Abstract
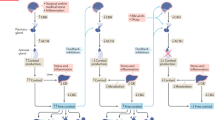
The “fight or flight” response to critical illness relies on increased cortisol availability, traditionally attributed to several-fold-increased cortisol production via hypothalamus–pituitary–adrenal-axis activation. Recent studies provided evidence against this concept with clinical implications. First, high cortisol availability during critical illness is driven by suppressed cortisol binding and reduced cortisol breakdown rather than increased cortisol production. This implies reduction of hydrocortisone doses when prescribed in ICU. Second, plasma ACTH is low, explained by feedback inhibition by peripherally driven high free cortisol and/or other central glucocorticoid-receptor ligands. Third, ICU patients have elevated plasma concentrations of the ACTH-precursor hormone, pro-opiomelanocortin, because of impaired pituitary processing into ACTH, and pro-opiomelanocortin could drive some adrenocortical cortisol production in face of low ACTH. Fourth, in prolonged critically ill patients, endogenously suppressed ACTH, aggravated by exogenous corticosteroids, associates with poor outcome. In long-stay ICU patients, central adrenal insufficiency may occur due to lack of trophic ACTH signaling. Finally, the Cosyntropin test is not suitable to assess adrenocortical reserve in ICU patients as the test is confounded by increased cortisol distribution volume. These insights necessitate further research focusing on the need, if any, of treating ICU patients with corticosteroids, and timing thereof, outside indications for pharmacological anti-inflammatory drugs.





Similar content being viewed by others
References
Téblick A, Peeters B, Langouche L, Van den Berghe G. Adrenal function and dysfunction in critically ill patients. Nat Rev Endocrinol. 2019;15:417–27.
Charmandari E, Nicolaides NC, Chrousos GP. Adrenal insufficiency. Lancet. 2014;383:2152–67.
Betterle C, Morlin L. Autoimmune Addison’s disease. Endocr Dev. 2011;20:161–72.
Annane D, Sébille V, Troché G, Raphaël JC, Gajdos P, Bellissant E. A 3-level prognostic classification in septic shock based on cortisol levels and cortisol response to corticotropin. JAMA. 2000;283:1038–45.
Annane D, Sébille V, Charpentier C, Bollaert P-E, François B, Korach J-M, Capellier G, Cohen Y, Azoulay E, Troché G, Chaumet-Riffaud Ph, Bellissant E. Effect of treatment with low doses of hydrocortisone and fludrocortisone on mortality in patients with septic shock. JAMA. 2002;288:862–71.
Annane D, Pastores SM, Rochwerg B, Arlt W, Balk RA, Beishuizen A, Briegel J, Carcillo J, Christ-Crain M, Cooper MS, Marik PE, Meduri GU, Olsen KM, Rodgers S, Russell JA, Van den Berghe G. Guidelines for the diagnosis and management of critical illness-related corticosteroid insufficiency (CIRCI) in critically ill patients (Part I): Society of Critical Care Medicine (SCCM) and European Society of Intensive Care Medicine (ESICM) 2017. Intensive Care Med. 2017;43:1751–63.
Boonen E, Vervenne H, Meersseman Ph, Andrew R, Mortier L, Declercq PE, Vanwijngaerden Y-M, Spriet I, Wouters PJ, Vander Perre S, Langouche L, Vanhorebeek I, Walker BR, Van den Berghe G. Reduced cortisol metabolism during critical illness. N Engl J Med. 2013;368:1477–88.
Boonen E, Meersseman Ph, Vervenne H, Meyfroidt G, Guïza F, Wouters PJ, Veldhuis JD, Van den Berghe G. Reduced nocturnal ACTH-driven cortisol secretion during critical illness. Am J Physiol Endocrinol Metab. 2014;306:E883–92.
Peeters B, Güiza F, Boonen E, Meersseman Ph, Langouche L, Van den Berghe G. Drug-induced HPA axis alterations during acute critical illness: a multivariable association study. Clin Endocrinol (Oxf). 2017;86:26–36.
Peeters B, Meersseman Ph, Vander Perre S, Wouters PJ, Vanmarcke D, Debaveye Y, Billen J, Vermeersch P, Langouche L, Van den Berghe G. Adrenocortical function during prolonged critical illness and beyond: a prospective observational study. Intensive Care Med. 2018;44:1720–9.
Nenke MA, Rankin W, Chapman MJ, Stevens NE, Diener KR, Hayball JD, Lewis JG, Torpy DJ. Depletion of high-affinity corticosteroid-binding globulin corresponds to illness severity in sepsis and septic shock; clinical implications. Clin Endocrinol (Oxf). 2015;82:801–7.
Jenniskens M, Weckx R, Dufour T, Vander Perre S, Pauwels L, Derde S, Téblick A, Güiza F, Van den Berghe G, Langouche L. The hepatic glucocorticoid receptor is crucial for cortisol homeostasis and sepsis survival in humans and male mice. Endocrinology. 2018;159:2790–802.
Hamrahian AH, Oseni TS, Arafah BM. Measurements of serum free cortisol in critically ill patients. N Engl J Med. 2004;350:1629–38.
Tomlinson JW, Walker EA, Bujalska IJ, Draper N, Lavery GG, Cooper MS, Hewison M, Stewart PM. 11beta-hydroxysteroid dehydrogenase type 1: a tissue-specific regulator of glucocorticoid response. Endocr Rev. 2004;25:831–66.
Nixon M, Upreti R, Andrew R. 5alpha-Reduced glucocorticoids: a story of natural selection. J Endocrinol. 2012;212:111–27.
Peeters B, Meersseman Ph, Vander Perre S, Wouters PJ, Debaveye Y, Langouche L, Van den Berghe G. ACTH and cortisol responses to CRH in acute, subacute, and prolonged critical illness: a randomized, double-blind, placebo-controlled, crossover cohort study. Intensive Care Med. 2018;44:2048–58.
Téblick A, Vander Perre S, Pauwels L, Derde S, Van Oudenhove T, Langouche L, Van den Berghe G. The role of pro-opiomelanocortin in the ACTH-cortisol dissociation of sepsis. Crit Care. 2021;25:65–79.
Jacobs A, Derese I, Vander Perre S, Wouters PJ, Verbruggen S, Billen J, Vermeersch P, Guerra GG, Joosten K, Vanhorebeek I, Van den Berghe G. Dynamics and prognostic value of the hypothalamus-pituitary-adrenal axis responses to pediatric critical illness and association with corticosteroid treatment: a prospective observational study. Intensive Care Med. 2020;46:70–81.
Boonen E, Langouche L, Janssens T, Meersseman Ph, Vervenne H, De Samblanx E, Pironet Z, Van Dyck L, Vander Perre S, Derese I, Van den Berghe G. Impact of duration of critical illness on the adrenal glands of human intensive care patients. J Clin Endocrinol Metab. 2014;99:4214–22.
Lamberts SW, Bruining HA, de Jong FH. Corticosteroid therapy in severe illness. N Engl J Med. 1997;337:1285–92.
Verstraete S, Verbruggen SC, Hordijk JA, Vanhorebeek I, Dulfer K, Güiza F, van Puffelen E, Jacobs A, Leys S, Durt A, Van Cleemput H, Eveleens RD, Garcia Guerra G, Wouters PJ, Joosten KF, Van den Berghe G. Long-term developmental effects of withholding parenteral nutrition for 1 week in the pediatric intensive care unit: a 2-year follow-up of the PEPaNIC international, randomized controlled trial. Lancet Respir Med. 2019;7:141–53.
Hermans G, Van Aerde N, Meersseman P, Van Mechelen H, Debaveye Y, Wilmer A, Gunst J, Casaer MP, Dubois J, Wouters P, Gosselink R, Van den Berghe G. Five-year mortality and morbidity impact of prolonged versus brief ICU stay: a propensity score matched cohort study. Thorax. 2019;74:1037–45.
Van Aerde N, Meersseman P, Debaveye Y, Wilmer A, Gunst J, Casaer MP, Wauters J, Wouters PJ, Gosselink R, Van den Berghe G, Hermans G. Five-year outcome of muscle weakness at intensive care unit discharge: a secondary analysis of a propensity score matched cohort study. Thorax. 2021;76:561–7.
Güiza F, Vanhorebeek I, Verstraete S, Verlinden I, Derese I, Ingels C, Dulfer K, Verbruggen SC, Garcia Guerra G, Joosten KF, Wouters PJ, Van den Berghe G. Effect of early parenteral nutrition during pediatric critical illness on DNA methylation as a potential mediator of impaired neurocognitive development: a pre-planned secondary analysis of the PEPaNIC international, randomized controlled trial. Lancet Respir Med. 2020;8:288–303.
Funding
This work was supported by the European Respiratory Society (ERS Gold Medal in ARDS), the Research Foundation Flanders (FWO) grant G091918N, the European Research Council Advanced Grant (AdvG-2017-785806) from European Union’s Horizon 2020 research and innovation program, and the Methusalem program of the Flemish Government (METH/14/06 via the KU Leuven).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Van den Berghe, G. Adrenal function/dysfunction in critically ill patients: a concise narrative review of recent novel insights. J Anesth 35, 903–910 (2021). https://doi.org/10.1007/s00540-021-02977-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-021-02977-x