Abstract

A primary Echinococcus granulosus infection of the spine involving the vertebrae T8 and T9 of a 6-year-old child was treated elsewhere by thoracotomy, partial corporectomy, multiple laminectomies and uninstrumented fusion. Owing to inappropriate stabilization, severe deformity developed secondary to these surgeries. X-rays, CT and MRI scans of the spine revealed a severe thoracic kyphoscoliosis of more than 100° (Fig. 1) and recurrence of Echinococcus granulosus infection. The intraspinal cyst formation was located between the stretched dural sac and the vertebral bodies of the kyphotic apex causing significant compression of the cord (Figs. 2, 3, 4). A progressive neurologic deficit was reported by the patient. At the time of referral, the patient was wheelchair bound and unable to walk by herself (Frankel Grade C). Standard antiinfectious therapy of Echinococcus granulosus requires a minimum treatment period of 3 months. This should be done before any surgical intervention because in case of a rupture of an active cyst, the delivered lipoprotein antigens of the parasite may cause a potentially lethal anaphylactic shock. Owing to the critical neurological status, we decided to perform surgery without full length preoperative antiinfectious therapy. Surgical treatment consisted in posterior vertebral column resection technique with an extensive bilateral costotransversectomy over three levels, re-decompression with cyst excision around the apex and multilevel corporectomy of the apex of the deformity. Stabilisation and correction of the spinal deformity were done by insertion of a vertebral body replacement cage anteriorly and posterior shortening by compression and by a multisegmental pedicle screw construct. After the surgery, antihelminthic therapy was continued. The patients neurological deficits resolved quickly: 4 weeks after surgery, the patient had Frankel Grade D and was ambulatory without any assistance. After an 18-month follow-up, the patient is free of recurrence of infection and free of neurologically deficits (Frankel E). This case demonstrates that inappropriate treatment—partial resection of the cyst, inappropriate anterior stabilization and posterior multilevel laminectomies without posterior stabilization—may lead to severe progressive kyphoscoliotic deformity and recurrence of infection, both leading to significant neurological injury presenting as a very difficult to treat pathology.

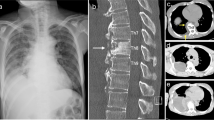
X-rays of the patient showing a kyhoscoliotic deformity. a ap view, b lateral view

CT reconstruction of the whole spine showing the apex of the deformity is located in the area of the previous surgeries

Sagittal CT-cut showing the bone bloc at the apex with a translation deformity

Sagittal T2-weighted MRI image showing the cystic formation at the apex








Similar content being viewed by others
References
BM Altinörs N, Caner HH, Erdogan B (2000) Central nervous system hydatidosis in Turkey: a cooperative study and literature survey analysis of 458 cases. J Neurosurg 93:1–8
Bhojraj SY, Shetty NR (1999) Primary hydatid disease of the spine: an unusual cause of progressive paraplegia: case report and review of the literature. J Neurosurg 91:216–218
Bilgic S, Kose O, Sehirlioglu A, Safaz I, Ozkan H (2008) Primary paraspinal hydatid cyst treated with puncture, aspiration, injection and re-aspiration (PAIR) technique: a case report. Eur Spine J 18:165–167
Braithwaite PA, Lees RF (1981) Vertebral hydatid disease: radiological assessment. Radiology 140:763–766
Garcia-Vicuna R, Carvajal I, Ortiz-Garcia A, Lopez-Robledillo JC, Laffon A, Sabando P (2000) Primary solitary Echinococcosis in cervical spine. Postsurgical successful outcome after long-term albendazole treatment. Spine 25:520–523
Govender TS, Aslam M, Parbhoo A, Corr P (2000) Hydatid disease of the spine. A long-term followup after surgical treatment. Clin Orthop Relat Res 143–147
Güneçs M, Akdemir H, Tuğcu B, Günaldi O, Gümüçs E, Akpinar A (2009) Multiple intradural spinal hydatid disease: a case report and review of literature. Spine 20:346–350
Hamdan TA, Al-Kaisy MA (2000) Dumbbell hydatid cyst of the spine: case report and review of the literature. Spine 25:1296–1299
Herrera A, Martinez AA, Rodriguez J (2005) Spinal hydatidosis. Spine 30:2439–2444
Islekel S, Zileli M, Ersahin Y (1998) Intradural spinal hydatid cysts. Eur Spine J 7:162–164
Kalkan E, Cengiz SL, Cicek O, Erdi F, Baysefer A (2007) Primary spinal intradural extramedullary hydatid cyst in a child. J Spinal Cord Med 30:297–300
Khazim R, Fares Y, Heras-Palou C, Ruiz Barnes P (2003) Posterior decompression of spinal hydatidosis: long term results: Fundacion Jimenez Diaz, Madrid, Spain. Clin Neurol Neurosurg 105:209–214
Kotil TZ, Tatar T, Bilge T (2007) Spinal hydatidosis accompanied by a secondary infection: case report. J Neurosurgery Spine 6:585–590
Papagelopoulos PJ, Peterson HA, Ebersold MJ, Emmanuel PR, Choudhury SN, Quast LM (1997) Spinal column deformity and instability after lumbar or thoracolumbar laminectomy for intraspinal tumors in children and young adults. Spine 22:442–451
Papanikolaou A (2008) Osseous hydatid disease. Trans R Soc Trop Med Hyg 102:233–238
Prabhakar MM, Acharya AJ, Modi DR, Jadav B (2005) Spinal hydatid disease: a case series. J Spinal Cord Med 28:426–431
Sapkas GS, Machinis TG, Chloros GD, Fountas KN, Themistocleous GS, Vrettakos G (2006) Spinal hydatid disease, a rare but existent pathological entity: case report and review of the literature. South Med J 99:178–183
Schnepper GD, Johnson WD (2004) Recurrent spinal hydatidosis in North America. Case report and review of the literature. Neurosurg Focus 17:1–6
Spies C, Weisskopf M, Ohnsorge JA (2008) Intraspinal echinococcosis within the lumbar spine of an 18-year-old male patient. Z Orthop Unfall 146:463–467
Tuzun M, Hekimoğlu B (2002) CT findings in skeletal cystic echinococcosis. Acta Radiol 43:533–538
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thaler, M., Gabl, M., Lechner, R. et al. Severe kyphoscoliosis after primary Echinococcus granulosus infection of the spine. Eur Spine J 19, 1415–1422 (2010). https://doi.org/10.1007/s00586-010-1398-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-010-1398-6