Abstract
Background
Extremes of unhealthy body weight, particularly obesity, are known to increase the risk of chronic kidney diseases. However, the current knowledge of kidney health outcomes associated with unhealthy body weight remains incomprehensive, especially in pediatrics. Therefore, the present study aimed to evaluate body mass index (BMI) and its potential associations with kidney health in a selected subset of school students in Sri Lanka.
Methods
This cross-sectional study was conducted among students of both sexes in the range of 11–18 years of age (N = 1078) in education zones with no reported cases of chronic kidney disease of uncertain etiology. Based on sex- and age-specific BMI percentiles (LMS method), the participants were classified into five BMI groups (severely thin, thin, healthy, overweight, and obese) for measurement of urinary biomarkers of kidney injury: kidney injury molecule (KIM-1), neutrophil gelatinase-associated lipocalin (NGAL), and albumin creatinine ratio (ACR).
Results
The median urinary levels of NGAL, ACR, and particularly KIM-1, which is a more sensitive indicator of kidney injury, showed no significant differences across the BMI strata. Importantly, moderate correlations of BMI with KIM-1 and NGAL were identified in severely thin girls.
Conclusions
According to the present study, these findings do not produce plausibly strong evidence to establish a potential association of BMI with altered kidney function in the studied pediatric communities. Particularly, a likelihood of abnormal kidney health outcomes associated with undernutrition is apparent in severely thin girls. However, in-depth studies are warranted to develop a comprehensive understanding of the associations of nutritional status with pediatric kidney health in Sri Lanka.
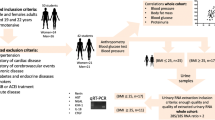
Graphical Abstract

A higher resolution version of the Graphical abstract is available as Supplementary information

Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are not publicly available due to restrictions under the approval of the ethics review board. However, they are available from the corresponding author upon reasonable request.
References
Lobstein T, Jackson-Leach R, Moodie ML, Hall KD, Gortmaker SL, Swinburn BA, James WPT, Wang Y, McPherson K (2015) Child and adolescent obesity: part of a bigger picture. Lancet 385:2510–2520. https://doi.org/10.1016/S0140-6736(14)61746-3
Estrada E, Eneli I, Hampl S, Mietus-Snyder M, Mirza N, Rhodes E, Sweeney B, Tinajero-Deck L, Woolford SJ, Pont SJ, Children’s Hospital Association (2014) Children’s Hospital Association consensus statements for comorbidities of childhood obesity. Child Obes 10:304–317. https://doi.org/10.1089/chi.2013.0120
Doyon A, Schaefer F (2013) The prodromal phase of obesity-related chronic kidney disease: early alterations in cardiovascular and renal function in obese children and adolescents. Nephrol Dial Transplant 28:50–57. https://doi.org/10.1093/ndt/gft263
Kaneko K, Kimata T, Tsuji S, Shiraishi K, Yamauchi K, Murakami M, Kitagawa T (2011) Impact of obesity on childhood kidney. Pediatr Rep 3:e27. https://doi.org/10.4081/pr.2011.e27
Gunta SS, Mak RH (2013) Is obesity a risk factor for chronic kidney disease in children? Pediatr Nephrol 28:1949–1956. https://doi.org/10.1007/s00467-012-2353-z
Bonventre JV, Vaidya VS, Schmouder R, Feig P, Dieterle F (2010) Next-generation biomarkers for detecting kidney toxicity. Nat Biotechnol 28:436–440. https://doi.org/10.1038/nbt0510-436
De Silva PMCS, Gunasekara TDKSC, Gunarathna SD, Sandamini PMMA, Pinipa RAI, Ekanayake EMDV, Thakshila WAKG, Jayasinghe SS, Chandana EPS, Jayasundara N (2021) Urinary biomarkers of renal injury KIM-1 and NGAL: reference intervals for healthy pediatric population in Sri Lanka. Children 8:684. https://doi.org/10.3390/children8080684
Polidori N, Giannini C, Salvatore R, Pelliccia P, Parisi A, Chiarelli F, Mohn A (2020) Role of urinary NGAL and KIM-1 as biomarkers of early kidney injury in obese prepubertal children. J Pediatr Endocrinol Metab JPEM 33:1183–1189. https://doi.org/10.1515/jpem-2020-0138
Khanna D, Peltzer C, Kahar P, Parmar MS (2022) Body mass index (BMI): a screening tool analysis. Cureus 14:e22119. https://doi.org/10.7759/cureus.22119
Rahman M, Berenson AB (2010) Accuracy of current body mass index obesity classification for white, black and Hispanic reproductive-age women. Obstet Gynecol 115:982–988. https://doi.org/10.1097/AOG.0b013e3181da9423
WHO Expert Consultation (2004) Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 363:157–163. https://doi.org/10.1016/S0140-6736(03)15268-3
de Onis M, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J (2007) Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ 85:660–667. https://doi.org/10.2471/blt.07.043497
WHO Multicentre Growth Reference Study Group (2006) WHO Child Growth Standards based on length/height, weight and age. Acta Paediatr 450:76–85. https://doi.org/10.1111/j.1651-2227.2006.tb02378.x
Kuczmarski RJ, Ogden CL, Guo SS, Grummer-Strawn LM, Flegal KM, Mei Z, Wei R, Curtin LR, Roche AF, Johnson CL (2002) 2000 CDC Growth Charts for the United States: methods and development. Vital Health Stat 11 1–190
Warnakulasuriya LS, Samaranayake DL, Adikaram AVN, Fernando MMA, Rytter E, Ciba I, Bergsten P, Forslund AH, Renuka Ruchira Silva KD, Wickramasinghe VP (2021) Metabolic abnormalities in a cohort of overweight and obese children in an urban setting of Sri Lanka. Int J Endocrinol 2021:9936889. https://doi.org/10.1155/2021/9936889
Shinsugi C, Gunasekara D, Gunawardena NK, Subasinghe W, Miyoshi M, Kaneko S, Takimoto H (2019) Double burden of maternal and child malnutrition and socioeconomic status in urban Sri Lanka. PloS One 14:e0224222. https://doi.org/10.1371/journal.pone.0224222
Ranasinghe AV, Kumara GWGP, Karunarathna RH, De Silva AP, Sachintani KGD, Gunawardena JMCN, Kumari SKCR, Sarjana MSF, Chandraguptha JS, De Silva MVC (2019) The incidence, prevalence and trends of chronic kidney disease and chronic kidney disease of uncertain aetiology (CKDu) in the north central province of Sri Lanka: an analysis of 30,566 patients. BMC Nephrol 20:338. https://doi.org/10.1186/s12882-019-1501-0
WHO Growth reference 5-19 years - BMI-for-age (5-19 years). https://www.who.int/tools/growth-reference-data-for-5to19-years/indicators/bmi-for-age. Accessed 25 Sep 2022
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH (2000) Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 320:1240–1243. https://doi.org/10.1136/bmj.320.7244.1240
Gul A, Yilmaz R, Ozmen ZC, Gumuser R, Demir O, Unsal V (2020) Assessment of renal function in obese and overweight children with NGAL and KIM-1 biomarkers. Nutr Hosp 34:436–442. https://doi.org/10.20960/nh.02651
Ozturk A, Mazicioglu MM, Hatipoglu N, Budak N, Keskin G, Yazlak Z, Balci N, Yildiz H, Yildiz K, Ustunbas HB, Kurtoglu S (2008) Reference body mass index curves for Turkish children 6 to 18 years of age. J Pediatr Endocrinol Metab 21:827–836. https://doi.org/10.1515/jpem.2008.21.9.827
Hernandez E, Kim M, Kim WG, Yoon J (2016) Nutritional aspects of night eating and its association with weight status among Korean adolescents. Nutr Res Pract 10:448–455. https://doi.org/10.4162/nrp.2016.10.4.448
Zhu P, Herrington WG, Haynes R, Emberson J, Landray MJ, Sudlow CLM, Woodward M, Baigent C, Lewington S, Staplin N (2021) Conventional and genetic evidence on the association between adiposity and CKD. J Am Soc Nephrol 32:127–137. https://doi.org/10.1681/ASN.2020050679
Jiang Z, Wang Y, Zhao X, Cui H, Han M, Ren X, Gang X, Wang G (2023) Obesity and chronic kidney disease. Am J Physiol Endocrinol Metab 324:E24–E41. https://doi.org/10.1152/ajpendo.00179.2022
Wang Y, Chen X, Song Y, Caballero B, Cheskin LJ (2008) Association between obesity and kidney disease: a systematic review and meta-analysis. Kidney Int 73:19–33. https://doi.org/10.1038/sj.ki.5002586
Kim YH, Kang JG, Lee SJ, Han K, Ihm S-H, Cho K-H, Park Y-G (2020) Underweight increases the risk of end-stage renal diseases for type 2 diabetes in Korean population: data from the National Health Insurance Service health checkups 2009–2017. Diabetes Care 43:1118–1125. https://doi.org/10.2337/dc19-2095
Naderi N, Kleine C-E, Park C, Hsiung J-T, Soohoo M, Tantisattamo E, Streja E, Kalantar-Zadeh K, Moradi H (2018) Obesity paradox in advanced kidney disease: from bedside to the bench. Prog Cardiovasc Dis 61:168–181. https://doi.org/10.1016/j.pcad.2018.07.001
Goknar N, Oktem F, Ozgen IT, Torun E, Kuçukkoc M, Demir AD, Cesur Y (2015) Determination of early urinary renal injury markers in obese children. Pediatr Nephrol 30:139–144. https://doi.org/10.1007/s00467-014-2829-0
Bostan Gayret Ö, Taşdemir M, Erol M, Tekin Nacaroğlu H, Zengi O, Yiğit Ö (2018) Are there any new reliable markers to detect renal injury in obese children? Ren Fail 40:416–422. https://doi.org/10.1080/0886022X.2018.1489284
Ece A, Gözü A, Bükte Y, Tutanç M, Kocamaz H (2007) The effect of malnutrition on kidney size in children. Pediatr Nephrol 22:857–863. https://doi.org/10.1007/s00467-006-0338-5
Anjum M, Moorani KN, Sameen I, Mustufa MA, Kulsoom S (2016) Functional and structural abnormalities of the kidney and urinary tract in severely malnourished children - a hospital based study. Pak J Med Sci 32:1135–1140. https://doi.org/10.12669/pjms.325.10457
Wickramasinghe VP, Lamabadusuriya SP, Atapattu N, Sathyadas G, Kuruparanantha S, Karunarathne P (2004) Nutritional status of schoolchildren in an urban area of Sri Lanka. Ceylon Med J 49:114–118. https://doi.org/10.4038/cmj.v49i4.1920
Acknowledgements
The authors would like to thank all the students who participated in the study, academic and non-academic staff members of the schools, government authorities, and parents for their valuable support.
Funding
This work was supported by the Accelerating Higher Education Expansion and Development (AHEAD) Operation of the Ministry of Higher Education funded by the World Bank (grant number: AHEAD DOR 02/40) and the Duke Global Health Pilot Grant.
Author information
Authors and Affiliations
Contributions
Conceptualization: PMCSDS, NJ. Data curation: PMCSDS, TDKSCG. Formal analysis: PMCSDS, TDKSCG. Funding acquisition: PMCSDS, NJ. Investigation: PMCSDS, NJ, TDKSCG. Methodology: PMCSDS, NJ, TDKSCG. Project administration: PMCSDS, NJ. Resources: PMCSDS, NJ, SS, EPSC, CH, SSJ. Software: TDKSCG, PMCSDS. Supervision: PMCSDS, EPSC, NJ, SS, CH, SSJ. Validation: PMCSDS, NJ, SS, CH, SSJ, EPSC. Visualization: TDKSCG, PMCSDS. Writing—original draft: TDKSCG. Writing—review and editing: PMCSDS, NJ, SS, CH, SSJ, and EPSC.
Corresponding author
Ethics declarations
Ethical approval
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Ethics Review Committee of the Faculty of Medicine, University of Ruhuna, Sri Lanka (reference no: 2020.P.124; Date: 29.01.2021).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gunasekara, T.D.K.S.C., De Silva, P.M.C.S., Chandana, E.P.S. et al. Body mass index and implications for pediatric kidney health: a cross-sectional study with urinary biomarkers. Pediatr Nephrol 39, 167–175 (2024). https://doi.org/10.1007/s00467-023-06071-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06071-0