Abstract
Background
Systemic inflammation (SI) is linked to chronic kidney disease (CKD) progression and multiple complications. Data regarding SI biomarkers in pediatric patients are scarce. This case–control and cross-sectional study investigates the correlation of neutrophil–lymphocyte ratio (NLR), platelet-lymphocyte ratio (PLR), total iron binding capacity (TIBC) and serum albumin to serum interleukin-6 (IL-6).
Methods
NLR and PLR were measured in 53 patients (median age: 12.9 years), including 17 on dialysis and 36 with a median glomerular filtration rate of 39 ml/min/1.73m2, and in 25 age and sex-matched healthy controls. Iron profile, serum albumin and IL-6 were measured in the patient group. IL-6 levels > 3rd quartile were classified as high.
Results
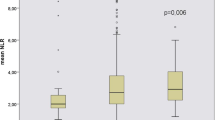
Patients presented higher NLR and PLR and particularly those on dialysis (p < 0.001 and p = 0.001). We observed a significant correlation between natural logarithm (ln) of IL-6 (lnIL-6) and NLR (rs = 0.344, p = 0.014), serum albumin (rs = -0.350, p = 0.011) and TIBC (rs = -0.345, p = 0.012) after adjustment for CKD stage, while the correlation between lnIL-6 and PLR was not significant (rs = 0.206, p = 0.151). Combination of NLR, serum albumin and TIBC predicted high IL-6 (13 patients) with an AUC of 0.771 (95% CI 0.608–0.943). Pairing of NLR ≥ 1.7 and TIBC ≤ 300 μg/dL exhibited the highest sensitivity (76.9%), while incorporating serum albumin ≤ 3.8 g/dL along with them achieved the highest specificity (95%) for detecting high IL-6 levels.
Conclusion
Both NLR and PLR levels increase in CKD, especially in patients on chronic dialysis. NLR, rather than PLR, along with TIBC and serum albumin, are associated with IL-6 in pediatric CKD.
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information



Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Akchurin OM, Kaskel F (2015) Update on inflammation in chronic kidney disease. Blood Purif 39:84–92
Cheung WW, Paik KH, Mak RH (2010) Inflammation and cachexia in chronic kidney disease. Pediatr Nephrol 25:711–724
Holle J, Querfeld U, Kirchner M, Anninos A, Okun J, Thurn-Valsassina D, Bayazit A, Niemirska A, Canpolat N, Bulut IK, Duzova A, Anarat A, Shroff R, Bilginer Y, Caliskan S, Candan C, Harambat J, Özcakar ZB, Soylemezoglu O, Tschumi S, Habbig S, Yilmaz E, Balat A, Zurowska A, Cakar N, Kranz B, Ertan P, Melk A, Azukaitis K, Schaefer F (2019) Indoxyl sulfate associates with cardiovascular phenotype in children with chronic kidney disease. Pediatr Nephrol 34:2571–2582
Karava V, Kondou A, Dotis J, Christoforidis A, Taparkou A, Farmaki E, Kollios K, Liakopoulos V, Printza N (2023) Association between adipokine profile, systemic inflammation, muscle and protein energy wasting in children with chronic kidney disease. J Ren Nutr 33:629–638
Akchurin O, Patino E, Dalal V, Meza K, Bhatia D, Brovender S, Zhu YS, Cunningham-Rundles S, Perelstein E, Kumar J, Rivella S, Choi ME (2019) Interleukin-6 Contributes to the Development of Anemia in Juvenile CKD. Kidney Int Rep 4:470–483
Yamamura-Miyazaki N, Michigami T, Ozono K, Yamamoto K, Hasuike Y (2022) Factors associated with 1-year changes in serum fibroblast growth factor 23 levels in pediatric patients with chronic kidney disease. Clin Exp Nephrol 26:1014–1021
Meza K, Biswas S, Zhu YS, Gajjar A, Perelstein E, Kumar J, Akchurin O (2021) Tumor necrosis factor-alpha is associated with mineral bone disorder and growth impairment in children with chronic kidney disease. Pediatr Nephrol 36:1579–1587
Lai HL, Kartal J, Mitsnefes M (2007) Hyperinsulinemia in pediatric patients with chronic kidney disease: the role of tumor necrosis factor-alpha. Pediatr Nephrol 22:1751–1756
Don BR, Kaysen G (2004) Serum albumin: relationship to inflammation and nutrition. Semin Dial 17:432–437
Bross R, Zitterkoph J, Pithia J, Benner D, Rambod M, Kovesdy CP, Kopple JD, Kalantar-Zadeh K (2009) Association of serum total iron-binding capacity and its changes over time with nutritional and clinical outcomes in hemodialysis patients. Am J Nephrol 29:571–581
Graterol Torres F, Molina M, Soler-Majoral J, Romero-González G, Rodríguez Chitiva N, Troya-Saborido M, SociasRullan G, Burgos E, Paúl Martínez J, UrrutiaJou M, Cañameras C, RieraSadurní J, Vila A, Bover J (2022) Evolving concepts on inflammatory biomarkers and malnutrition in chronic kidney disease. Nutrients 4:4297
Brito GMC, Fontenele AMM, Carneiro ECRL, Nogueira IAL, Cavalcante TB, Vale AAM, Monteiro SCM, Salgado Filho N (2021) Neutrophil-to-Lymphocyte and Platelet-to-Lymphocyte ratios in nondialysis chronic kidney patients. Int J Inflam 2021:6678960
Okyay GU, Inal S, Oneç K, Er RE, Paşaoğlu O, Paşaoğlu H, Derici U, Erten Y (2013) Neutrophil to lymphocyte ratio in evaluation of inflammation in patients with chronic kidney disease. Ren Fail 35:29–36
Li P, Xia C, Liu P, Peng Z, Huang H, Wu J, He Z (2020) Neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio in evaluation of inflammation in non-dialysis patients with end-stage renal disease (ESRD). BMC Nephrol 21:511
Ahbap E, Sakaci T, Kara E, Sahutoglu T, Koc Y, Basturk T, Sevinc M, Akgol C, Kayalar AO, Ucar ZA, Bayraktar F, Unsal A (2016) Neutrophil-to-lymphocyte ratio and platelet-tolymphocyte ratio in evaluation of inflammation in end-stage renal disease. Clin Nephrol 85:199–208
Turkmen K, Guney I, Yerlikaya FH, Tonbul HZ (2012) The relationship between neutrophil-to-lymphocyte ratio and inflammation in end-stage renal disease patients. Ren Fail 34:155–159
Valga F, Monzón T, Henriquez F, Antón-Pérez G (2019) Neutrophil-to-lymphocyte and platelet-to-lymphocyte ratios as biological markers of interest in kidney disease. Nefrologia 39:243–249
Cetın N, Kocaturk E, Tufan AK, Kıraz ZK, Alatas O (2022) Immature granulocytes as biomarkers of inflammation in children with predialysis chronic kidney disease. Pediatr Nephrol 38:219–225
Schwartz GJ, Muñoz A, Schneider MF, Mak RH, Kaskel F, Warady BA, Furth SL (2009) New equations to estimate GFR in children with CKD. J Am Soc Nephrol 20:629–637
Eleftheriadis T, Liakopoulos V, Antoniadi G, Stefanidis I (2010) Which is the best way for estimating transferrin saturation? Ren Fail 32:1022–1023
Honda H, Qureshi AR, Heimbürger O, Barany P, Wang K, Pecoits-Filho R, Stenvinkel P, Lindholm B (2006) Serum albumin, C-reactive protein, interleukin 6, and fetuin a as predictors of malnutrition, cardiovascular disease, and mortality in patients with ESRD. Am J Kidney Dis 47:139–148
Tripepi G, Mallamaci F, Zoccali C (2005) Inflammation markers, adhesion molecules, and all-cause and cardiovascular mortality in patients with ESRD: searching for the best risk marker by multivariate modeling. J Am Soc Nephrol 16(Suppl 1):S83–S88
Zhong X, Ma A, Zhang Z, Liu Y, Liang G (2021) Neutrophil-to-lymphocyte ratio as a predictive marker for severe pediatric sepsis. Transl Pediatr 10:657–665
Eun S, Ho IG, Bae GE, Kim H, Koo CM, Kim MK, Yoon SH (2021) Neutrophil-to-lymphocyte ratio for the diagnosis of pediatric acute appendicitis: a systematic review and meta-analysis. Eur Rev Med Pharmacol Sci 25:7097–7107
Han SY, Lee IR, Park SJ, Kim JH, Il SJ (2016) Usefulness of neutrophil-lymphocyte ratio in young children with febrile urinary tract infection. Korean J Pediatr 59:139–144
Omran A, Awad H, Ibrahim M, El-Sharkawy S, Elfiky S, Rezk AR (2022) Lung ultrasound and neutrophil lymphocyte ratio in early diagnosis and differentiation between viral and bacterial pneumonia in young children. Children (Basel) 9:1457
Aryani IGAD, Yantie NPVK, Gunawijaya E, Gustawan IW (2021) Correlation between neutrophil-to-lymphocyte ratio, platelet-to-lymphocyte ratio and mean platelet volume with severity of carditis in children with rheumatic fever. Cardiol Young 32:1396–1400
O’Brien CE, Price ET (2013) The blood neutrophil to lymphocyte ratio correlates with clinical status in children with cystic fibrosis: a retrospective study. PLoS One 8:e77420
Milas GP, Fragkos S (2021) Neutrophil to lymphocyte ratio and gastrointestinal involvement among Henoch Schonlein purpura patients: a systematic review and meta-analysis. J Pediatr Gastroenterol Nutr 73:437–443
Chang LS, Lin YJ, Yan JH, Guo MMH, Lo MH, Kuo HC (2020) Neutrophil-to-lymphocyte ratio and scoring system for predicting coronary artery lesions of Kawasaki disease. BMC Pediatr 20:398
Lano G, Sallée M, Pelletier M, Bataille S, Fraisse M, McKay N, Brunet P, Dou L, Burtey S (2022) Neutrophil:lymphocyte ratio correlates with the uremic toxin indoxyl sulfate and predicts the risk of death in patients on hemodialysis. Nephrol Dial Transplant 37:2528–2537
Turkmen K, Erdur FM, Ozcicek F, Ozcicek A, Akbas EM, Ozbicer A, Demirtas L, Turk S, Tonbul HZ (2013) Platelet-to-lymphocyte ratio better predicts inflammation than neutrophil-to-lymphocyte ratio in end-stage renal disease patients. Hemodial Int 17:391–396
Moosmann J, Krusemark A, Dittrich S, Ammer T, Rauh M, Woelfle J, Metzler M, Zierk J (2022) Age- and sex-specific pediatric reference intervals for neutrophil-to-lymphocyte ratio, lymphocyte-to-monocyte ratio, and platelet-to-lymphocyte ratio. Int J Lab Hematol 44:296–301
An X, Mao HP, Wei X, Chen JH, Yang X, Li ZB, Yu XQ, Li ZJ (2012) Elevated neutrophil to lymphocyte ratio predicts overall and cardiovascular mortality in maintenance peritoneal dialysis patients. Int Urol Nephrol 44:1521–1528
Li H, Lu X, Xiong R, Wang S (2017) High neutrophil-to-lymphocyte ratio predicts cardiovascular mortality in chronic hemodialysis patients. Mediators Inflamm 2017:9327136
Abe T, Kato S, Tsuruta Y, Sugiura S, Katsuno T, Kosugi T, Tsuboi N, Matsuo S, Maruyama S (2015) Neutrophil/lymphocyte ratio as a predictor of cardiovascular events in incident dialysis patients: a Japanese prospective cohort study. Clin Exp Nephrol 19:718–724
Neuen BL, Leather N, Greenwood AM, Gunnarsson R, Cho Y, Mantha ML (2016) Neutrophil-lymphocyte ratio predicts cardiovascular and all-cause mortality in hemodialysis patients. Ren Fail 38:70–76
Soehnlein O (2012) Multiple roles for neutrophils in atherosclerosis. Circ Res 110:875–888
Hedrick CC (2015) Lymphocytes in atherosclerosis. Arterioscler Thromb Vasc Biol 35:253–257
Yuan Q, Wang J, Peng Z, Zhou Q, Xiao X, Xie Y, Wang W, Huang L, Tang W, Sun D, Zhang L, Wang F, Zhao MH, Tao L, He K, Xu H, C-STRIDE study group (2019) Neutrophil-to-lymphocyte ratio and incident end-stage renal disease in Chinese patients with chronic kidney disease: results from the Chinese Cohort Study of Chronic Kidney Disease (C-STRIDE). J Transl Med 17:86
Kocyigit I, Eroglu E, Unal A, Sipahioglu MH, Tokgoz B, Oymak O, Utas C (2013) Role of neutrophil/lymphocyte ratio in prediction of disease progression in patients with stage-4 chronic kidney disease. J Nephrol 26:358–365
Altunoren O, Akkus G, Sezal DT, Ciftcioglu M, Guzel FB, Isiktas S, Torun GI, Uyan M, Sokmen MF, Sevim HA, Sarısık FN, Senel ME, Erken E, Gungor O (2019) Does neutrophyl to lymphocyte ratio really predict chronic kidney disease progression? Int Urol Nephrol 51:129–137
Fertrin KY (2020) Diagnosis and management of iron deficiency in chronic inflammatory conditions (CIC): is too little iron making your patient sick? Hematology Am Soc Hematol Educ Program 2020:478–486
Okuda Y, Obi Y, Streja E, Laster M, Rhee C, Langman CB, Jernigan SM, Salusky IB, Tentori F, Schreiber MJ, Brunelli SM, Kalantar-Zadeh K (2019) Serum albumin and hospitalization among pediatric patients with end-stage renal disease who started dialysis therapy. Pediatr Nephrol 34:1799–1809
Amaral S, Hwang W, Fivush B, Neu A, Frankenfield D, Furth S (2008) Serum albumin level and risk for mortality and hospitalization in adolescents on hemodialysis. Clin J Am Soc Nephrol 3:759–767
Wong CS, Hingorani S, Gillen DL, Sherrard DJ, Watkins SL, Brandt JR, Ball A, Stehman-Breen CO (2002) Hypoalbuminemia and risk of death in pediatric patients with end-stage renal disease. Kidney Int 61:630–637
Oliveira EA, Cheung WW, Toma KG, Mak RH (2019) Muscle wasting in chronic kidney disease. Pediatr Nephrol 33:789–798
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflicts of interest
None declared.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Karava, V., Kondou, A., Dotis, J. et al. Exploring systemic inflammation in children with chronic kidney disease: correlates of interleukin 6. Pediatr Nephrol 39, 1567–1576 (2024). https://doi.org/10.1007/s00467-023-06234-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06234-z