Abstract
Introduction
Self-administered methoxyflurane, also known as Penthrox, at a sub-anesthetic dose is a short-term, fast-acting, and safe analgesic that may provide suitable pain relief for cancer patients. This review aims to compile the existing evidence on methoxyflurane and its efficacy in reducing pain during cancer-related procedures.
Methods
A literature search was conducted through OVID Medline and Embase. The search was limited to articles published between 2012 and 2021 and studies were included if they assessed the efficacy of methoxyflurane to reduce pain in cancer-related procedures. All types of cancer were included.
Results
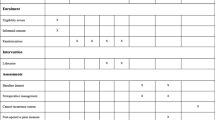
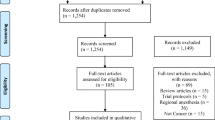
The literature search yielded seven studies published between 2012 and 2021. The studies analyzed assessed methoxyflurane use in prostate biopsy, colonoscopy, removal of brachytherapy rods, and bone marrow biopsy. Various research designs were employed, including three randomized controlled trials, two prospective observational studies, one retrospective, and one non-randomized controlled trial. In all, methoxyflurane has a demonstrated ability to reduce pain in these procedures.
Conclusion
In the limited studies available in evaluating the efficacy of methoxyflurane for reducing procedural pain during cancer-related procedures, all have demonstrated clinical equivalency or superiority. Pain relief appears to be equivalent however methoxyflurane overcomes the standard limitations of respiratory sedation and has demonstrated quicker procedural recovery times than traditional sedation methods. The accumulated data to date supports the use of methoxyflurane which can supplement or supplant current methods of analgesia in cancer-related procedures.

Similar content being viewed by others
References
Grummet J, Huang S, Konstantatos A, Frydenberg M (2012) The “green whistle”: a novel method of analgesia for transrectal prostate biopsy. BJU Int 110:85–88. https://doi.org/10.1111/j.1464-410X.2012.11613.x
Gaskell AL, Jephcott CG, Smithells JR, Sleigh JW (2016) Self-administered methoxyflurane for procedural analgesia: experience in a tertiary Australasian centre. Anaesthesia 71(4):417–423. https://doi.org/10.1111/anae.13377
Nguyen NQ, Toscano L, Lawrence M, Moore J, Holloway RH, Bartholomeusz D, Lidums I, Tam W, Roberts-Thomson IC, Mahesh VN, Debreceni TL, Schoeman MN (2013) Patient-controlled analgesia with inhaled methoxyflurane versus conventional endoscopist-provided sedation for colonoscopy: a randomized multicenter trial. Gastrointest Endosc 78(6):892–901. https://doi.org/10.1016/j.gie.2013.05.023
Lee C, Woo HH (2015) Penthrox inhaler analgesia in transrectal ultrasound-guided prostate biopsy: Penthrox inhaler analgesia in TRUSPB. ANZ J Surg 85(6):433–437. https://doi.org/10.1111/ans.12694
Huang S, Pepdjonovic L, Konstantatos A, Frydenberg M, Grummet J (2016) Penthrox alone versus Penthrox plus periprostatic infiltration of local analgesia for analgesia in transrectal ultrasound-guided prostate biopsy. ANZ J Surg 86(3):139–142. https://doi.org/10.1111/ans.12974
Spruyt O, Westerman D, Milner A, Bressel M, Wein S (2014) A randomised, double-blind, placebo-controlled study to assess the safety and efficacy of methoxyflurane for procedural pain of a bone marrow biopsy. BMJ Support Palliat Care 4(4):342–348. https://doi.org/10.1136/bmjspcare-2013-000447
Hayne D, Grummet J, Espinoza D et al (2021) ‘Pain-free TRUS B’: a phase 3 double-blind placebo-controlled randomized trial of methoxyflurane with periprostatic local anaesthesia to reduce the discomfort of transrectal ultrasonography-guided prostate biopsy (ANZUP 1501). BJU Int 129:591–600. https://doi.org/10.1111/bju.15552
Greco MT, Roberto A, Corli O, Deandrea S, Bandieri E, Cavuto S et al (2014) Quality of cancer pain management: an update of a systematic review of undertreatment of patients with cancer. J Clin Oncol 32(36):4149–4154. https://doi.org/10.1200/JCO.2014.56.0383
Dayan AD (2016) Analgesic use of inhaled methoxyflurane: evaluation of its potential nephrotoxicity. Hum Exp Toxicol 35(1):91–100. https://doi.org/10.1177/0960327115578743
Allison SJ, Docherty PD, Pons D, Chase JG (2021) Methoxyflurane toxicity: historical determination and lessons for modern patient and occupational exposure. N Z Med J 134(1534):76–90
Ruff R, Kerr S, Kerr D, Zalcberg D, Stevens J (2018) Occupational exposure to methoxyflurane administered for procedural sedation: an observational study of 40 exposures. BJA 120(6):1435–1437. https://doi.org/10.1016/j.bja.2018.01.029
Jephcott C, Grummet J, Nguyen N, Spruyt O (2018) A review of the safety and efficacy of inhaled methoxyflurane as an analgesic for outpatient procedures. Br J Anaesth 120(5):1040–1048. https://doi.org/10.1016/j.bja.2018.01.011
Author information
Authors and Affiliations
Contributions
Samuel Finkelstein: co primary author Etinosa Oliogu: co primary author Albert Yee: editing, manuscript review Lauren Milton: screening of articles PRISMA guidelines, co author Leon Rivlin: conception and design, manuscript review Patrick Henry: literature review, editing Tara Behroozian: screening of articles according to PRISMA guidelines, co author Edward Chow: conception and design, editing Joel Finkelstein: senior responsible investigator, manuscript review, editing.
Corresponding author
Ethics declarations
Ethics approval
Ethical approval was not required for this study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Finkelstein, S., Oliogu, E., Yee, A. et al. Literature review on the use of methoxyflurane in the management of pain in cancer-related procedures. Support Care Cancer 31, 232 (2023). https://doi.org/10.1007/s00520-023-07694-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-07694-7