Abstract
Objectives
In the last decades, the number of cancer patients admitted in intensive care units (ICUs) for septic shock has dramatically increased. However, prognosis data remain scarce.
Methods
To assess the 180-day mortality rate in cancer patients admitted to the ICU for septic shock, a 5-year prospective study was performed. All adult patients admitted for septic shock were included and categorized into the following two groups and four subgroups: cancer patients (solid tumor or hematological malignancy) and non-cancer patients (immunocompromised or not). Data were collected and compared between the groups. Upon early ICU admission, the decision to forgo life-sustaining therapy (DFLST) or not was made by consultation among hematologists, oncologists, and the patients or their relatives.
Results
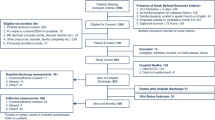
During the study period, 496 patients were admitted for septic shock: 252 cancer patients (119 hematological malignancies and 133 solid tumors) and 244 non-cancer patients. A DFLST was made for 39% of the non-cancer patients and 52% of the cancer patients. The 180-day mortality rate among the cancer patients was 51% and 68% for those with hematological malignancies and solid cancers, respectively. The mortality rate among the non-cancer patients was 44%. In a multivariate analysis, the performance status, Charlson comorbidity index, simplified acute physiology score 2, sequential organ failure assessment score, and DFLST were independent predictors of 180-day mortality.
Conclusions
Despite early admission to the ICU, the 180-day mortality rate due to septic shock was higher in cancer patients compared with non-cancer patients, due to excess mortality in the patients with solid tumors. The long-term prognosis of cancer patients with septic shock is modulated by their general state, severity of organ failure, and DFLST.



Similar content being viewed by others
References
Azoulay E, Schellongowski P, Darmon M, Bauer PR, Benoit D, Depuydt P, Divatia JV, Lemiale V, van Vliet M, Meert AP, Mokart D, Pastores SM, Perner A, Pène F, Pickkers P, Puxty KA, Vincent F, Salluh J, Soubani AO, Antonelli M, Staudinger T, von Bergwelt-Baildon M, Soares M (2017) The intensive care medicine research agenda on critically ill oncology and hematology patients. Intensive Care Med 43(9):1366–1382
Shimabukuro-Vornhagen A, Boll B, Kochanek M, Azoulay E, von Bergwelt-Baildon MS (2016) Critical care of patients with cancer. CA Cancer J Clin
Brunet F, Lanore JJ, Dhainaut JF, Dreyfus F, Vaxelaire JF, Nouira S, Giraud T, Armaganidis A, Monsallier JF (1990) Is intensive care justified for patients with haematological malignancies? Intensive Care Med 16(5):291–297
Pene F, Soares M (2008) Can we still refuse ICU admission of patients with hematological malignancies? Intensive Care Med 34(5):790–792
Schellongowski P, Sperr WR, Wohlfarth P, Knoebl P, Rabitsch W, Watzke HH, Staudinger T (2016) Critically ill patients with cancer: chances and limitations of intensive care medicine-a narrative review. ESMO Open 1(5):e000018
Schellongowski P, Staudinger T, Kundi M, Laczika K, Locker GJ, Bojic A, Robak O, Fuhrmann V, Jager U, Valent P, Sperr WR (2011) Prognostic factors for intensive care unit admission, intensive care outcome, and post-intensive care survival in patients with de novo acute myeloid leukemia: a single center experience. Haematologica 96(2):231–237
Soares M, Bozza FA, Azevedo LC, Silva UV, Correa TD, Colombari F et al (2016) Effects of organizational characteristics on outcomes and resource use in patients with cancer admitted to intensive care units. J Clin Oncol 34(27):3315–3324
Azoulay E, Soares M, Darmon M, Benoit D, Pastores S, Afessa B (2011) Intensive care of the cancer patient: recent achievements and remaining challenges. Ann Intensive Care 1(1):5
Azoulay E, Pene F, Darmon M, Lengline E, Benoit D, Soares M et al (2015) Managing critically ill hematology patients: time to think differently. Blood Rev 29(6):359–367
Park HY, Suh GY, Jeon K, Koh WJ, Chung MP, Kim H, Kwon OJ, Kim K, Jang JH, Jung CW, Kang E, Kim MJ (2008) Outcome and prognostic factors of patients with acute leukemia admitted to the intensive care unit for septic shock. Leuk Lymphoma 49(10):1929–1934
Williams MD, Braun LA, Cooper LM, Johnston J, Weiss RV, Qualy RL, Linde-Zwirble W (2004) Hospitalized cancer patients with severe sepsis: analysis of incidence, mortality, and associated costs of care. Crit Care 8(5):R291–R298
Kiehl MG, Beutel G, Boll B, Buchheidt D, Forkert R, Fuhrmann V et al (2018) Consensus statement for cancer patients requiring intensive care support. Ann Hematol 97(7):1271–1282
Pene F, Percheron S, Lemiale V, Viallon V, Claessens YE, Marque S et al (2008) Temporal changes in management and outcome of septic shock in patients with malignancies in the intensive care unit. Crit Care Med 36(3):690–696
Rosolem MM, Rabello LS, Lisboa T, Caruso P, Costa RT, Leal JV et al (2012) Critically ill patients with cancer and sepsis: clinical course and prognostic factors. J Crit Care 27(3):301–307
Larche J, Azoulay E, Fieux F, Mesnard L, Moreau D, Thiery G et al (2003) Improved survival of critically ill cancer patients with septic shock. Intensive Care Med 29(10):1688–1695
Zuber B, Tran TC, Aegerter P, Grimaldi D, Charpentier J, Guidet B, Mira JP, Pène F, CUB-Réa Network (2012) Impact of case volume on survival of septic shock in patients with malignancies. Crit Care Med 40(1):55–62
Jamme M, Daviaud F, Charpentier J, Marin N, Thy M, Hourmant Y, Mira JP, Pène F (2017) Time course of septic shock in immunocompromised and nonimmunocompromised patients. Crit Care Med 45(12):2031–2039
Legrand M, Max A, Peigne V, Mariotte E, Canet E, Debrumetz A, Lemiale V, Seguin A, Darmon M, Schlemmer B, Azoulay É (2012) Survival in neutropenic patients with severe sepsis or septic shock. Crit Care Med 40(1):43–49
Rhodes A, Evans LE, Alhazzani W, Levy MM, Antonelli M, Ferrer R, Kumar A, Sevransky JE, Sprung CL, Nunnally ME, Rochwerg B, Rubenfeld GD, Angus DC, Annane D, Beale RJ, Bellinghan GJ, Bernard GR, Chiche JD, Coopersmith C, de Backer DP, French CJ, Fujishima S, Gerlach H, Hidalgo JL, Hollenberg SM, Jones AE, Karnad DR, Kleinpell RM, Koh Y, Lisboa TC, Machado FR, Marini JJ, Marshall JC, Mazuski JE, McIntyre LA, McLean AS, Mehta S, Moreno RP, Myburgh J, Navalesi P, Nishida O, Osborn TM, Perner A, Plunkett CM, Ranieri M, Schorr CA, Seckel MA, Seymour CW, Shieh L, Shukri KA, Simpson SQ, Singer M, Thompson BT, Townsend SR, van der Poll T, Vincent JL, Wiersinga WJ, Zimmerman JL, Dellinger RP (2017) Surviving sepsis campaign: international guidelines for management of sepsis and septic shock: 2016. Intensive Care Med 43(3):304–377
Levy MM, Evans LE, Rhodes A (2018) The surviving sepsis campaign bundle: 2018 update. Intensive Care Med 44(6):925–928
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC (2016) The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 315(8):801–810
Angus DC, van der Poll T (2013) Severe sepsis and septic shock. N Engl J Med 369(21):2063
Kumar A, Roberts D, Wood KE, Light B, Parrillo JE, Sharma S, Suppes R, Feinstein D, Zanotti S, Taiberg L, Gurka D, Kumar A, Cheang M (2006) Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Crit Care Med 34(6):1589–1596
Annane D, Aegerter P, Jars-Guincestre MC, Guidet B (2003) Current epidemiology of septic shock: the CUB-Rea network. Am J Respir Crit Care Med 168(2):165–172
Friedman G, Silva E, Vincent JL (1998) Has the mortality of septic shock changed with time. Crit Care Med 26(12):2078–2086
Vincent JL, Lefrant JY, Kotfis K, Nanchal R, Martin-Loeches I, Wittebole X et al (2018) Comparison of European ICU patients in 2012 (ICON) versus 2002 (SOAP). Intensive Care Med 44(3):337–344
Gordon AC, Mason AJ, Thirunavukkarasu N, Perkins GD, Cecconi M, Cepkova M, Pogson DG, Aya HD, Anjum A, Frazier GJ, Santhakumaran S, Ashby D, Brett SJ, for the VANISH Investigators (2016) Effect of early vasopressin vs norepinephrine on kidney failure in patients with septic shock: the VANISH randomized clinical trial. JAMA 316(5):509–518
Asfar P, Meziani F, Hamel JF, Grelon F, Megarbane B, Anguel N, Mira JP, Dequin PF, Gergaud S, Weiss N, Legay F, le Tulzo Y, Conrad M, Robert R, Gonzalez F, Guitton C, Tamion F, Tonnelier JM, Guezennec P, van der Linden T, Vieillard-Baron A, Mariotte E, Pradel G, Lesieur O, Ricard JD, Hervé F, du Cheyron D, Guerin C, Mercat A, Teboul JL, Radermacher P, SEPSISPAM Investigators (2014) High versus low blood-pressure target in patients with septic shock. N Engl J Med 370(17):1583–1593
Holst LB, Haase N, Wetterslev J, Wernerman J, Guttormsen AB, Karlsson S, Johansson PI, Åneman A, Vang ML, Winding R, Nebrich L, Nibro HL, Rasmussen BS, Lauridsen JRM, Nielsen JS, Oldner A, Pettilä V, Cronhjort MB, Andersen LH, Pedersen UG, Reiter N, Wiis J, White JO, Russell L, Thornberg KJ, Hjortrup PB, Müller RG, Møller MH, Steensen M, Tjäder I, Kilsand K, Odeberg-Wernerman S, Sjøbø B, Bundgaard H, Thyø MA, Lodahl D, Mærkedahl R, Albeck C, Illum D, Kruse M, Winkel P, Perner A (2014) Lower versus higher hemoglobin threshold for transfusion in septic shock. N Engl J Med 371(15):1381–1391
Mouncey PR, Osborn TM, Power GS, Harrison DA, Sadique MZ, Grieve RD, Jahan R, Harvey SE, Bell D, Bion JF, Coats TJ, Singer M, Young JD, Rowan KM, ProMISe Trial Investigators (2015) Trial of early, goal-directed resuscitation for septic shock. N Engl J Med 372(14):1301–1311
Ranieri VM, Thompson BT, Barie PS, Dhainaut JF, Douglas IS, Finfer S, Gårdlund B, Marshall JC, Rhodes A, Artigas A, Payen D, Tenhunen J, al-Khalidi HR, Thompson V, Janes J, Macias WL, Vangerow B, Williams MD, PROWESS-SHOCK Study Group (2012) Drotrecogin alfa (activated) in adults with septic shock. N Engl J Med 366(22):2055–2064
Venkatesh B, Finfer S, Cohen J, Rajbhandari D, Arabi Y, Bellomo R, Billot L, Correa M, Glass P, Harward M, Joyce C, Li Q, McArthur C, Perner A, Rhodes A, Thompson K, Webb S, Myburgh J, ADRENAL Trial Investigators and the Australian–New Zealand Intensive Care Society Clinical Trials Group (2018) Adjunctive glucocorticoid therapy in patients with septic shock. N Engl J Med 378(9):797–808
Annane D, Renault A, Brun-Buisson C, Megarbane B, Quenot JP, Siami S, Cariou A, Forceville X, Schwebel C, Martin C, Timsit JF, Misset B, Ali Benali M, Colin G, Souweine B, Asehnoune K, Mercier E, Chimot L, Charpentier C, François B, Boulain T, Petitpas F, Constantin JM, Dhonneur G, Baudin F, Combes A, Bohé J, Loriferne JF, Amathieu R, Cook F, Slama M, Leroy O, Capellier G, Dargent A, Hissem T, Maxime V, Bellissant E, CRICS-TRIGGERSEP Network (2018) Hydrocortisone plus fludrocortisone for adults with septic shock. N Engl J Med 378(9):809–818
Peake SL, Delaney A, Bailey M, Bellomo R, Cameron PA, Cooper DJ et al (2014) Goal-directed resuscitation for patients with early septic shock. N Engl J Med 371(16):1496–1506
Siegel RL, Miller KD, Jemal A (2017) Cancer statistics, 2017. CA Cancer J Clin 67(1):7–30
Taccone FS, Artigas AA, Sprung CL, Moreno R, Sakr Y, Vincent JL (2009) Characteristics and outcomes of cancer patients in European ICUs. Crit Care 13(1):R15
Wohlfarth P, Staudinger T, Sperr WR, Bojic A, Robak O, Hermann A et al (2014) Prognostic factors, long-term survival, and outcome of cancer patients receiving chemotherapy in the intensive care unit. Ann Hematol 93(10):1629–1636
Moore JX, Akinyemiju T, Bartolucci A, Wang HE, Waterbor J, Griffin R (2018) A prospective study of cancer survivors and risk of sepsis within the REGARDS cohort. Cancer Epidemiol 55:30–38
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383
Tolsma V, Schwebel C, Azoulay E, Darmon M, Souweine B, Vesin A, Goldgran-Toledano D, Lugosi M, Jamali S, Cheval C, Adrie C, Kallel H, Descorps-Declere A, Garrouste-Orgeas M, Bouadma L, Timsit JF (2014) Sepsis severe or septic shock: outcome according to immune status and immunodeficiency profile. Chest 146(5):1205–1213
Pavon A, Binquet C, Kara F, Martinet O, Ganster F, Navellou JC, Castelain V, Barraud D, Cousson J, Louis G, Perez P, Kuteifan K, Noirot A, Badie J, Mezher C, Lessire H, Quantin C, Abrahamowicz M, Quenot JP (2013) Profile of the risk of death after septic shock in the present era: an epidemiologic study. Crit Care Med 41(11):2600–2609
Acknowledgments
The authors thank Mojgan HESSAMFAR, MD, for her kind contribution to realize the statistical analysis.
Author information
Authors and Affiliations
Contributions
FC and NI designed the study. FC, NI, and MD collected demographic, clinical, and paraclinical data. TL and NM regularly treated hematological patients of the study. AD and AR regularly treated oncological patients of the study. FC, NI, GM, and OG regularly treated septic shocks in ICU. FC performed the statistical analysis. FC, MD, and NI wrote the article. All authors reviewed and approved the article.
Corresponding author
Ethics declarations
Patients were informed of the anonymous use of their medical data for clinical research in accordance with French legal standards (CNIL no. 2009055).
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Camou, F., Didier, M., Leguay, T. et al. Long-term prognosis of septic shock in cancer patients. Support Care Cancer 28, 1325–1333 (2020). https://doi.org/10.1007/s00520-019-04937-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-04937-4