Abstract
Purpose
Cancer patients were particularly vulnerable to the adverse impacts of the COVID-19 pandemic given their reliance on the healthcare system, and their weakened immune systems. This systematic review examines the social, psychological, and economic impacts of COVID-19 on cancer patients.
Methods
The systematic search, conducted in March 2021, captures the experience of COVID-19 Wave I, when the most severe restrictions were in place globally, from a patient perspective.
Results
The search yielded 56 studies reporting on the economic, social, and psychological impacts of COVID-19. The economic burden associated with cancer for patients during the pandemic included direct and indirect costs with both objective (i.e. financial burden) and subjective elements (financial distress). The pandemic exasperated existing psychological strain and associated adverse outcomes including worry and fear (of COVID-19 and cancer prognosis); distress, anxiety, and depression; social isolation and loneliness. National and institutional public health guidelines to reduce COVID-19 transmission resulted in suspended cancer screening programmes, delayed diagnoses, postponed or deferred treatments, and altered treatment. These altered patients’ decision making and health-seeking behaviours.
Conclusion
COVID-19 compounded the economic, social, and psychological impacts of cancer on patients owing to health system adjustments and reduction in economic activity. Identification of the impact of COVID-19 on cancer patients from a psychological, social, and economic perspective following the pandemic can inform the design of timely and appropriate interventions and supports, to deal with the backlog in cancer care and enhance recovery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cancer is a leading cause of death globally, with almost 10 million deaths and 19.3 million incidences worldwide in 2020 [1]. This has a significant economic burden globally, estimated at $1.16 trillion in 2010 [2]. Such cost estimates capture expenditure on several types of cancer care, depending on prevalence, treatment patterns, and pharmaceutical spend. However, the economic burden of cancer extends beyond the costs of healthcare delivery. Patients and survivors also face objective costs (i.e. financial burden), arising from out-of-pocket payments. These vary depending on the public healthcare system in which they are treated, and insurance coverage. Additionally, there are subjective costs (financial distress) [3], which incorporates the psychological consequences and coping behaviours associated with the financial burden of cancer. Financial distress has adverse effects on health outcomes, collectively affecting quality of life (QoL) and well-being [3]. Recently, the COVID-19 pandemic disrupted health services globally. Cancer patients were particularly vulnerable to its adverse impacts given their reliance on the healthcare system, and their weakened immune systems.
Here, we investigate the social, psychological, and economic costs of the pandemic on cancer patients. National and institutional public health guidelines issued to protect against COVID-19 both influenced cancer care. Stay-at-home orders, social distancing, reconfigured healthcare delivery, reduced healthcare capacity, and re-distributed resources were needed to meet the demands of COVID-19. This in turn negatively impacted cancer care.
This systematic review examines the social, psychological, and economic impacts of COVID-19 on cancer patients. The systematic search, conducted in March 2021, captures the experience of COVID-19 Wave I, when the most severe restrictions were in place globally. Taking a patient perspective, the findings provide reflections on how cancer care for patients undergoing treatment was affected by the pandemic. Consideration is given to innovations arising during the pandemic and lessons learned for designing future developments and supports, which are to mitigate the social, psychological, and economic impacts associated with cancer.
Methods
Study selection criteria
This systematic review was conducted in accordance with the principles of conducting systematic reviews [4]. The PICOCS framework (i.e. population, intervention, comparators, outcomes, context, studies) was used to support inclusion criteria [5] (see Table 1). (There was a minor adaptation including “context” and excluding “comparator” as it was not applicable.) Studies published between January 2020 and March 2021 examining the impact of the COVID-19 pandemic on adult cancer patients undergoing treatment and survivors (2 years post-diagnosis) were examined. Inclusion and exclusion criteria are outlined in Table 1. Studies included were limited to those written in English and focused on the economic, social, and psychological implications of COVID-19 on cancer patients/survivors. Table 2
Literature search strategy
A comprehensive search strategy was employed using a combination of free-text words and subject headings relevant to CINAHL, MEDLINE, PsycINFO, PsycArticles, and EMBASE databases and refined using Boolean operators. Searches were performed on the 31st of March 2021. Full search terms and combinations are provided in Appendices 1 and 2. The search protocol was registered (CRD42021246651).
Data extraction and quality assessment
Data extraction is presented in tabular format to assist reporting uniformity, reproducibility, and minimising bias (provided on Table 3). The evidence was combined and summarised using a narrative synthesis. Methodological quality of studies was evaluated using the Joanna Briggs Institute critical appraisal tools (for cross-sectional, prevalence, cohort, and qualitative studies) and the Consensus on Health Economic Criteria (CHEC) list for cost analyses. Two authors performed quality assessment independently (AL and AK). If there was conflict or uncertainty, a third author was consulted. Risk of bias in a study was considered high if the “yes” score was ≤ 4; moderate if 5–6; and low risk if the score was ≥ 7 on the JBI tools. Quality review results are presented in Appendix 3.
Results
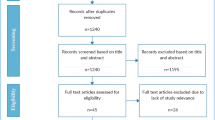
In total 5383 references were imported into Rayyan, and 243 duplicates were removed. A total of 5140 records were screened by title and abstract by reviewers in two pairs (AL and AM; AK and FJD) and independently assessed against the inclusion criteria. In sum, 732 studies were identified for full-text review; 167 were considered for inclusion of which 56 report on the economic, social, and psychological impacts of COVID-19 [6] (see Fig. 1).
Of these, 96% were single-country studies, predominately from the USA (20%), Italy (18%), India (11%), and China (11%). The remainder were from elsewhere in Europe (19%), Middle East (11%), Asia (4%), Brazil (4%), or Canada (2%). Most studies included patients with multiple cancer types (64%). Others focus on specific cancer sites: breast (18%), gynaecological (5%), head and neck (3.6%), lung (3.6%), thyroid (1.8%), colorectal (1.8%), or lymphoma (1.8%).
Social and psychological impacts of COVID-19 on cancer patients
Worry and fear
The most common mental health domain(s) identified were worry and/or fear around their cancer and getting COVID-19. Firstly, there was a heightened sense of fear of cancer recurrence or disease progression due to COVID-19-related disruptions or delays in cancer care [7,8,9,10,11,12,13,14]. Instruments used to measure fear and the level of fear experienced varied. For example, in a survey of 16 European countries, 71% of patients were concerned about cancer progression if their treatment/follow-up was cancelled/postponed [8]. In contrast, a survey in India reported fear of treatment delays and cancer progression as mostly moderate or minimal [10].
Secondly, there was fear and worry around getting COVID-19 amongst cancer patients [7,8,9, 11,12,13, 15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35]. A Singaporean study reported that 66% of patients had an elevated level fear of COVID-19 [36]. Gheorghe et al. [37] found that 68.5% of Romanian cancer patients were “very” or “somewhat worried” about COVID-19 compared to the influenza virus. Biagioli et al. [38] found that 37.3% of Italian cancer patients were “very or extremely” afraid of going to hospital because of an increased risk of contracting COVID-19 there, and 24.5% were “very or completely” afraid that their cancer care would become less important than being protected against COVID-19 infection, which would then have a negative impact on their prognosis. They also found that 53.8% believed they were at a higher risk of COVID-19 infection than the general population. Similarly, Erdem and Karaman [39] report that one-third of Turkish cancer patients were afraid to leave their house. These were more likely to be > 65 years, female, with stage 1 cancer, and with low education attainment. Those that did attend hospital appointments (~ 33%) were more likely to have stage 4 cancer; wore a mask (67%); and preferred not to use public transport owing to COVID-19 risk (95%). The majority (97%) did not accept visitors to their houses and washed their hands more often than usual (97.3%). Those finished treatment (radiotherapy or surgery) with co-morbidities (40%) were also afraid of COVID-19, in particular, females [7]. Higher levels of worry were found among females and older patients in Italy [16, 30], patients with comorbidities, immunocompromised and on active treatment in Denmark, the USA, and China [24, 28, 33], and amongst those with higher stress levels in Iran [40].
Patients tended to prioritise their cancer care over fear of contracting COVID-19, suggesting they were more afraid of delayed treatment and cancer progression than COVID-19 [10]. However, some sub-groups were willing to postpone/delay appointments and treatments [16, 21, 32].
Worryingly, as much as 61.8% were found to fear both COVID-19 infection and cancer progression equally [37]. In practice, the two fears/worries are intertwined, with patients reporting fear of getting COVID-19 infection when in hospital for treatment [11] and fearing that chemotherapy treatment could increase risk of COVID-19 infection (27% of Italian cancer patients sampled [41]). Disparity also existed amongst those who worried more about COVID-19 infection than their cancer, low socioeconomic groups [37], those undergoing palliative care [42], older [8, 16], frailer patients with co-morbidities [16], or those with a good understanding of immunosuppression [10].
Distress, anxiety, and depression
Košir et al. [9] conducted an international survey and found those currently or undergoing treatment within the last 6 months reporting higher levels of psychological distress on average; the most common concern being contracting COVID-19. Some American cancer patients found attending in-person appointments or treatment alone, and the cancellation or movement to virtual social support groups was emotionally challenging and distressing [26]. In France, being unemployed aggravated psychological distress further [43].
Several studies reported anxiety amongst samples of all cancer patients during the pandemic [29, 36, 42, 44]. Additionally, higher levels of anxiety were found amongst female patients in the UK, USA, Poland, and China [19, 26, 33, 35, 43, 45]; patients from lower income households [11]; older and more vulnerable patients in the Netherlands and Northern Italy [18, 30]; married patients in Singapore [36]; and patients with lower educational attainment in Italy, Singapore, and China [35, 36, 46]. In contrast, younger Chinese cancer patients demonstrated elevated levels of anxiety, suicide ideation, and low sleep quality, during the pandemic [47]. While in China, Wang et al. [33] found those employed had a lower risk of anxiety and depression.
Higher levels of depression were reported amongst female patients in China [43], older patients in Turkey [14], those from lower income households in South Korea and India [11, 44], patients who were unemployed in China [43], and unmarried non-parents in South Korea [11].
Social isolation and loneliness
Several studies reported social isolation and loneliness amongst cancer patients [9, 20, 38, 48, 49] which was mediated by detachment from loved ones, lack of social interaction, loneliness, fear of infection, worries about the future, and economic difficulties [38]. Several at-risk groups identified as feeling isolated and anxious. These included American women with ovarian cancer (10%) [20] and young cancer patients (aged 18–39) undergoing cancer care who felt more isolated (52%) than pre-pandemic, specifically missing social interactions [9]. Elran-Barak and Mozeikov [48] reported that lower levels of education and living without minor children in Israel were associated with feelings of loneliness and isolation. Leach et al. [26] in the USA found cancer patients experiencing social distancing and living alone had feelings of loneliness, while disruptions to cancer care were associated with increased loneliness and social isolation [26, 49]. Some patients’ perceived risk of COVID-19 infection caused them to engage in extreme levels of social isolation where they had no visitors and lived alone [26]. For others, the pandemic exasperated underlying situations. For example, Miaskowski et al. [49] upon comparing a more stressed group to a less stressed group found the former reported significantly higher levels of loneliness and social isolation and less resilience than the less stressed group.
Implications of social and psychological impacts
The review revealed that depression and anxiety progression might be associated with deliberate appointment delays [14]. When delays were at post-treatment follow-up or palliative care, this was exasperated further [42]. Also, Shinan‐Altman et al. [31] found that while incidences were low, patients with higher anxiety had more contact with healthcare professionals during the pandemic. Nevertheless, amongst the sample, anxiety did not directly influence healthcare decision-making.
Changes to the way healthcare organisations altered cancer care, to reduced COVID-19 transmission and increased uncertainty, for which tolerance and resilience varied. Hill et al. [23] found COVID-19 fear and intolerance of uncertainty were strongly correlated. Studies reported that health management changes to treatment plans increased patients’ psychological burden [9, 14, 20, 40, 43, 50,51,52,53]. These changes also increased uncertainty with an association between intolerance of uncertainty and anxiety, depressive symptoms, and stress [23]. While uncertainties can be reduced with additional information, health literacy is influenced by socio-economic factors. Erdem and Karaman [39] found that higher educational status was associated with better knowledge of COVID-19 transmission. Better knowledge of COVID-19 was associated with patients aged 40–54 years, in higher education, being female, living in urban areas, with a profession, and a higher income amongst a sample of Romanian cancer patients [37].
Collectively, adverse effects on specific mental health domains had a broad impact. For example, loneliness and isolation amongst cancer patients contributed to declines in general mental health [48] and translated into declines in QoL [15, 20]. Several studies found deterioration in QoL due to COVID-19 compounded by the effects of treatment and financial implications in terms of affordability of care [20, 26]. Despite some respondents being aware of and worried about their QoL [20], those with higher stress levels concerning COVID-19 had worse QoL [40]. Lower QoL and emotional functioning scores were correlated with concerns about contracting COVID-19 [24], with negative spill-over effects found on general health status and physical health in Italy [53] and Israel [48], respectively. Aggravating this further was postponement of care, which negatively impacted QoL [53]. Socio-economic differences were found here too. A higher QoL was correlated with patients who were older [54], employed, with fewer co-morbidities, and not receiving treatment within the last two months [24]. Patients with brain tumours, endometrial/cervical/vulva, and thoracic cancers had lower QoL scores [24]. Being female, having lower educational attainment, crowded housing conditions, and longer illness duration also negatively affected self-reported health status among patients in Israel [48].
Economic impact of COVID-19 on cancer patients and care
Out-of-pocket expenses
From an individual perspective where treatments are not covered under government schemes or insurance, patients experience a large financial burden, in-terms of out-of-pocket expenses, expensive health insurance premiums, or deductibles [26]. This was the case for a considerable proportion of cancer patients in India [44] and Jordan [50]. While this is not a new phenomenon, it has been exasperated by COVID-19. Modified workflows and redistributed cancer care resources saw widespread use of telemedicine, with mixed effects. Transition to telemedicine saved US patients’ time and money ($170) [55]. In contrast, Bakkar et al. [50] found that treatment changes incurred additional patient costs in Jordan. Globally, testing for COVID-19 (negative results were required to attend appointments) introduced varying fee structures with additional costs experienced amongst cancer patients in India [56] and South Korea [11]. These costs affected patients’ decision to undergo cancer treatment particularly in poorer countries [56].
Household finances
Widespread lockdowns during COVID-19 Wave I caused an economic downturn, with negative implications on labour markets. Cancer patients in India (22.2%) expressed fears around losing their jobs and the implications of the expected economic crisis for their family [13]. Similarly, in the USA, cancer patients reported concerns with maintaining employment. These economic conditions exasperated pre-existing cancer financial burdens, including paying for prescriptions and high insurance deductibles in private healthcare markets in the USA [26]. US patients were also concerned with affordability of treatments and transportation to medical facilities [34]. Reduced earnings caused some patients to choose not to attend medical appointments. For example, 46% of cancer patients in India reported financial difficulties as the primary reason for missed consultations [57].
Several studies identified socio-economic factors associated with the economic impacts of COVID-19. Patients that were unemployed, with low educational attainment, or with lower incomes, or were under financial pressure had greater difficulties accessing care in India [44]. In the USA, non-Hispanic white, married, more educated, and older cancer patients were less likely to cite financial worries [26]. These socio-economic inequalities coupled with increased financial burden create barriers to accessing care [44].
Payers and providers
The consequences of COVID-19-related healthcare changes are potentially worsening patients’ clinical condition, which also has economic consequences at the provider level with implications for patients. For example, there is an increased likelihood of post-operative ICU following delayed surgery [58]. During the pandemic, demands for services like respiratory assistance increased. This dual increase in demand had resource implications for healthcare providers; reduced resources limit choices to delivering post-operative cancer care or care for COVID-19 patients [59].
The introduction and expansion of telemedicine during the pandemic had mixed effects for healthcare providers and payers. Parikh et al. [55] reported the transition to telemedicine saved hospitals time and money in the USA. However, Goenka et al. [60] report that while it did ensure continuation of care, its cost and financial impacts must be considered. It may not be financially suitable for all care due to implementation and maintenance costs compared with reimbursement received, cost savings to patients (direct and indirect), and care coordination. Mahl et al. [42] found similar results for tele-consultation technologies for palliative and follow-up services in Brazil. Furthermore, the high prevalence of anxieties and fears discussed above culminated in increased demand for support services and information, as demonstrated by the increased volume of calls, emails, and messages found in one North American study [34]. One Italian study found such communications tended to have more negative than positive messages (57% vs 43%) [21].
Innovations to mitigate impacts
Social and psychological impacts, along with modified workflows that redistributed healthcare resources, had an economic impact on patients and healthcare systems. US patients experiencing higher stress had more financial concerns [49], and COVID-19 exasperated existing financial burden associated with cancer on families, with some not being able to afford to attend consultations [57]. Studies revealed coping strategies adopted by cancer survivors and patients to deal with the impact of the pandemic [20, 61]. Mechanisms used to cope included connection to family and friends, spirituality/prayer, music therapy, emotional supports, positive reframing, and daily routine, including self-care, hobbies, and planning [30, 61, 62]. These strategies were an important predictor of QoL [20] and positive health behaviours. Positive lifestyle choices were likely to alleviate mental health burden and improve HRQoL [30, 35, 54], while others employed avoidance coping strategies, including self-distraction and substance use [62].
Using positive coping strategies was important as delivery of support services was adversely impacted by COVID-19 [13, 51, 61]. Such supports included psychological and peer group support services, counseling for patients [13, 51, 61], and caregiver supports [35]. Maintaining or quickly resuming these supports during the pandemic was associated with less anxiety [35] and distress [51]. Additionally, patients with higher social support had more contact with healthcare professionals during the COVID-19 pandemic [31].
Discussion
Economic burden associated with cancer for patients is measured through direct and indirect costs with both objective (i.e. financial burden) and subjective approaches (financial distress) [3]. This adjustment to economic burden measurement coincides with the growing knowledge of cancer as a chronic disease, which widens perspective and shifts understanding of possible side effects beyond clinical outcomes.
Pre-pandemic psychological strain was caused by possible cancer treatment side effects which have adverse health outcomes [63]. The pandemic exasperated these health outcomes further. National and institutional public health guidelines to reduce COVID-19 transmission resulted in suspended cancer screening programmes, delayed diagnoses, postponed or deferred treatments, and altered treatment regimes in many countries. These health system shocks also altered patients’ decision making and health-seeking behaviours. For example, to shield from COVID-19, patients delayed seeking medical appointments, avoided clinical settings, etc. In the immediate and long term, this has direct impacts on health outcomes, increasing cancer morbidity and mortality. Longer-term strategic outcomes are also hampered with deferred cancer strategies that have direct consequences for achieving high-level targets such as the United Nations' (UN) Sustainable Development Goal 3 of good health and well-being for all and the European Commission Cancer Mission of improving the lives of those affected by cancer through prevention and cure.
Collectively, these types of costs can affect patients’ QoL that represents an additional cost to their well-being [3, 64, 65]. This review predominately captures the experience during the first wave of the pandemic, when national lockdowns and public health guidelines were at the highest level internationally. So while many of the impacts and costs from previous frameworks [3] were identified in the review, the studies adopted a short-term perspective. We suspect that as the pandemic persists, and more longitudinal data becomes available, further costs and impacts will be documented capturing a broader range of costs, for example, re-distribution of resources in healthcare delivery and subsequent opportunity costs of telemedicine from a patient and provider perspective, the associated treatment costs of COVID-19, or the feelings of isolation that affected QoL.
Despite gaps in range and severity of costs, evidence from this review demonstrates the demand for psychological support and information to alleviate fears and provide reassurance to patients. COVID-19 increased information asymmetries in the delivery of all healthcare services, including cancer care. Imperfect and inadequate information create uncertainties which influence patients’ behaviour and decision-making. With poor information and high levels of uncertainty, patients were risk adverse, reducing their health-seeking behaviours, avoiding public transport, clinical settings, etc. Such behaviours have long-term impacts; later diagnosis and delayed treatment adversely impact cancer patients’ health outcomes, QoL, and mortality.
While economies and healthcare systems are recovering, COVID-19 remains a threat for cancer patients. Accurate and effective information and support for cancer patients are still needed to mitigate further impacts and to support patients in its aftermath. In some settings, tele-health could be used to provide this; however, a one-size-fits-all approach is not suitable. Supports and information need to be tailored to the target audience, depending on the healthcare system characteristics, resources available, and the socio-economic profile of the patient population. This is imperative as we emerge from the pandemic, to mitigate its affects, promote recovery in health systems and in patients, and implement learnings for future possible pandemics.
The review revealed several approaches to minimise the economic, social, and psychological impacts of COVID-19 for cancer patients, centring around provision of information and support services and coping strategies. Regarding information, three recommendations emerged. Firstly, more information is required, specifically with regard to how to cope with the pandemic [9]. Secondly, effective communication between physicians and patients is required [14]. Effectively delivered communications provide valuable information that can reduce information asymmetries. Thirdly, information could be provided via online education programmes, which may alleviate anxiety and improve HRQoL [35], as appropriately designed interventions can reduce cancer-related psychosocial outcomes and quality of life [66, 67].
Limitations
This review mainly captured the first wave of the COVID-19 pandemic in March 2020. Many studies were reliant on single institutions (e.g. [44, 55]) and lack long-term follow-up [55]. In some cases, data were only available for short periods (e.g. [44, 59]) which had negative implications on sample size. Data collection methods varied, with many using online methods that can exclude those experiencing technology barriers.
Conclusion
COVID-19 compounded the economic, social, and psychological impacts of cancer on patients owing to health system adjustments and reduction in economic activity. Identification of the impact of COVID-19 on cancer patients from a psychological, social, and economic perspective following the pandemic can inform the design of timely and appropriate interventions and supports, to deal with the backlog in cancer care and enhance recovery. While the long-term effects and economic fallout for cancer patients are not easily quantified, they are real and further support is required to alleviate the issues cancer patients face.
Data Availability
Materials and codes available upon request to the authors.
References
Sung H, Ferlay J, Siegel R, Laversanne M, Soerjomataram I, Jemal A, et al. 2020 Global cancer statistics. GLOBOCAN estimates of incidence and mortality worldwide for. 36.
Stewart BW, Wild CP(ed). World Cancer Report Lyon: WHO press; 2014 [Available from: https://publications.iarc.fr/Non-Series-Publications/World-Cancer-Reports/World-Cancer-Report-2014.
Essue BM, Iragorri N, Fitzgerald N, de Oliveira C (2020) The psychosocial cost burden of cancer: a systematic literature review. Psychooncology 29(11):1746–1760
Higgins JP. Cochrane handbook for systematic reviews of interventions version 5.0. 1. The Cochrane Collaboration. http://www.cochrane-handbook org. 2008.
Davies KS (2011) Formulating the evidence based practice question: a review of the frameworks. Evid Based Libr Inf Pract 6(2):75–80
Murphy A, Lawlor, A., Kirby, A. Drummond, F.D. 2021 A systematic review of the impact of COVID-19 pandemic on cancer patients and survivors from an economic and social perspective. University College Cork, Cork, Ireland.
Catania C, Spitaleri G, Del Signore E, Attili I, Radice D, Stati V, et al. 2020 Fears and perception of the impact of COVID-19 on patients with lung cancer: a mono-institutional survey. Frontiers Oncol 10.
Gultekin M, Ak S, Ayhan A, Strojna A, Pletnev A, Fagotti A et al (2021) Perspectives, fears and expectations of patients with gynaecological cancers during the COVID-19 pandemic: a Pan-European study of the European Network of Gynaecological Cancer Advocacy Groups (ENGAGe). Cancer Med 10(1):208–219
Košir U, Loades M, Wild J, Wiedemann M, Krajnc A, Roškar S et al (2020) The impact of COVID-19 on the cancer care of adolescents and young adults and their well-being: results from an online survey conducted in the early stages of the pandemic. Cancer 126(19):4414–4422
Ghosh J, Ganguly S, Mondal D, Pandey P, Dabkara D, Biswas B (2020) Perspective of oncology patients during COVID-19 pandemic: a prospective observational study from India. JCO Global Oncol 6:844–51
Kim SY, Kim S. 2021. Do COVID-19-related treatment changes influence fear of cancer recurrence, anxiety, and depression in breast cancer patients? Cancer nursing.
Lou E, Teoh D, Brown K, Blaes A, Holtan SG, Jewett P et al (2020) Perspectives of cancer patients and their health during the COVID-19 pandemic. PLoS ONE 15(10):e0241741
Mitra M, Basu M (2020) A study on challenges to health care delivery faced by cancer patients in India during the COVID-19 pandemic. J Prim Care Commun Health 11:1–5
Yildirim OA, Poyraz K, Erdur E. 2021 Depression and anxiety in cancer patients before and during the SARS-CoV-2 pandemic: association with treatment delays. Qual Life Res: Int J Qual Life Asp Treat Care Rehabil
Bäuerle A, Musche V, Schmidt K, Schweda A, Fink M, Weismüller B et al (2021) Mental health burden of german cancer patients before and after the outbreak of COVID-19: predictors of mental health impairment. Int J Environ Res Public Health 18(5):2318
Campi R, Tellini R, Grosso AA, Amparore D, Mari A, Viola L et al (2021) Deferring elective urologic surgery during the COVID-19 pandemic: the patients’ perspective. Urology 147:21–26
Chia JMX, Goh ZZS, Chua ZY, Ng KYY, Ishak D, Fung SM et al (2021) Managing cancer in context of pandemic: a qualitative study to explore the emotional and behavioural responses of patients with cancer and their caregivers to COVID-19. BMJ Open 11(1):e041070
de Joode K, Dumoulin DW, Engelen V, Bloemendal HJ, Verheij M, van Laarhoven HWM et al (2020) Impact of the coronavirus disease 2019 pandemic on cancer treatment: the patients’ perspective. Eur J Cancer 136:132–139
Fox L, Wylie H, Cahill F, Haire A, Green S, Kibaru J et al (2021) Gender differences in concerns about participating in cancer research during the COVID-19 pandemic. Cancer control J Moffitt Cancer Center 28:1073274821989315
Frey MK, Ellis AE, Zeligs K, Chapman-Davis E, Thomas C, Christos PJ et al (2020) Impact of the coronavirus disease 2019 pandemic on the quality of life for women with ovarian cancer. Am J Obstet Gynecol 223(5):725.e1-.e9
Gebbia V, Piazza D, Valerio MR, Borsellino N, Firenze A (2020) Patients with cancer and COVID-19: a WhatsApp messenger-based survey of patients’ queries, needs, fears, and actions taken. JCO global oncology 6:722–729
Han J, Zhou F, Zhang L, Su Y, Mao L (2021) Psychological symptoms of cancer survivors during the COVID-19 outbreak: a longitudinal study. Psychooncology 30(3):378–384
Hill EM, Frost A, Martin JD. 2021 Experiences of women with ovarian cancer during the covid-19 pandemic: examining intolerance of uncertainty and fear of covid-19 in relation to psychological distress. J Psychosoc Oncol
Jeppesen SS, Bentsen KK, Jørgensen TL, Holm HS, Holst-Christensen L, Tarpgaard LS et al (2021) Quality of life in patients with cancer during the COVID-19 pandemic – a Danish cross-sectional study (COPICADS). Acta Oncol 60(1):4–12
Kamposioras K, Saunders M, Jonathan Lim KH, Marti K, Anderson D, Cutting M, 2020 et al. The impact of changes in service delivery in patients with colorectal cancer during the initial phase of the COVID-19 pandemic. Clin Colorectal Cancer
Leach CR, Kirkland EG, Masters M, Sloan K, Rees-Punia E, Patel AV, et al. 2021 Cancer survivor worries about treatment disruption and detrimental health outcomes due to the COVID-19 pandemic. J Psychosoc Oncol
Ng KYYZS, Tan SH, Ishak NDB, Goh ZZS, Chua ZY, Chia JMX, Chew EL, Shwe T, Mok JKY, Leong SS, Lo JSY, Ang ZLT, Leow JL, Lam CWJ, Kwek JW, Dent R, Tuan J, Lim ST, Hwang WYK, Griva K, Ngeow J (2020) Understanding the psychological impact of COVID-19 pandemic on patients with cancer, their caregivers, and health care workers in Singapore. JCO Global Oncol 6:1494–509
Papautsky EL, Hamlish T (2021) Emotional response of US breast cancer survivors during the COVID-19 pandemic. Cancer Invest 39(1):3–8
Philip KEJ, Lonergan B, Cumella A, Farrington-Douglas J, Laffan M, Hopkinson NS (2020) COVID-19 related concerns of people with long-term respiratory conditions: a qualitative study. BMC Pulm Med 20(1):319
Pigozzi E, Tregnago D, Costa L, Insolda J, Turati E, Rimondini M et al (2021) Psychological impact of Covid-19 pandemic on oncological patients: a survey in Northern Italy. PLoS ONE 16(3):e0248714
Shinan-Altman S, Levkovich I, Tavori G (2020) Healthcare utilization among breast cancer patients during the COVID-19 outbreak. Palliat Support Care 18(4):385–391
Vanni G, Materazzo M, Pellicciaro M, Ingallinella S, Rho M, Santori F et al (2020) Breast cancer and COVID-19: the effect of fear on patients’ decision-making process. In vivo (Athens, Greece) 34(3):1651–1659
Wang Y, Duan Z, Ma Z, Mao Y, Li X, Wilson A et al (2020) Epidemiology of mental health problems among patients with cancer during COVID-19 pandemic. Transl Psychiatry 10(1):263
Yan F, Rauscher E, Hollinger A, Caputo MA, Ready J, Fakhry C et al (2020) The role of head and neck cancer advocacy organizations during the COVID-19 pandemic. Head Neck 42(7):1526–1532
Yang S, Dong D, Gu H, Gale RP, Ma J, Huang X. 2020 Impact of stopping therapy during the SARS-CoV-2 pandemic in persons with lymphoma. J Cancer Res Clin Oncol
Ng KYY, Zhou S, Tan SH, Ishak NDB, Goh ZZS, Chua ZY et al (2020) Understanding the psychological impact of COVID-19 pandemic on patients with cancer, their caregivers, and health care workers in Singapore. JCO Global Oncol 6:1494–1509
Gheorghe AS, Negru ŞM, Niţipir C, Mazilu L, Marinca M, Gafton B et al (2021) Knowledge, attitudes and practices related to the COVID-19 outbreak among Romanian adults with cancer: a cross-sectional national survey. ESMO Open 6(1):100027
Biagioli V, Albanesi B, Belloni S, Piredda A, Caruso R (2021) Living with cancer in the COVIDâ 19 pandemic: an Italian survey on selfâ isolation at home. Eur J Cancer Care 30(2):1–11
Erdem D, Karaman I (2020) Awareness and perceptions related to COVIDâ 19 among cancer patients: a survey in oncology department. Eur J Cancer Care 29(6):1–10
Charsouei S, Esfahlani MZ, Dorosti A, Zamiri RE (2021) Effects of COVID-19 pandemic on perceived stress, quality of life, and coping strategies of women with breast cancer with spinal metastasis under chemotherapy. Int J Women’s Health Reprod Sci 9(1):55–60
Zuliani S, Zampiva I, Tregnago D, Casali M, Cavaliere A, Fumagalli A et al (2020) Organisational challenges, volumes of oncological activity and patients’ perception during the severe acute respiratory syndrome coronavirus 2 epidemic. Eur J Cancer 135:159–169
Mahl C, Melo LRS, Almeida MHA, Carvalho CS, Santos LLS, Nunes PS et al (2020) Delay in head and neck cancer care during the COVID-19 pandemic and its impact on health outcomes. Braz Oral Res 34:e126
Chaix B, Delamon G, Guillemassé A, Brouard B, Bibault J-E (2020) Psychological distress during the COVID-19 pandemic in France: a national assessment of at-risk populations. Gen Psychiatr 33(6):1–6
Rajan S, Akhtar N, Tripathi A, Kumar V, Chaturvedi A, Mishra P et al (2021) Impact of COVID-19 pandemic on cancer surgery: patient’s perspective. J Surg Oncol 123(5):1188–1198
Sigorski D, Sobczuk P, Osmola M, Kuć K, Walerzak A, Wilk M et al (2020) Impact of COVID-19 on anxiety levels among patients with cancer actively treated with systemic therapy. ESMO Open. 5(5):e000970
Merz V, Ferro A, Piras EM, Zanutto A, Caffo O, Messina C (2021) Electronic medical record-assisted telephone follow-up of breast cancer survivors during the COVID-19 pandemic: a single institution experience. JCO Oncol Pract 17(1):e44–e52
Yang G, Xiao C, Li S, Yang N (2020) The effect and mechanism of adverse childhood experience on suicide ideation in young cancer patients during coronavirus disease 2019 (COVID-19) pandemic. Risk Manag Healthc Policy 13:1293–1300
Elran-Barak R, Mozeikov M (2020) One month into the reinforcement of social distancing due to the COVID-19 outbreak: subjective health, health behaviors, and loneliness among people with chronic medical conditions. Int J Environ Res Public Health 17(15):5403
Miaskowski C, Paul SM, Snowberg K, Abbott M, Borno H, Chang S et al (2020) Stress and symptom burden in oncology patients during the COVID-19 pandemic. J Pain Symptom Manage 60(5):e25–e34
Bakkar S, Al-Omar K, Aljarrah Q, Al-Dabbas Md, Al-Dabbas N, Samara S et al (2020) Impact of COVID-19 on thyroid cancer surgery and adjunct therapy. Updat Surg 72(3):867–9
Juanjuan L, Santa-Maria CA, Hongfang F, Lingcheng W, Pengcheng Z, Yuanbing X et al (2020) Patient-reported outcomes of patients with breast cancer during the COVID-19 outbreak in the epicenter of China: a cross-sectional survey study. Clin Breast Cancer 20(5):e651–e662
Massicotte V, Hans I, Savard J (2021) COVID-19 pandemic stressors and psychological symptoms in breast cancer patients. Curr Oncol (Toronto, Ont) 28(1):294–300
Greco F, Altieri VM, Esperto F, Mirone V, Scarpa RM. 2020 Impact of COVID-19 pandemic on health-related quality of life in uro-oncologic patients: what should we wait for? Clinical Genitourinary Cancer.
Baffert K-A, Darbas T, Lebrun-Ly V, Pestre-Munier J, Peyramaure C, Descours C et al (2021) Quality of life of patients with cancer during the COVID-19 pandemic. In vivo (Athens, Greece) 35(1):663–670
Parikh NR, Chang EM, Kishan AU, Kaprealian TB, Steinberg ML, Raldow AC (2020) Time-driven activity-based costing analysis of telemedicine services in radiation oncology. Int J Radiat Oncol Biol Phys 108(2):430–434
Deshmukh S, Naik S, Zade B, Patwa R, Gawande J, Watgaonkar R et al (2020) Impact of the pandemic on cancer care: lessons learnt from a rural cancer center in the first 3 months. J Surg Oncol 122(5):831–838
Akhtar N, Rajan S, Chakrabarti D, Kumar V, Gupta S, Misra S et al (2021) Continuing cancer surgery through the first six months of the COVID-19 pandemic at an academic university hospital in India: a lower-middle-income country experience. J Surg Oncol 123(5):1177–1187
Sud A, Jones ME, Broggio J, Loveday C, Torr B, Garrett A et al (2020) Collateral damage: the impact on outcomes from cancer surgery of the COVID-19 pandemic. Ann Oncol Off J Eur Soc Med Oncol 31(8):1065–1074
Mari G, Giordano R, Uccelli M, Cesana G, Olmi S, Ferrari GC et al (2020) Do we really know how much the COVID-19 pandemic affected the surgical practice in Northern Italy? A multi-center comparative study and cost analysis. Chirurgia (Bucharest, Romania : 1990) 115(4):469–75
Goenka A, Ma D, Teckie S, Alfano C, Bloom B, Hwang J et al (2021) Implementation of telehealth in radiation oncology: rapid integration during COVID-19 and its future role in our practice. Adv Radiat Oncol 6(1):100575
Singh N, Kumar S, Rathore P, Vig S, Vallath N, Mohan A et al (2020) Concerns and coping strategies of persons under institutional quarantine during SARS-CoV-2 pandemic. Indian J Palliat Care 26:99–105
Frey MK, Chapman-Davis E, Glynn SM, Lin J, Ellis AE, Tomita S et al (2021) Adapting and avoiding coping strategies for women with ovarian cancer during the COVID-19 pandemic. Gynecol Oncol 160(2):492–498
Carrera PM, Kantarjian HM, Blinder VS (2018) The financial burden and distress of patients with cancer: understanding and stepping-up action on the financial toxicity of cancer treatment. CA Cancer J Clin 68(2):153–165
Lathan CS, Cronin A, Tucker-Seeley R, Zafar SY, Ayanian JZ, Schrag D (2016) Association of financial strain with symptom burden and quality of life for patients with lung or colorectal cancer. J Clin Oncol 34(15):1732
Tompa E, Kalcevich C, McLeod C, Lebeau M, Song C, McLeod K et al (2017) The economic burden of lung cancer and mesothelioma due to occupational and para-occupational asbestos exposure. Occup Environ Med 74(11):816–822
Nikita, Rani R, Kumar R. 2022 Body image distress among cancer patients: needs for psychosocial intervention development. Supportive Care in Cancer
Rawl SM, Given BA, Given CW, Champion VL, Kozachik SL, Barton D, et al., editors. 2002. Intervention to improve psychological functioning for newly diagnosed patients with cancer. Oncology Nursing Forum
Funding
Open Access funding provided by the IReL Consortium This work was funded by MSD Global Oncology Policy grant programme.
Author information
Authors and Affiliations
Contributions
All the authors contributed to the study conception and design. Material preparation and data collection and analysis were performed by all the authors. AK drafted the manuscript, and all the authors commented on previous versions of the manuscript. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This is a systematic review so no ethical approval is required. The review is registered on PROSPERO (CRD42021246651).
Consent to participate
NA
Consent to publish
NA
Competing interests
The author’s institution received the financial grant which supported the work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kirby, A., Drummond, F.J., Lawlor, A. et al. Counting the social, psychological, and economic costs of COVID-19 for cancer patients. Support Care Cancer 30, 8705–8731 (2022). https://doi.org/10.1007/s00520-022-07178-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-022-07178-0