Abstract
Background
Preterm birth alters nephrogenesis and reduces the total nephron number. Intrauterine growth restriction (IUGR) seems to worsen nephron loss, but only a few studies have investigated its role in neonatal kidney impairment. We investigated whether IUGR, defined as reduced estimated fetal growth and/or placental flow alterations and low birth weight z-score, increases the risk of developing acute kidney injury (AKI) in very preterm infants.
Methods
We performed a retrospective study including infants born with a birth weight (BW) ≤ 1500 g and/or gestational age (GA) ≤ 32 weeks admitted to our center between January 2016 and December 2021. Neonatal AKI was defined according to the neonatal KDIGO classification based on the decline of urine output and/or creatinine elevation. We used multivariable linear regressions to verify the association between AKI and GA, BW z-score, IUGR definition, and hemodynamically significant patent ductus arteriosus (PDA).
Results
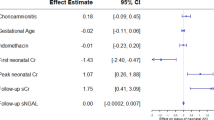
We included 282 infants in the analysis, with a median (IQR) GA = 29.4 (27.4, 31.3) weeks, BW = 1150 (870, 1360) g, and BW z-score = − 0.57 (− 1.64, 0.25). AKI was diagnosed in 36 (13%) patients, and 58 (21%) had PDA. AKI was significantly associated with BW z-score (beta (std. error) = − 0.08 (0.03), p = 0.008) and severe IUGR (beta (std. error) = 0.21 (0.08), p = 0.009), after adjusting for GA and PDA.
Conclusions
Our data suggest that low BW z-score and IUGR could represent adjunctive risk factors for kidney impairment in preterm babies.
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information


Similar content being viewed by others
References
Rodríguez MM, Gómez AH, Abitbol CL et al (2004) Histomorphometric analysis of postnatal glomerulogenesis in extremely preterm infants. Pediatr Dev Pathol 7:17–25
Carmody JB, Swanson JR, Rhone ET, Charlton JR (2014) Recognition and reporting of AKI in very low birth weight infants. Clin J Am Soc Nephrol 9:2036–2043
Jetton JG, Boohaker LJ, Sethi SK et al (2017) Incidence and outcomes of neonatal acute kidney injury (AWAKEN): a multicentre, multinational, observational cohort study. Lancet Child Adolesc Heal 1:184–194
Nada A, Bonachea EM, Askenazi DJ (2017) Acute kidney injury in the fetus and neonate. Semin Fetal Neonatal Med 22:90
Lee CC, Chan OW, Lai MY et al (2017) Incidence and outcomes of acute kidney injury in extremely-low-birth-weight infants. PLoS One 12:e0187764
Mammen C, Al Abbas A, Skippen P et al (2012) Long-term risk of CKD in children surviving episodes of acute kidney injury in the intensive care unit: a prospective cohort study. Am J Kidney Dis 59:523–530
Askenazi DJ, Griffin R, McGwin G et al (2009) Acute kidney injury is independently associated with mortality in very low birthweight infants: a matched case-control analysis. Pediatr Nephrol 24:991–997
Cataldi L, Leone R, Moretti U et al (2005) Potential risk factors for the development of acute renal failure in preterm newborn infants: a case-control study. Arch Dis Child Fetal Neonatal Ed 90:F514–F519
Coleman C, Tambay Perez A, Selewski DT, Steflik HJ (2022) Neonatal acute kidney injury. Front Pediatr 10:389
Shimada S, Kasai T, Hoshi A et al (2003) Cardiocirculatory effects of patent ductus arteriosus in extremely low-birth-weight infants with respiratory distress syndrome. Pediatr Int 45:255–262
Keijzer-Veen MG, Schrevel M, Finken MJJ et al (2005) Microalbuminuria and lower glomerular filtration rate at young adult age in subjects born very premature and after intrauterine growth retardation. J Am Soc Nephrol 16:2762–2768
Gordijn SJ, Beune IM, Thilaganathan B et al (2016) Consensus definition of fetal growth restriction: a Delphi procedure. Ultrasound Obstet Gynecol 48:333–339
Jensen EA, Dysart K, Gantz MG et al (2019) The diagnosis of bronchopulmonary dysplasia in very preterm infants an evidence-based approach. Am J Respir Crit Care Med 200:751–759
Selewski DT, Charlton JR, Jetton JG et al (2015) Neonatal acute kidney injury. Pediatrics 136:e463–e473
Villar J, Ismail LC, Victora CG et al (2014) International standards for newborn weight, length, and head circumference by gestational age and sex: the Newborn Cross-Sectional Study of the INTERGROWTH-21st Project. Lancet 384:857–868
Fenton TR, Kim JH (2013) A systematic review and meta-analysis to revise the Fenton growth chart for preterm infants. BMC Pediatr 13:59
Stoops C, Stone S, Evans E et al (2019) Baby NINJA (Nephrotoxic Injury Negated by Just-in-Time Action): reduction in nephrotoxic medication-associated acute kidney injury in the neonatal intensive care unit. J Pediatr 215:223
Nyengaard JR, Bendtsen TF (1992) Glomerular number and size in relation to age, kidney weight, and body surface in normal man. Anat Rec 232:194–201
Sutherland MR, Gubhaju L, Black MJ (2011) Stereological assessment of renal development in a baboon model of preterm birth. Am J Nephrol 33(Suppl 1):25–33
Popescu CR, Sutherland MR, Cloutier A et al (2013) Hyperoxia exposure impairs nephrogenesis in the neonatal rat: role of HIF-1α. PLoS OneE 8:e82421
Baldelomar EJ, Charlton JR, Beeman SC, Bennett KM (2018) Measuring rat kidney glomerular number and size in vivo with MRI. Am J Physiol Renal Physiol 314:F399–F406
Merlet-Bénichou C, Gilbert T, Muffat-Joly M et al (1994) Intrauterine growth retardation leads to a permanent nephron deficit in the rat. Pediatr Nephrol 8:175–180
Hinchliffe SA, Lynch MRJ, Sargent PH et al (1992) The effect of intrauterine growth retardation on the development of renal nephrons. Br J Obstet Gynaecol 99:296–301
Keijzer-Veen MG, Finken MJJ, Nauta J et al (2005) Is blood pressure increased 19 years after intrauterine growth restriction and preterm birth? A prospective follow-up study in The Netherlands. Pediatrics 116:725–731
Park B, Lee JW, Kim HS et al (2019) Effects of prenatal growth status on subsequent childhood renal function related to high blood pressure. J Korean Med Sci 34:e174
Konje JC, Okaro CI, Bell SC et al (1997) A cross-sectional study of changes in fetal renal size with gestation in appropriate- and small-for-gestational-age fetuses. Ultrasound Obstet Gynecol 10:22–26
Akkoc G, Duzova A, Korkmaz A et al (2022) Long-term follow-up of patients after acute kidney injury in the neonatal period: abnormal ambulatory blood pressure findings. BMC Nephrol 23:116
Hershkovitz D, Burbea Z, Skorecki K, Brenner BM (2007) Fetal programming of adult kidney disease: cellular and molecular mechanisms. Clin J Am Soc Nephrol 2:334–342
Al Salmi I, Hannawi S (2021) Birthweight predicts glomerular filtration rate in adult-life: population based cross sectional study. Ren Fail 43:664–675
Yudkin JS, Martyn CN, Phillips DIW, Gale CR (2001) Associations of micro-albuminuria with intra-uterine growth retardation. Nephron 89:309–314
Painter RC, Roseboom TJ, Van Montfrans GA et al (2005) Microalbuminuria in adults after prenatal exposure to the Dutch famine. J Am Soc Nephrol 16:189–194
Battista MC, Oligny LL, St-Louis J, Brochu M (2002) Intrauterine growth restriction in rats is associated with hypertension and renal dysfunction in adulthood. Am J Physiol Endocrinol Metab 283:E124–E131
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sinelli, M., Zannin, E., Doni, D. et al. Association of intrauterine growth restriction and low birth weight with acute kidney injury in preterm neonates. Pediatr Nephrol 38, 3139–3144 (2023). https://doi.org/10.1007/s00467-023-05936-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-05936-8