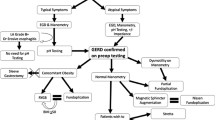
Summary
Background
Patients suffering from colorectal deep endometriosis (DE) experience gastrointestinal symptoms with almost the same frequency as gynecological pain symptoms. Preoperatively existing gastrointestinal symptoms may translate into pathological gastrointestinal quality of life index (GIQLI) and low anterior resection syndrome scores (LARS). This prospective questionnaire-based case control study aims to assess the prevalence of gastrointestinal complaints reflected by changes in LARS and GIQLI scores in patients with colorectal deep endometriosis prior to surgical treatment and compare those to a healthy control group.
Methods
The study was conducted at the Hospital St. John of God in Vienna and included a total of 97 patients with histologically confirmed colorectal DE with radical surgical treatment and 96 women in whom DE was excluded via transvaginal sonography (TVS) or visually. Gastrointestinal symptoms reflected by LARS and GIQLI scores were evaluated presurgically and in controls.
Results
A total of 193 premenopausal patients were included in this study. A mean GIQLI of 90.7 ± 22.0 and 129.4 ± 11.1 was observed among patients and controls, respectively, showing a significantly higher morbidity concerning gastrointestinal symptoms and decreased quality of life (QoL) compared to healthy controls (p < 0.001). The LARS score results demonstrated that 18.6% of the patients with bowel DE presented with a major LARS and 27.8% with a minor LARS presurgically compared to 2.1% and 9.4% of control patients, respectively (p < 0.001).
Conclusion
Patients with colorectal DE experience a quality of gastrointestinal symptoms translating into a decreased QoL and pathological GIQLI and LARS scores already presurgically. As a consequence, these instruments should be interpreted with caution.



Similar content being viewed by others
References
Bulun SE, Yilmaz BD, Sison C, Miyazaki K, Bernardi L, Liu S, et al. Endometriosis. Endocr Rev. 2019;40(4):1048–79.
Adamson GD, Kennedy S, Hummelshoj L. Creating solutions in endometriosis: global collaboration through the World Endometriosis Research Foundation. J Endometr Pelvic Pain Disord. 2010;2(1):3–6.
Zondervan KT, Becker CM, Missmer SA. Endometriosis. N Engl J Med. 2020;382(13):1244–56.
Giudice LC, Kao LC. Endometriosis. Lancet. 2004;364(9447):1789–99.
Montanari E, Dauser B, Keckstein J, Kirchner E, Nemeth Z, Hudelist G. Association between disease extent and pain symptoms in patients with deep infiltrating endometriosis. Reprod Biomed Online. 2019;39(5):845–51.
Riiskjær M, Forman A, Kesmodel US, Andersen LM, Ljungmann K, Seyer-Hansen M. Pelvic pain and quality of life before and after laparoscopic bowel resection for rectosigmoid endometriosis: a prospective, observational study. Dis Colon Rectum. 2018;61(2):221–9.
Maroun P, Cooper MJ, Reid GD, Keirse MJ. Relevance of gastrointestinal symptoms in endometriosis. Aust N Z J Obstet Gynaecol. 2009;49(4):411–4.
Remorgida V, Ferrero S, Fulcheri E, Ragni N, Martin DC. Bowel endometriosis: presentation, diagnosis, and treatment. Obstet Gynecol Surv. 2007;62(7):461–70.
Roman H, Ness J, Suciu N, Bridoux V, Gourcerol G, Leroi AM, et al. Are digestive symptoms in women presenting with pelvic endometriosis specific to lesion localizations? A preliminary prospective study. Hum Reprod. 2012;27(12):3440–9.
Roman H, Vassilieff M, Gourcerol G, Savoye G, Leroi AM, Marpeau L, et al. Surgical management of deep infiltrating endometriosis of the rectum: pleading for a symptom-guided approach. Hum Reprod. 2010;26(2):274–81.
Fauconnier A, Staraci S, Huchon C, Roman H, Panel P, Descamps P. Comparison of patient-and physician-based descriptions of symptoms of endometriosis: a qualitative study. Hum Reprod. 2013;28(10):2686–94.
Seaman HE, Ballard KD, Wright JT, de Vries CS. Endometriosis and its coexistence with irritable bowel syndrome and pelvic inflammatory disease: findings from a national case-control study—part 2. BJOG. 2008;115(11):1392–6.
Abrão MS, Petraglia F, Falcone T, Keckstein J, Osuga Y, Chapron C. Deep endometriosis infiltrating the recto-sigmoid: critical factors to consider before management. Hum Reprod Update. 2015;21(3):329–39.
Hudelist G, English J, Thomas AE, Tinelli A, Singer CF, Keckstein J. Diagnostic accuracy of transvaginal ultrasound for non-invasive diagnosis of bowel endometriosis: systematic review and meta-analysis. Ultrasound Obstet Gynecol. 2011;37(3):257–63.
Gerges B, Li W, Leonardi M, Mol BW, Condous G. Meta-analysis and systematic review to determine the optimal imaging modality for the detection of rectosigmoid deep endometriosis. Ultrasound Obstet Gynecol. 2021;58(2):190–200.
Guerriero S, Ajossa S, Orozco R, Perniciano M, Jurado M, Melis GB, et al. Accuracy of transvaginal ultrasound for diagnosis of deep endometriosis in the rectosigmoid: systematic review and meta-analysis. Ultrasound Obstet Gynecol. 2016;47(3):281–9.
Eypasch E, Williams JI, Wood-Dauphinee S, Ure BM, Schmülling C, Neugebauer E, et al. Gastrointestinal quality of life index: development, validation and application of a new instrument. Br J Surg. 1995;82(2):216–22.
Juul T, Elfeki H, Christensen P, Laurberg S, Emmertsen KJ, Bager P. Normative data for the low anterior resection syndrome score (LARS score). Ann Surg. 2019;269(6):1124–8.
Riiskjaer M, Greisen S, Glavind-Kristensen M, Kesmodel US, Forman A, Seyer-Hansen M. Pelvic organ function before and after laparoscopic bowel resection for rectosigmoid endometriosis: a prospective, observational study. BJOG. 2016;123(8):1360–7.
Bokor A, Hudelist G, Dobó N, Dauser B, Farella M, Brubel R, et al. Low anterior resection syndrome following different surgical approaches for low rectal endometriosis: a retrospective multicenter study. Acta Obstet Gynecol Scand. 2021;100(5):860–7.
Hudelist G, Aas-Eng MK, Birsan T, Berger F, Sevelda U, Kirchner L, et al. Pain and fertility outcomes of nerve-sparing, full-thickness disk or segmental bowel resection for deep infiltrating endometriosis—a prospective cohort study. Acta Obstet Gynecol Scand. 2018;97(12):1438–46.
Ng A, Yang P, Wong S, Vancaillie T, Krishnan S. Medium to long-term gastrointestinal outcomes following disc resection of the rectum for treatment of endometriosis using a validated scoring questionnaire. Aust N Z J Obstet Gynaecol. 2016;56(4):408–13.
Croese AD, Lonie JM, Trollope AF, Vangaveti VN, Ho Y‑H. A meta-analysis of the prevalence of low anterior resection syndrome and systematic review of risk factors. Int J Surg. 2018;56:234–41.
Emmertsen KJ, Laurberg S. Low anterior resection syndrome score: development and validation of a symptom-based scoring system for bowel dysfunction after low anterior resection for rectal cancer. Ann Surg. 2012;255(5):922–8.
Acknowledgements
The authors thank Ayman Tammaa MD, Alexander Krell MD and Friedrich Reh MD for their assistance leading to the writing of this paper during the patient recruitment phase of the current study.
Author information
Authors and Affiliations
Contributions
L. M. Reh: study design, execution and analysis, manuscript writing; E. Darici: study design, execution and analysis; E. Montanari: study design, execution and analysis; B. Senft: statistical analysis; J. Keckstein: study design, manuscript writing; B. Dauser: study design, manuscript writing; G. Hudelist: study design, manuscript writing. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
L. M. Reh, E. Darici, E. Montanari, J. Keckstein, B. Senft, B. Dauser, and G. Hudelist declare that they have no competing interests.
Ethical approval
The study was approved on 17 November 2020 by the ethics committee/IRB of the Hospital St. John of God in Vienna, Austria.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Lena Maria Reh and Ezgi Darici contributed equally to this work.
Rights and permissions
About this article
Cite this article
Reh, L.M., Darici, E., Montanari, E. et al. Differences in intensity and quality of bowel symptoms in patients with colorectal endometriosis. Wien Klin Wochenschr 134, 772–778 (2022). https://doi.org/10.1007/s00508-022-02088-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-022-02088-x