Abstract
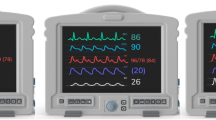
Monitoring the patient's physiological functions is critical in clinical anesthesia. The latest version of the Japanese Society of Anesthesiologists' Guidelines for Safe Anesthesia Monitoring, revised in 2019, covers various factors, including electroencephalogram monitoring, oxygenation, ventilation, circulation, and muscle relaxation. However, with recent advances in monitoring technologies, the information provided has become more detailed, requiring practitioners to update their knowledge. At a symposium organized by the Journal of Anesthesia in 2023, experts across five fields discussed their respective topics: anesthesiologists need to interpret not only the values displayed on processed electroencephalogram monitors but also raw electroencephalogram data in the foreseeable future. In addition to the traditional concern of preventing hypoxemia, monitoring for potential hyperoxemia and the effects of mechanical ventilation itself will become increasingly important. The importance of using AI analytics to predict hypotension, assess nociception, and evaluate microcirculation may increase. With the recent increase in the availability of neuromuscular monitoring devices in Japan, it is important for anesthesiologists to become thoroughly familiar with the features of each device to ensure its effective use. There is a growing desire to develop and introduce a well-organized, integrated “single screen” monitor.
Similar content being viewed by others
Data availabilty
Not applicable.
Abbreviations
- EEG:
-
Electroencephalogram
- BIS:
-
Bispectral index
- PSi:
-
Patient state index
- SpO2 :
-
Oxygen saturation
- PaO2 :
-
Arterial partial pressure of oxygen
- ORi:
-
Oxygen reserve index
- IOH:
-
Intraoperative hypotension
References
Prys-Roberts C. Anaesthesia: a practical or impractical construct? Br J Anaesth. 1987;59:1341–5.
Kang H, Mohamed HMH, Takashina M, Mori T, Fujino Y, Hagihira S. Individual indicators of appropriate hypnotic level during propofol anesthesia: highest alpha power and effect-site concentrations of propofol at loss of response. J Anesth. 2017;31:502–9.
Steriade M, Nuñez A, Amzica F. Intracellular analysis of relations between the slow (< 1 Hz) neocortical oscillation and other sleep rhythms of the electroencephalogram. J Neurosci. 1993;13:3266–83.
Steriade M, Contreras D, Curró Dossi R, Nuñez A. The slow (< 1 Hz) oscillation in reticular thalamic and thalamocortical neurons: scenario of sleep rhythm generation in interacting thalamic and neocortical networks. J Neurosci. 1993;13:3284–99.
Miyasaka K, Shelley K, Takahashi S, Kubota H, Ito K, Yoshiya I, Yamanishi A, Cooper JB, Steward DJ, Nishida H, Kiani J, Ogino H, Sata Y, Kopotic RJ, Jenkin K, Hannenberg A, Gawande A. Tribute to Dr. Takuo Aoyagi, inventor of pulse oximetry. J Anesth. 2021;35:671–709.
Scheeren TWL, Belda FJ, Perel A. The oxygen reserve index (ORI): a new tool to monitor oxygen therapy. J Clin Monit Comput. 2018;32:379–89.
Ishida Y, Okada T, Kobayashi T, Uchino H. ORi™: a new indicator of oxygenation. J Anesth. 2021;35:734–40.
Yoshida K, Isosu T, Noji Y, Hasegawa M, Iseki Y, Oishi R, Imaizumi T, Sanbe N, Obara S, Murakawa M. Usefulness of oxygen reserve index (ORi™), a new parameter of oxygenation reserve potential, for rapid sequence induction of general anesthesia. J Clin Monit Comput. 2018;32:687–91.
Koishi W, Kumagai M, Ogawa S, Hongo S, Suzuki K. Monitoring the Oxygen Reserve Index can contribute to the early detection of deterioration in blood oxygenation during one-lung ventilation. Minerva Anestesiol. 2018;84:1063–9.
Fukada T, Tsuchiya Y, Iwakiri H, Ozaki M, Nomura M. Comparisons of the efficiency of respiratory rate monitoring devices and acoustic respiratory sound during endoscopic submucosal dissection. J Clin Monit Comput. 2022;36:1013–9.
Kitsiripant C, Fukada T, Iwakiri H, Tsuchiya Y, Ozaki M, Nomura M. Comparison of Nellcor™ PM1000N and Masimo Radical-7(®) for detecting apnea in volunteers. J Anesth. 2017;31:709–13.
Maheshwari K, Cywinski JB, Papay F, Khanna AK, Mathur P. Artificial intelligence for perioperative medicine: perioperative intelligence. Anesth Analg. 2023;136:637–45.
Hatib F, Jian Z, Buddi S, Lee C, Settels J, Sibert K, Rinehart J, Cannesson M. Machine-learning algorithm to predict hypotension based on high-fidelity arterial pressure waveform analysis. Anesthesiology. 2018;129:663–74.
Awad H, Alcodray G, Raza A, Boulos R, Essandoh M, Bhandary S, Dalton R. Intraoperative hypotension-physiologic basis and future directions. J Cardiothorac Vasc Anesth. 2022;36:2154–63.
Michard F, Liu N, Kurz A. The future of intraoperative blood pressure management. J Clin Monit Comput. 2018;32:1–4.
Meijer FS, Martini CH, Broens S, Boon M, Niesters M, Aarts L, Olofsen E, van Velzen M, Dahan A. Nociception-guided versus standard care during remifentanil-propofol anesthesia: a randomized controlled trial. Anesthesiology. 2019;130:745–55.
Meijer F, Honing M, Roor T, Toet S, Calis P, Olofsen E, Martini C, van Velzen M, Aarts L, Niesters M, Boon M, Dahan A. Reduced postoperative pain using Nociception Level-guided fentanyl dosing during sevoflurane anaesthesia: a randomised controlled trial. Br J Anaesth. 2020;125:1070–8.
Ince C. Hemodynamic coherence and the rationale for monitoring the microcirculation. Critical care (London, England). 2015;19(Suppl 3):S8.
Foss NB, Kehlet H. Perioperative haemodynamics and vasoconstriction: time for reconsideration? Br J Anaesth. 2019;123:100–3.
Thilen SR, Weigel WA, Todd MM, Dutton RP, Lien CA, Grant SA, Szokol JW, Eriksson LI, Yaster M, Grant MD, Agarkar M, Marbella AM, Blanck JF, Domino KB. 2023 American society of Anesthesiologists practice guidelines for monitoring and antagonism of neuromuscular blockade: a report by the American society of Anesthesiologists task force on neuromuscular blockade. Anesthesiology. 2023;138:13–41.
Acknowledgements
We would like to thank the Scientific English Editing Section of Fukushima Medical University for editing a draft of this manuscript.
Funding
Departmental funding only.
Author information
Authors and Affiliations
Contributions
SO organized the manuscript, wrote, and edited the article. NO edited the manuscript. SH, KY, YK, ST, and KM wrote the manuscript. All authors reviewed and approved the final draft.
Corresponding author
Ethics declarations
Conflict of interest
Shinju Obara is an Editor of Journal of Anesthesia, and an Editorial board of JA Clinical Reports. Naoyuki Hirata is an Editor of Journal of Anesthesia, and an Editorial board of JA Clinical Reports. Kenichi Masui had received payments for delivering domestic lectures from Masimo Japan Corporation (Tokyo, Japan), Covidien Japan Inc. (Tokyo, Japan), and MSD K.K. (Tokyo, Japan), and is an Editor of Journal of Anesthesia, and an Editorial board of JA Clinical Reports.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Obara, S., Hirata, N., Hagihira, S. et al. What are standard monitoring devices for anesthesia in future?. J Anesth (2024). https://doi.org/10.1007/s00540-024-03347-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00540-024-03347-z