Abstract
Background
Post-transplant outcomes for acute liver failure (ALF) are unsatisfactory, and there are debates about the most suitable type of graft. Given the critical shortage of donor organs, accurate assessment of post-transplant outcome in ALF patients is crucial to avoid a futile liver transplantation (LT).
Methods
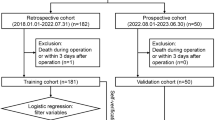
A database of 160 consecutive adult ALF patients who underwent primary LT between 2000 and 2009 in a tertiary LT center was analyzed.
Results
The most common causes of ALF were hepatitis B virus infection (30%) and herbal/folk medicine use (30%). Thirty-six (22.5%) and 124 (77.5%) patients underwent deceased-donor LT (DDLT) and adult-to-adult living-donor LT (LDLT), respectively. During a median follow-up period of 38 (range 1–132) months, the DDLT and LDLT groups showed similar patient (P = 0.99) and graft (P = 0.97) survival rates. The overall 1- and 3-year patient survival rates were 78.8 and 74.6%, respectively. Five predictors of patient survival were identified by bootstrapping and multivariate analysis: vasopressor requirement, estimated glomerular filtration rate, serum sodium concentration, recipient age, and donor age, at the time of transplant. By summing scores weighted in each of these predictor categories, we designed a prognostic scoring system (scores from −2 to 20) that estimated 1-year post-transplant mortality from 0 to 100% (c statistic 0.79).
Conclusions
Long-term outcomes after LDLT and DDLT were comparable in adult patients with ALF. A simple prognostic scoring system that includes 5 predictive variables at the time of LT may help estimate post-transplant survival in ALF patients, regardless of the type of transplant.


Similar content being viewed by others
Abbreviations
- ALF:
-
Acute liver failure
- APAP:
-
Acetaminophen
- BMI:
-
Body mass index
- DDLT:
-
Deceased-donor liver transplantation
- ESLD:
-
End-stage liver disease
- GFR:
-
Glomerular filtration rate
- GRWR:
-
Graft-to-recipient weight ratio
- HAV:
-
Hepatitis A virus
- HBV:
-
Hepatitis B virus
- HR:
-
Hazard ratio
- INR:
-
International normalized ratio
- IQR:
-
Inter-quartile range
- KONOS:
-
Korean Network for Organ Sharing
- LDLT:
-
Living-donor liver transplantation
- LT:
-
Liver transplantation
- MDRD:
-
Modification of diet in renal disease
- MELD:
-
Model for end-stage liver disease
- PH:
-
Proportional hazards
- ROC:
-
Receiver operating characteristic
- USN:
-
Ultrasonography
References
Polson J, Lee WM. AASLD position paper: the management of acute liver failure. Hepatology. 2005;41:1179–97.
Ostapowicz G, Fontana RJ, Schiodt FV, Larson A, Davern TJ, Han SH, et al. Results of a prospective study of acute liver failure at 17 tertiary care centers in the United States. Ann Intern Med. 2002;137:947–54.
Campsen J, Blei AT, Emond JC, Everhart JE, Freise CE, Lok AS, et al. Outcomes of living donor liver transplantation for acute liver failure: the adult-to-adult living donor liver transplantation cohort study. Liver Transplant. 2008;14:1273–80.
Liu CL, Fan ST, Lo CM, Yong BH, Fung AS, Wong J. Right-lobe live donor liver transplantation improves survival of patients with acute liver failure. Br J Surg. 2002;89:317–22.
Uemoto S, Inomata Y, Sakurai T, Egawa H, Fujita S, Kiuchi T, et al. Living donor liver transplantation for fulminant hepatic failure. Transplantation. 2000;70:152–7.
Park SJ, Lim YS, Hwang S, Heo NY, Lee HC, Suh DJ, et al. Emergency adult-to-adult living-donor liver transplantation for acute liver failure in a hepatitis B virus endemic area. Hepatology. 2010;51(3):903–11.
Roberts MS, Angus DC, Bryce CL, Valenta Z, Weissfeld L. Survival after liver transplantation in the United States: a disease-specific analysis of the UNOS database. Liver Transplant. 2004;10:886–97.
Burroughs AK, Sabin CA, Rolles K, Delvart V, Karam V, Buckels J, et al. 3-Month and 12-month mortality after first liver transplant in adults in Europe: predictive models for outcome. Lancet. 2006;367:225–32.
Polson J. Assessment of prognosis in acute liver failure. Semin Liver Dis. 2008;28:218–25.
Liou IW, Larson AM. Role of liver transplantation in acute liver failure. Semin Liver Dis. 2008;28:201–9.
Barshes NR, Lee TC, Balkrishnan R, Karpen SJ, Carter BA, Goss JA. Risk stratification of adult patients undergoing orthotopic liver transplantation for fulminant hepatic failure. Transplantation. 2006;81:195–201.
Bernal W, Cross TJ, Auzinger G, Sizer E, Heneghan MA, Bowles M, et al. Outcome after wait-listing for emergency liver transplantation in acute liver failure: a single centre experience. J Hepatol. 2009;50:306–13.
Kamath PS, Wiesner RH, Malinchoc M, Kremers W, Therneau TM, Kosberg CL, et al. A model to predict survival in patients with end-stage liver disease. Hepatology. 2001;33:464–70.
Levey AS, Coresh J, Greene T, Stevens LA, Zhang YL, Hendriksen S, et al. Using standardized serum creatinine values in the modification of diet in renal disease study equation for estimating glomerular filtration rate. Ann Intern Med. 2006;145:247–54.
Sauerbrei W, Schumacher M. A bootstrap resampling procedure for model building: application to the Cox regression model. Stat Med. 1992;11:2093–109.
Sullivan LM, Massaro JM, D’Agostmo RB. Presentation of multivariate data for clinical use: The Framingham Study risk score functions. Stat Med. 2004;23:1631–60.
Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology. 1982;143:29–36.
Hosmer DW, Lemeshow S. Applied logistic regression. 2nd ed. New York: Wiley; 2000.
Harrell FE Jr, Lee KL, Mark DB. Multivariable prognostic models: issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat Med. 1996;15:361–87.
Wiesner R, Edwards E, Freeman R, Harper A, Kim R, Kamath P, et al. Model for end-stage liver disease (MELD) and allocation of donor livers. Gastroenterology. 2003;124:91–6.
Earl TM, Chari RS. Which types of graft to use in patients with acute liver failure? (A) Auxiliary liver transplant (B) Living donor liver transplantation (C) The whole liver. (C) I take the whole liver only. J Hepatol. 2007;46:578–82.
Hwang S, Lee SG, Ahn CS, Kim KH, Moon DB, Ha TY, et al. An increase in deceased donor incidence alleviated the need for urgent adult living donor liver transplantation in a Korean high-volume center. Transplant Proc. 2010;42:1497–501.
Bernal W, Wendon J, Rela M, Heaton N, Williams R. Use and outcome of liver transplantation in acetaminophen-induced acute liver failure. Hepatology. 1998;27:1050–5.
Bjoro K, Ericzon BG, Kirkegaard P, Hockerstedt K, Soderdahl G, Olausson M, et al. Highly urgent liver transplantation: possible impact of donor-recipient ABO matching on the outcome after transplantation. Transplantation. 2003;75:347–53.
Wigg AJ, Gunson BK, Mutimer DJ. Outcomes following liver transplantation for seronegative acute liver failure: experience during a 12-year period with more than 100 patients. Liver Transplant. 2005;11:27–34.
Devlin J, Wendon J, Heaton N, Tan KC, Williams R. Pretransplantation clinical status and outcome of emergency transplantation for acute liver failure. Hepatology. 1995;21:1018–24.
Riordan SM, Williams R. Mechanisms of hepatocyte injury, multiorgan failure, and prognostic criteria in acute liver failure. Semin Liver Dis. 2003;23:203–15.
Gonwa TA, Jennings L, Mai ML, Stark PC, Levey AS, Klintmalm GB. Estimation of glomerular filtration rates before and after orthotopic liver transplantation: evaluation of current equations. Liver Transplant. 2004;10:301–9.
Cocchetto DM, Tschanz C, Bjornsson TD. Decreased rate of creatinine production in patients with hepatic disease: implications for estimation of creatinine clearance. Ther Drug Monit. 1983;5:161–8.
Biggins SW, Kim WR, Terrault NA, Saab S, Balan V, Schiano T, et al. Evidence-based incorporation of serum sodium concentration into MELD. Gastroenterology. 2006;130:1652–60.
Lim YS, Larson TS, Benson JT, Kamath PS, Kremers WK, Therneau TM, et al. Serum sodium, renal function, and survival of patients with end-stage liver disease. J Hepatol. 2010;52:523–8.
Yun BC, Kim WR, Benson JT, Biggins SW, Therneau TM, Kremers WK, et al. Impact of pretransplant hyponatremia on outcome following liver transplantation. Hepatology. 2009;49:1610–5.
Dawwas MF, Lewsey JD, Neuberger JM, Gimson AE. The impact of serum sodium concentration on mortality after liver transplantation: a cohort multicenter study. Liver Transplant. 2007;13:1115–24.
Londono MC, Guevara M, Rimola A, Navasa M, Taura P, Mas A, et al. Hyponatremia impairs early posttransplantation outcome in patients with cirrhosis undergoing liver transplantation. Gastroenterology. 2006;130:1135–43.
Simpson KJ, Bates CM, Henderson NC, Wigmore SJ, Garden OJ, Lee A, et al. The utilization of liver transplantation in the management of acute liver failure: comparison between acetaminophen and non-acetaminophen etiologies. Liver Transplant. 2009;15:600–9.
Acknowledgments
The authors thank Drs. Ki-Hun Kim, Chul-Soo Ahn, Duk-Bog Moon, Tae-Yong Ha, Gi-Won Song, Dong-Hwan Jung, Eunsil Yu, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Hwa Chung, and Yung Sang Lee for their help in data collection.
Conflict of interest
None of the authors have any potential conflicts of interest to disclose that are relevant to this manuscript, and the study was not funded by any commercial organization.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jin, YJ., Lim, YS., Han, S. et al. Predicting survival after living and deceased donor liver transplantation in adult patients with acute liver failure. J Gastroenterol 47, 1115–1124 (2012). https://doi.org/10.1007/s00535-012-0570-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-012-0570-7