Abstract
Introduction
While the effects of VBT on coronal parameters have been investigated in various studies, this has not yet been the case for sagittal parameters. This is of particular relevance considering that VBT does not allow direct correction of the sagittal profile. Thus, we investigated the effects of VBT on sagittal parameters in patients with adolescent idiopathic scoliosis.
Materials and methods
Retrospective, 2-Center study. Patients who underwent VBT and presented a 2-years follow-up were included. The differences in sagittal parameters were evaluated, along with modifications of sagittal profile following Abelin-Genevois’ classification.
Results
Data from 86 patients were obtained. Mean Cobb angle was 52.4 ± 13.9° at thoracic level and 47.6 ± 14.3° at lumbar level before surgery, and 28.5 ± 13.6 and 26.6 ± 12.7° at the 2-year follow-up, respectively. Mean thoracic kyphosis increased from 28.3 ± 13.8 to 33 ± 13°, the lumbar lordosis (LL) was unvaried (from 47.5 ± 13.1 to 48.4 ± 13.5°), PT decreased from 9.4 ± 8.5 to 7.4 ± 6.1°, the sagittal vertical axis SVA decreased from 4.5 ± 31.4 to − 3.6 ± 27.9 mm. No kyphotic effect on LL in patients who underwent lumbar instrumentation was observed. Before surgery, 39 patients had a type 1 sagittal profile, 18 were type 2a, 14 type 2b and 15 type 3. Postoperatively, 54 were type 1, 8 were 2a, 13 were 2b and 11 were type 3.
Conclusions
VBT positively influences sagittal parameters and does not have a kyphotic effect on LL.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vertebral Body Tethering (VBT) is currently being investigated as a new option for the treatment of Adolescent Idiopathic Scoliosis (AIS): while published results are promising, the research aiming to identify the ideal candidate for this technique is still ongoing [1,2,3,4,5,6,7,8,9,10,11,12]. Scoliosis is a three-dimensional deformity caused by a lengthening of the anterior column in comparison to the posterior elements [13, 14]. The deformity induced by scoliosis in the coronal plane has been widely studied and classified, with the Lenke classification representing the gold standard for both classification and surgical planning in patients with AIS [15, 16]. The Lenke classification included modifiers to describe the sagittal profile of scoliotic curves, but this description translated into only limited guidelines for surgical planning from a sagittal point of view. It is acknowledged that sagittal balance has a strong correlation with health-related quality of life (HRQoL) in adult patients [17]. Even if less information is available regarding the effect of sagittal alignment after AIS surgery on HRQoL during the adult life, taking this aspect into consideration in the surgical strategy when planning AIS correction seems reasonable. As showed by Abelin-Genevois and colleagues, only 44% of patients with AIS present a physiological sagittal profile with three alternating curves (cervical lordosis, thoracic kyphosis and lumbar lordosis) and are defined as type 1 in their classification [18]. Of the remaining AIS patients, type 2 present hypokyphosis, sometimes in conjunction with kyphosis of the thoracolumbar junction (2b) and type 3 show a proximal cervicothoracic kyphosis with a long thoracolumbar lordosis [18]. While it is established that posterior fusion and the use of osteotomies allow reconstruction of the physiological sagittal profile in these patients [18], there are only very limited data regarding the effect of VBT on sagittal parameters [10]. In particular, the role of VBT on the overall sagittal alignment has not yet been investigated. Furthermore, despite offering promising advantages in comparison to fusion, as it does not limit spine mobility [19], lumbar tethering is not performed by many surgeons as an anterior instrumentation may potentially have a kyphotic effect on the lumbar spine. To the best of our knowledge, there is no published data regarding the role of lumbar VBT in respect to sagittal parameters. The authors of the present study retrospectively analyzed and compared the sagittal profile of patients undergoing VBT before surgery and at the 2-year follow-up. The aim of this study was to investigate the effect of VBT on sagittal profile and to rule out a negative effect of VBT on sagittal alignment.
Materials and methods
Patient recruitment
The present study was conducted according to the Strengthening the Reporting of Observational Studies in Epidemiology: the STROBE Statement [20]. A retrospective analysis was performed, of all consecutive, skeletally immature patients (Risser ≤ 4 and/or Sanders ≤ 7) who underwent single or bilateral VBT for AIS at two different institutions (Eifelklinik St. Brigida in Simmerath, Germany and Grenoble Alps Scoliosis Center in Grenoble, France) between June 2017 and July 2019, and for whom a 2-year follow-up was available. All X-rays were obtained following a standard protocol to allow comparison of the films. While curve magnitude is not considered an exclusion criterion for VBT, the authors perform this technique only in flexible curves correcting to ≤ 30° on bending X-rays. Patients reporting radiculopathy or neurological deficit at clinical examination are also not eligible for VBT. Exclusion criteria for the present study were previous spine surgery, incomplete perioperative documentation and incomplete X-rays at follow-up (e.g., isolated thoracic or lumbar X-ray, missing lateral projection, low quality of imaging). The ethics committee of the University of Aachen approved this study (EK 130/19).
Surgical technique
After general anesthesia performed with a double-lumen tube, patients were positioned in strict lateral decubitus with the convex side of the curve facing upwards. Thoracic curves down to L1 were approached with a video-assisted thoracic surgery (VATS), with one or two intercostal incisions, about 6 cm each, and one or two thoracoscopic portals. Lumbar instrumentations were performed via a mini-retroperitoneal approach. Bilateral surgeries were performed in one stage, with the lumbar curve instrumented first as, in the authors’ opinion, this step is the more physically and mentally demanding one [21].
Outcomes of interest
In order to analyze the influence of VBT on sagittal alignment, the following parameters were measured on standing X-rays before surgery and at the 2-year follow-up: thoracic kyphosis (TK, T1-T12), lumbar lordosis (LL, L1-S1), pelvic tilt (PT), pelvic incidence (PI), and sagittal vertical axis (SVA). The type of sagittal profile (1, 2a, 2b or 3) was assessed for every subject before surgery and at the last follow-up, following the classification of sagittal profile for AIS patient developed by Abelin-Genevois and colleagues [18].
Statistical analysis
For the statistical analysis, we referred to IBM SPSS software. A two-tailed, paired T Test was performed to compare the observed sagittal parameters before surgery and at the last follow-up (TK, LL, PT and SVA). The parameters were expressed as mean ± standard deviation and the confidence interval was set at 95% for all comparisons. Patients were divided into four subgroups according to the sagittal profile and comparisons between the subgroups before and after surgery were performed as percentages. Sub-analysis of LL in patients who underwent lumbar instrumentation was also performed.
Results
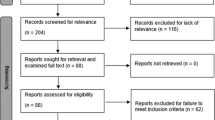
During the observation period, unilateral or bilateral VBT was performed on 97 consecutive, skeletally immature patients. Eleven patients were excluded because of incomplete series of X-rays at the last follow-up. Thus, the data from 86 patients were available for this analysis.
Demographic and perioperative data
Of the 86 considered patients, 72 (84%) were female and 14 (16%) were male. The mean age at surgery was 13.2 ± 2.4 years. Thirty-six patients were Risser 0 (42%), seven were Risser 1 (8%), four were Risser 2 (5%), 19 were Risser 3 (22%) and 20 were Risser 4 (23%).
Fifty-four patients underwent unilateral VBT (45 thoracic and nine lumbar instrumentations) and 32 underwent bilateral VBT. On average, 8.5 ± 1.8 levels were instrumented. The mean estimated blood loss was 318.3 ± 163.4 ml (Estimated blood volume 7%, range 2.5–25%), with only one patient receiving a cell salvage transfusion. The mean length of surgery was 258.3 ± 67.8 min; the mean inpatient stay was 8.0 ± 1.3 days.
Six postoperative complications were observed: five recurrent pleural effusion after bilateral VBT and one case of psoas irritation through the head of the L4 screw. The latter patient underwent revision surgery to remove the screw in L4, after which symptoms resolved without affecting curve correction.
A summary of demographic and perioperative data is presented in Table 1.
Radiographic data
Before surgery, the mean Cobb angle measured 52.4 ± 13.9° at thoracic level and 47.6 ± 14.3° at lumbar level. At the 2-year follow-up, the mean thoracic Cobb angle measured 28.5 ± 13.6° (P < 0.0001) and the mean lumbar Cobb angle measured 26.6 ± 12.7° (P < 0.0001). No overcorrections were observed in this cohort, but 5 patients required revision (re-tethering) for loss of correction and/or add on scoliosis after tether rupture.
Regarding sagittal parameters, the mean PI measured 49.8 ± 11.3°. The mean TK increased from 28.3 ± 13.8 to 33 ± 13° at the last follow-up (P < 0.0001). LL remained stable from 47.5 ± 13.1 to 48.4 ± 13.5° (P = 0.3). Also in the cohort of patients who underwent lumbar instrumentation (41 patients, nine lumbar and 32 bilateral instrumentations), LL remained stable from 48.9 ± 13.9 to 49.1 ± 16.3° (P = 0.8). SVA decreased from 4.5 ± 31.4 to − 3.6 ± 27.9 mm (P = 0.2). PT decreased from 9.4 ± 8.5 to 7.4 ± 6.1° (P = 0.06).
Performing a sub-analysis of sagittal parameters of patients who maintained a non-physiological sagittal profile after VBT (postoperative type 2a, 2b and 3), also in this restricted cohort an increase in TK (from 22 ± 14.1 to 26.8 ± 14.6°, P = 0.03) was observed, while LL remained stable (from 45.3 ± 10.8 to 47 ± 12.1°, P = 0.3).
Results of the radiological parameters are summarized in Table 2. No kyphotic effect on LL in patients who underwent lumbar instrumentation was observed.
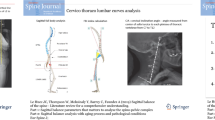
According to the classification proposed by Abelin-Genevois [18], before surgery 39 patients were type 1 (45%), 18 were type 2a (21%), 14 were type 2b (17%) and 15 were type 3 (17%). At the last available follow-up, all patients that before surgery were type 1 retained the same, physiologic sagittal profile. Fifteen patients who did not have a physiologic profile before surgery were type 1 after VBT (overall 54 patients, 63%). Most type 2b and 3 patients maintained the preoperative profile after VBT, while type 2a patients had a more variable behavior. A summary of the sagittal profile before and after VBT is shown in Table 3. A clinical example is presented in Fig. 1.
Discussion
The main finding of this study is that, despite not allowing direct correction on the sagittal plane, VBT positively influences sagittal parameters. Thoracic kyphosis was significantly increased and lumbar lordosis was maintained for the curves treated. The overall sagittal alignment was very predictable for type 1, 2b and 3 patients, while 2a patients showed a more variable behavior. Of note, the majority of patients had a physiologic profile after VBT, while less than a half of the subjects had a type 1 profile prior to VBT. A significant increase in TK was observed both in the entire cohort and in the patients who presented a non-physiologic sagittal alignment after surgery (type 2a, 2b and 3). Furthermore, the sub-analysis of patients who underwent lumbar instrumentation showed that LL did not decrease after VBT, ruling out a hypothetical kyphotic effect of this technique on the lumbar spine.
The observed correction on the coronal plane, despite being statistically significant, cannot be considered representative of the clinical findings. The Cobb angles before and after surgery were measured as average value on the entire cohort, which comprehended a heterogeneous array of curves, both instrumented and non-instrumented. This leads to an underestimation of the size of the treated curves. A sub-analysis of the different curves and instrumentations was not performed, as an evaluation of the correction on the coronal plane was not the aim of this study. While VBT was originally developed for growth modulation in patients with a considerable residual growth, this technique is being increasingly applied in patients approaching skeletal maturity (Risser 4 and/or Sanders 7) [1], relying on the tissue remodeling process induced by Wolff’s law.
Since the authors included all consecutive patients who underwent VBT and who fulfilled the inclusion criteria, the values of blood loss and surgical time in the whole cohort had not yet the benefit of the right side of the learning curve. With increasing experience, blood loss reached a plateau of 80–100 ml per treated curve and surgical time was reduced to about 20 min per screw, even if a plateau has not yet been reached [22]. These values are coherent with other published data on VBT [6].
Regarding the analysis of sagittal parameters, we observed a statistically significant improvement of TK both in the entire cohort and in patients who had a non-physiologic profile after VBT. This finding is of particular clinical significance, as it is established that scoliosis typically leads to hypokyphosis and that maintenance of TK is required in order to preserve LL and consequently sagittal balance [23].
LL remained stable after VBT, also in case of lumbar instrumentation. The authors believe this could be connected to remodeling of intervertebral disks after surgery, but further studies are required to support this hypothesis. As the patients did not present a PI-LL mismatch before surgery (average PI-LL = 11°), and the amount of preoperative LL was similar to that of the healthy pediatric population [24], an increase in LL was not required nor expected. More relevant in this setting, is the observation that LL did not decrease after surgery, thus ruling out a possible kyphotic effect of VBT even in case of lumbar instrumentation.
While patients had good global balance before surgery (as shown by low values of SVA and PT), these values were further decreased at last follow-up. Increased values of SVA and PT cause increased muscle effort in standing patients [17] and its reduction suggest an improvement in the ergonomics of the erect position. Interestingly, the decrease in both values has been observed despite the increase in thoracic kyphosis (which actually acts in the opposite direction). This phenomenon might be explained by a change in the architecture of the spinal shape, which provided a more balanced distribution of body mass over the hip joints.
Given the consistency in the results obtained regarding sagittal profile, the classification proposed by Abelin-Genevois may represent a powerful tool for the prediction of sagittal profile after VBT. The type of profile observed for each patient in the first standing x-ray after surgery was maintained over time through all follow-ups (data not shown). Notably, all patients that had a physiologic sagittal alignment before surgery (type 1) maintained it after VBT, while most type 2b and 3 maintained the preoperative profile. Many type 2a patients gained a physiologic type 1 profile after VBT. As suggested by Abelin-Genevois and colleagues, type 2 patients necessitate a restoration of TK, which can be obtained with Ponte osteotomies at the apex of the curve in posterior fusion [18]. As VBT allows for an increase in TK, this may explain the behavior of the 2a type subjects who gained a physiologic profile after surgery. However, this mechanism may be not powerful enough to restore the shape and location of the thoracolumbar junction, leading to patients type 2b and 3 to maintain the original sagittal profile.
Being VBT an anterior, non-fusion technique, doubt can arise regarding its a-priori ability to modify the sagittal profile. Our data show that the thoracic kyphosis is increased and that the lumbar lordosis is maintained in the instrumented curves. No experimental data are available to explain the mechanism underlying the sagittal improvement. We suggest one hypothesis that might provide an explanation. The use of an instrumentation that provides compression to the anterior column can have a shortening effect on it, and this would explain the increase in thoracic kyphosis that we observed. Still, it does not explain why the lumbar lordosis is not decreased. To explain this aspect, we have considered that the correction of the lumbar scoliosis pushes the apical vertebrae towards the midline, increasing the length of the spinal elements into the sagittal plane. In addition, we hypothesize that the mechanical behavior of the thoracic versus the lumbar spine can be different, regarding the center of rotation of the corrective maneuvers and the kinematics of the thoracic versus the lumbar spine. In the thoracic spine, the coronally oriented facets favor the rotation of the motion segments rather than the flexion–extension. This would create a posterior tension band effect resulting in anterior shortening. In the lumbar spine facet joints are oriented sagittally, thus favoring flexion–extension over torsion: this would result in a relaxed posterior column favoring an anterior tension-band effect. Further biomechanic studies will be required to clarify this point.
Another mechanism that can explain the improvement of the sagittal profile is positioning of the screws, which allows, to some extent, derotation of the vertebral bodies. This is obtained by positioning the screws more posterior at the apex of the curve, where the vertebrae are most rotated, in respect to the more anterior screws at the cranial and caudal ends of the curve, where the vertebrae are in a more neutral position. We hypothesize that this technique will derotate the apex by cord-tensioning based on the fact that the screws will readjust to the shortest distance between each other. It is possible that derotation at the apex, as performed in VBT, has the same effect as Ponte osteotomies in posterior fusion, thus allowing restoration of TK and consequently of a physiological sagittal profile in many type 2a patients. This principle appears to be insufficient in type 2b and 3 patients, where the type of sagittal alignment was not modified by VBT.
While VBT allows for an overall improvement of sagittal parameters, not all patients obtain a physiologic profile after surgery. However, as VBT has been proven to be a motion-preserving surgical technique [19, 25, 26], spine mobility may be able to compensate for a non-physiologic sagittal profile and thus the achievement of an ideal alignment may be less relevant than it is for fusion surgery. Further biomechanic and long-term studies will be required to confirm this hypothesis.
This study does not come without limitations, the first one being the retrospective nature of this work. Furthermore, the number of patients in the cohort is limited, most of all considering the sub-analysis performed on different subgroups of patients. Of note, as the measurements were obtained on 2D films, an overestimation of TK both before and after surgery is possible; as we measured TK from T1 to T12, we could not perform a correction using the formula proposed by Parvaresh and colleagues [27]. Further studies on a bigger cohort and a longer follow-up are required to better understand the effects of VBT on sagittal parameters.
Conclusion
In conclusion, our study showed that VBT had a positive influence on sagittal parameters and the majority of the patients had a physiologic sagittal profile after surgery. Moreover, lumbar VBT did not have a kyphotic effect on LL. These findings add important evidence on the effects of VBT on sagittal parameters, which may also play a role in the definition of the ideal candidate for VBT. Further studies on a larger cohort and with a longer follow-up are required to clarify this point.
Availability of data and materials
Data can be made available in anonymized form and upon reasonable request.
References
Alanay A, Yucekul A, Abul K, Ergene G, Senay S, Ay B, Cebeci BO, Yalinay Dikmen P, Zulemyan T, Yavuz Y, Yilgor C (2020) Thoracoscopic vertebral body tethering for adolescent idiopathic scoliosis: follow-up curve behavior according to sanders skeletal maturity staging. Spine 45(22):E1483–E1492. https://doi.org/10.1097/BRS.0000000000003643
Bassett WP, Antonacci D, Cuddihy LA et al (2019) Treatment of immature idiopathic scoliosis patients with a non-fusion anterior scoliosis correction (ASC) technique. Amsterdam
Boudissa M, Eid A, Bourgeois E, Griffet J, Courvoisier A (2017) Early outcomes of spinal growth tethering for idiopathic scoliosis with a novel device: a prospective study with 2 years of follow-up. Child’s Nerv Syst 33(5):813–818. https://doi.org/10.1007/s00381-017-3367-4
Hoernschemeyer DG, Boeyer ME, Robertson ME, Loftis CM, Worley JR, Tweedy NM, Gupta SU, Duren DL, Holzhauser CM, Ramachandran VM (2020) Anterior vertebral body tethering for adolescent scoliosis with growth remaining: a retrospective review of 2 to 5-year postoperative results. J Bone Jt Surg Am Vol 102(13):1169–1176. https://doi.org/10.2106/JBJS.19.00980
Newton PO, Kluck DG, Saito W, Yaszay B, Bartley CE, Bastrom TP (2018) Anterior spinal growth tethering for skeletally immature patients with scoliosis: a retrospective look two to four years postoperatively. J Bone Jt Surg Am Vol 100(19):1691–1697. https://doi.org/10.2106/JBJS.18.00287
Newton PO, Bartley CE, Bastrom TP, Kluck DG, Saito W, Yaszay B (2020) Anterior spinal growth modulation in skeletally immature patients with idiopathic scoliosis: a comparison with posterior spinal fusion at 2 to 5 years postoperatively. J Bone Jt Surg Am. https://doi.org/10.2106/JBJS.19.01176
Samdani AF, Ames RJ, Kimball JS, Pahys JM, Grewal H, Pelletier GJ, Betz RR (2014) Anterior vertebral body tethering for idiopathic scoliosis: two-year results. Spine 39(20):1688–1693. https://doi.org/10.1097/BRS.0000000000000472
Samdani AF, Ames RJ, Kimball JS, Pahys JM, Grewal H, Pelletier GJ, Betz RR (2015) Anterior vertebral body tethering for immature adolescent idiopathic scoliosis: one-year results on the first 32 patients. Eur Spine J 24(7):1533–1539. https://doi.org/10.1007/s00586-014-3706-z
Jain V, Lykissas M, Trobisch P, Wall EJ, Newton PO, Sturm PF, Cahill PJ, Bylski-Austrow DI (2014) Surgical aspects of spinal growth modulation in scoliosis correction. Instr Course Lect 63:335–344
Baroncini A, Trobisch PD, Birkenmaier C, Da Paz S, Migliorini F (2021) Radiographic results after vertebral body tethering. Z Orthop Unfall. https://doi.org/10.1055/a-1387-8334
Rushton PRP, Nasto L, Parent S, Turgeon I, Aldebeyan S, Miyanji F (2021) Anterior vertebral body tethering (AVBT) for treatment of idiopathic scoliosis in the skeletally immature: results of 112 cases. Spine. https://doi.org/10.1097/BRS.0000000000004061
Samdani AF, Pahys JM, Ames RJ, Grewal H, Pelletier GJ, Hwang SW, Betz RR (2021) Prospective follow-up report on anterior vertebral body tethering for idiopathic scoliosis: interim results from an FDA IDE study. J Bone Jt Surg Am. https://doi.org/10.2106/JBJS.20.01503
Roaf R 1(966) The basic anatomy of scoliosis. J Bone Jt Surg Br Vol 48(4): 786–792. https://doi.org/10.1302/0301-620X.48B4.786
Trobisch P, Suess O, Schwab F (2010) Idiopathic scoliosis. Dtsch Arztebl Int 107(49):875–883. https://doi.org/10.3238/arztebl.2010.0875
Lenke LG, Betz RR, Harms J, Bridwell KH, Clements DH, Lowe TG, Blanke K (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Jt Surg Am Vol 83(8): 1169–1181
Lenke LG, Edwards CC, Bridwell KH (2003) The Lenke classification of adolescent idiopathic scoliosis: how it organizes curve patterns as a template to perform selective fusions of the spine. Spine 28(20):S199-207. https://doi.org/10.1097/01.BRS.0000092216.16155.33
Glassman SD, Bridwell K, Dimar JR, Horton W, Berven S, Schwab F (2005) The impact of positive sagittal balance in adult spinal deformity. Spine 30(18):2024–2029. https://doi.org/10.1097/01.brs.0000179086.30449.96
Abelin-Genevois K, Sassi D, Verdun S, Roussouly P (2018) Sagittal classification in adolescent idiopathic scoliosis: original description and therapeutic implications. Eur Spine J 27(9):2192–2202. https://doi.org/10.1007/s00586-018-5613-1
Baroncini A, Trobisch PD, Berrer A, Kobbe P, Tingart M, Eschweiler J, Da Paz S, Migliorini F (2021) Return to sport and daily life activities after vertebral body tethering for AIS: analysis of the sport activity questionnaire. Eur Spine J. https://doi.org/10.1007/s00586-021-06768-6
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2007) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Ann Intern Med 147(8):573–577. https://doi.org/10.7326/0003-4819-147-8-200710160-00010
Baroncini A, Rodriguez L, Verma K, Trobisch PD (2019) Feasibility of single-staged bilateral anterior scoliosis correction in growing patients. Glob Spine J. https://doi.org/10.1177/2192568219892904
Baroncini A, Migliorini F, Trobisch PD (2020) learning curve for non-fusion anterior scoliosis correction: analysis on 90 consecutive patients
Newton PO, Yaszay B, Upasani VV, Pawelek JB, Bastrom TP, Lenke LG, Lowe T, Crawford A, Betz R, Lonner B (2010) Preservation of thoracic kyphosis is critical to maintain lumbar lordosis in the surgical treatment of adolescent idiopathic scoliosis. Spine 35(14):1365–1370. https://doi.org/10.1097/BRS.0b013e3181dccd63
Mac-Thiong J-M, Labelle H, Roussouly P (2011) Pediatric sagittal alignment. Eur Spine J 20(Suppl 5):586–590. https://doi.org/10.1007/s00586-011-1925-0
Buyuk AF, Milbrandt TA, Mathew SE, Larson AN (2021) Measurable thoracic motion remains at 1 year following anterior vertebral body tethering, with sagittal motion greater than coronal motion. J Bone Jt Surg, Publish Ahead of Print. https://doi.org/10.2106/JBJS.20.01533
Pehlivanoglu T, Oltulu I, Erdag Y, Akturk UD, Korkmaz E, Yildirim E, Sarioglu E, Ofluoglu E, Aydogan M (2021) Comparison of clinical and functional outcomes of vertebral body tethering to posterior spinal fusion in patients with adolescent idiopathic scoliosis and evaluation of quality of life: preliminary results. Spine Deform 9(4):1175–1182
Parvaresh KC, Osborn EJ, Reighard FG, Doan J, Bastrom TP, Newton PO (2017) Predicting 3D thoracic kyphosis using traditional 2D radiographic measurements in adolescent idiopathic scoliosis. Spine Deform 5(3):159–165. https://doi.org/10.1016/j.jspd.2016.12.002
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
PDT: Globus Medical (personal fees), Zimmer Biomet (personal fees). PB: Nuvasive (personal fees), Depuy Synthes (personal fees), Medacta (personal fees), Zimmer Biomet (personal fees), K2M (personal fees), Medtronic (personal fees), Stoeckli Medical (grants). AC: Zimmer Biomet (personal fees). AB, FM, JE, FH, PK: none.
Ethical approval
RWTH Aachen, Faculty of Medicine, approval EK 130/19.
Consent to participate
Due to the retrospective nature of the study, consent to participate or for publication was not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Baroncini, A., Courvoisier, A., Berjano, P. et al. The effects of vertebral body tethering on sagittal parameters: evaluations from a 2-years follow-up. Eur Spine J 31, 1060–1066 (2022). https://doi.org/10.1007/s00586-021-07076-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-07076-9