Abstract
Background
Idiopathic intracranial hypertension is characterized by increased intracranial pressure with unidentified pathology. Despite its use as the first-line treatment, data on acetazolamide’s effectiveness and safety in pediatric idiopathic intracranial hypertension is sparse. This study's objective was to assess those issues and the need for routine blood gas monitoring during treatment.
Methods
Retrospective observational cohort study, based on multicenter computerized medical charts of pediatric patients with idiopathic intracranial hypertension diagnosed between 2007–2018 in three medical centers serving one metropolitan area (an estimated population of 400,000 children). Clinical and laboratory data of children up to 18 years old, fulfilling the Friedman criteria and taking acetazolamide, were collected and analyzed.
Results
Sixty-eight patients were included with a mean acetazolamide treatment duration of 8.5 months and a median maximal dose 18 mg/kg/d. Sixty-two children had mild (76%), moderate (13%), or severe (1.5%) metabolic acidosis. At least one adverse effect (neurologic, gastrointestinal, renal) was recorded among 27% of patients. No significant difference was found between the mean pH of children with or without clinical adverse effects (p = 0.35). No correlation was found between laboratory acidosis and adverse effect severity (p = 0.3), or between median acetazolamide dose and acidosis level (p = 0.57).
Conclusions
Although laboratory finding of metabolic acidosis is common among patients with idiopathic intracranial hypertension treated with acetazolamide, it is not correlated with clinics. Therefore, we recommend sending blood tests during acetazolamide treatment based on clinical judgment.
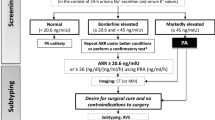
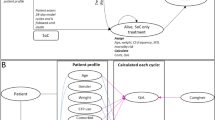
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information

Similar content being viewed by others
Data availability
For additional information and access to the data, please reach out to the study’s corresponding author.
Abbreviations
- IIH:
-
Idiopathic intracranial hypertension pressure
- MA:
-
Metabolic acidosis
- ICP:
-
Intracranial pressure
- CT:
-
Computerized tomography
- MRI:
-
Magnetic resonance imaging
- LP:
-
Lumbar puncture
- CSF:
-
Cerebrospinal fluid
- CA:
-
Carbonic anhydrase
- BMI:
-
Body mass index
References
Wall M, Kupersmith MJ, Kieburtz KD et al (2014) The idiopathic intracranial hypertension treatment trial: clinical profile at baseline. JAMA Neurol 71:693–701. https://doi.org/10.1001/jamaneurol.2014.133
Corbett JJ, Savino PJ, Thompson HS et al (1982) Visual loss in pseudotumor cerebri. Follow-up of 57 patients from five to 41 years and a profile of 14 patients with permanent severe visual loss. Arch Neurol 39:461–474. https://doi.org/10.1001/archneur.1982.00510200003001
Thambisetty M, Lavin PJ, Newman NJ et al (2007) Fulminant idiopathic intracranial hypertension. Neurology 68:229–232. https://doi.org/10.1212/01.wnl.0000251312.19452.ec
Hilely A, Hecht I, Goldenberg-Cohen N et al (2019) Long-Term Follow-up of Pseudotumor Cerebri Syndrome in Prepubertal Children, Adolescents, and Adults. Pediatr Neurol 101:57–63. https://doi.org/10.1016/j.pediatrneurol.2019.04.018
Hoffmann J, Huppertz HJ, Schmidt C et al (2013) Morphometric and volumetric MRI changes in idiopathic intracranial hypertension. Cephalalgia 33:1075–1084. https://doi.org/10.1177/0333102413484095
Maralani PJ, Hassanlou M, Torres C et al (2012) Accuracy of brain imaging in the diagnosis of idiopathic intracranial hypertension. Clin Radiol 67:656–663. https://doi.org/10.1016/j.crad.2011.12.002
Butros SR, Goncalves LF, Thompson D et al (2012) Imaging features of idiopathic intracranial hypertension, including a new finding: widening of the foramen ovale. Acta Radiol 53:682–688. https://doi.org/10.1258/ar.2012.110705
Friedman DI, Liu GT, Digre KB (2013) Revised diagnostic criteria for the pseudotumor cerebri syndrome in adults and children. Neurology 81:1159–1165. https://doi.org/10.1212/WNL.0b013e3182a55f17
Mercille G, Ospina LH (2007) Pediatric Idiopathic Intracranial Hypertension: A Review. Pediatr Rev 28:e77–e86. https://doi.org/10.1542/pir.28-11-e77
Markey KA, Mollan SP, Jensen RH et al (2016) Understanding idiopathic intracranial hypertension: Mechanisms, management, and future directions. Lancet Neurol 15:78–91. https://doi.org/10.1016/S1474-4422(15)00298-7
Standridge SM (2010) Idiopathic intracranial hypertension in children: A review and algorithm. Pediatr Neurol 43:377–390. https://doi.org/10.1016/j.pediatrneurol.2010.08.001
Ball AK, Clarke CE (2006) Idiopathic intracranial hypertension. Lancet Neurol 5:433–442. https://doi.org/10.1016/S1474-4422(06)70442-2
Wall M (1990) Sensory visual testing in idiopathic intracranial hypertension: measures sensitive to change. Neurology 40:1859–1864. https://doi.org/10.1212/WNL.40.12.1859
Mollan SP, Davies B, Silver NC et al (2018) Idiopathic intracranial hypertension: Consensus guidelines on management. J Neurol Neurosurg Psychiatry 89:1088–1100. https://doi.org/10.1136/jnnp-2017-317440
Thuente DD, Buckley EG (2005) Pediatric optic nerve sheath decompression. Ophthalmology 112:724–727. https://doi.org/10.1016/j.ophtha.2004.11.049
Aylward SC, Reem RE (2017) Pediatric Intracranial Hypertension. Pediatr Neurol 66:32–43. https://doi.org/10.1016/j.pediatrneurol.2016.08.010
Çelebisoy N, Gökçay F, Şirin H et al (2007) Treatment of idiopathic intracranial hypertension: Topiramate vs Acetazolamide, an open-label study. Acta Neurol Scand 116:322–327. https://doi.org/10.1111/j.1600-0404.2007.00905.x
McCarthy KD, Reed DJ (1974) The effect of Acetazolamide and furosemide on cerebrospinal fluid production and choroid plexus carbonic anhydrase activity. J Pharmacol Exp Ther 189:194–201
Smith SV, Friedman DI (2017) The Idiopathic Intracranial Hypertension Treatment Trial: A Review of the Outcomes. Headache 57:1303–1310. https://doi.org/10.1111/head.13144
Wall M, Kupersmith MJ, Thurtell MJ et al (2017) The Longitudinal Idiopathic Intracranial Hypertension Trial: Outcomes from Months 6–12. Am J Ophthalmol 176:102–107. https://doi.org/10.1016/j.ajo.2017.01.004
Van Berkel MA, Elefritz JL (2018) Evaluating off-label uses of acetazolamide. Am J Health Syst Pharm 75:524–531. https://doi.org/10.2146/ajhp170279
Wall M, McDermott MP, Kieburtz KD et al (2014) Effect of Acetazolamide on visual function in patients with idiopathic intracranial hypertension and mild visual loss: the idiopathic intracranial hypertension treatment trial. JAMA 311:1641–1651. https://doi.org/10.1001/jama.2014.3312
Van Patot MC, Leadbetter G, Keyes LE et al (2008) Prophylactic low-dose Acetazolamide reduces the incidence and severity of acute mountain sickness. High Alt Med Biol 9:289–293. https://doi.org/10.1089/ham.2008.1029
Karimy JK, Duran D, Hu JK et al (2016) Cerebrospinal fluid hypersecretion in pediatric hydrocephalus. Neurosurg Focus 41:E10. https://doi.org/10.3171/2016.8.FOCUS16278
Karimy JK, Zhang J, Kurland DB et al (2017) Inflammation-dependent cerebrospinal fluid hypersecretion by the choroid plexus epithelium in posthemorrhagic hydrocephalus. Nat Med 23:997–1003. https://doi.org/10.1038/nm.4361
Supuran CT (2018) Applications of carbonic anhydrases inhibitors in renal and central nervous system diseases. Expert Opin Ther Pat 28:713–721. https://doi.org/10.1080/13543776.2018.1519023
Supuran CT (2015) Acetazolamide for the treatment of idiopathic intracranial hypertension. Expert Rev Neurother 15:851–856. https://doi.org/10.1586/14737175.2015.1066675
Martínez-Monseny AF, Bolasell M, Callejón-Póo L et al (2019) AZATAX: Acetazolamide safety and efficacy in cerebellar syndrome in PMM2 congenital disorder of glycosylation (PMM2-CDG). Ann Neurol 85:740–751. https://doi.org/10.1002/ana.25457
Tovia E, Reif S, Oren A, Mitelpunkt A et al (2017) Treatment Response in Pediatric Patients with Pseudotumor Cerebri Syndrome. J Neuroophthalmol 37:393–397. https://doi.org/10.1097/wno.0000000000000516
Sharan S, Dupuis A, Hébert D et al (2010) The effect of oral Acetazolamide on weight gain in children. Can J Ophthalmol 45:41–45. https://doi.org/10.3129/i09-198
Markhorst JM, Stunnenberg BC, Ginjaar IB et al (2014) Clinical experience with long-term acetazolamide treatment in children with nondystrophic myotonias: a three-case report. Pediatr Neurol 51:537–541. https://doi.org/10.1016/j.pediatrneurol.2014.05.027
ten Hove MW, Friedman DI, Patel AD et al (2016) Safety and Tolerability of Acetazolamide in the Idiopathic Intracranial Hypertension Treatment Trial. J Neuroophthalmol 36:13–19. https://doi.org/10.1097/WNO.0000000000000322
Acknowledgements
The graphical abstract for this work was created using the 'Noun project' application.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Yarden Bulkowstein and Adi Nitzan-Luques contributed equally to this work.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bulkowstein, Y., Nitzan‑Luques, A., Schnapp, A. et al. The manifestations of metabolic acidosis during acetazolamide treatment in a cohort of pediatric idiopathic intracranial hypertension. Pediatr Nephrol 39, 185–191 (2024). https://doi.org/10.1007/s00467-023-06084-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06084-9