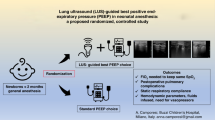
Summary
Background
Maintenance of the open lung alveoli in the expiration on mechanical ventilation in acute lung injury/acute respiratory distress syndrome (ALI/ARDS) remains challenging despite advances in lung imaging. The inspiratory lower inflection point (LIP) on the ventilator pressure–volume (P–V) curve estimates the required end-expiratory pressure for recruitment of alveolar consolidation. Alternatively, the end-expiratory pressure for recruitment of crater-like subpleural alveolar consolidation could be simply followed with ultrasound. These two methods for setting the ventilators positive end-expiratory pressure (PEEP) were compared.
Methods
The observational study in surgical/neurosurgical intensive care between October 2009 and November 2011 included 17 deeply sedated or relaxed patients. LIP was measured with continuous low-flow method, as a pressure in cmH2O. Expiratory levelling between lower border of subpleural consolidation and adjacent pleural line, which means lung recruitment, was followed with linear ultrasound probe. PEEP in cmH2O at which the levelling occurs was compared with LIP pressure.
Results
LIP pressure never exceeds the PEEP for recruitment of subpleural consolidations followed with ultrasound. A significant correlation (r = 0.839; p < 0.05) was found between two methods.
Conclusions
In this study, positive end-expiratory pressures for recruitment of subpleural consolidations followed by ultrasound always exceed the pressures measured with LIP. Respecting this, ultrasound method could be the guide for PEEP lung recruitment.
Zusammenfassung
Grundlagen
Die Erhaltung offener Lungenalveolen bei Exspiration während mechanischer Beatmung bei akuter Lungenverletzung und ARDS bleibt trotz Fortschritten in der Lungenbildgebung eine Herausforderung. Der inspiratorische untere Wendepunkt auf der Druck-Volumen Kurve des Ventilators schätzt den erforderlichen end-exspiratorischen Druck für das Recruitment einer alveolaren Konsolidierung. Als Alternative könnte der end-exspiratorische Druck für das Recruitment von Krater-ähnlichen subpleuraler alveolarer Konsolidierung einfach mit Ultraschall verfolgt werden. Diese beiden Methoden zur Festlegung des notwendigen positiven end-exspiratorischen Drucks des Ventilators wurden verglichen.
Methodik
Diese Beobachtungsstudie wurde auf einer chirurgisch/neurochirurgischen Intensivstation zwischen Oktober 2009 und November 2011 an 17 tief sedierten oder relaxierten Patienten durchgeführt. Der untere Wendepunkt wurde mit der kontinuierlichen Niedrig-Fluss Methode als ein Druck in cmH2O Wassersäule gemessen. Das exspiratorische Niveau zwischen der unteren Grenze subpleuraler Konsolidierung und der angrenzenden pleuralen Linie (= Lungen recruitment) wurde mittels eines linearen Schallkopfs beobachtet. Der in cm Wassersäule gemessene end-exspiratorische Druck, bei dem das Levelling stattfindet, wurde festgehalten und mit den Werten verglichen, die durch Bestimmung des unteren Wendepunktes erhoben wurden.
Ergebnisse
Der mittels Bestimmung des unteren Wendepunktes erhobene Druck war nie höher als der mittels Ultraschall gemessene positive end-exspiratorische Druck, der für das Recruitment subpleuraler Alveolen nötig ist. Es wurde eine signifikante Korrelation (r = 0,839, p < 0,05) zwischen beiden Methoden gefunden.
Schlussfolgerungen
Die mit Ultraschall erhobenen Werte waren in unserer Studie immer höher als die über Bestimmung des unteren Wendepunkts erhobenen Werte. Die Berücksichtigung dieser Ultraschallmethode könnte in Anbetracht unserer Ergebnisse zur Bestimmung des für Recruitment der Lunge notwendigen positiven end-exspiratorischen Drucks dienen.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Positive end-expiratory pressure (PEEP) prevents repetitive alveolar closure and reopening during ventilation which leads to ventilator-induced lung injury, along with lung overdistension [1, 2]. Optimal PEEP levels for alveolar recruitment in acute lung injury/acute respiratory distress syndrome (ALI/ARDS) are not defined. Similar clinical outcomes are seen with lower or higher PEEP levels [3]. According to other authors, higher PEEP levels appear to be safe and beneficial, whereas lower PEEP levels may even worsen the outcomes [4].
Besides computed tomography (CT) as the gold standard, electrical impedance tomography, oesophageal pressure-guided PEEP and empirical method, bedside observing of pressure volume (P–V) curves on the ventilator and estimating lower inflection point (LIP) on the inflating limb are useful, although contradictory procedures for setting the optimal PEEP. P–V curves correlate well with lung recruitment findings on CT [5]. The presence of LIP in the P–V curve, which appoints the start of massive inspiratory alveolar opening, indicates a significant potential for lung recruitment [6]. Among the quasi-static P–V curve methods [7, 8], the simplest one is the continuous-flow method [7].
Lung ultrasound is a well-established, repeatable diagnostic method in critical care units [9, 10]. Left ventricular hydrostatic lung oedema and permeability lung oedema, commonly named alveolar-interstitial syndromes, originally appeared to have the same ultrasound pattern [11]. Different later studies described specific ultrasound findings for permeability oedema in ALI/ARDS with possible assessment of lung recruitment [12–15]. Recently, a model for distinguishing between the left ventricular hydrostatic lung oedema and permeability lung oedema (ALI/ARDS) is described [16]. Lung consolidation is more typical for ALI/ARDS than elevated extravascular lung water which is recognised by B lines [17]. Recent works [18, 19] confirm ultrasound as a valuable method for the assessment of lung recruitment with a proposal for new aeration score [19].
Acute alveolar consolidations reaching visceral pleura are present in 98.5 % patients [20] with ALI/ARDS. They are easy to be found with ultrasound and could be followed in the whole respiratory cycle, if they do not escape behind the rib shadows.
The aim of the study was to determine the relation between LIP on the ventilator quasi-static P–V curve and PEEP for recruitment of subpleural consolidations followed by ultrasound. In other words, we compare LIP as a setting method for PEEP with ultrasound as a checking method for PEEP.
Methods
This study was carried out in the surgical/neurosurgical intensive care unit at the University Hospital Centre “Sisters of Mercy” from October 2009 to November 2011 by three anaesthesiologists/intensivists. The study was based on a routine unmodified measurement of quasi-static P–V curves with PEEP recruitment and was approved by the Hospital Ethics Committee, registered on Clinical Trials.gov; identifier NCT01478217. The written informed consent for the study was taken from patients next to kin. Patients with known pre-existing bronchial, parenchymal or pleural disorders were excluded, as well as patients with intracranial hypertension and pregnancy.
In total, 17 patients with criteria for pulmonary and extrapulmonary ALI/ARDS (Table 1) in semirecumbent position on volume assist-controlled, pressure-controlled or pressure-supported mechanical ventilation on the Draeger Evita 4 ventilator were included until starting measuring LIP. Severe hypovolemia was excluded by absence of variations for more than 15 % in maximal aortic velocities measured on left ventricular outflow track in apical 5-chamber view with pulse-wave Doppler in one respiratory cycle. Measurements were proceeded in between 48 h after starting mechanical ventilation. At least two crater-like subpleural consolidations not deeper than 1.5 cm from the pleural line measured on zero end-expiratory pressure (ZEEP) had to be visible by ultrasound: one in the non-dependent intercostal spaces and the other in dependent lower intercostal spaces in ipsilateral or contralateral hemithoraces. They all have to be visible in the entire respiratory cycle, without disappearing behind the rib shadow. We signed as non-dependent spaces those above mamilla and anterior to the middle axillary line. Linear transducer L38 5–10 MHz on Sonosite MicroMaxx in breast feature at a depth of 3.3–6 cm was used. Patients were sedated with midazolam–sufentanyl infusion or sufentanyl infusion and 40–120 mg propofol supplements for achieving apnoic conditions before starting LIP measurements [21]. Sedated patients with high risk of hypotension were temporarily partially relaxed with vecuronium. Three patients were periodically relaxed with vecuronium before measurements.
All existing ventilation modes were switched to volume-controlled ventilation with continuous flow, ZEEP, inspiratory oxygen fraction (FiO2) 1.0 and 5 s of tube disconnection. Propofol supplements were given as needed, dependent on haemodynamic. Hypotension was treated with increasing rates of noradrenalin when it has been included before or with ephedrine bolus, when mean arterial pressure failed less than 65 mmHg.
Tidal volumes were adapted to 6 ml/kg, if previous volumes differed. Respiratory rate was gradually decreased to 8/min, inversing inspiratory to expiratory ratio to 1.5:1. The inspiratory flow varied between 6–11 L/min [8, 22] dependent on set tidal volume, and end-expiratory flow of 0 L/min was followed on flow-time curve ruling out intrinsic PEEP. Tracheal tubes in size from 7.5 to 9 mm were used. P–V curves were freezed and LIP approximated on pressure abscissa. Patients with invisible LIP were excluded from the study.
Mechanical ventilation was then continued in pressure-supported or pressure-controlled mode, or volume assist-controlled mode (decelerating flow) with 6 ml/kg tidal volumes and with starting PEEP 2 cmH2O under measured LIP. Shredded lower border [20] of subpleural consolidation was followed with linear transducer in expiratory elevating, which means recruiting, towards adjacent pleural line which was at the same time sliding, ruling out atelectasis. Supplements of 2 cm H2O PEEP were added until levelling or near-levelling between the lower border of consolidation and adjacent pleural line (Fig. 1). Near-levelling was considered as lower border denivelation under pleural line not more than 0.25 cm.
Lowering tidal volumes started with plateau airway pressures more than 30 cmH2O. If levelling did not occur with 22 cmH2O PEEP, no more PEEP was added and the consolidation was signed as 22 or more. Ventilation was continued with PEEP according to LIP enlarged for 2 cmH2O.
Measured LIP value in cmH2O against mean PEEP in cmH2O resulted from levelling or near-levelling between lower consolidation border and abutting pleural line (recruitment PEEP) were logarithmically transformed by the Bland–Altman method and compared with Spearman rank-order correlation. Statistica 10, StatSoft Inc, Tulsa, USA was used as statistic software. Statistical significance was fixed at 0.05.
Results
Four consolidations in four different lung quadrants could be followed in only three patients, three different quadrants with consolidation in eight patients and two quadrants in six patients due to frequent disappearing of consolidations behind the rib shadow in recruiting expiratory phase. Altogether 48 consolidations were analysed, 19 in dependent and 29 in non-dependent intercostal spaces. Four consolidations were not recruitable—two in dependent and two in non-dependent spaces. Hypotension less than 60 mmHg of mean arterial pressure after propofol administration occurred in three out of eight sedated patients in time of LIP measurements; in six cases, incomplete muscle relaxation with vecuronium 2–6 mg was temporarily used because of the marked predicted hypotension risk (altogether nine relaxed patients in time of LIP measurements). No marked hypotension was registered during PEEP elevating in the time of ultrasound examination. No oxygen desaturations under the existing values were registered during LIP procedures on FiO2 1.0.
Measurements with patient characteristics are presented in Table 2 and Fig. 2. A statistically significant correlation was found between LIP and mean PEEP measurements for recruitment of subpleural consolidations followed with lung ultrasound (r = 0.839; p < 0.05).
Discussion
The main finding of this study is that pressure values for optimal PEEP determined by LIP from continuous-flow method never exceed PEEP for recruitment of subpleural consolidations followed with lung ultrasound. LIP values reached the PEEP recruitment values measured with ultrasound in six consolidations, only when 2 cmH2O PEEP over LIP were added like in clinical conditions. It means that LIP does not overestimate PEEP, and incomplete lung recruitment occurs relying only on LIP. This is sparing for the heart, especially the right and everything behind it (brain, splanchnicus).
Secondly, lung ultrasound following PEEP re-aeration of subpleural consolidations appears to be an easy and probably reliable method for PEEP up and downsizing, if we keep in mind that lung ultrasound could not detect overdistension and if we do not tend to recruit every alveolus. Apart from recruitment, PEEP contemporary hyperinflates normally aerated lung regions [23]. To put it crudely, the deeper the consolidation is, the higher PEEP is needed, but not uniformly for the whole lung. Superficial consolidation in the dependent zone needs higher PEEP for recruitment than a deep consolidation in the non-dependent zone. Although dependent zones in pulmonary ARDS are worth as poorly recruitable [6], we found only two dependent consolidations that did not re-aerate until 22 cmH2O of PEEP, together with the other two non-recruitable consolidations in non-dependent zones. This is probably because only crater-like consolidations (see Fig. 1) were followed, which seems to be more recruitable than hyperechoic homogenous subpleural consolidations.
Disappearing of B lines was not considered as recruitment criteria in this study, although they were commonly visible. A great study from Bouhemad et al. [19] with a good correlation between recruited end-expiratory lung volumes based on P–V curves and ultrasound re-aeration score already exists.
It is known that recruitment, rapid or slow, occurs above the LIP and even above the upper inflection point, along the entire P–V curve [24], but insisting on formatting the whole P–V curve with high tidal volumes could be sometimes unnecessary with abrupt thoracic venous stasis and abrupt venous return. Lower tidal volumes give steeper inflating limb and minimal changes for the LIP on the pressure abscissa vs. an estimation with high tidal volumes. After all, it is doubtful if LIP values are sometimes the same as the expiratory inflection point on deflation limb which is accepted as another point for optimal PEEP [22].
LIP measurement accuracy could be questionable due to possible right shift of the P–V curve due to high inspiratory flow or left shift due to low tidal volume, patient movements or even respiratory efforts on un-relaxed patients. The best ventilator flow control is probably on the rising inspiratory branch of the P–V curve, where LIP appears at the beginning. Continuous ventilation gas flow generates additional pressure gradient due to tube and airway resistance, and it was presumed that the dynamic P–V curves observed on the standard continuous-flow ventilation do not give accurate lung compliance course. However, studies [25] have shown that dynamic curves correlate well with static curves as long as the ventilator inspiratory flow is continuous, because the drop in pressure due to the inspiratory resistance will also be continuous. In that case, the curve steepness depends only on thorax–lung elastance. The shape of the P–V curve remains identical, but the rising branch of P–V curve shifts to the right on the pressure scale depending on the flow. The observed LIP shifts to the right [26] and lung recruitment pressure overestimation could be expected, but only minimal if low flow is used. Neuromuscular blockade seems to have only minor effect on elastic chest-wall properties [21, 27], whether the patients are with or without relaxation.
Lung hysteresis is the difference between higher end-expiratory lung volumes and lower inspiratory volumes in the time of LIP measurement, both by the same pressure values. This could be a reason for awareness of possible PEEP overestimation on P–V curve and possible lung expiratory overdistension. Hysteresis occurs due to airway and tissue resistance, inflammatory mediators and surfactant and is less marked with low-flow ventilation. The results of LIP measurements should be used considering all the respiratory and perfusion side effects on the whole body. Nevertheless, LIP is still considered a useful PEEP approximation method [28].
Even though high respiratory rate in the time of measurement (8/min) and keeping on low tidal volumes could be less reliable for estimation, such manoeuvres require less supplemental sedation, because patients tolerate such ventilation better and theoretically there should be less hypotension. Higher respiratory rates and tidal volumes would be even better, but with required higher inspiratory flow and a risk of present end-expiratory flow, which means auto-PEEP if inspiratory to expiratory ratio is set on 1.5:1. Draeger Evita 4 ventilator has no automated low-flow manoeuvre. However, hypotension remains the biggest problem with heavy sedation when muscle relaxation is unwanted.
We tried to optimise the ultrasound method and minimise the interobserver variations with defining maximal depth of subpleural consolidations and defining near-levelling of lower border of consolidation and abutting pleural line as a PEEP recruitment.
The first limiting factor of our study is a small number of patients. Only two subpleural consolidations per patient were the inclusion criteria due to their common getaway behind the rib shadow in recruitment phase. They poorly represent the whole lung surface. On the other hand, more homogeneous air and tissue distribution in patients with visible LIP than in those without LIP gave us the rationale to compare LIP measurements in six patients with only two ultrasound sites, dependent and non-dependent, representing lung quadrants with possible recruitment [6, 29]. There were no CT controls as a gold standard. The fact is that LIP is an inspiratory phenomenon, and ultrasound was done in expiration.
Ventilation modes were different during LIP and ultrasound assessments. This represents a bias, especially in spontaneous pressure support mode, which could contribute to dynamic intrinsic PEEP. Although the difference between collapsed crater-like consolidation in inspiration and expiration is obvious, ruling-out measurement in wrong time, we have no data about possible intrinsic PEEP.
Different flows were used for LIP measurements, because of limited minimal flows on the ventilator for different tidal volumes with fixed respiratory rate. According to the body mass, different tracheal tubes were used for different airways and different thorax–lung elastances. Lu et al. [7] found similar LIP with 3 L/min or 9 L/min flow on the same patient. We assume that the flow adjusted to the tidal volume is enough reliable for creating the initial limb on the P–V curve in seeking for LIP and safe for the patient. Minimal-allowed ventilator flow should be used.
Focusing only on expiratory pleural-line movements, we did not measure other respiratory parameters after continuing ventilation according to LIP. Possible gas-exchange improvements have to be included in further studies [30].
As a conclusion, in rapid everyday bedside measurements of respiratory elastance, ultrasound findings of subpleural consolidation recruitment could give us a useful tool for estimating optimal PEEP in ALI/ARDS, but with caution to overdistension as they exceed LIP values. Further studies will clarify the usefulness of lung ultrasound and subpleural consolidations in predicting the optimal PEEP.
References
Amato MB, Barbas CS, Medeiros DM, Magaldi RB, Schettino GP, Lorenzi-Filho G, et al. Effect of a protective ventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med. 1998;338:347–54.
The Acute Respiratory Distress Syndrome Network. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342:1301–8.
Brower RG, Lanken PN, MacIntyre N, Matthay MA, Morris A, et al. Higher versus lower positive end-expiratory pressures in patients with the acute respiratory distress syndrome. N Engl J Med. 2004;351:327–36.
Gattinoni L, Caironi P. Refining ventilatory treatment for acute lung injury and acute respiratory distress syndrome. JAMA. 2008;299:691–3.
Lu Q, Constantin JM, Nieszkowska A, Elman M, Vieira S, Rouby JJ. Measurement of alveolar derecruitment in patients with acute lung injury:computerized tomography versus pressure–volume curve. Crit Care. 2006;10:R95.
Vieira SR, Puybasset L, Lu Q, Richecoeur J, Cluzel P, Coriat P, et al. A scanographic assessment of pulmonary morphology in acute lung injury: significance of the lower inflection point detected on the lung pressure-volume curve. Am J Respir Crit Care Med. 1999;159:1612–23.
Lu Q, Vieira SR, Richecoeur J, Puybasset L, Kalfon P, Coriat P, et al. A simple automated method for measuring pressure-volume curves during mechanical ventilation. Am J Respir Crit Care Med. 1999;159:275–82.
Pestana D, Hernandez-Gancedo C, Royo C, Una R, Villagran MJ, Pena N, Criado A. Adjusting positive end-expiratory pressure and tidal volume in acute respiratory distress syndrome according to the pressure–volume curve. Acta Anaesthesiol Scand. 2003;47:326–34.
Bouhemad B, Zhang M, Lu Q, Rouby JJ. Clinical review: bedside lung ultrasound in critical care practice. Crit Care. 2007;11:205.
Lichtenstein D, editor. General ultrasound in the critically ill. Berlin: Springer; 2005.
Lichtenstein D, Meziere G, Biderman P, Gepner A, Barre O. The comet tail artifact. An ultrasound sign of alveolar-interstitial syndrome. Am J Respir Crit Care Med. 1997;156(5):1640–6.
Reissig A, Kroegel C. Transthoracic sonography of diffuse parenchymal lung disease: the role of comet tail artifacts. J Ultrasound Med. 2003;22(2):173–80.
Tsubo T, Sakai I, Suzuki A, Okawa H, Ishihara H, Matsuki A. Density detection in dependent left lung region using transesophageal echocardiography. Anesthesiology. 2001;94(5):793–8.
Tsubo T, Yatsu Y, Suzuki A, Iwakawa T, Okawa H, Ishihara H, Matsuki A. Daily changes of the area of density in the dependent lung region: evaluation using transesophageal echocardiography. Intensive Care Med. 2001;27:1881–6.
TsuboT, Yatsu Y, Tanabe T, Okawa H, Ishihara H, Matsuki A. Evaluation of density area in dorsal lung region during prone position using transesophageal echocardiography. Crit Care Med. 2004;32:83–7.
Copetti R, Soldati G, Copetti P. Chest sonography: a useful tool to differentiate acute cardiogenic pulmonary edema from acute respiratory distress syndrome. Cardiovasc Ultrasound. 2008;6:16–25.
Soldati G, Copetti R, Sher S. Sonographic interstitial syndrome: the sound of lung water. J Ultrasound Med. 2009;28:163–74.
Bouhemad B, Liu ZH, Arbelot C, Zhang M, Ferarri F, Le-Guen M, Girard M, Lu Q, Rouby JJ. Ultrasound assessment of antibiotic-induced pulmonary reaeration in ventilator-associated pneumonia. Crit Care Med. 2010;38:84–92.
Bouhemad B, Brisson H, Le-Guen M, Arbelot C, Lu Q, Rouby JJ. Bedside ultrasound assessment of positive end-expiratory pressure-induced lung recruitment. Am J Respir Crit Care Med. 2011;183:341–7.
Lichtenstein D, Meziere G, Seitz J. The dynamic air bronchogram: a lung ultrasound sign of alveolar consolidation ruling out atelectasis. Chest. 2009;135:1421–5.
Decailliot F, Demoule A, Maggiore SM, et al. Pressure-volume curves with and without muscle paralysis in acute respiratory distress syndrome. Intensive Care Med. 2006;32:1322–8.
Holzapfel L, Robert D, Perrin F, Blanc PL, Palmier B, Guerin C. Static pressure–volume curves and effect of positive end-expiratory pressure on gas exchange in adult respiratory distress syndrome. Crit Care Med. 1983;11(8):591–7.
Puybasset L, Muller JC, Cluzel P, Coriat P, Rouby JJ, The CT Scan ARDS Study Group. Regional distribution of gas and tissue in acute respiratory distress syndrome: III. Consequences on the effects of positive end-expiratory pressure. Intensive Care Med. 2000;26:1215–27.
Crotti S, Mascheroni D, Caironi P, et al. Recruitment and derecruitment during acute respiratory failure: a clinical study. Am J Respir Crit Care Med. 2001;164:131–40.
Ranieri M, Giuliani R, Fiore T, Dambrosio M, Milic-Emili J. Volume-pressure curve of the respiratory system predicts effects of PEEP in ARDS: “Occlusion” versus “Constant Flow” technique. Am J Respir Crit Care Med. 1994;149:19–27.
Rittner F, Döring M. Curves and loops in mechanical ventilation. Telford: Dräger Medical AG&CO.KG; 2005
Behrakis PK, Higgs BD, Baydur A, Zin WA, Milic-Emili J. Respiratory mechanics during halothane anesthesia and anesthesia-paralysis in humans. J Appl Physiol. 1983;55:1085–92.
Borelli M, Blanch L, Lucangelo U. Pressure–volume curves: useful in clinical practice. In: Kuhlen R, Moreno R, Ranieri M, Rhodes A, editors. Controversies in intensive care medicine. Berlin: ESICM, MWV Medizinisch Wissenschaftliche Verlagsgesellschaft; 2008.
Rouby JJ, Lu Q, Vieira S. Pressure/volume curves and lung computed tomography in acute respiratory distress syndrome. Eur Respir J Suppl. 2003;42:27s–36s.
Stefanidis K, Dimopoulos S, Tripodaki E-S, et al. Lung sonography and recruitment in patients with early acute respiratory distress syndrome: a pilot study. Crit Care. 2011;15:R185.
Conflict of interest
The authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rode, B., Vučić, M., Širanović, M. et al. Positive end-expiratory pressure lung recruitment: comparison between lower inflection point and ultrasound assessment. Wien Klin Wochenschr 124, 842–847 (2012). https://doi.org/10.1007/s00508-012-0303-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-012-0303-1