Abstract
Purpose
This study was performed to examine and compare the incidence of extubation recall in surgical patients who underwent remimazolam anesthesia with flumazenil antagonism during emergence and in those who underwent propofol anesthesia.
Methods
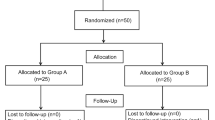
One hundred sixty-three patients who underwent surgery using general endotracheal or supraglottic airway anesthesia with propofol (n = 97) or remimazolam (n = 66) were retrospectively analyzed. Remimazolam was antagonized by flumazenil after discontinuation of remimazolam at the end of surgery. The endotracheal tube or supraglottic airway was removed after surgery was complete, and consciousness and adequate spontaneous breathing were confirmed. The incidence of extubation recall was compared between the remimazolam and propofol anesthesia groups using propensity score matching.
Results
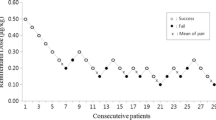
Extubation recall was observed in 28 patients (17%). After propensity score matching, the incidence of extubation recall did not significantly differ between the remimazolam and propofol anesthesia groups (15.6% vs. 18.8%; p = 1.000).
Conclusion
The incidence of extubation recall after remimazolam anesthesia with flumazenil antagonism during emergence did not significantly differ from that after propofol anesthesia.
Similar content being viewed by others
References
Popat M, Mitchell V, Dravid R, Patel A, Swampillai C, et al. Difficult Airway Society Guidelines for the management of tracheal extubation. Anaesthesia. 2012;67(3):318–40.
Inoue S, Abe R, Tanaka Y, Kawaguchi M. Anesthesia management by residents does not alter the incidence of recall of tracheal extubation: a teaching hospital-based propensity score analysis. Br J Anesth (English Edition). 2017;67(3):251–7.
Takahashi M, Nakahashi K, Karashima Y, Kitaguchi K, Furuya H. The memory of tracheal extubation during emergence from general anesthesia. Masui. 2001;50(6):613–8.
Wesolowski AM, Zaccagnino MP, Malapero RJ, Kaye AD, Urman RD. Remimazolam: pharmacologic considerations and clinical role in anesthesiology. Pharmacotherapy. 2016;36(9):1021–7.
Nordstrom O, Sandin R. Recall during intermittent propofol anaesthesia. Br J Anaesth. 1996;76(5):699–701.
Smith I, Monk TG, White PF, Ding Y. Propofol infusion during regional anesthesia: sedative, amnestic, and anxiolytic properties. Anesth Analg. 1994;79(2):313–9.
Noguchi A, Hosokawa K, Amaya F, Yokota I. Factors related to memory absence and delusional memories in patients in intensive care units managed with light sedation. Intensive Crit Care Nurs. 2020;59(8): 102830.
Sivilotti ML. Flumazenil, naloxone and the “coma cocktail.” Br J Clin Pharmacol. 2016;81(3):428–36.
Wang J, Sun P, Liang P. Neuropsychopharmacological effects of midazolam on the human brain. Brain Inform. 2020;7(1):15.
Brimacombe J. The advantages of the LMA over the tracheal tube or facemask: a meta-analysis. Can J Anaesth. 1995;42(11):1017–23.
El-Boghdadly K, Bailey CR, Wiles MD. Postoperative sore throat: a systematic review. Anaesthesia. 2016;71(6):706–17.
Acknowledgements
We thank T. Ojima (Hamamatsu University School of Medicine) for his statistical assistance. We thank Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection and analysis were performed by TS. The first draft of the manuscript was written by TS. All authors commented on the revised versions and read and approved the final manuscript
Corresponding author
Ethics declarations
Conflict of interest
None.
Prior presentation
Part of this article was presented at the 68th Annual Meeting of the Japanese Society of Anesthesiologists (June 3–4, 2021, online, Japan).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Sato, T., Mimuro, S., Kurita, T. et al. Recall of extubation after remimazolam anesthesia with flumazenil antagonism during emergence: a retrospective clinical study. J Anesth 36, 688–692 (2022). https://doi.org/10.1007/s00540-022-03093-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-022-03093-0