 17(10):1499–1505. https://doi.org/10.1016/J.SPINEE.2017.05.015
Lattig F (2009) Bone cement augmentation in the prevention of adjacent segment failure after multilevel adult deformity fusion. J Spinal Disord Tech 22(6):439–443. https://doi.org/10.1097/BSD.0B013E31818D6493
Inose H, Kato T, Yuasa M, et al (2018) Comparison of decompression, decompression plus fusion, and decompression plus stabilization for degenerative spondylolisthesis a prospective, randomized study. Clin Spine Surg; 31(7):347–352. www.clinicalspinesurgery.com
Austevoll IM, Gjestad R, Solberg T et al (2020) Comparative effectiveness of microdecompression alone vs decompression plus instrumented fusion in lumbar degenerative spondylolisthesis. JAMA Netw Open. https://doi.org/10.1001/jamanetworkopen.2020.15015
Hu SS (2004) Blood loss in adult spinal surgery. Eur Spine J. https://doi.org/10.1007/s00586-004-0753-x
Tang H, Zhu J, Ji F, Wang S, Xie Y, Fei H (2014) Risk factors for postoperative complication after spinal fusion and instrumentation in degenerative lumbar scoliosis patients. J Orthop Surg Res. https://doi.org/10.1186/1749-799X-9-15
Bao L, Wang Y, Lu M et al (2020) Hypercalcemia caused by humoral effects and bone damage indicate poor outcomes in newly diagnosed multiple myeloma patients. Cancer Med 9(23):8962–8969. https://doi.org/10.1002/cam4.3594
Buege MJ, Do B, Lee HC et al (2019) Corrected calcium versus ionized calcium measurements for identifying hypercalcemia in patients with multiple myeloma. Cancer Treat Res Commun. https://doi.org/10.1016/j.ctarc.2019.100159
Szychowski JM, Roth DL, Clay OJ, Mittelman MS (2010) Patient death as a censoring event or competing risk event in models of nursing home placement. Stat Med 29(3):371. https://doi.org/10.1002/SIM.3797
Author information
Authors and Affiliations
Contributions
All authors were involved in the design. HZ and RP performed the data extraction. HZ performed the data analysis. All authors reviewed and edited the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Each author certifies that he or she has no commercial associations (e.g. consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article.
Ethical approval
Investigation performed at Massachusetts General Hospital, Boston USA. Local Institutional Review Board (IRB) approval was obtained for this study (registration number 2018P000688).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
See Fig. 1.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zijlstra, H., Pierik, R.J., Crawford, A.M. et al. Analysis of complications and revisions after spine surgery in 270 multiple myeloma patients with spinal involvement. Eur Spine J 32, 4335–4354 (2023). https://doi.org/10.1007/s00586-023-07903-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07903-1