Abstract
Background
To evaluate the effect of lumbar microdiscectomy (LM) in pain, disability and quality of life in a 5-year period and to identify potential demographic and clinical risk factors.
Methods
One hundred patients who underwent LM by the same surgeon participated in this prospective study. Clinical assessment was made with validated questionnaires preoperatively and up to 5 years postoperatively. Subsequently, associations between clinical outcomes and demographic data were recorded.
Results
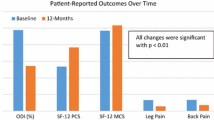
In every assessment questionnaire, there was a significant improvement in the first postoperative month, which lasted up to 1 year post-discectomy. After that, improvement was statistically significant (p < 0.05) but without clinical importance. Women reported more pain preoperatively and 1 month after surgery. Urban residents also presented more pain preoperatively. Older patients had more pain, disability and worse quality of life 1–5 years postoperatively. Similarly, patients with lower education presented the worst scores in every questionnaire at the same time. Smokers reported less pain 1.5–4 postoperative years. Higher alcohol consumption and obesity were associated with lower levels of preoperative pain. However, obese patients had worse SF-36 and ODI scores after the 6th postoperative month. Patients with heavy jobs presented the worst preoperative ODI scores.
Conclusion
Significant clinical improvement was recorded from the first postoperative month to the first postoperative year; stabilization was noticed later on. Feminine gender, urban residency, older age, low level of education, obesity and heavy physical occupation were negative prognostic factors. Oddly smoking and alcohol were correlated with less pain.


Similar content being viewed by others
Abbreviations
- AUDIT:
-
Alcohol Use Disorders Identification Test
- BMI:
-
Body mass index
- LDH:
-
Lumbar disc herniation
- LM:
-
Lumbar microdiscectomy
- MC:
-
Modic changes
- MRI:
-
Magnetic resonance imaging
- ODI:
-
Oswestry Disability Index
- RMDQ:
-
Roland Morris Disability Questionnaire
- SD:
-
Standard deviation
- SPORT:
-
Spine Patient Outcomes Research Trial
- SPSS:
-
Statistical Package for Social Sciences
- VAS:
-
Visual analogue scale
- WHO:
-
World Health Organization
References
Kelsey JL, White AA (1980) Epidemiology and impact of low-back pain. Spine 5(2):133–142
Deyo RA (1991) Nonsurgical care of low back pain. Neurosurg Clin N Am 2(4):851–862
Asch HL, Lewis PJ, Moreland DB et al (2002) Prospective multiple outcomes study of outpatient lumbar microdiscectomy: should 75 to 80% success rates be the norm? J Neurosurg 96(1 Suppl):34–44
Mohanlal P, Pal D, Timothy J (2006) Localisation of spinal level in lumbar microdiscectomy. Eur J Orthop Surg Traumatol 16:207. https://doi.org/10.1007/s00590-005-0059-7
Boscainos PJ, Sapkas G, Stilianessi E, Prouskas K, Papadakis SA (2003) Greek versions of the Oswestry and Roland-Morris disability questionnaires. Clin Orthop Relat Res Number 411:40–53. https://doi.org/10.1097/01.blo.0000068361.47147.79
Deyo R, Loeser J, Bigos S (1990) Herniated lumbar intervertebral disc. Αnn Intern Med 112:598
Ahmadi SA, Burkert IP, Steiger HJ et al (2018) Multidimensional long-term outcome analysis after single-level lumbar microdiscectomy: a retrospective single-centre study. Eur J Orthop Surg Traumatol 28:189. https://doi.org/10.1007/s00590-017-2043-4
Lurie J, Tosteson T, Tosteson A et al (2014) Surgical versus non-operative treatment for lumbar disc herniation: eight-year results for the spine patient outcomes research trial (SPORT). Spine 39(1):3–16. https://doi.org/10.1097/BRS.0000000000000088
McGirt MJ, Eustacchio S, Varga P et al (2009) A prospective cohort study of close interval computed tomography and magnetic resonance imaging after primary lumbar discectomy. Factors associated with recurrent disc herniation and disc height loss. Spine 34(19):2044–2051. https://doi.org/10.1097/BRS.0b013e3181b34a9a
Thomé C, Barth M, Scharf J, Schmiedek P (2005) Outcome after lumbar sequestrectomy compared with microdiscectomy: a prospective randomized study. J Neurosurg Spine 2(3):271–278. https://doi.org/10.3171/spi.2005.2.3.0271
Carragee EJ, Spinnickie AO, Alamin TF, Paragioudakis S (2006) A prospective controlled study of limited versus subtotal posterior discectomy: short-term outcomes in patients with herniated lumbar intervertebral discs and large posterior anular defect. Spine 31(6):653–657. https://doi.org/10.1097/01.brs.0000203714.76250.68
Gelalis ID, Papanastasiou EI, Theodorou DJ et al (2018) Postoperative MRI findings 5 years after lumbar microdiscectomy. Eur J Orthop Surg Traumatol. https://doi.org/10.1007/s00590-018-2338-0
Yorimitsu E, Chiba K, Toyama Y, Hirabayashi K (2001) Long-term outcomes of standard discectomy for lumbar disc herniation: a follow-up study of more than 10 years. Spine 26(6):652–657
Loupasis GA, Stamos K, Katonis PG, Sapkas G, Korres DS, Hartofilakidis G (1999) Seven- to 20-year outcome of lumbar discectomy. Spine 24(22):2313
Barth M, Weiss C, Thomé C (2008) Two-year outcome after lumbar microdiscectomy versus microscopic sequestrectomy: part 1: evaluation of clinical outcome. Spine 33(3):265–272. https://doi.org/10.1097/BRS.0b013e318162018c
Dora C, Schmid MR, Elfering A, Zanetti M, Hodler J, Boos N (2005) Lumbar disk herniation: do MR imaging findings predict recurrence after surgical discectomy? Radiology 235(2):562–567. https://doi.org/10.1148/radiol.2352040624
McGirt MJ, Ambrossi GL, Datoo G, Sciubba DM, Witham TF, Wolinsky JP, Gokaslan ZLBA (2009) Recurrent disc herniation and long-term back pain after primary lumbar discectomy: review of outcomes reported for limited versus aggressive disc removal. Neurosurgery 64(2):338–344. https://doi.org/10.1227/01.NEU.0000337574.58662.E2
Swartz KR, Trost GR (2003) Recurrent lumbar disc herniation. Neurosurg Focus 15(3):E10
Weber H (1983) Lumbar disc herniation: a controlled, prospective study with ten years of observation. Spine 8(2):131–140
Dalgic A, Yildirim AE, Okay O et al (2015) Initial discectomy associated with aging lead to adjacent disc disease and recurrence. Turk Neurosurg 26(4):595–600. https://doi.org/10.5137/1019-5149.JTN.13206-14.0
Ganzer D, Giese K, Hunfeld T et al (2002) Lumbar microdiscectomy with and without prophylaxis of perineural scar formation using ADCON-L barrier gel: 2-year results. Eur J Orthop Surg Traumatol 12:1. https://doi.org/10.1007/s00590-002-0011-z
Li T, Han D, Liu B et al (2014) Clinical assessment of reformed lumbar microdiscectomy. Eur J Orthop Surg Traumatol 24:23. https://doi.org/10.1007/s00590-012-1123-8
Cinotti G, Roysam GS, Eisenstein SM, Postacchini F (1998) Ipsilateral recurrent lumbar disc herniation. A prospective, controlled study. J Bone Joint Surg Br 80(5):825–832
Guo JJ, Yang H, Tang T (2009) Long-term outcomes of the revision open lumbar discectomy by fenestration: a follow-up study of more than 10 years. Int Orthop 33(5):1341–1345. https://doi.org/10.1007/s00264-008-0648-2
Atlas SJ, Keller RB, Chang Y et al (2001) Surgical and nonsurgical management of sciatica secondary to a lumbar disc herniation: five-year outcomes from the maine lumbar spine study. Spine 26:1179–1187
Koerner JD, Glaser J, Radcliff K (2015) Which variables are associated with patient-reported outcomes after discectomy? review of SPORT disc herniation studies. Clin Orthop Relat Res 473(6):2000–2006. https://doi.org/10.1007/s11999-014-3671-1
Huang W, Han Z, Liu J, Yu L, Yu X (2016) Risk factors for recurrent lumbar disc herniation. A systematic review and meta-analysis. Medicine 95(2):e2378. https://doi.org/10.1097/MD.0000000000002378
Akmal M, Kesani A, Anand B, Singh A, Wiseman M, Goodship A (2004) Effect of nicotine on spinal disc cells: a cellular mechanism for disc degeneration. Spine 29:568–575. https://doi.org/10.1097/01.BRS.0000101422.36419.D8
Schmidt H, Kettler A, Heuer F et al (2007) Intradiscal pressure, shear strain, and fiber strain in the intervertebral disc under combined loading. Spine 32:748–755. https://doi.org/10.1097/01.brs.0000259059.90430.c2
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors Ioannis D Gelalis, Evangelos I Papanastasiou, Emilios E Pakos, Avraam Ploumis, Dimitrios V Papadopoulos, Maria Mantzari, Ioannis S. Gkiatas, Marios D. Vekris and Anastasios V. Korompilias declare that they do not have any conflict of interest.
Rights and permissions
About this article
Cite this article
Gelalis, I.D., Papanastasiou, E.I., Pakos, E.E. et al. Clinical outcomes after lumbar spine microdiscectomy: a 5-year follow-up prospective study in 100 patients. Eur J Orthop Surg Traumatol 29, 321–327 (2019). https://doi.org/10.1007/s00590-018-2359-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-018-2359-8