Abstract
Purpose
The prognostic ability of the STarT Back Tool (SBT) reportedly varies, but the factors affecting this are unclear. This study investigated the influences of care setting (chiropractic, GP, physiotherapy, spine centre), episode duration (0–2, 3–4, 4–12, >12 weeks), and outcome time period (3, 6, 12 months) on SBT prognostic ability.
Methods
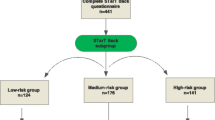
This was a secondary analysis of data from three primary care cohorts [chiropractic (n = 416), GP (n = 265), and physiotherapy (n = 200) practices] and one cohort from a secondary care outpatient spine centre (n = 974) in Denmark. Care pathways were not systematically affected by SBT risk subgroup (non-stratified care). Using generalised estimating equations, we investigated statistical interactions between SBT risk subgroups and potentially influential factors on the prognostic ability of the SBT subgroups, when Roland Morris Disability Questionnaire scores were the outcome.
Results
SBT risk subgroup, age, care setting, and episode duration were all independent prognostic factors. The only investigated factor that modified the prognostic ability of the SBT subgroups was episode duration.
Conclusions
These results indicate that the prognostic ability of the SBT in these non-stratified care settings was unaffected by care setting on its own. However, the prognosis of patients is affected by diverse clinical characteristics that differ between patient populations, many of which are not assessed by the SBT. When controlling for some of those factors and testing potential interactions, the results showed that only episode duration affected the SBT prognostic ability and, specifically, that the SBT was less predictive in very acute patients (<2 weeks duration).



Similar content being viewed by others
References
Hayden JA, Dunn KM, van der Windt DA, Shaw WS (2010) What is the prognosis of back pain? Best Pract Res Clin Rheumatol 24:167–179
Hoy D, Bain C, Williams G, March L, Brooks P, Blyth F, Woolf A, Vos T, Buchbinder R (2012) A systematic review of the global prevalence of low back pain. Arthritis Rheum 64:2028–2037
Foster NE, Hill JC, O’Sullivan P, Hancock M (2013) Stratified models of care. Best Pract Res Clin Rheumatol 27:649–661
Hill JC, Dunn KM, Lewis M, Mullis R, Main CJ, Foster NE, Hay EM (2008) A primary care back pain screening tool: identifying patient subgroups for initial treatment. Arthritis Rheum 59(5):632–641
Pransky G, Borkan JM, Young AE, Cherkin DC (2011) Are we making progress?: the tenth international forum for primary care research on low back pain. Spine (Phila Pa 1976) 36:1608–1614
Bruyere O, Demoulin M, Brereton C, Humblet F, Flynn D, Hill JC, Maquet D, Van BJ, Reginster JY, Crielaard JM, Demoulin C (2012) Translation validation of a new back pain screening questionnaire (the STarT Back Screening Tool) in French. Arch Public Health 7(70):12. doi:10.1186/0778-7367-70-12
Bruyere O, Demoulin M, Beaudart C, Hill JC, Maquet D, Genevay S, Mahieu G, Reginster JY, Crielaard JM, Demoulin C (2013) Validity and Reliability of the French version of the STarT Back Screening Tool for patients with low back pain. Spine (Phila Pa 1976) 39(2):123–128
Gusi N, Del Pozo-Cruz B, Olivares PR, Hernandez-Mocholi M, Hill JC (2011) The Spanish version of the “STarT Back Screening Tool” (SBST) in different subgroups. Aten Primaria 43(7):356–361. doi:10.1016/j.aprim.2010.05.019
Morso L, Albert H, Kent P, Manniche C, Hill J (2011) Translation and discriminative validation of the STarT Back Screening Tool into Danish. Eur Spine J 20(12):2166–2173. doi:10.1007/s00586-011-1911-6
Field J, Newell D (2012) Relationship between STarT Back Screening Tool and prognosis for low back pain patients receiving spinal manipulative therapy. Chiropr Man Therap 20(1):17. doi:10.1186/2045-709X-20-17
Morso L, Kent P, Albert HB, Hill JC, Kongsted A, Manniche C (2013) The predictive and external validity of the STarT Back Tool in Danish primary care. Eur Spine J 22(8):1859–1867. doi:10.1007/s00586-013-2690-z
Morso L, Kent P, Manniche C, Albert HB (2013) The predictive ability of the STarT Back Screening Tool in a Danish secondary care setting. Eur Spine J 23(1):120–128. doi:10.1007/s00586-013-2861-y
Bekkering GE, Hendriks HJ, van Tulder MW, Knol DL, Simmonds MJ, Oostendorp RA, Bouter LM (2005) Prognostic factors for low back pain in patients referred for physiotherapy: comparing outcomes and varying modeling techniques. Spine (Phila Pa 1976) 30:1881–1886
Coste J, Delecoeuillerie G, de Cohen LA, Le Parc JM, Paolaggi JB (1994) Clinical course and prognostic factors in acute low back pain: an inception cohort study in primary care practice. BMJ 308:577–580
Newell D, Field J, Pollard D (2014) Using the STarT Back Tool: Does timing of stratification matter? Man Ther. doi:10.1016/j.math.2014.08.001
Hestbaek L, Munck A, Hartvigsen L, Jarbøl D, Søndergaard Kongsted A (2014) Low Back Pain in Primary care: a description of 1250 patients with low back pain in Danish general and chiropractic practice. Int J Family Med. doi:10.1155/2014/106102
DNcoBR E.Danish National Commitee on Biomedical Research Ethics (2011) Guidelines about Notification. http://www.cvk.sum.dk/English/guidelinesaboutnotification.aspx. Accessed 21 Sept 2014
Kent P, Lauridsen HH (2011) Managing missing scores on the Roland Morris Disability Questionnaire. Spine (Phila Pa 1976) 36:1878–1884
Grotle M, Foster NE, Dunn KM, Croft P (2010) Are prognostic indicators for poor outcome different for acute and chronic low back pain consulters in primary care? Pain 151:790–797
Acknowledgments
We thank all the clinicians who took part in the data collection.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Morso, L., Kongsted, A., Hestbaek, L. et al. The prognostic ability of the STarT Back Tool was affected by episode duration. Eur Spine J 25, 936–944 (2016). https://doi.org/10.1007/s00586-015-3915-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-3915-0