Abstract
Purpose
Over the past 2 decades, cancer has been the leading cause of death worldwide. Accordingly, cancer patients are the largest group of patients admitted to a hospice, accounting for 40% of overall hospice admissions every year. Therefore, the purpose of this systematic review is to investigate the outcomes of caring for cancer patients at hospices.
Methods
PubMed, Scopus, and Web of Science databases were searched for English language articles published during the period from January 2008 to January 2022. The keywords used to search in this systematic review were included hospice, cancer, and neoplasm (for PubMed search only), which were searched in the titles and abstracts of the articles.
Results
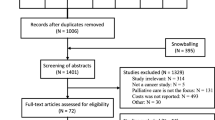
Out of 803 articles found in the initial search, 38 were selected based on inclusion criteria. The studies indicated that hospice care resulted in outcomes such as reduced referral and admission to the emergency department (only one study reporting opposite results), reduced length and number of hospital admissions, reduced use of chemotherapy and radiotherapy, increased pain reports, improved pain management, enhanced end-of-life quality, significantly reduced cost of treatment, reduced number of invasive interventions, death at home, increased survival and satisfaction of patients, and poor nutritional support.
Conclusion
Given the numerous and significant benefits of care in a hospice for cancer patients, health managers are recommended to consider developing hospices and introducing patients to these centers. Besides, they need to compensate for some shortcomings by, for example, providing better nutritional support and developing a care plan based on the type of cancers that the patients are suffering in hospices so that more specialized services can be delivered.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, Dr. Hanie Dahmardeh, upon reasonable request.
Code availability
N/A.
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A (2015) Global cancer statistics, 2012. CA: Cancer J Clin 65(2):87–108. https://doi.org/10.3322/caac.21262
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clin 68(6):394–424. https://doi.org/10.3322/caac.21492
Loke SS, Rau KM, Huang CF (2011) Impact of combined hospice care on terminal cancer patients. J Palliat Med 14(6):683–687. https://doi.org/10.1089/jpm.2010.0331
Loke SS, Rau KM (2011) Differences between inpatient hospice care and in-hospital nonhospice care for cancer patients. Cancer Nurs 34(3):E21–E26. https://doi.org/10.1097/NCC.0b013e3181ff78b6
Paris J, Morrison RS (2014) Evaluating the effects of inpatient palliative care consultations on subsequent hospice use and place of death in patients with advanced GI cancers. Journal of Oncology Practice 10(3):174–177. https://doi.org/10.1200/JOP.2014.001429
Negarandeh R, Mardani Hamooleh M, Rezaee N (2015) Concept Analysis of Palliative Care in Nursing: Introducing a Hybrid Model. J Mazandaran Univ Med Sci 25 (130):40-51. http://jmums.mazums.ac.ir/article-1-6392-en.htm
Wright AA, Hatfield LA, Earle CC, Keating NL (2014) End-of-life care for older patients with ovarian cancer is intensive despite high rates of hospice use. J Clin Oncol 32(31):3534–3539. https://doi.org/10.1200/jco.2014.55.5383
Cagle JG, Pek J, Clifford M, Guralnik J, Zimmerman S (2015) Correlates of a good death and the impact of hospice involvement: findings from the national survey of households affected by cancer. Support Care Cancer 23(3):809–818. https://doi.org/10.1007/s00520-014-2404-z
Monroe TB, Carter MA, Feldt KS, Dietrich MS, Cowan RL (2013) Pain and hospice care in nursing home residents with dementia and terminal cancer. Geriatr Gerontol Int 13(4):1018–1025. https://doi.org/10.1111/ggi.12049
Huskamp HA, Keating NL, Malin JL, Zaslavsky AM, Weeks JC, Earle CC et al (2009) Discussions with physicians about hospice among patients with metastatic lung cancer. Arch Intern Med 169(10):954–962. https://doi.org/10.1001/archinternmed.2009.127
Fairfield KM, Murray KM, Wierman HR, Han PK, Hallen S, Miesfeldt S et al (2012) Disparities in hospice care among older women dying with ovarian cancer. Gynecol Oncol 125(1):14–18. https://doi.org/10.1016/j.ygyno.2011.11.041
Choi YS, Yim E, Tae Y, Kim A (2016) Satisfaction with hospital care services and changes experienced after hospitalization among the cancer patients of general cancer wards and hospice wards in South Korea. Indian J Sc Technol 9:46. https://doi.org/10.17485/ijst/2016/v9i46/107851
Carlson MD, Herrin J, Du Q, Epstein AJ, Barry CL, Morrison RS et al (2010) Impact of hospice disenrollment on health care use and medicare expenditures for patients with cancer. J Clin Oncol 28(28):4371–4375. https://doi.org/10.1200/jco.2009.26.1818
Shiovitz S, Bansal A, Burnett-Hartman AN, Karnopp A, Adams SV, Warren-Mears V et al (2015) Cancer-directed therapy and hospice care for metastatic cancer in American Indians and Alaska Natives. Cancer Epidemiol Biomark Prev 24(7):1138–1143. https://doi.org/10.1158/1055-9965.epi-15-0251
Enomoto LM, Schaefer EW, Goldenberg D, Mackley H, Koch WM, Hollenbeak CS (2015) The cost of hospice services in terminally Ill patients with head and neck cancer. JAMA Otolaryngol Head Neck Surg 141(12):1066–1074. https://doi.org/10.1001/jamaoto.2015.2162
Wang YM, Guo HQ (2012) Follow-up study of survival of patients with advanced cancer in a hospice setting. Asian Pac J Cancer Prev 13(7):3357–3360. https://doi.org/10.7314/apjcp.2012.13.7.3357
Saito AM, Landrum MB, Neville BA, Ayanian JZ, Weeks JC, Earle CC (2011) Hospice care and survival among elderly patients with lung cancer. J Palliat Med 14(8):929–939. https://doi.org/10.1089/jpm.2010.0522
Obermeyer Z, Clarke AC, Makar M, Schuur JD, Cutler DM (2016) Emergency care use and the medicare hospice benefit for individuals with cancer with a poor prognosis. J Am Geriatr Soc 64(2):323–329. https://doi.org/10.1111/jgs.13948
Karikari-Martin P, McCann JJ, Farran CJ, Hebert LE, Haffer SC, Phillips M (2016) Race, Any cancer, income, or cognitive function: what inf luences hospice or aggressive services use at the end of life among community-dwelling medicare beneficiaries? Am J Hosp Palliat Care 33(6):537–545. https://doi.org/10.1177/1049909115574263
Chang H, Lin M, Chen C, Chen T, Tsai S, Cheng S et al (2016) Medical care utilization and costs on end-of-life cancer patients: the role of hospice care. Medicine (Baltimore) 95(44):e5216. https://doi.org/10.1097/MD.0000000000005216
Bergman J, Saigal CS, Lorenz KA, Hanley J, Miller DC, Gore JL et al (2011) Hospice use and high-intensity care in men dying of prostate cancer. Arch Intern Med 171(3):204–210. https://doi.org/10.1001/archinternmed.2010.394
Tan WS, Lee A, Yang SY, Chan S, Wu HY, Ng CWL et al (2016) Integrating palliative care across settings: a retrospective cohort study of a hospice home care programme for cancer patients. Palliat Med 30(7):634–641. https://doi.org/10.1177/0269216315622126
Chiang JK, Lee YC, Kao YH (2017) Trend analysis of end-of-life care between hospice and nonhospice groups of cancer patients in Taiwan for 2002-11. Medicine (Baltimore).96(34):e7825. https://doi.org/10.1097/MD.0000000000007825
Obermeyer Z, Makar M, Abujaber S, Dominici F, Block S, Cutler DM (2014) Association between the Medicare hospice benefit and health care utilization and costs for patients with poor-prognosis cancer. JAMA 312(18):1888–1896. https://doi.org/10.1001/jama.2014.14950
Kang SC, Lin MH, Hwang IH, Lin MH, Chang HT, Hwang SJ (2012) Impact of hospice care on end-of-life hospitalization of elderly patients with lung cancer in Taiwan. J Chin Med Assoc 75(5):221–226. https://doi.org/10.1016/j.jcma.2012.04.005
Bentur N, Resnizky S, Balicer R, Eilat-Tsanani T (2014) Utilization and cost of services in the last 6 months of life of patients with cancer - with and without home hospice care. Am J Hosp Palliat Care 31(7):723–725. https://doi.org/10.1177/1049909113499604
Kao YH, Chiang JK (2015) Effect of hospice care on quality indicators of end-of-life care among patients with liver cancer: a national longitudinal population-based study in Taiwan 2000–2011. BMC Palliat Care 14:39. https://doi.org/10.1186/s12904-015-0036-9
Wang HM, Koong SL, Hsiao SC, Chen JS, Liu TW, Tang ST (2011) Impact of availability of an inpatient hospice unit on the parent hospital’s quality of palliative care for Taiwanese cancer decedents, 2001–2006. J Pain Symptom Manage 42(3):400–409. https://doi.org/10.1016/j.jpainsymman.2010.12.011
Duggan KT, Hildebrand Duffus S, D’Agostino RB Jr, Petty WJ, Streer NP, Stephenson RC (2017) The Impact of Hospice Services in the Care of Patients with Advanced Stage Nonsmall Cell Lung Cancer. J Palliat Med 20(1):29–34. https://doi.org/10.1089/jpm.2016.0064
Kumar P, Wright AA, Hatfield LA, Temel JS, Keating NL (2017) Family Perspectives on Hospice Care Experiences of Patients with Cancer. Journal of clinical oncology : official journal of the American Society of Clinical Oncology 35(4):432–439. https://doi.org/10.1200/JCO.2016.68.9257
Huang KS, Wang SH, Chuah SK, Rau KM, Lin YH, Hsieh MC et al (2017) The effects of hospice-shared care for gastric cancer patients. PLoS ONE 12(2):e0171365. https://doi.org/10.1371/journal.pone.0171365
Chiang JK, Kao YH, Lai NS (2015) The impact of hospice care on survival and healthcare costs for patients with lung cancer: a national longitudinal population-based study in Taiwan. PLoS ONE 10(9):e0138773. https://doi.org/10.1371/journal.pone.0138773
Hunnicutt JN, Tjia J, Lapane KL (2017) Hospice use and pain management in elderly nursing home residents with cancer. J Pain Symptom Manage 53(3):561–570. https://doi.org/10.1016/j.jpainsymman.2016.10.369
Deng D, Lin W, Law F (2015) The study on evaluation and improvement of quality of life in patients with advanced cancer by China’s hospice program. Am J Hosp Palliat Care 32(4):365–371. https://doi.org/10.1177/1049909114523331
Yoon S, Scarton L, Duckworth L, Yao Y, Ezenwa M, Suarez M et al (2021) Pain, symptom distress, and pain barriers by age among patients with cancer receiving hospice care: Comparison of baseline data. J Geriatr Oncol 12(7):1068–1075. https://doi.org/10.1016/j.jgo.2021.04.008
Dai Y, Huang Y, Lai M, Liu H, Shiao C (2021) Optimal timing for hospice-shared care initiation in terminal cancer patients. Support Care Cancer 29(11):6871–6880. https://doi.org/10.1007/s00520-021-06284-9
Lin WY, Chiu TY, Ho CT, Davidson LE, Hsu HS, Liu CS et al (2014) Hospice shared-care saved medical expenditure and reduced the likelihood of intensive medical utilization among advanced cancer patients in Taiwan–a nationwide survey. Support Care Cancer 22(7):1907–1914. https://doi.org/10.1007/s00520-014-2168-5
Sammon JD, McKay RR, Kim SP, Sood A, Sukumar S, Hayn MH et al (2015) Burden of hospital admissions and utilization of hospice care in metastatic prostate cancer patients. Urology 85(2):343–349. https://doi.org/10.1016/j.urology.2014.09.053
Shao YY, Hsiue EHC, Hsu CH, Yao CA, Chen HM, Lai MS et al (2017) National policies fostering hospice care increased hospice utilization and reduced the invasiveness of end-of-life care for cancer patients. Oncologist 22(7):843–849. https://doi.org/10.1634/theoncologist.2016-0367
Chiang JK, Kao YH (2016) Impact of home hospice care on patients with advanced lung cancer: a longitudinal population-based study in Taiwan. J Palliat Med 19(4):380–386. https://doi.org/10.1089/jpm.2015.0278
Kim SJ, Han KT, Kim TH, Park EC (2015) Does hospital need more hospice beds? Hospital charges and length of stays by lung cancer inpatients at their end of life: a retrospective cohort design of 2002–2012. Palliat Med 29(9):808–816. https://doi.org/10.1177/0269216315582123
Kim JH, Kim SM, Joo JS, Lee KS (2012) Factors associated with medical cost among patients with terminal cancer in hospice units. J Palliat Care 28(1):5–12. https://doi.org/10.1177/082585971202800102
Chou C, Lai W, Pan B, Yang Y, Huang K (2021) Effects of hospice care for terminal head and neck cancer patients: a nationwide population-based matched cohort study. J Palliat Med 24(9):1299–1306. https://doi.org/10.1089/jpm.2020.0375
Kalidindi Y, Jung J, Segel J, Leslie D (2020) Impact of length of hospice on spending and utilization among medicare beneficiaries with lung cancer. Am J Hosp Palliat Care 37(11):918–924. https://doi.org/10.1177/1049909120909304
Mor V, Wagner T, Levy C, Ersek M, Miller S, Gidwani-Marszowski R et al (2019) Association of Expanded VA Hospice care with aggressive care and cost for veterans with advanced lung cancer. JAMA Oncol 5(6):810–816. https://doi.org/10.1001/jamaoncol.2019.0081
Amano K, Maeda I, Morita T, Tatara R, Katayama H, Uno T et al (2016) Need for nutritional support, eating-related distress and experience of terminally ill patients with cancer: a survey in an inpatient hospice. BMJ Support Palliat Care 6(3):373–376. https://doi.org/10.1136/bmjspcare-2014-000783
Blauwhoff-Buskermolen S, Ruijgrok C, Ostelo RW, de Vet HC, Verheul HM, de van der Schueren MA et al (2016) The assessment of anorexia in patients with cancer: cut-off values for the FAACT–A/CS and the VAS for appetite. Supportive Care Cancer. 24(2):661–6. https://doi.org/10.1007/s00520-015-2826-2
LeBlanc TW, Abernethy AP, Casarett DJ (2015) What is different about patients with hematologic malignancies? A retrospective cohort study of cancer patients referred to a hospice research network. J Pain Symptom Manage 49(3):505–512
Author information
Authors and Affiliations
Contributions
All listed authors significantly contributed to this project. Study protocol was developed by AZ, HD, and SS. AZ and SS carried out study selection and data extraction. AZ and SS provided the content expertise for study design and participated in writing the discussion section of the manuscript. HD is the reference librarian who conducted the literature search. SS provided the methodological expertise and supervised the work. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
N/A
Consent to participate
N/A
Consent for publication
We give our consent for the publication of identifiable details, which can include photograph(s) and/or videos and/or case history and/or details within the text (“Material”) to be published in the above Journal and Article.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sharafi, S., Ziaee, A. & Dahmardeh, H. What are the outcomes of hospice care for cancer patients? A systematic review. Support Care Cancer 31, 64 (2023). https://doi.org/10.1007/s00520-022-07524-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-022-07524-2