Abstract
Background
Acute kidney injury (AKI) and fluid overload (FO) are associated with poor outcomes in children receiving extracorporeal membrane oxygenation (ECMO). Our objective is to evaluate the impact of AKI and FO on pediatric patients receiving ECMO for cardiac pathology.
Methods
We performed a secondary analysis of the six-center Kidney Interventions During Extracorporeal Membrane Oxygenation (KIDMO) database, including only children who underwent ECMO for cardiac pathology. AKI was defined using Kidney Disease: Improving Global Outcomes (KDIGO) creatinine criteria. FO was defined as < 10% (FO–) vs. ≥ 10% (FO +) and was evaluated at ECMO initiation, peak during ECMO, and ECMO discontinuation. Primary outcomes were mortality and length of stay (LOS).
Results
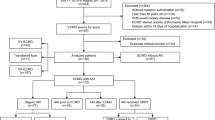
Data from 191 patients were included. Non-survivors (56%) were more likely to be FO + than survivors at peak ECMO fluid status and ECMO discontinuation. There was a significant interaction between AKI and FO. In the presence of AKI, the adjusted odds of mortality for FO + was 4.79 times greater than FO– (95% CI: 1.52–15.12, p = 0.01). In the presence of FO + , the adjusted odds of mortality for AKI + was 2.7 times higher than AKI– [95%CI: 1.10–6.60; p = 0.03]. Peak FO + was associated with a 55% adjusted relative increase in LOS [95%CI: 1.07–2.26, p = 0.02].
Conclusions
The association of peak FO + with mortality is present only in the presence of AKI + . Similarly, AKI + is associated with mortality only in the presence of peak FO + . FO + was associated with LOS. Studies targeting fluid management have the potential to improve LOS and mortality outcomes.
Graphical abstract
A higher resolution version of the Graphical abstract is available as Supplementary information.


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available due to regulatory requirements from the participating site institutional review boards but are available from the corresponding author on reasonable request.
Abbreviations
- AKI:
-
Acute Kidney Injury by Kidney Disease: Improving Global Outcomes or Neonatal Modification Serum Creatinine Criteria
- AKIKST :
-
Acute Kidney Injury by Kidney Disease: Improving Global Outcomes or Neonatal Modification Serum Creatinine Criteria or by utilization of kidney support therapy
- aOR:
-
Adjusted odds ratio
- AVV:
-
Atrioventricular valve
- CI:
-
Confidence interval
- CPB:
-
Cardiopulmonary bypass
- ECMO:
-
Extracorporeal membrane oxygenation
- EHR:
-
Electronic health record
- ELSO:
-
Extracorporeal Life Support Organization
- FO:
-
Fluid overload
- IQR:
-
Interquartile range
- KDIGO:
-
Kidney Disease: Improving Global Outcomes
- KIDMO:
-
Kidney Interventions During Extracorporeal Membrane Oxygenation
- KST:
-
Kidney support therapy
- LOS:
-
Length of stay
- MV:
-
Mechanical ventilation
- OR:
-
Unadjusted odds ratio
- SCr:
-
Serum creatinine
- Severe AKI:
-
Kidney Disease: Improving Global Outcomes stage 2 or 3 acute kidney injury
- VA ECMO:
-
Venoarterial extracorporeal membrane oxygenation
References
Joffe AR, Lequier L, Robertson CM (2012) Pediatric outcomes after extracorporeal membrane oxygenation for cardiac disease and for cardiac arrest: a review. ASAIO J 58:297–310. https://doi.org/10.1097/MAT.0b013e31825a21ff
Barbaro RP, Paden ML, Guner YS, Raman L, Ryerson LM, Alexander P, Nasr VG, Bembea MM, Rycus PT, Thiagarajan RR (2017) Pediatric extracorporeal life support organization registry international report 2016. ASAIO J 63:456–463. https://doi.org/10.1097/MAT.0000000000000603
Gist KM, Selewski DT, Brinton J, Menon S, Goldstein SL, Basu RK (2020) Assessment of the independent and synergistic effects of fluid overload and acute kidney injury on outcomes of critically Ill children. Pediatr Crit Care Med 21:170–177. https://doi.org/10.1097/PCC.0000000000002107
Li S, Krawczeski CD, Zappitelli M, Devarajan P, Thiessen-Philbrook H, Coca SG, Kim RW, Parikh CR (2011) Incidence, risk factors, and outcomes of acute kidney injury after pediatric cardiac surgery: a prospective multicenter study. Crit Care Med 39:1493–1499. https://doi.org/10.1097/CCM.0b013e31821201d3
Blinder JJ, Goldstein SL, Lee VV, Baycroft A, Fraser CD, Nelson D, Jefferies JL (2012) Congenital heart surgery in infants: effects of acute kidney injury on outcomes. J Thorac Cardiovasc Surg 143:368–374. https://doi.org/10.1016/j.jtcvs.2011.06.021
Jetton JG, Boohaker LJ, Sethi SK, Wazir S, Rohatgi S, Soranno DE, Chishti AS, Woroniecki R, Mammen C, Swanson JR, Sridhar S, Wong CS, Kupferman JC, Griffin RL, Askenazi DJ (2017) Incidence and outcomes of neonatal acute kidney injury (AWAKEN): a multicentre, multinational, observational cohort study. Lancet Child Adolesc Health 1:184–194. https://doi.org/10.1016/S2352-4642(17)30069-X
Mah KE, Hao S, Sutherland SM, Kwiatkowski DM, Axelrod DM, Almond CS, Krawczeski CD, Shin AY (2018) Fluid overload independent of acute kidney injury predicts poor outcomes in neonates following congenital heart surgery. Pediatr Nephrol 33:511–520. https://doi.org/10.1007/s00467-017-3818-x
Arikan AA, Zappitelli M, Goldstein SL, Naipaul A, Jefferson LS, Loftis LL (2012) Fluid overload is associated with impaired oxygenation and morbidity in critically ill children. Pediatr Crit Care Med 13:253–258. https://doi.org/10.1097/PCC.0b013e31822882a3
Selewski DT, Askenazi DJ, Bridges BC, Cooper DS, Fleming GM, Paden ML, Verway M, Sahay R, King E, Zappitelli M (2017) The impact of fluid overload on outcomes in children treated with extracorporeal membrane oxygenation: a multicenter retrospective cohort study. Pediatr Crit Care Med 18:1126–1135. https://doi.org/10.1097/PCC.0000000000001349
Gorga SM, Sahay RD, Askenazi DJ, Bridges BC, Cooper DS, Paden ML, Zappitelli M, Gist KM, Gien J, Basu RK, Jetton JG, Murphy HJ, King E, Fleming GM, Selewski DT (2020) Fluid overload and fluid removal in pediatric patients on extracorporeal membrane oxygenation requiring continuous renal replacement therapy: a multicenter retrospective cohort study. Pediatr Nephrol 35:871–882. https://doi.org/10.1007/s00467-019-04468-4
Mallory PP, Selewski DT, Askenazi DJ, Cooper DS, Fleming GM, Paden ML, Murphy L, Sahay R, King E, Zappitelli M, Bridges BC (2020) Acute kidney injury, fluid overload, and outcomes in children supported with extracorporeal membrane oxygenation for a respiratory indication. ASAIO J 66:319–326. https://doi.org/10.1097/MAT.0000000000001000
Boehne M, Sasse M, Karch A, Dziuba F, Horke A, Kaussen T, Mikolajczyk R, Beerbaum P, Jack T (2017) Systemic inflammatory response syndrome after pediatric congenital heart surgery: incidence, risk factors, and clinical outcome. J Card Surg 32:116–125. https://doi.org/10.1111/jocs.12879
Warren OJ, Smith AJ, Alexiou C, Rogers PL, Jawad N, Vincent C, Darzi AW, Athanasiou T (2009) The inflammatory response to cardiopulmonary bypass: part 1–mechanisms of pathogenesis. J Cardiothorac Vasc Anesth 23:223–231. https://doi.org/10.1053/j.jvca.2008.08.007
Fleming GM, Sahay R, Zappitelli M, King E, Askenazi DJ, Bridges BC, Paden ML, Selewski DT, Cooper DS (2016) The incidence of acute kidney injury and its effect on neonatal and pediatric extracorporeal membrane oxygenation outcomes: a multicenter report from the kidney intervention during extracorporeal membrane oxygenation study group. Pediatr Crit Care Med 17:1157–1169. https://doi.org/10.1097/PCC.0000000000000970
Murphy HJ, Gien J, Sahay R, King E, Selewski DT, Bridges BC, Cooper DS, Fleming GM, Paden ML, Zappitelli M, Gist KM, Basu RK, Jetton JG, Askenazi D (2021) Acute Kidney injury, fluid overload, and renal replacement therapy differ by underlying diagnosis in neonatal extracorporeal support and impact mortality disparately. Blood Purif 50:808–817. https://doi.org/10.1159/000512538
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP (2014) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Int J Surg 12:1495–1499. https://doi.org/10.1016/j.ijsu.2014.07.013
Kellum JA, Lameire N (2013) Diagnosis, evaluation, and management of acute kidney injury: a KDIGO summary (Part 1). Crit Care 17:204. https://doi.org/10.1186/cc11454
Selewski DT, Charlton JR, Jetton JG, Guillet R, Mhanna MJ, Askenazi DJ, Kent AL (2015) Neonatal acute kidney injury. Pediatrics 136:e463-473. https://doi.org/10.1542/peds.2014-3819
Sutherland SM, Zappitelli M, Alexander SR, Chua AN, Brophy PD, Bunchman TE, Hackbarth R, Somers MJ, Baum M, Symons JM, Flores FX, Benfield M, Askenazi D, Chand D, Fortenberry JD, Mahan JD, McBryde K, Blowey D, Goldstein SL (2010) Fluid overload and mortality in children receiving continuous renal replacement therapy: the prospective pediatric continuous renal replacement therapy registry. Am J Kidney Dis 55:316–325. https://doi.org/10.1053/j.ajkd.2009.10.048
Brogan TV, Lequier L, Lorusso R, MacLaren G, Peek GJ (2017) Extracorporeal life support : the ELSO red book. Extracorporeal Life Support Organization, Ann Arbor
Askenazi DJ, Ambalavanan N, Hamilton K, Cutter G, Laney D, Kaslow R, Georgeson K, Barnhart DC, Dimmitt RA (2011) Acute kidney injury and renal replacement therapy independently predict mortality in neonatal and pediatric noncardiac patients on extracorporeal membrane oxygenation. Pediatr Crit Care Med 12:e1-6. https://doi.org/10.1097/PCC.0b013e3181d8e348
Hall A, Crichton S, Dixon A, Skorniakov I, Kellum JA, Ostermann M (2020) Fluid removal associates with better outcomes in critically ill patients receiving continuous renal replacement therapy: a cohort study. Crit Care 24:279. https://doi.org/10.1186/s13054-020-02986-4
Extracorporeal Life Support Organization (2017) ELSO guidelines for cardiopulmonary extracorporeal life support. https://www.elso.org/Portals/0/ELSO%20Guidelines%20General%20All%20ECLS%20Version%201_4.pdf. Accessed 5 Aug 2021
Silvester W (1997) Mediator removal with CRRT: complement and cytokines. Am J Kidney Dis 30:S38-43. https://doi.org/10.1016/s0272-6386(97)90541-2
Jonckheer J, Vergaelen K, Spapen H, Malbrain M, De Waele E (2019) Modification of nutrition therapy during continuous renal replacement therapy in critically Ill pediatric patients: a narrative review and recommendations. Nutr Clin Pract 34:37–47. https://doi.org/10.1002/ncp.10231
Wolf MJ, Chanani NK, Heard ML, Kanter KR, Mahle WT (2013) Early renal replacement therapy during pediatric cardiac extracorporeal support increases mortality. Ann Thorac Surg 96:917–922. https://doi.org/10.1016/j.athoracsur.2013.05.056
Hoste EA, Maitland K, Brudney CS, Mehta R, Vincent JL, Yates D, Kellum JA, Mythen MG, Shaw AD (2014) Four phases of intravenous fluid therapy: a conceptual model. Br J Anaesth 113:740–747. https://doi.org/10.1093/bja/aeu300
Vaara ST, Ostermann M, Bitker L, Schneider A, Poli E, Hoste E, Fierens J, Joannidis M, Zarbock A, van Haren F, Prowle J, Selander T, Backlund M, Pettila V, Bellomo R (2021) Restrictive fluid management versus usual care in acute kidney injury (REVERSE-AKI): a pilot randomized controlled feasibility trial. Intensive Care Med 47:665–673. https://doi.org/10.1007/s00134-021-06401-6
Hjortrup PB, Haase N, Bundgaard H, Thomsen SL, Winding R, Pettila V, Aaen A, Lodahl D, Berthelsen RE, Christensen H, Madsen MB, Winkel P, Wetterslev J, Perner A (2016) Restricting volumes of resuscitation fluid in adults with septic shock after initial management: the CLASSIC randomised, parallel-group, multicentre feasibility trial. Intensive Care Med 42:1695–1705. https://doi.org/10.1007/s00134-016-4500-7
Chen C, Kollef MH (2015) Targeted fluid minimization following initial resuscitation in septic shock: a pilot study. Chest 148:1462–1469. https://doi.org/10.1378/chest.15-1525
Kaddourah A, Basu RK, Bagshaw SM, Goldstein SL (2017) Epidemiology of acute kidney injury in critically ill children and young adults. N Engl J Med 376:11–20. https://doi.org/10.1056/NEJMoa1611391
Kellum JA, Sileanu FE, Murugan R, Lucko N, Shaw AD, Clermont G (2015) Classifying AKI by urine output versus serum creatinine level. J Am Soc Nephrol 26:2231–2238. https://doi.org/10.1681/ASN.2014070724
Kaddourah A, Basu RK, Goldstein SL, Sutherland SM (2019) Oliguria and acute kidney injury in critically ill children: implications for diagnosis and outcomes. Pediatr Crit Care Med 20:332–339. https://doi.org/10.1097/PCC.0000000000001866
Alten JA, Cooper DS, Blinder JJ, Selewski DT, Tabbutt S, Sasaki J, Gaies MG, Bertrandt RA, Smith AH, Reichle G, Gist KM, Banerjee M, Zhang W, Hock KM, Borasino S (2021) Epidemiology of acute kidney injury after neonatal cardiac surgery: a report from the multicenter neonatal and pediatric heart and renal outcomes network. Crit Care Med 49:e941–e951. https://doi.org/10.1097/CCM.0000000000005165
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, analysis, and writing of the first draft were performed by Kevin Pettit, Katja Gist, and Rashmi Sahay. Dr. Geoffrey Fleming was the leader of the KIDMO group and recently passed away. He was an integral member of the team and was involved in study conception and design. All other authors assisted in the writing of the manuscript and have read and approved the final manuscript.
Corresponding author
Ethics declarations
Informed consent
Ethical oversight for this retrospective research was provided by local institutional review boards at each participating site with a waiver of informed consent.
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose that are relevant to the content of this article.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pettit, K.A., Selewski, D.T., Askenazi, D.J. et al. Synergistic association of fluid overload and acute kidney injury on outcomes in pediatric cardiac ECMO: a retrospective analysis of the KIDMO database. Pediatr Nephrol 38, 1343–1353 (2023). https://doi.org/10.1007/s00467-022-05708-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-022-05708-w