Abstract
The relationship between cervicitis and fertility has been poorly studied in dairy cows. Endocervical inflammation, determined by an increase of polymorphonuclear leukocytes (PMN), is linked with lower hazard of pregnancy. The objective of the present study was to evaluate if an increase in PMN in the cervical mucosa is associated with decreased fertility in dairy cows. Endocervical samples were collected from dairy cows (n = 243) between 30 and 40 days postpartum. All cows had completed their uterine involution and did not show clinical uterine diseases. A cytological sample was taken by passing the first ring of the cervix using an endocervical brush. A smear was made and stained using the diff quick technique. One hundred cells were counted, and the proportion of PMN was obtained. The cut-off point for the percentage of PMN that corresponded to a decrease in fertility was obtained by analyzing the ROC curve. The cut-off point for the proportion of PMN influencing a decreased fertility was 6%. Thirty-five percent (86/243) of the cows had ≥ 6% PMN. The conception rate at first service was higher in cows with < 6% PMN (43%) than in cows with ≥ 6% PMN (31.4%) [odds ratio = 1.74, CI = 1.0–3.0 (P = 0.047)]. The cumulative proportion of pregnant cows at day 210 postpartum was higher in cows that had < 6% PMN (82%) than cows with ≥ 6% PMN (69%) [odds ratio = 2.2, CI = 1.1–3.9 (P = 0.017)]. Cows with < 6% PMN had a reduced interval from calving to conception than cows with ≥ 6% PMN [97 days (89–106 days) vs. 110 days (89–123 days); median (95% CI); P < 0.05]. In conclusion, a higher proportion of PMN in the cervical mucosa is associated with decreased fertility in dairy cows.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Around 40% of postpartum dairy cows develop uterine pathologies such as metritis, endometritis, or subclinical endometritis (Sheldon et al. 2019). These conditions prolong the interval from calving to the first ovulation, reduce fertility in the first service, extend the calving to conception period, and increase pregnancy losses (Sheldon et al. 2009; LeBlanc 2014). A significant proportion of cows experience some degree of clinical cervicitis after calving; Hartmann et al. (2016) observed that 60.8% of cows between 42 and 50 days postpartum had hyperemia, edema, or cervical mucosa prolapse. The inflammatory state of the cervix in postpartum cows and its relationship with fertility have been poorly studied. Deguillaume et al. (2012) noted that an increase in the proportion of polymorphonuclear leukocytes (PMN) in the cervical mucosa before day 35 postpartum is associated with reduced fertility. In this study, ≥ 5% PMN in the cervical mucosa, regardless of endometrial inflammation, was linked to a decreased hazard of pregnancy within 300 days postpartum.
Research on uterine pathologies and their connection to reproductive performance in dairy cows has primarily focused on metritis, clinical endometritis, and subclinical endometritis, while cervicitis has received less attention (Sheldon et al. 2006; LeBlanc 2014). Therefore, the objective of the present study was to evaluate if an increase in PMN in the cervical mucosa is associated with decreased fertility in dairy cows.
Materials and methods
Animals
The study was conducted in the Tizayuca, Hidalgo, Mexico (central highland of Mexico) dairy area. The climate of the region is temperate subhumid, with an average annual temperature of 15.5 °C and an average annual rainfall of 861 mm. Holstein cows (n = 243) with different parities (1 to 6 calving) and a body condition score (BCS) greater than 2 (1–5) were included in the study. Cows were housed in free stall pens under similar management and feeding conditions. Average milk production per cow was in the range of 7500–8000 kg per lactation. All cows were examined transrectally after parturition, and those with uterine pathologies (retained placenta, metritis, and endometritis) received treatment. Cows were diagnosed healthy when they completed their uterine involution (uterus and cervix without abnormalities) and did not show abnormal vaginal secretions by transrectal palpation. It is important to emphasize that vaginoscopy was not used in the clinical evaluation of the cervix. The voluntary waiting period was 50 days. Cows were identified in estrus by observing estrus behavior and mating acceptance, and were inseminated by the same technician under the am-pm/pm-am program. Pregnancy diagnosis was performed by transrectal palpation on day 45 after insemination.
Cytological sampling
Between 30 and 40 days postpartum, all cows diagnosed as healthy had a cytological sample of the cervical mucosa with an endocervical brush (cytobrush) used in human gynecology. A bovine insemination gun was attached with a cytobrush. The gun was covered for protection from vaginal contamination with a bovine split universal sheath. Once the first ring of the cervix was passed, the cytobrush was exposed and rolled twice onto the cervical mucosa and then reintroduced back in the protective sheath of the gun. After obtaining the sample, a smear was made on a slide, fixed in alcohol, and stained using the diff quick technique (Madoz et al. 2014). One hundred endometrial cells were counted, and the proportion of PMN was calculated.
Statistical analysis
The cut-off point of the PMN corresponding to a decrease in reproductive efficiency was obtained by analyzing the ROC curve using SigmaPlot 10.0 (2006). The cut-off point was the point on the ROC curve that had the highest combined sensitivity and specificity.
To analyze the conception rate at first service and cumulative pregnancy rate at day 210 postpartum, logistic regression analysis was performed using the GLM function of the statistical software R 4.0.2 (2020). Independent variables were parity (primiparous vs. multiparous), type of puerperium [physiological vs. pathological (cows with a precedent of retained placenta and purulent vaginal discharge during their puerperium), and PMN cut-off point. The interval from calving to first service and the number of services per conception was analyzed by Mann–Whitney U test of the statistical program R 4.0.2 (2020). Survival analysis was performed to estimate the survival function for the event variable (PMN) through the time variable (interval from calving to conception); the Kaplan and Meier method was implemented in the survfit function of the statistical program R 4.0.2 (2020).
Results
The cut-off point for the proportion of PMN influencing a decreased fertility was 6% (74.4% sensitivity; 45.4% specificity; 0.58 area under the curve; P < 0.05; Fig. 1). Thirty-five percent of the cows had ≥ 6% PMN in the cervix mucosa. Parity and type of puerperium did not affect the proportion of PMN (P > 0.05). Table 1 shows the odds ratio for pregnancy at first service and cumulative pregnancies at day 210 postpartum. Conception rate at first service and cumulative percentage of pregnant cows at day 210 postpartum were higher in cows with < 6% PMN than in cows with ≥ 6% PMN. Parity and type of puerperium did not affect the conception rate at first service and pregnancy rate at day 210 postpartum.
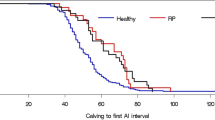
Cows with < 6% PMN had a reduced interval from calving to conception than cows with ≥ 6% PMN [97 days (89–106 days) vs. 110 days (89–123 days); median (95% CI); P < 0.05; Fig. 2]. The interval from calving to first service and number of services per conception were similar in cows with < 6% PMN (82.4 ± 2.7 days and 1.70 ± 0.07) vs. ≥ 6% PMN (84.6 ± 3.5 days and 1.85 ± 0.12; P > 0.05).
Survival curve of the interval from calving to conception (days open) of cows with < 6% PMN vs. ≥ 6% PMN in the uterine cervical mucosa. Cows with < 6% of PMN had a reduced interval from calving to conception than cows with ≥ 6% [97 days (89–106 days) vs. 110 days (89–123 days); median (95% CI); P < 0.05]
Discussion
The present study has shown an association between the presence of PMN in the cervical mucosa and fertility in dairy cows. Cows with ≥ 6% PMN in the uterine cervical mucosa presented a reduced conception rate at first service, and a reduced cumulative pregnancy rate at day 210 postpartum, as well as a higher interval from calving to conception (days open) than cows with < 6% PMN.
The cut-off point (≥ 6% of PMN) to establish that a cow has an endocervical inflammatory process (cytological endocervicitis) was close to that used in the study by Deguillaume et al. (2012). In that study, it was established that cows with no clinical history of cervicitis and ≥ 5% PMN in the cervical mucosa had an inflammatory process in the cervix, which also extended the days from calving to conception. On the other hand, in the present study, the prevalence of cytological endocervicitis was 35%, which is close to the 42% observed by Deguillaume et al. (2012). It is interesting to note that both the cut-off point and the prevalence fall within the ranges for the diagnosis of subclinical endometritis (Wagener et al. 2017).
Ahmadi et al. (2005) and Yavari et al. (2009) found that there is an association between the proportion of PMN in cervical mucosa with the proportion of PMN at the endometrium; that is, the migration of PMN that occurs in the endometrium is similar to that observed in the cervical mucosa. These studies would suggest that inflammation of the cervical mucosa could be an extension of an endometrial inflammatory process; however, Deguillaume et al. (2012) found that cervicitis was not associated with endometritis in 25% of the cows. Therefore, they propose that the effect of cervicitis on fertility reduction is not necessarily linked to the effect of endometritis. These observations align with the study by Hartmann et al. (2016), where they conclude that after clinical, cytological, and histological examinations, that cervicitis can occur independently of endometritis and it can impair fertility in dairy cows.
The cervix is a physical barrier contributing to the innate immune mechanisms of the uterus (Dadarwal et al. 2017). During parturition and puerperium, bacterial contamination of the uterus causes inflammation of the endometrium and cervix. Nearly 80% of the cows presented bacterial contamination in the uterus during the first 3 weeks postpartum (Sheldon and Dobson 2004). Cervicitis can be explained by direct bacterial contamination or infections from internal regions of the uterus, which is favored by possible injuries during parturition. On the other hand, an infectious process of the cervix can be a risk factor for contamination of the endometrium in cases with no concomitant pathologies (Deguillaume et al. 2012).
The mechanism by which cytological endocervicitis affects fertility has been poorly studied; however, it can be speculated that it would be related to the same mechanism by which endometritis decreases fertility. It has been documented that mediating factors of the endometrial inflammatory process decrease embryo quality (Hill and Gilbert 2008). Likewise, the presence of PMN in the endometrium of cows at the time of service and on the day of embryo collection was associated with a decrease in the number and quality of the embryos (Drillich et al. 2012). On the other hand, during endometritis, fertility may decrease because follicular development and estradiol synthesis are compromised, as well as the subsequent corpus luteum development, secreting reduced levels of progesterone (Sheldon et al. 2009). Although described effects have been observed in cows with clinical or subclinical endometritis, similar mediating factors of the inflammatory process have also been identified in cows that only suffered from clinical cervicitis (Vallejo-Timarán et al. 2021).
Deguillaume et al. (2012) observed an independent effect of cervical mucosa inflammation and, furthermore, an additive effect of the combination of cervicitis and endometritis on the hazard of pregnancy within the 300 days postpartum. These same authors suggest that it would be advisable to replace the concept of “uterine health” with that of “genital health” to encompass inflammation of both the uterus and the cervix. In this context, endocervical cytology could be a simple and less invasive tool for assessing the status of “genital health.”
Conclusion
The findings suggest that a higher presence of PMN (≥ 6%) in the cervical mucosa leads to decrease in the initial pregnancy rate and the overall pregnancy rate by day 210 postpartum. Additionally, it lengthens the interval between calving and conception in dairy cows.
Data availability
The data generated and analyzed in this work will be made available upon request to the corresponding author.
References
Ahmadi MR, Khodakaram A, Tafti S, Nazifi H, Ghaisari R (2005) The comparative evaluation of uterine and cervical mucosa cytology with endometrial histopathology in cows. Comp Clin Pathol 14:90–94. https://doi.org/10.1007/s00580-005-0565-3
Dadarwal D, Palmer C, Griebel P (2017) Mucosal immunity of the postpartum bovine genital tract. Theriogenology 104:62–71. https://doi.org/10.1016/j.theriogenology.2017.08.010
Deguillaume L, Geffré A, Desquilbet L, Dizien A, Thoumire S, Vornière C, Constant F, Fournier R, Chastant-Maillard S (2012) Effect of endocervical inflammation on days to conception in dairy cows. J Dairy Sci 95:1776–1783. https://doi.org/10.3168/jds.2011-4602
Drillich M, Tesfaye D, Rings F, Schellander K, Heuwieser W, Hoelker M (2012) Effects of polymorphonuclear neutrophile infiltration into the endometrial environment on embryonic development in superovulated cows. Theriogenology 77:570–578. https://doi.org/10.1016/j.theriogenology.2011.08.033
Hartmann D, Rohkohl J, Merbach S, Heilkenbrinker T, Klindworth HP, Schoon HA, Hoedemaker M (2016) Prevalence of cervicitis in dairy cows and its effect on reproduction. Theriogenology 85:247–253. https://doi.org/10.1016/j.theriogenology.2015.09.029
Hill J, Gilbert R (2008) Reduced quality of bovine embryos cultured in media conditioned by exposure to an inflamed endometrium. Aust Vet J 86:312–316. https://doi.org/10.1111/j.1751-0813.2008.00326.x
LeBlanc SJ (2014) Reproductive tract inflammatory disease in postpartum dairy cows. Animal 8(Suppl 1):54–63. https://doi.org/10.1017/s1751731114000524
Madoz LV, Giuliodori MJ, Migliorisi AL, Jaureguiberry M, de la Sota RL (2014) Endometrial cytology, biopsy, and bacteriology for the diagnosis of subclinical endometritis in grazing dairy cows. J Dairy Sci 97:195–201. https://doi.org/10.3168/jds.2013-6836
R Core Team (2020) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. URL https://www.R-project.org/
Sheldon IM, Cronin JG, Bromfield JJ (2019) Tolerance and innate immunity shape the development of postpartum uterine disease and the impact of endometritis in dairy cattle. Annu Rev Anim Biosci 15:361–384. https://doi.org/10.1146/annurev-animal-020518-115227
Sheldon IM, Dobson H (2004) Postpartum uterine health in cattle. Anim Reprod Sci 82–83:295–306. https://doi.org/10.1016/j.anireprosci.2004.04.006
Sheldon IM, Lewis GS, LeBlanc SJ, Gilbert RO (2006) Defining postpartum uterine disease in cattle. Theriogenology 65:1516–1530. https://doi.org/10.1016/j.theriogenology.2005.08.021
Sheldon IM, Price SB, Cronin J, Gilbert RO, Gadsby JE (2009) Mechanisms of infertility associated with clinical and subclinical endometritis in high producing dairy cattle. Reprod Domest Anim 44(Suppl 3):1–9. https://doi.org/10.1111/j.1439-0531.2009.01465.x
Systat (2006) Sigmaplot User’s Guide, version 10.0. Systat Software Inc., Chicago, IL
Vallejo-Timarán DA, Bazzazan A, Segura M, Prieto-Cárdenas NE, Lefebvre RC (2021) Pre- and postpartum concentrations of interleukin 1α, interleukin 8, and α1-acid glycoprotein in vaginal fornix and endometrium of dairy cows with clinical cervicitis. Front Vet Sci 7:21–31. https://doi.org/10.3389/fvets.2020.605773
Wagener K, Gabler C, Drillich M (2017) A review of the ongoing discussion about definition, diagnosis and pathomechanism of subclinical endometritis in dairy cows. Theriogenology 94:21–30. https://doi.org/10.1016/j.theriogenology.2017.02.005
Yavari M, Haghkhah M, Ahmadi MR, Gheisari HR, Nazifi S (2009) Comparison of cervical and uterine cytology between different classification of postpartum endometritis and bacterial isolates in Holstein dairy cows. Int J Dairy Sci 4:19–26. https://doi.org/10.3923/ijds.2009.19.26
Acknowledgements
The authors appreciate the support of the farmers of the dairy area in Tizayuca, Hidalgo.
Funding
This study was funded by X (grant number X)
Author information
Authors and Affiliations
Contributions
Study conception and design: Marco Antonio Oropeza, Rodolfo Luzbel de la Sota, Carlos Fernando Aréchiga, and Joel Hernández-Cerón. Data management and analysis: Marco Antonio Oropeza, Rodolfo Luzbel de la Sota, Noé Juárez, and Joel Hernández-Cerón. Development of the experiment: Marco Antonio Oropeza and Mario Bedolla. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Funding
This study was not supported by any funding.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the Institutional Committee for the Care and Use of Experimental Animals of the National Autonomous University of Mexico School of Veterinary Medicine and Animal Husbandry.
Informed consent
For this type of study informed consent is not required.
Consent for publication
For this type of study consent for publication is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Oropeza, M.A., de la Sota, R.L., Bedolla, M. et al. Association between polymorphonuclear leukocytes in the cervical mucosa and fertility in dairy cows. Comp Clin Pathol 33, 201–205 (2024). https://doi.org/10.1007/s00580-023-03539-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00580-023-03539-1