Abstract
Background
Smoking is associated with many intra and postoperative events, especially respiratory complications. Hypoxemia and airway damage are found to aggravate any pre-existing respiratory pathology among smokers. One lung ventilation (OLV) carries a 4–10 % risk of development of hypoxia.
Aim
The purpose of this study was to predict the incidence of hypoxemia for smokers during OLV for patients undergoing video-assisted thoracoscopic surgery (VATS).
Patients and methods
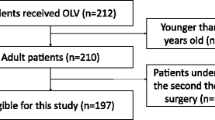
Sixty patients undergoing VATS using OLV by double lumen tube were included in this pilot cross-sectional study. These patients were divided into 2 groups, group S which included 30 heavy smoker patients (smoking more than 20 cigarettes per day for more than 20 years) and group NS which included 30 non-smoker patients. Intra and postoperative arterial oxygen tension (PaO2), arterial carbon dioxide tension (PaCO2), and intraoperative peak airway pressure were compared between the 2 groups.
Results
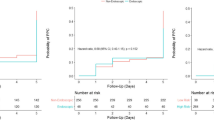
PaO2 was significantly higher in the non-smoker group than in the smoker group, both at the start and end of OLV. It was 173 ± 68 mmHg for NS compared with 74 ± 10.8 mmHg for S at the start of OLV; at the end of OLV it was 410 ± 78 mmHg for the former and 360 ± 72 mmHg for the latter (P < 0.05).
Conclusion
From this study it can be concluded that for heavy smoker patients there was a significant reduction in arterial oxygen tension (PaO2) in comparison with non-smokers. However, hypoxemia reported for both groups was comparable.
Similar content being viewed by others
References
Hawn MT, Houston TK, Campagna EJ, Graham LA, Singh J, Bishop M, Henderson WG. The attributable risk of smoking on surgical complications. Ann Surg. 2011;254(6):914–20.
Muro S. Cigarette smoking is the most important causal factor for developing chronic obstructive pulmonary disease (COPD). Nihon Rinsho. 2011;69(10):1735–40.
Vignoud L, Pin I, Boudier A, Pison C, Nadif R, Le Moual N, Slama R, Makao MN, Kauffmann F, Siroux V. Smoking and asthma: disentangling their mutual influences using a longitudinal approach. Respir Med. 2011;105(12):1805–14.
Sakamoto K, Sonobe H, Hiroi A, Tanaka H, Hino Y, Takahuta K, Ikeda T, Habara T. Influence of smoking and abdominal obesity on lung age. Rinsho Byori. 2011;59(9):831–7.
Olea E, Ferrer E, Prieto-Lloret J, Gonzalez-Martin C, Vega-Agapito V, Gonzalez-Obeso E, Agapito T, Peinado V, Obeso A, Barbera JA, Gonzalez C. Effects of cigarette smoke and chronic hypoxia on airways remodeling and resistance. Clinical significance. Respir Physiol Neurobiol. 2011;179(2–3):305–13.
Wong J, Lam DP, Abrishami A, Chan MT, Chung F. Short-term preoperative smoking cessation and postoperative complications: a systematic review and meta-analysis. Can J Anaesth. 2012;59(3):268–79.
Zaman M, Bilal H, Mahmood S, Tang A. Does getting smokers to stop smoking before lung resections reduce their risk? Interact Cardiovasc Thorac Surg. 2012;14(3):320–3.
Park HY, Sin D. Smoking kills, quitting heals: the importance of smoking cessation in COPD. Clin Respir J. 2011;5(4):185–6.
Waheedullah K, Konrad S. Hypoxemia during one-lung ventilation: prediction, prevention, and treatment. Anesthesiology. 2009;110(6):1402–11.
Schwarzkopf K, Klein U, Schreiber T, Preussler NP, Bloos F, Helfritsch H, Sauer F, Karzai W. Oxygenation during one-lung ventilation: the effects of inhaled nitric oxide and increasing levels of inspired fraction of oxygen. Anesth Analg. 2001;92:842–7.
Slinger P, Suissa S, Triolet W. Predicting arterial oxygenation during one-lung anaesthesia. Can J Anaesth. 1992;39:1030–5.
Slinger P, Triolet W, Wilson J. Improving arterial oxygenation during one-lung ventilation. Anesthesiology. 1988;68:291–5.
Hurford WE, Alfille PH. A quality improvement study of the placement and complications of double-lumen endobronchial tubes. J Cardiothorac Vasc Anesth. 1993;7:517–20.
Guenoun T, Journois D, Silleran-Chassany J, Frappier J, D’attellis N, Salem A, Safran D. Prediction of arterial oxygenation during one-lung ventilation: analysis of preoperative and intraoperative variables. J Cardiothorac Vasc Anesth. 2004;16:199–203.
Brodsky JB, Macario A, Mark JBD. Tracheal diameter predicts double-lumen tube size: a method for selecting left double-lumen tubes. Anesth Analg. 1996;82:861–4.
Chang JE, Ding D, Martin-Lazaro J, White A, Stevenson DD. Smoking, environmental tobacco smoke, and aspirin-exacerbated respiratory disease. Ann Allergy Asthma Immunol. 2012;108(1):14–9.
Rennard SI, Togo S, Holz O. Cigarette smoke inhibits alveolar repair. A mechanism for the development of emphysema. Proc Am Thorac Soc. 2006;3:703–8.
Wright JL. The importance of ultramicroscopic emphysema in cigarette smoke-induced lung disease. Lung. 2001;179:71–81.
Lu DF, Stanley C, Nunez G, Frazer D. A mathematical description of pressures in alveolar pores of Kohn. J Biomech Eng. 1991;113:104–7.
Masuko H, Sakamoto T, Kaneko Y, Iijima H, Naito T, Noguchi E, Hirota T. Lower FEV1 in non-COPD, nonasthmatic subjects: association with smoking, annual decline in FEV1, total IgE levels, and TSLP genotypes. Int J Chronic Obstr Pulm Dis. 2011;6:181–9.
Inoue S, Nishimine N, Kitaguchi K, Furuya H, Taniguchi S. Double lumen tube location predicts tube malposition and hypoxaemia during one-lung ventilation. Br J Anaesth. 2004;92(2):195–201.
Ng A, Swanevelder J. Hypoxaemia associated with one-lung anaesthesia: new discoveries in ventilation and perfusion. Br J Anaesth. 2011;106(6):761–3.
Pennefather SH, Russell GN. Placement of double lumen tubes—time to shed light on an old problem. Br J Anaesth. 2000;84:308–10.
Michelet P, Roch A, Brousse D, D’Journo X-B, Bregeon F, Lambert D, Perrin G, Papazian L, Thomas P, Carpentier J-P, Auffray J-P. Effects of PEEP on oxygenation and respiratory mechanics during one-lung ventilation. Br J Anaesth. 2005;95:267–73.
Tusman G, Bohm SH, Sipmann FS, Maisch S. Lung recruitment improves the efficiency of ventilation and gas exchange during one-lung ventilation anesthesia. Anesth Analg. 2004;98:1604–9.
Cinnella G, Grasso S, Natale C, Sollitto F, Cacciapaglia M, Angiolillo M, Pavone G, Mirabella L, Dambrosio M. Physiological effects of a lung-recruiting strategy applied during one-lung ventilation. Acta Anaesthesiol Scand. 2008;52:766–75.
Kilpatrick B, Slinger P. Lung protective strategies in anaesthesia. Br J Anaesth. 2010;105:i108–16.
Brodsky JB, Lemmens HJ. Left double-lumen tubes: clinical experience with 1,170 patients. J Cardiothorac Vasc Anesth. 2003;17:289–98.
Pfitzner J, Pfitzner L. The theoretical basis for using apnoeic oxygenation via the nonventilated lung during one-lung ventilation to delay the onset of arterial hypoxaemia. Anaesth Intensive Care. 2005;33:794–800.
Slinger P. Pro: low tidal volume is indicated during one-lung ventilation. Anesth Analg. 2006;103:268–70.
Lohser J. One-lung ventilation calls for one-lung recruitment. Anesth Analg. 2007;104:220.
Bardoczky GI, Yernault JC, Engelman EE, Velghe CE, Cappello M, Hollander AA. Intrinsic positive end-expiratory pressure during one-lung ventilation for thoracic surgery: the influence of preoperative pulmonary function. Chest. 1996;110:180–4.
Bardoczky GI, d’Hollander AA, Rocmans P, Estenne M, Yernault JC. Respiratory mechanics and gas exchange during one-lung ventilation for thoracic surgery: the effects of end-inspiratory pause in stable COPD patients. J Cardiothorac Vasc Anesth. 1998;12:137–41.
Ducros L, Moutafis M, Castelain MH, Liu N, Fischler M. Pulmonary air trapping during two-lung and one-lung ventilation. J Cardiothorac Vasc Anesth. 1999;13:35–9.
Wrigge H, Uhlig U, Zinserling J, Behrends-Callsen E, Ottersbach G, Fischer M, Uhlig S, Putensen C. The effects of different ventilatory settings on pulmonary and systemic inflammatory responses during major surgery. Anesth Analg. 2004;98:775–81.
Warner DO. Preventing postoperative pulmonary complications. Anesthesiology. 2000;92:1467–72.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Khalil, M.A. Smoking as a risk factor for intraoperative hypoxemia during one lung ventilation. J Anesth 27, 550–556 (2013). https://doi.org/10.1007/s00540-013-1559-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-013-1559-y