Abstract
Background
In patients requiring mechanical circulatory support (MCS), the incidence of acute kidney injury (AKI) is between 37 and 63%. In this study, we performed an exploratory analysis evaluating the relationship of multiple urine biomarkers with AKI development in pediatric MCS patients.
Methods
This is a single center retrospective study in a pediatric cohort receiving MCS from August 2014 to November 2020. We measured 14 urine biomarkers of kidney injury on day 1 following MCS initiation and analyzed their association with development of AKI in the first 7 days of MCS initiation.
Results
Sixty patients met inclusion criteria. Patients with AKI were more likely to be supported by venoarterial extracorporeal membrane oxygenation (65% vs. 8.3%, p < 0.001), compared to the no AKI group and less likely to have ventricular assist devices (10% vs. 50%, p < 0.001). There was a significant increase in the median urine albumin and urine osteoactivin in the AKI group, compared to the no AKI group (p = 0.020 and p = 0.018, respectively). When normalized to urine creatinine (UCr), an increased log osteoactivin/UCr was associated with higher odds of AKI development (OR: 2.05; 95% CI: 1.07, 4.44; p = 0.028), and higher log epidermal growth factor (EGF)/UCr (OR: 0.41; 95% CI: 0.15, 0.96) was associated with decreased odds of AKI.
Conclusions
Early increase in urine osteoactivin is associated with AKI development within 7 days of MCS initiation in pediatric patients. Contrary, an increased urine EGF is associated with kidney protection.
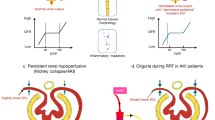
Graphical Abstract

A higher resolution version of the Graphical abstract is available as Supplementary information

Similar content being viewed by others
References
Sutherland SM, Byrnes JJ, Kothari M, Longhurst CA, Dutta S, Garcia P, Goldstein SL (2015) AKI in hospitalized children: comparing the pRIFLE, AKIN, and KDIGO definitions. Clin J Am Soc Nephrol 10:554–561
Kaddourah A, Basu RK, Bagshaw SM, Goldstein SL, AWARE Investigators (2017) Epidemiology of acute kidney injury in critically ill children and young adults. N Engl J Med 376:11–20
Selewski DT, Jordan BK, Askenazi DJ, Dechert RE, Sarkar S (2013) Acute kidney injury in asphyxiated newborns treated with therapeutic hypothermia. J Pediatr 162:725-729.e1
Carmody JB, Swanson JR, Rhone ET, Charlton JR (2014) Recognition and reporting of AKI in very low birth weight infants. Clin J Am Soc Nephrol 9:2036–2043
Zappitelli M, Moffett BS, Hyder A, Goldstein SL (2011) Acute kidney injury in non-critically ill children treated with aminoglycoside antibiotics in a tertiary healthcare centre: a retrospective cohort study. Nephrol Dial Transplant 26:144–150
Jetton JG, Boohaker LJ, Sethi SK, Wazir S, Rohatgi S, Soranno DE, Chishti AS, Woroniecki R, Mammen C, Swanson JR, Sridhar S, Wong CS, Kupferman JC, Griffin RL, Askenazi DJ, NK Collaborative (NKC) (2017) Incidence and outcomes of neonatal acute kidney injury (AWAKEN): a multicentre, multinational, observational cohort study. Lancet Child Adolesc Health 1:184–194
Alkandari O, Eddington KA, Hyder A, Gauvin F, Ducruet T, Gottesman R, Phan V, Zappitelli M (2011) Acute kidney injury is an independent risk factor for pediatric intensive care unit mortality, longer length of stay and prolonged mechanical ventilation in critically ill children: a two-center retrospective cohort study. Crit Care 15:R146
Koralkar R, Ambalavanan N, Levitan EB, McGwin G, Goldstein S, Askenazi D (2011) Acute kidney injury reduces survival in very low birth weight infants. Pediatr Res 69:354–358
Askenazi DJ, Griffin R, McGwin G, Carlo W, Ambalavanan N (2009) Acute kidney injury is independently associated with mortality in very low birthweight infants: a matched case-control analysis. Pediatr Nephrol 24:991–997
Askenazi DJ, Koralkar R, Hundley HE, Montesanti A, Patil N, Ambalavanan N (2013) Fluid overload and mortality are associated with acute kidney injury in sick near-term/term neonate. Pediatr Nephrol 28:661–666
Xu X, Nie S, Zhang A, Mao J, Liu HP, Xia H, Xu H, Liu Z, Feng S, Zhou W, Liu X, Yang Y, Tao Y, Feng Y, Chen C, Wang M, Zha Y, Feng JH, Li Q, Ge S, Chen J, He Y, Teng S, Hao C, Liu BC, Tang Y, He W, He P, Hou FF (2018) Acute kidney injury among hospitalized children in China. Clin J Am Soc Nephrol 13:1791–1800
Searns JB, Gist KM, Brinton JT, Pickett K, Todd J, Birkholz M, Soranno DE (2020) Impact of acute kidney injury and nephrotoxic exposure on hospital length of stay. Pediatr Nephrol 35:799–806
Chawla LS, Bellomo R, Bihorac A, Goldstein SL, Siew ED, Bagshaw SM, Bittleman D, Cruz D, Endre Z, Fitzgerald RL, Forni L, Kane-Gill SL, Hoste E, Koyner J, Liu KD, Macedo E, Mehta R, Murray P, Nadim M, Ostermann M, Palevsky PM, Pannu N, Rosner M, Wald R, Zarbock A, Ronco C, Kellum JA, Acute Disease Quality Initiative Workgroup 16 2 (2017) Acute kidney disease and renal recovery: consensus report of the Acute Disease Quality Initiative (ADQI) 16 Workgroup. Nat Rev Nephrol 13:241–257
Zarbock A, Kellum JA, Schmidt C, Van Aken H, Wempe C, Pavenstadt H, Boanta A, Gerss J, Meersch M (2016) Effect of early vs delayed initiation of renal replacement therapy on mortality in critically ill patients with acute kidney injury: the ELAIN randomized clinical trial. JAMA 315:2190–2199
Meersch M, Kullmar M, Schmidt C, Gerss J, Weinhage T, Margraf A, Ermert T, Kellum JA, Zarbock A (2018) Long-term clinical outcomes after early initiation of RRT in critically ill patients with AKI. J Am Soc Nephrol 29:1011–1019
Goldstein SL, Dahale D, Kirkendall ES, Mottes T, Kaplan H, Muething S, Askenazi DJ, Henderson T, Dill L, Somers MJG, Kerr J, Gilarde J, Zaritsky J, Bica V, Brophy PD, Misurac J, Hackbarth R, Steinke J, Mooney J, Ogrin S, Chadha V, Warady B, Ogden R, Hoebing W, Symons J, Yonekawa K, Menon S, Abrams L, Sutherland S, Weng P, Zhang F, Walsh K (2020) A prospective multi-center quality improvement initiative (NINJA) indicates a reduction in nephrotoxic acute kidney injury in hospitalized children. Kidney Int 97:580–588
Thongprayoon C, Cheungpasitporn W, Lertjitbanjong P, Aeddula NR, Bathini T, Watthanasuntorn K, Srivali N, Mao MA, Kashani K (2019) Incidence and impact of acute kidney injury in patients receiving extracorporeal membrane oxygenation: a meta-analysis. J Clin Med 8:981
Thongprayoon C, Lertjitbanjong P, Cheungpasitporn W, Hansrivijit P, Fulop T, Kovvuru K, Kanduri SR, Davis PW, Vallabhajosyula S, Bathini T, Watthanasuntorn K, Prasitlumkum N, Chokesuwattanaskul R, Ratanapo S, Mao MA, Kashani K (2020) Incidence and impact of acute kidney injury on patients with implantable left ventricular assist devices: a meta-analysis. Ren Fail 42:495–512
McCullough PA, Bouchard J, Waikar SS, Siew ED, Endre ZH, Goldstein SL, Koyner JL, Macedo E, Doi K, Di Somma S, Lewington A, Thadhani R, Chakravarthi R, Ice C, Okusa MD, Duranteau J, Doran P, Yang L, Jaber BL, Meehan S, Kellum JA, Haase M, Murray PT, Cruz D, Maisel A, Bagshaw SM, Chawla LS, Mehta RL, Shaw AD, Ronco C (2013) Implementation of novel biomarkers in the diagnosis, prognosis, and management of acute kidney injury: executive summary from the tenth consensus conference of the Acute Dialysis Quality Initiative (ADQI). Contrib Nephrol 182:5–12
Stanski N, Menon S, Goldstein SL, Basu RK (2019) Integration of urinary neutrophil gelatinase-associated lipocalin with serum creatinine delineates acute kidney injury phenotypes in critically ill children. J Crit Care 53:1–7
Mishra J, Dent C, Tarabishi R, Mitsnefes MM, Ma Q, Kelly C, Ruff SM, Zahedi K, Shao M, Bean J, Mori K, Barasch J, Devarajan P (2005) Neutrophil gelatinase-associated lipocalin (NGAL) as a biomarker for acute renal injury after cardiac surgery. Lancet 365:1231–1238
Devarajan P (2008) Neutrophil gelatinase-associated lipocalin–an emerging troponin for kidney injury. Nephrol Dial Transplant 23:3737–3743
Nickolas TL, O’Rourke MJ, Yang J, Sise ME, Canetta PA, Barasch N, Buchen C, Khan F, Mori K, Giglio J, Devarajan P, Barasch J (2008) Sensitivity and specificity of a single emergency department measurement of urinary neutrophil gelatinase-associated lipocalin for diagnosing acute kidney injury. Ann Intern Med 148:810–819
Mostafa EA, Shahin KM, El Midany AAH, Hassaballa AS, El-Sokkary IN, Gamal MA, Elsaid ME, ElBarbary MG, Khorshid R, Elelwany SE (2022) Validation of cardiac surgery-associated neutrophil gelatinase-associated lipocalin score for prediction of cardiac surgery-associated acute kidney injury. Heart Lung Circ 31:272–277
Mishra J, Ma Q, Prada A, Mitsnefes M, Zahedi K, Yang J, Barasch J, Devarajan P (2003) Identification of neutrophil gelatinase-associated lipocalin as a novel early urinary biomarker for ischemic renal injury. J Am Soc Nephrol 14:2534–2543
Mori K, Lee HT, Rapoport D, Drexler IR, Foster K, Yang J, Schmidt-Ott KM, Chen X, Li JY, Weiss S, Mishra J, Cheema FH, Markowitz G, Suganami T, Sawai K, Mukoyama M, Kunis C, D’Agati V, Devarajan P, Barasch J (2005) Endocytic delivery of lipocalin-siderophore-iron complex rescues the kidney from ischemia-reperfusion injury. J Clin Invest 115:610–621
Askenazi DJ, Koralkar R, Patil N, Halloran B, Ambalavanan N, Griffin R (2016) Acute kidney injury urine biomarkers in very low-birth-weight infants. Clin J Am Soc Nephrol 11:1527–1535
Wasung ME, Chawla LS, Madero M (2015) Biomarkers of renal function, which and when? Clin Chim Acta 438:350–357
Colhoun HM, Marcovecchio ML (2018) Biomarkers of diabetic kidney disease. Diabetologia 61:996–1011
Saeidi B, Koralkar R, Griffin RL, Halloran B, Ambalavanan N, Askenazi DJ (2015) Impact of gestational age, sex, and postnatal age on urine biomarkers in premature neonates. Pediatr Nephrol 30:2037–2044
Dobiliene D, Masalskiene J, Rudaitis S, Vitkauskiene A, Peciulyte J, Kevalas R (2019) Early diagnosis and prognostic value of acute kidney injury in critically ill patients. Medicina (Kaunas) 55:506
Goldstein SL, Mottes T, Simpson K, Barclay C, Muething S, Haslam DB, Kirkendall ES (2016) A sustained quality improvement program reduces nephrotoxic medication-associated acute kidney injury. Kidney Int 90:212–221
Selewski DT, Charlton JR, Jetton JG, Guillet R, Mhanna MJ, Askenazi DJ, Kent AL (2015) Neonatal acute kidney injury. Pediatrics 136:e463–e473
Schwartz GJ, Munoz A, Schneider MF, Mak RH, Kaskel F, Warady BA, Furth SL (2009) New equations to estimate GFR in children with CKD. J Am Soc Nephrol 20:629–637
Hessey E, Ali R, Dorais M, Morissette G, Pizzi M, Rink N, Jouvet P, Lacroix J, Phan V, Zappitelli M (2017) Evaluation of height-dependent and height-independent methods of estimating baseline serum creatinine in critically ill children. Pediatr Nephrol 32:1953–1962
Krawczeski CD, Goldstein SL, Woo JG, Wang Y, Piyaphanee N, Ma Q, Bennett M, Devarajan P (2011) Temporal relationship and predictive value of urinary acute kidney injury biomarkers after pediatric cardiopulmonary bypass. J Am Coll Cardiol 58:2301–2309
Harrell FE Jr, Lee KL, Mark DB (1996) Multivariable prognostic models: issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat Med 15:361–387
Brisco MA, Testani JM, Cook JL (2016) Renal dysfunction and chronic mechanical circulatory support: from patient selection to long-term management and prognosis. Curr Opin Cardiol 31:277–286
Menez S, Ju W, Menon R, Moledina DG, Thiessen Philbrook H, McArthur E, Jia Y, Obeid W, Mansour SG, Koyner JL, Shlipak MG, Coca SG, Garg AX, Bomback AS, Kellum JA, Kretzler M, Parikh CR, Translational research investigating biomarker endpoints in AKI (TRIBE-AKI) Consortium and the Kidney Precision Medicine Project (2021) urinary EGF and MCP-1 and risk of CKD after cardiac surgery. JCI Insight 6:e147464
Worawichawong S, Worawichawong S, Radinahamed P, Muntham D, Sathirapongsasuti N, Nongnuch A, Assanatham M, Kitiyakara C (2016) Urine epidermal growth factor, monocyte chemoattractant protein-1 or their ratio as biomarkers for interstitial fibrosis and tubular atrophy in primary glomerulonephritis. Kidney Blood Press Res 41:997–1007
Patel-Chamberlin M, Wang Y, Satirapoj B, Phillips LM, Nast CC, Dai T, Watkins RA, Wu X, Natarajan R, Leng A, Ulanday K, Hirschberg RR, Lapage J, Nam EJ, Haq T, Adler SG (2011) Hematopoietic growth factor inducible neurokinin-1 (Gpnmb/osteoactivin) is a biomarker of progressive renal injury across species. Kidney Int 79:1138–1148
Zhou L, Zhuo H, Ouyang H, Liu Y, Yuan F, Sun L, Liu F, Liu H (2017) Glycoprotein non-metastatic melanoma protein b (Gpnmb) is highly expressed in macrophages of acute injured kidney and promotes M2 macrophages polarization. Cell Immunol 316:53–60
Acknowledgements
We acknowledge the support of the ECMO and clinical teams in the PICU, NICU, and CTICU, at Nationwide Children’s Hospital.
Funding
This work was supported by a grant from the Nationwide Children’s Heart Center intramural program (51108–0005-1222).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Graphical abstract
(PPTX 2200 kb)
Supplementary Table 1
(DOCX 14 kb)
Supplementary Table 2
(DOCX 18 kb)
Supplementary Table 3
(DOCX 15 kb)
Supplementary Table 4
(DOCX 15 kb)
Supplementary Table 5
(DOCX 14 kb)

Supplementary figure 1
Adjusted relationship between selected biomarkers and the probability of stage 2 or 3 AKI. The shaded region shows 95% confidence limits. UCr, urine creatinine (mg/mL); EGF, epidermal growth factor (ng/mL); NGAL, neutrophil gelatinase-associated lipocalin (ng/mL); KIM-1, kidney injury molecule-1 (ng/mL) (PNG 242 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Harris, R.E., Yates, A.R., Nandi, D. et al. Urinary biomarkers associated with acute kidney injury in pediatric mechanical circulatory support patients. Pediatr Nephrol 39, 569–577 (2024). https://doi.org/10.1007/s00467-023-06089-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06089-4