Abstract
Background
This cross-sectional study investigates the association of fibroblast growth-factor 23 (FGF23) and other bone mineral parameters with iron status and anemia in pediatric chronic kidney disease (CKD).
Methods
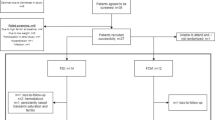
Serum calcium, phosphorus, 25-hydroxyvitamin D (25(OH)D), intact parathormone, c-terminal FGF23, a-Klotho, iron (Fe), ferritin, unsaturated iron-binding capacity, and hemoglobin (Hb) were measured in 53 patients from 5 to 19 years old with GFR < 60 mL/min/1.73 m2. Transferrin saturation (TSAT) was calculated.
Results
Absolute (ferritin ≤ 100 ng/mL, TSAT ≤ 20%) and functional iron deficiency (ferritin > 100 ng/mL, TSAT ≤ 20%) were observed in 32% and 7.5% of patients, respectively. In CKD stages 3–4 (36 patients), lnFGF23 and 25(OH)D were correlated with Fe (rs = − 0.418, p = 0.012 and rs = 0.467, p = 0.005) and TSAT (rs = − 0.357, p = 0.035 and rs = 0.487, p = 0.003) but not to ferritin. In this patient group, lnFGF23 and 25(OH)D were correlated with Hb z-score (rs = − 0.649, p < 0.001 and rs = 0.358, p = 0.035). No correlation was detected between lnKlotho and iron parameters. In CKD stages 3–4, in multivariate backward logistic regression analysis, including bone mineral parameters, CKD stage, patient age, and daily alphacalcidol dose as covariates, lnFGF23 and 25(OH)D were associated with low TSΑΤ (15 patients) (OR 6.348, 95% CI 1.106–36.419, and OR 0.619, 95% CI 0.429–0.894, respectively); lnFGF23 was associated with low Hb (10 patients) (OR 5.747, 95% CI 1.270–26.005); while the association between 25(OH)D and low Hb did not reach statistical significance (OR 0.818, 95% CI 0.637–1.050).
Conclusions
In pediatric CKD stages 3–4, iron deficiency and anemia are associated with increased FGF23, independently of Klotho. Vitamin D deficiency might contribute to iron deficiency in this population.
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information

Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Atkinson MA, Martz K, Warady BA, Neu AM (2010) Risk for anemia in pediatric chronic kidney disease patients: a report of NAPRTCS. Pediatr Nephrol 25:1699–1706
Babitt JL, Lin HY (2012) Mechanisms of anemia in CKD. J Am Soc Nephrol 23:1631–1634
Patino E, Akchurin O (2022) Erythropoiesis-independent effects of iron in chronic kidney disease. Pediatr Nephrol 37:777–788
Atkinson MA, Furth SL (2011) Anemia in children with chronic kidney disease. Nat Rev Nephrol 7:635–641
Karava V, Christoforidis A, Kondou A, Dotis J, Printza N (2021) Update on the crosstalk between adipose tissue and mineral balance in general population and chronic kidney disease. Front Pediatr 9:696942
Leifheit-Nestler M, Haffner D (2021) How FGF23 shapes multiple organs in chronic kidney disease. Mol Cell Pediatr 8:12
Babitt JL, Sitara D (2019) Crosstalk between FGF23, iron, erythropoietin, and inflammation in kidney disease. Curr Opin Nephrol Hypertens 28:304–310
Zhang R, Wang SY, Yang F, Ma S, Lu X, Kan C, Zhang JB (2021) Crosstalk of fibroblast growth factor 23 and anemia-related factors during the development and progression of CKD (Review). Exp Ther Med 22:1159
Wheeler JA, Clinkenbeard EL (2019) Regulation of fibroblast growth factor 23 by iron, EPO, and HIF. Curr Mol Biol Rep 5:8–17
David V, Martin A, Isakova T, Spaulding C, Qi L, Ramirez V, Zumbrennen-Bullough KB, Sun CC, Lin HY, Babitt JL, Wolf M (2016) Inflammation and functional iron deficiency regulate fibroblast growth factor 23 production. Kidney Int 89:135–146
Coe LM, Madathil SV, Casu C, Lanske B, Rivella S, Sitara D (2014) FGF-23 is a negative regulator of prenatal and postnatal erythropoiesis. J Biol Chem 289:9795–9810
Agoro R, Montagna A, Goetz R, Aligbe O, Singh G, Coe LM, Mohammadi M, Rivella S, Sitara D (2018) Inhibition of fibroblast growth factor 23 (FGF23) signaling rescues renal anemia. FASEB J 32:3752–3764
Mehta RC, Cho ME, Cai X, Lee J, Chen J, He J, Flack J, Shafi T, Saraf SL, David V, Feldman HI, Isakova T, Wolf M, CRIC Study Investigators (2021) Iron status, fibroblast growth factor 23 and cardiovascular and kidney outcomes in chronic kidney disease. Kidney Int 100:1292–1302
Nam KH, Kim H, An SY, Lee M, Cha MU, Park JT, Yoo TH, Lee KB, Kim YH, Sung SA, Lee J, Kang SW, Choi KH, Ahn C, Han SH (2018) Circulating fibroblast growth factor-23 levels are associated with an increased risk of anemia development in patients with nondialysis chronic kidney disease. Sci Rep 8:7294
Abu-Zaid A, Magzoub D, Aldehami MA, Behiry AA, Bhagavathula AS, Hajji R (2021) The effect of iron supplementation on FGF23 in chronic kidney disease patients: a systematic review and time-response meta-analysis. Biol Trace Elem Res 199:4516–4524
Tsai MH, Leu JG, Fang YW, Liou HH (2016) High fibroblast growth factor 23 levels associated with low hemoglobin levels in patients with chronic kidney disease stages 3 and 4. Medicine (Baltimore) 95:e3049
Mehta R, Cai X, Hodakowski A, Lee J, Leonard M, Ricardo A, Chen J, Hamm L, Sondheimer J, Dobre M, David V, Yang W, Go A, Kusek JW, Feldman H, Wolf M, Isakova T, CRIC Study Investigators (2017) Fibroblast growth factor 23 and anemia in the chronic renal insufficiency cohort study. Clin J Am Soc Nephrol 12:1795–1803
Bielesz B, Reiter T, Hammerle FP, Winnicki W, Bojic M, Gleiss A, Kieweg H, Ratzinger F, Sunder-Plassmann G, Marculescu R (2020) The role of iron and erythropoietin in the association of fibroblast growth factor 23 with anemia in chronic kidney disease in humans. J Clin Med 9:2640
Limm-Chan B, Wesseling-Perry K, Pearl MH, Jung G, Tsai-Chambers E, Weng PL, Hanudel MR (2021) Associations among erythropoietic, iron-related, and FGF23 parameters in pediatric kidney transplant recipients. Pediatr Nephrol 36:3241–3249
Schwartz GJ, Muñoz A, Schneider MF, Mak RH, Kaskel F, Warady BA, Furth SL (2009) New equations to estimate GFR in children with CKD. J Am Soc Nephrol 20:629–637
Eleftheriadis T, Liakopoulos V, Antoniadi G, Stefanidis I (2010) Which is the best way for estimating transferrin saturation? Ren Fail 32:1022–1023
Drüeke TB, Parfrey PS (2012) Summary of the KDIGO guideline on anemia and comment: reading between the (guide)line(s). Kidney Int 82:952–960
Janus J, Moerschel SK (2010) Evaluation of anemia in children. Am Fam Physician 81:1462–1471
Goyal KK, Saha A, Sahi PK, Kaur M, Dubey NK, Goyal P, Upadhayay AD (2018) Hepcidin and proinflammatory markers in children with chronic kidney disease: a case-control study. Clin Nephrol 89:363–370
Yamamura-Miyazaki N, Michigami T, Ozono K, Yamamoto K, Hasuike Y (2022) Factors associated with 1-year changes in serum fibroblast growth factor 23 levels in pediatric patients with chronic kidney disease. Clin Exp Nephrol 26:1014–1021
Zhao SJ, Wang ZX, Chen L, Wang FX, Kong LD (2022) Effect of different phosphate binders on fibroblast growth factor 23 levels in patients with chronic kidney disease: a systematic review and meta-analysis of randomized controlled trials. Ann Palliat Med 11:1264–1277
Vadakke Madathil S, Coe LM, Casu C, Sitara D (2014) Klotho deficiency disrupts hematopoietic stem cell development and erythropoiesis. Am J Pathol 184:827–841
Park MY, Le Henaff C, Sitara D (2022) Administration of α-Klotho does not rescue renal anemia in mice. Front Pediatr 10:924915
Aucella F, Scalzulli RP, Gatta G, Vigilante M, Carella AM, Stallone C (2003) Calcitriol increases burst-forming unit-erythroid proliferation in chronic renal failure. A synergistic effect with r-HuEpo. Nephron Clin Pract 95:c121–c127
Bacchetta J, Zaritsky JJ, Sea JL, Chun RF, Lisse TS, Zavala K, Nayak A, Wesseling-Perry K, Westerman M, Hollis BW, Salusky IB, Hewison M (2014) Suppression of iron-regulatory hepcidin by vitamin D. J Am Soc Nephrol 25:564–572
Altemose KE, Kumar J, Portale AA, Warady BA, Furth SL, Fadrowski JJ, Atkinson MA (2018) Vitamin D insufficiency, hemoglobin, and anemia in children with chronic kidney disease. Pediatr Nephrol 33:2131–2136
Patel NM, Gutiérrez OM, Andress DL, Coyne DW, Levin A, Wolf M (2010) Vitamin D deficiency and anemia in early chronic kidney disease. Kidney Int 77:715–720
Arabi SM, Ranjbar G, Bahrami LS, Vafa M, Norouzy A (2020) The effect of vitamin D supplementation on hemoglobin concentration: a systematic review and meta-analysis. Nutr J 19:11
Andıran N, Çelik N, Akça H, Doğan G (2012) Vitamin D deficiency in children and adolescents. J Clin Res Pediatr Endocrinol 4:25–29
Dusso AS, Puche RC (1985) The effect of 1 alpha, 25-dihydroxycholecalciferol on iron metabolism. Blut 51:103–108
Akalin N, Okuturlar Y, Harmankaya O, Gedıkbaşi A, Sezıklı S, Koçak Yücel S (2014) Prognostic importance of fibroblast growth factor-23 in dialysis patients. Int J Nephrol 2014:602034
Eser B, Yayar O, Buyukbakkal M, Erdogan B, Ercan Z, Merhametsiz O, Haspulat A, Oğuz EG, Dogan İ, Canbakan B, Ayli MD (2015) Fibroblast growth factor is associated to left ventricular mass index, anemia and low values of transferrin saturation. Nefrologia 35:465–472
Thomas DW, Hinchliffe RF, Briggs C, Macdougall IC, Littlewood T, Cavill I (2013) Guideline for the laboratory diagnosis of functional iron deficiency. Br J Haematol 161:639–648
Tessitore N, Solero GP, Lippi G, Bassi A, Faccini GB, Bedogna V, Gammaro L, Brocco G, Restivo G, Bernich P, Lupo A, Maschio G (2001) The role of iron status markers in predicting response to intravenous iron in haemodialysis patients on maintenance erythropoietin. Nephrol Dial Transplant 16:1416–1423
Chiang WC, Tsai TJ, Chen YM, Lin SL, Hsieh BS (2002) Serum soluble transferrin receptor reflects erythropoiesis but not iron availability in erythropoietin-treated chronic hemodialysis patients. Clin Nephrol 58:363–369
Hanudel MR, Eisenga MF, Rappaport M, Chua K, Qiao B, Jung G, Gabayan V, Gales B, Ramos G, de Jong MA, van Zanden JJ, de Borst MH, Bakker SJL, Nemeth E, Salusky IB, Gaillard CAJM, Ganz T (2019) Effects of erythropoietin on fibroblast growth factor 23 in mice and humans. Nephrol Dial Transplant 34:2057–2065
Clinkenbeard EL, Hanudel MR, Stayrook KR, Appaiah HN, Farrow EG, Cass TA, Summers LJ, Ip CS, Hum JM, Thomas JC, Ivan M, Richine BM, Chan RJ, Clemens TL, Schipani E, Sabbagh Y, Xu L, Srour EF, Alvarez MB, Kacena MA, Salusky IB, Ganz T, Nemeth E, White KE (2017) Erythropoietin stimulates murine and human fibroblast growth factor-23, revealing novel roles for bone and bone marrow. Haematologica 102:e427–e430
Honda H, Michihata T, Shishido K, Takahashi K, Takahashi G, Hosaka N, Ikeda M, Sanada D, Shibata T (2017) High fibroblast growth factor 23 levels are associated with decreased ferritin levels and increased intravenous iron doses in hemodialysis patients. PLoS One 12:e0176984
Dignass A, Farrag K, Stein J (2018) Limitations of serum ferritin in diagnosing iron deficiency in inflammatory conditions. Int J Chronic Dis 2018:9394060
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Karava, V., Dotis, J., Kondou, A. et al. Fibroblast growth-factor 23 and vitamin D are associated with iron deficiency and anemia in children with chronic kidney disease. Pediatr Nephrol 38, 2771–2779 (2023). https://doi.org/10.1007/s00467-023-05903-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-05903-3