Abstract
Introduction and purpose
The purpose of this study was to evaluate and compare disability, quality of life and satisfaction outcomes between young people and elderly who were operated on for degenerative lumbar disease.
Material and methods
A database of 263 patients undergoing lumbar surgery for degenerative conditions was collected. There were 74 patients who were 65 years old or above and 189 who were below 65 who had complete preoperative and 2-year postoperative HRQOL data measures: ODI, SF-36 and COMI.
Results
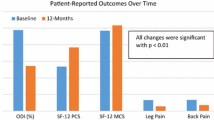
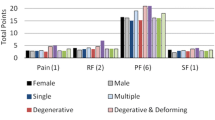
There were no significant differences in the outcomes between the two age groups (p > 0.05). An improvement from baseline in all quality of life measures in the two age groups was observed. A median improvement of 6.0 points was found in the ODI in the younger patients versus 12.0 in older ones. A median improvement in the SF36 physical component score of 6.95 was seen in the younger group while improvement was reported at 6.36 points in patients over 65. The SF36 mental component score improved by 4.48 points and 4.96 points, respectively. COMI improved a median of 1.2 points in both groups. In terms of satisfaction, 66.9 % of the younger patients were pleased or very pleased whereas this was found to be 59.7 % for the older group.
Conclusion
Older patients can see substantial clinical improvement after degenerative lumbar disease surgery similar to that obtained in younger patients in terms of quality of life and satisfaction. The improvement in terms of the disability is greater for older patients. Thus, age should not be a contraindication for this procedure.

Similar content being viewed by others
References
Koes B (2011) Management of low back pain in primary care: a new approach. Lancet 378(9802):1530–2
Balagué F, Mannion AF, Pellisé F, Cedraschi C (2012) Non-specific low back pain. Lancet 379(9814):482–491
Rajaee SS, Bae HW, Kanim L, Delamarter RB (2012) Spinal fusion in the United States: analysis of trends from 1998 to 2008. Spine 37(1):67–76
Bassols A, Bosch F, Campillo M, Baños JE (2003) El dolor de espalda en la población catalana. Prevalencia, características y conducta terapéutica. GacSanit 17(2):97–107
Robaina-Padrón FJ (2007) Controversias de la cirugía instrumentada y el tratamiento del dolor lumbar por enfermedad degenerativa. Resultados de la evidencia científica. Neurocirugia 18(5):406–413
Instituto Nacional de Estadística (2010) Long term evolution of the Spanish population. Madrid: INE on-line: http://www.ine.es/prensa/np587.pdf. Accessed Nov 2013
Carreon LY, Puno RM, Dimar JR, Glassman SD, Johnson JR (2003) Perioperative complications of posterior lumbar decompression and arthrodesis in older adults. J Bone Jt Surg Am 85(11):2089–2092
Sobottke R, Aghayev E, Röder C, Eysel P, Delank SK, Zweig T (2012) Predictors of surgical, general and follow-up complications in lumbar spinal stenosis relative to patient age as emerged from the Spine Tango Registry. Eur Spine J 21(3):411–417
Raffo CS, Lauerman WC (2006) Predicting morbidity and mortality of lumbar spine arthrodesis in patients in their ninth decade. Spine 31(1):99–103
Micankova Adamova B, Vohanka S, Dusek L, Jarkovsky J, Bednarik (2012) Prediction of long-term clinical outcome in patients with lumbar spinal stenosis. Eur Spine J 21(12):2611–2619
Glassman SD, Carreon LY, Dimar JR, Campbell MJ, Puno RM, Johnson JR (2007) Clinical outcomes in older patients after posterolateral lumbar fusion. Spine J 7(5):547–551
Resnick DK, Choudhri TF, Dailey AT, Hadley MN et al (2005) Guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Introduction and methodology. J Neurosurg Spine 2(6):637–638
Keats AS (1978) The ASA classification of physical status—a recapitulation. Anaesthesiology 49(4):233–236
Ware JE Jr, Sherbourne CD (1992) The MOS 36-item short-form healthy survey (SF-36). Conceptual framework and item selection. Med Care 30(6):473–83
Alonso J, Prieto L, Antó JM (1995) The Spanish version of the SF-36 health survey (the SF-36 health questionnaire): an instrument for measuring clinical results. Med Clin 104(20):771–776
Fairback JC, Pynsent PB (2000) The oswestry disability index. Spine 25(22):2940–2952
Alcántara-Bumbiedro S, Flórez-García MT, Echávarri-Pérez C, García- Pérez F (2006) Escala de incapacidad por dolor lumbar de Oswestry. Rehabilitación 40(3):150–158
Deyo R, Battie M, Beurskens A, Bombardier C, Croft P, Koes B et al (1998) Outcome measures for low back pain research: a proposal for standardised use. Spine 23:2003–2013
Ferrer M, Pellisé F, Escudero O, Alvarez L, Pont A, Alonso J, Deyo R (2006) Validation of a minimum outcome core set in the evaluation of patients with back pain. Spine 31(12):1372–1379
Lozano-Álvarez C, Pérez-Prieto D, Saló G, Molina A, Lladó A, Ramírez M (2012) Usefulness of the core outcome measures index in daily clinical practice for assessing patients with degenerative lumbar disease. Adv Orthop 2012:474685
Deyo RA, Gray DT, Kreuter W, Mirza S, Martin BI (2005) United States trends in lumbar fusion surgery for degenerative conditions. Spine 30(12):1441–1445
Glassman SD, Polly DW, Bono CM, Burkus K, Dimar JR (2009) Outcome of lumbar arthrodesis in patients sixty-five years of age or older. J Bone Jt Surg Am 91(4):783–790
Okuda S, Oda T, Miyauchi A, Haku T, Yamamoto T, Iwasaki M (2006) Surgical outcomes of posterior lumbar interbody fusion in elderly patients. J Bone Jt Surg Am 88(12):2714–2720
Crawford CH 3rd, Smail J, Carreon LY, Glassman SD (2011) Health-related quality of life after posterolateral lumbar arthrodesis in patients seventy-five years of age and older. Spine 36(13):1065–1068
Glassman SD, Copay AG, Berven SH, Polly DW, Subach BR, Carreon LY (2008) Defining substantial clinical benefit following lumbar spine arthrodesis. J Bone Jt Surg Am 90(9):1839–1847
Lingard EA, Sledge CB, Learmonth ID (2006) Patient expectations regarding total knee arthroplasty: differences among the United States, United Kingdom, and Australia. J Bone Jt Surg Am 88(6):1201–1207
Mannion AF, Denzler R, Dvorak J, Grob D (2010) Five-year outcome of surgical decompression of the lumbar spine without fusion. Eur Spine J 19(11):1883–1891
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pérez-Prieto, D., Lozano-Álvarez, C., Saló, G. et al. Should age be a contraindication for degenerative lumbar surgery?. Eur Spine J 23, 1007–1012 (2014). https://doi.org/10.1007/s00586-014-3178-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3178-1