Abstract
Background
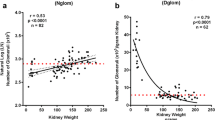
Infants with a solitary functioning kidney (SFK) are at risk for chronic kidney injury (CKI). Lack of compensatory kidney growth (CKG) is associated with CKI, but measuring CKG is challenging since it is typically reported relative to normal kidneys. This study aims to (1) standardize SFK growth in infants, (2) investigate the relationship between standardized kidney length and clinical outcomes, and (3) use these results to develop a risk-based prediction model and local clinical pathway for SFK care.
Methods
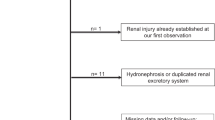
This was a quality improvement study of 166 infants with an SFK. Linear regression was used to assess kidney growth from 0 to 180 days of life. Univariate binary regression analysis was used to identify kidney length to body length thresholds associated with the development of CKI, defined as the composite outcome of chronic kidney disease (eGFR < 60 mL/min/1.73 m2), hypertension, or proteinuria.
Results
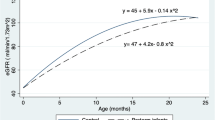
Kidneys grew in length from 0 to 180 days, and growth was constant when standardized to body length. Over follow-up, infants with a baseline kidney length to body length ≤ 0.088 were more likely to experience CKI than the rest of the cohort (27 vs. 8%, p = 0.04). Kidney length to body length ≤ 0.088 was also significantly associated with CKI development (OR 4.17, 95% CI 1.14–15.28, p = 0.04).
Conclusions
In this study, kidney length to body length ratio was a stable CKG metric over 0–180 days, and a baseline ratio ≤ 0.088 was a risk factor for CKI. Results will aid in developing a practical, point-of-care risk assessment tool, and overarching risk-stratified clinical pathway for infants with an SFK.
Graphical abstract
A higher resolution version of the Graphical abstract is available as Supplementary information



Similar content being viewed by others
References
Murugapoopathy V, Gupta IR (2020) A primer on congenital anomalies of the kidneys and urinary tracts (CAKUT). Clin J Am Soc Nephrol 15:723–731
Matsell DG, Bao C, Po White T, Chan E, Matsell E, Cojocaru D, Catapang M, Pediatric Nephrology Clinical Pathway Development Team (2021) Outcomes of solitary functioning kidneys-renal agenesis is different than multicystic dysplastic kidney disease. Pediatr Nephrol 36:3673–3680
Westland R, Schreuder MF, Bokenkamp A, Spreeuwenberg MD, van Wijk JA (2011) Renal injury in children with a solitary functioning kidney–the KIMONO study. Nephrol Dial Transplant 26:1533–1541
Matsell DG, Cojocaru D, Matsell EW, Eddy AA (2015) The impact of small kidneys. Pediatr Nephrol 30:1501–1509
Westland R, Kurvers RA, van Wijk JA, Schreuder MF (2013) Risk factors for renal injury in children with a solitary functioning kidney. Pediatrics 131:e478-485
Urisarri A, Gil M, Mandia N, Aldamiz-Echevarria L, Iria R, Gonzalez-Lamuno D, Couce ML (2018) Retrospective study to identify risk factors for chronic kidney disease in children with congenital solitary functioning kidney detected by neonatal renal ultrasound screening. Medicine 97:e11819
Poggiali IV, Simoes ESAC, Vasconcelos MA, Dias CS, Gomes IR, Carvalho RA, Oliveira MCL, Pinheiro SV, Mak RH, Oliveira EA (2019) A clinical predictive model of renal injury in children with congenital solitary functioning kidney. Pediatr Nephrol 34:465–474
McArdle Z, Schreuder MF, Moritz KM, Denton KM, Singh RR (2020) Physiology and pathophysiology of compensatory adaptations of a solitary functioning kidney. Front Physiol 11:725
Douglas-Denton R, Moritz KM, Bertram JF, Wintour EM (2002) Compensatory renal growth after unilateral nephrectomy in the ovine fetus. J Am Soc Nephrol 13:406–410
van Vuuren SH, Sol CM, Broekhuizen R, Lilien MR, Oosterveld MJ, Nguyen TQ, Goldschmeding R, de Jong TP (2012) Compensatory growth of congenital solitary kidneys in pigs reflects increased nephron numbers rather than hypertrophy. PLoS One 7:e49735
Gilad N, Weissmann-Brenner A, Gilboa Y, Dekel B, Achiron R, Perlman S (2020) Multicystic dysplastic kidney: prenatal compensatory renal growth pattern. J Ultrasound Med 40:2165–2171
Pulido JE, Furth SL, Zderic SA, Canning DA, Tasian GE (2014) Renal parenchymal area and risk of ESRD in boys with posterior urethral valves. Clin J Am Soc Nephrol 9:499–505
Westland R, Schreuder MF, van Goudoever JB, Sanna-Cherchi S, van Wijk JA (2014) Clinical implications of the solitary functioning kidney. Clin J Am Soc Nephrol 9:978–986
Krill A, Salami S, Rosen L, Friedman SC, Gitlin J, Palmer LS (2012) Evaluating compensatory hypertrophy: a growth curve specific for solitary functioning kidneys. J Urol 188:1613–1617
https://ethics.gc.ca/eng/tcps2-eptc2_2018_chapter2-chapitre2.html#a Last accessed Feb 28, 2022
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG (2009) Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42:377–381
Marzuillo P, Guarino S, Grandone A, Di Somma A, Diplomatico M, Rambaldi PF, Decimo F, Miraglia Del Giudice E, La Manna A, Polito C (2019) Congenital solitary kidney size at birth could predict reduced eGFR levels later in life. J Perinatol 39:129–134
La Scola C, Ammenti A, Puccio G, Lega MV, De Mutiis C, Guiducci C, De Petris L, Perretta R, Venturoli V, Vergine G, Zucchini A, Montini G (2016) Congenital solitary kidney in children: size matters. J Urol 196:1250–1256
Currarino G, Williams B, Dana K (1984) Kidney length correlated with age: normal values in children. Radiology 150:703–704
Dinkel E, Ertel M, Dittrich M, Peters H, Berres M, Schulte-Wissermann H (1985) Kidney size in childhood. Sonographical growth charts for kidney length and volume. Pediatr Radiol 15:38–43
Rosenbaum DM, Korngold E, Teele RL (1984) Sonographic assessment of renal length in normal children. AJR Am J Roentgenol 142:467–469
Loftus WK, Gent RJ, LeQuesne GW, Metreweli C (1998) Renal length in Chinese children: sonographic measurement and comparison with western data. J Clin Ultrasound 26:349–352
Capaccioli L, Stecco A, Vanzi E, Brizzi E (2000) Ultrasonographic study on the growth and dimensions of healthy children and adults organs. Ital J Anat Embryol 105:1–50
Chen JJ, Zhi J, Mao W, Steinhardt GF (2006) MrNomogram: a web-based multivariable pediatric renal nomogram. J Pediatr Urol 2:436–438
Obrycki L, Sarnecki J, Lichosik M, Sopinska M, Placzynska M, Stanczyk M, Mirecka J, Wasilewska A, Michalski M, Lewandowska W, Derezinski T, Pac M, Szwarc N, Annusewicz K, Rekuta V, Azukaitis K, Cekuolis A, Wierzbicka-Rucinska A, Jankauskiene A, Kalicki B, Jobs K, Tkaczyk M, Feber J, Litwin M (2021) Kidney length normative values in children aged 0–19 years - a multicenter study. Pediatr Nephrol. https://doi.org/10.1007/s00467-021-05303-5
Morozov D, Parvin N, Conaway M, Oxley G, Baldelomar EJ, Cwiek A, deRonde K, Beeman SC, Charlton JR, Bennett KM (2022) Estimating nephron number from biopsies: impact on clinical studies. J Am Soc Nephrol 33:39–48. https://doi.org/10.1681/ASN.2021070998
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Matsell, D.G., Bao, C., White, T.P. et al. Kidney length standardized to body length predicts outcome in infants with a solitary functioning kidney. Pediatr Nephrol 38, 173–180 (2023). https://doi.org/10.1007/s00467-022-05544-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-022-05544-y