Abstract
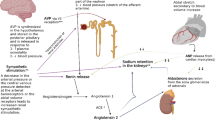
Edema is the abnormal accumulation of fluid in the interstitial compartment of tissues within the body. In nephrotic syndrome, edema is often seen in dependent areas such as the legs, but it can progress to cause significant accumulation in other areas leading to pulmonary edema, ascites, and/or anasarca. In this review, we focus on mechanisms and management of edema in children with nephrotic syndrome. We review the common mechanisms of edema, its burden in pediatric patients, and then present our approach and algorithm for management of edema in pediatric patients. The extensive body of experience accumulated over the last 5 decades means that there are many options, and clinicians may choose among these options based on their experience and careful monitoring of responses in individual patients.


Similar content being viewed by others
References
Eknoyan G (1997) A history of edema and its management. Kidney Int Suppl 59:S118–S126
Pal A, Kaskel F (2016) History of nephrotic syndrome and evolution of its treatment. Front Pediatr 4:56. https://doi.org/10.3389/fped.2016.00056
Gipson DS, Selewski DT, Massengill SF, Wickman L, Messer KL, Herreshoff E, Bowers C, Ferris ME, Mahan JD, Greenbaum LA, MacHardy J, Kapur G, Chand DH, Goebel J, Barletta GM, Geary D, Kershaw DB, Pan CG, Gbadegesin R, Hidalgo G, Lane JC, Leiser JD, Plattner BW, Song PX, Thissen D, Liu Y, Gross HE, DeWalt DA (2013) Gaining the PROMIS perspective from children with nephrotic syndrome: a Midwest pediatric nephrology consortium study. Health Qual Life Outcomes 11:30. https://doi.org/10.1186/1477-7525-11-30
Selewski DT, Troost JP, Massengill SF, Gbadegesin RA, Greenbaum LA, Shatat IF, Cai Y, Kapur G, Hebert D, Somers MJ, Trachtman H, Pais P, Seifert ME, Goebel J, Sethna CB, Mahan JD, Gross HE, Herreshoff E, Liu Y, Song PX, Reeve BB, DeWalt DA, Gipson DS (2015) The impact of disease duration on quality of life in children with nephrotic syndrome: a Midwest Pediatric Nephrology Consortium study. Pediatr Nephrol 30:1467–1476. https://doi.org/10.1007/s00467-015-3074-x
Rheault MN, Zhang L, Selewski DT, Kallash M, Tran CL, Seamon M, Katsoufis C, Ashoor I, Hernandez J, Supe-Markovina K, D'Alessandri-Silva C, De Jesus-Gonzalez N, Vasylyeva TL, Formeck C, Woll C, Gbadegesin R, Geier P, Devarajan P, Carpenter SL, Kerlin BA, Smoyer WE, Midwest Pediatric Nephrology Consortium (2015) AKI in children hospitalized with nephrotic syndrome. Clin J Am Soc Nephrol 10:2110–2118. https://doi.org/10.2215/CJN.06620615
Meyrier A, Niaudet P (2018) Acute kidney injury complicating Nephrotic syndrome of minimal change disease. Kidney Int 94:861–869
Prasad BS, Kumar M, Dabas A, Mishra K (2019) Profile of acute kidney injury in hospitalized children with idiopathic nephrotic syndrome. Indian Pediatr 56:119–122
Ellis D (2015) Pathophysiology, evaluation, and management of edema in childhood nephrotic syndrome. Front Pediatr 3:111. https://doi.org/10.3389/fped.2015.00111
Humphreys MH (1994) Mechanisms and management of nephrotic edema. Kidney Int 45:266–281. https://doi.org/10.1038/ki.1994.33
Noddeland H, Riisnes SM, Fadnes HO (1982) Interstitial fluid colloid osmotic and hydrostatic pressures in subcutaneous tissue of patients with nephrotic syndrome. Scand J Clin Lab Invest 42:139–146
Bockenhauer D (2013) Over- or underfill: not all nephrotic states are created equal. Pediatr Nephrol 28:1153–1156. https://doi.org/10.1007/s00467-013-2435-6
Siddall EC, Radhakrishnan J (2012) The pathophysiology of edema formation in the nephrotic syndrome. Kidney Int 82:635–642. https://doi.org/10.1038/ki.2012.180
Gupta S, Pepper RJ, Ashman N, Walsh SB (2019) Nephrotic syndrome: oedema formation and its treatment with diuretics. Front Physiol 9:1868
Dorhout EJ, Roos JC, Boer P, Yoe OH, Simatupang TA (1979) Observations on edema formation in the nephrotic syndrome in adults with minimal lesions. Am J Med 67:378–384. https://doi.org/10.1016/0002-9343(79)90782-4
Meltzer JI, Keim HJ, Laragh JH, Sealey JE, Jan KM, Chien S (1979) Nephrotic syndrome: vasoconstriction and hypervolemic types indicated by renin-sodium profiling. Ann Intern Med 91:688–696. https://doi.org/10.7326/0003-4819-91-5-688
Ichikawa I, Rennke HG, Hoyer JR, Badr KF, Schor N, Troy JL, Lechene CP, Brenner BM (1983) Role for intrarenal mechanisms in the impaired salt excretion of experimental nephrotic syndrome. J Clin Invest 71:91–103
Vogt B, Favre H (1991) Na+,K(+)-ATPase activity and hormones in single nephron segments from nephrotic rats. Clin Sci (Lond) 80:599–604
Buyukavci MA, Civilibal M, Elevli M, Selcuk Duru HN (2015) Hypo- and hypervolemic edema in children with steroid sensitive nephrotic syndrome. Turk J Med Sci 45:178–183
Iyengar AA, Kamath N, Vasudevan A, Phadke KD (2011) Urinary indices during relapse of childhood nephrotic syndrome. Indian J Nephrol 21:172–176. https://doi.org/10.4103/0971-4065.83030
Lu H, Kapur G, Mattoo TK, Lyman WD (2012) Hypoxia decreases podocyte expression of slit diaphragm proteins. Int J Nephrol Renov Dis 5:101–107. https://doi.org/10.2147/IJNRD.S27332
Svenningsen P, Bistrup C, Friis UG, Bertog M, Haerteis S, Krueger B, Stubbe J, Jensen ON, Thiesson HC, Uhrenholt TR, Jespersen B, Jensen BL, Korbmacher C, Skott O (2009) Plasmin in nephrotic urine activates the epithelial sodium channel. J Am Soc Nephrol 20:299–310. https://doi.org/10.1681/ASN.2008040364
Deschênes G, Wittner M, Stefano A, Jounier S, Doucet A (2001) Collecting duct is a site of sodium retention in PAN nephrosis: a rationale for amiloride therapy. J Am Soc Nephrol 12:598–601
Deschenes G, Doucet A (2000) Collecting duct (Na+/K+)-ATPase activity is correlated with urinary sodium excretion in rat nephrotic syndromes. J Am Soc Nephrol 11:604–615
Kottke MA, Walters TJ (2016) Where's the leak in vascular barriers? A review. Shock 46(3 Suppl 1):20–36. https://doi.org/10.1097/SHK.0000000000000666
Myburgh JA, Mythen MG (2013) Resuscitation fluids. N Engl J Med 369:1243–1251
Chignalia AZ, Yetimakman F, Christiaans SC, Unal S, Bayrakci B, Wagener BM, Russell RT, Kerby JD, Pittet JF, Dull RO (2016) The glycocalyx and trauma: a review. Shock 45:338–348
Fiorotto M, Coward WA (1979) Pathogenesis of oedema in protein-energy malnutrition: the significance of plasma colloid osmotic pressure. Br J Nutr 42:21–31
Geers AB, Koomans HA, Roos JC, Boer P, Dorhout Mees EJ (1984) Functional relationships in the nephrotic syndrome. Kidney Int 26:324–330. https://doi.org/10.1038/ki.1984.176
Siddall EC, Radhakrishnan J (2012) The pathophysiology of edema formation in the nephrotic syndrome. Kidney Int 82:635–642. https://doi.org/10.1038/ki.2012.180
Vande Walle JG, Donckerwolcke RA, Koomans HA (1999) Pathophysiology of edema formation in children with nephrotic syndrome not due to minimal change disease. J Am Soc Nephrol 10:323–331
Johnson MD, Malvin RL (1977) Stimulation of renal sodium reabsorption by angiotensin II. Am J Phys 232:F298–F306
Light DB, Schwiebert EM, Karlson KH, Stanton BA (1989) Atrial natriuretic peptide inhibits a cation channel in renal inner medullary collecting duct cells. Science 243:383–385
Perico N, Delaini F, Lupini C, Benigni A, Galbusera M, Boccardo P, Remuzzi G (1989) Blunted excretory response to atrial natriuretic peptide in experimental nephrosis. Kidney Int 36:57–64. https://doi.org/10.1038/ki.1989.161
Valentin JP, Qiu C, Muldowney WP, Ying WZ, Gardner DG, Humphreys MH (1992) Cellular basis for blunted volume expansion natriuresis in experimental nephrotic syndrome. J Clin Invest 90:1302–1312. https://doi.org/10.1172/JCI115995
Mansy H, Goodship TH, Tapson JS, Hartley GH, Keavey P, Wilkinson R (1989) Effect of a high protein diet in patients with the nephrotic syndrome. Clin Sci (Lond) 77:445–451
Cadnapaphornchai MA, Tkachenko O, Shchekochikhin D, Schrier RW (2014) The nephrotic syndrome: pathogenesis and treatment of edema formation and secondary complications. Pediatr Nephrol 29:1159–1167
Kapur G, Valentini RP, Imam AA, Mattoo TK (2009) Treatment of severe edema in children with nephrotic syndrome with diuretics alone--a prospective study. Clin J Am Soc Nephrol 4:907–913
Matsumoto H, Miyaoka Y, Okada T, Nagaoka Y, Wada T, Gondo A, Esaki S, Hayashi A, Nakao T (2011) Ratio of urinary potassium to urinary sodium and the potassium and edema status in nephrotic syndrome. Intern Med 50:551–555
Donckerwolcke RAMG, France A, Raes A, Vande Walle J (2003) Distal nephron sodium-potassium exchange in children with nephrotic syndrome. Clin Nephrol 59:259–266
Brater DC (1991) Clinical pharmacology of loop diuretics. Drugs 41:14–22. https://doi.org/10.2165/00003495-199100413-00004
Hammarlund MM, Paalzow LK, Odlind B (1984) Pharmacokinetics of furosemide in man after intravenous and oral administration. Application of moment analysis. Eur J Clin Pharmacol 26:197–207
Waller ES, Hamilton SF, Massarella JW, Sharanevych MA, Smith RV, Yakatan GJ, Doluisio JT (1981) Disposition and absolute bioavailability of furosemide in healthy males. J Pharm Sci 71:1105–1108
Hoorn EJ, Ellison DH (2017) Diuretic resistance. Am J Kidney Dis 69:136–142
Sica DA (2003) Drug absorption in the management of congestive heart failure: loop diuretics. Congest Heart Fail 9:287–292
Duffy M, Jain S, Harrell N, Kothari N, Reddi AS (2015) Albumin and furosemide combination for management of edema in nephrotic syndrome: a review of clinical studies. Cells 4:622–630
Agarwal R, Gorski JC, Sundblad K, Brater DC (2000) Urinary protein binding does not affect response to furosemide in patients with nephrotic syndrome. J Am Soc Nephrol 11:1100–1105
Brater DC, Day B, Burdette A, Anderson S (1984) Bumetanide and furosemide in heart failure. Kidney Int 26:183–189
Lau K, DeFronzo R, Morrison G, Rascoff J, Goldberg M, Agus ZS (1976) Effectiveness of bumetanide in nephrotic syndrome: a double-blind crossover study with furosemide. J Clin Pharmacol 16:489–497
Hropot M, Fowler N, Karlmark B, Giebisch G (1985) Tubular action of diuretics: distal effects on electrolyte transport and acidification. Kidney Int 28:477–489
Suki WN, Dawoud F, Eknoyan G, Martinez-Maldonado M (1972) Effects of metolazone on renal function in normal man. J Pharmacol Exp Ther 180:6–12
Preisig PA, Toto RD, Alpern RJ (1987) Carbonic anhydrase inhibitors. Renal Physiol 10:136–159
Vidt DG (1981) Mechanism of action, pharmacokinetics, adverse effects, and therapeutic uses of amiloride hydrochloride, a new potassium-sparing diuretic. Pharmacotherapy 1:179–187
Hinrichs GR, Mortensen LA, Jensen BL, Bistrup C (2018) Amiloride resolves resistant edema and hypertension in a patient with nephrotic syndrome; a case report. Phys Rep 6:e13743
Peters H, Noble NA (1997) Angiotensin II and L-arginine in tissue fibrosis: more than blood pressure. Kidney Int 51:1481–1486. https://doi.org/10.1038/ki.1997.203
Shin GT, Kim SJ, Ma KA, Kim HS, Kim D (2000) ACE inhibitors attenuate expression of renal transforming growth factor-beta1 in humans. Am J Kidney Dis 36:894–902
Berlyne GM, Brown C, Adler A, Feinroth MV, Feinroth M, Hirsch S, Friedman EA (1981) Water immersion in nephrotic syndrome. Arch Intern Med 141:1275–1278
Gheorghiade M, Orlandi C, Burnett JC, Demets D, Grinfeld L, Maggioni A, Swedberg K, Udelson JE, Zannad F, Zimmer C, Konstam MA (2005) Rationale and design of the multicenter, randomized, double-blind, placebo-controlled study to evaluate the efficacy of vasopressin antagonism in heart failure: outcome study with tolvaptan (EVEREST). J Card Fail 11:260–269
Okita K, Sakaida I, Okada M, Kaneko A, Chayama K, Kato M, Sata M, Yoshihara H, Ono N, Murawaki Y (2010) A multicenter, open-label, dose-ranging study to exploratively evaluate the efficacy, safety, and dose-response of tolvaptan in patients with decompensated liver cirrhosis. J Gastroenterol 45:979–987
Chen S, Zhao JJ, Tong NW, Guo XH, Qiu MC, Yang GY, Liu ZM, Ma JH, Zhang ZW, Gu F (2014) Randomized, double blinded, placebo-controlled trial to evaluate the efficacy and safety of tolvaptan in Chinese patients with hyponatremia caused by SIADH. J Clin Pharmacol 54:1362–1367
Petereit C, Zaba O, Teber I, Luders H, Grohe C (2013) A rapid and efficient way to manage hyponatremia in patients with SIADH and small cell lung cancer: treatment with tolvaptan. BMC Pulm Med 13:55
Park ES, Huh YS, Kim GH (2015) Is tolvaptan indicated for refractory oedema in nephrotic syndrome? Nephrology (Carlton) 20:103–106. https://doi.org/10.1111/nep.12348
Shimizu M, Ishikawa S, Yachi Y, Muraoka M, Tasaki Y, Iwasaki H, Kuroda M, Ohta K, Yachie A (2014) Tolvaptan therapy for massive edema in a patient with nephrotic syndrome. Pediatr Nephrol 29:915–917
Takada T, Masaki T, Hoshiyama A, Toki T, Kamata Y, Shichiri M (2018) Tolvaptan alleviates excessive fluid retention of nephrotic diabetic renal failure unresponsive to furosemide. Nephrology (Carlton) 23:883–886
Tanaka A, Nakamura T, Sato E, Ueda Y, Node K (2017) Different effects of tolvaptan in patients with idiopathic membranous nephropathy with nephrotic syndrome. Intern Med 56:191–196
Cil O, Esteva-Font C, Tas ST, Su T, Lee S, Anderson MO, Ertunc M, Verkman AS (2015) Salt-sparing diuretic action of a water-soluble urea analog inhibitor of urea transporters UT-A and UT-B in rats. Kidney Int 88:311–320
Knepper MA, Miranda CA (2013) Urea channel inhibitors: a new functional class of aquaretics. Kidney Int 83:991–993
Chen Y, Burnett JC (2018) Particulate guanylyl cyclase a/cGMP signaling pathway in the kidney: physiologic and therapeutic indications. Int J Mol Sci 19:1006. https://doi.org/10.3390/ijms19041006
Wilson SS, Ayaz SI, Levy PD (2015) Relaxin: a novel agent for the treatment of acute heart failure. Pharmacotherapy 35:315–327. https://doi.org/10.1002/phar.1548
Gimpelewicz C, Metra M, Cleland JGF, Szecsody P, Chang Wun CC, Boer-Martins L, Cotter G, Davison BA, Felker GM, Filippatos G, Greenberg BH, Pang P, Ponikowski P, Severin T, Voors AA, Teerlink JR (2017) Effects of serelaxin on the outcome of patients with or without substantial peripheral edema: a subgroup analysis from the RELAX-AHF trial. Am Heart J 190:113–122
Theilig F, Wu Q (2015) ANP-induced signaling cascade and its implications in renal pathophysiology. Am J Physiol Ren Physiol 308:F1047–F1055
Ueda K, Hirahashi J, Seki G, Tanaka M, Kushida N, Takeshima Y, Nishikawa Y, Fujita T, Nangaku M (2014) Successful treatment of acute kidney injury in patients with idiopathic nephrotic syndrome using human atrial natriuretic peptide. Intern Med 53:865–869
Boeing T, da Silva LM, Mariott M, Andrade SF, de Souza P (2017) Diuretic and natriuretic effect of luteolin in normotensive and hypertensive rats: role of muscarinic acetylcholine receptors. Pharmacol Rep 69:1121–1124. https://doi.org/10.1016/j.pharep.2017.05.010
Mariano LNB, Boeing T, da Silva R, Cechinel-Filho V, Niero R, da Silva LM, de Souza P, Andrade SF (2018) Preclinical evaluation of the diuretic and saluretic effects of (-)-epicatechin and the result of its combination with standard diuretics. Biomed Pharmacother 107:520–525
Availability of data and material
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Code availability
Not applicable.
Additional information
Answers:
1. c; 2. a; 3. b; 4. a
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Multiple-choice questions (answers follow reference list)
Multiple-choice questions (answers follow reference list)
-
1-
A 12-year-old male with SRNS presented to the ER with worsening edema. Exam showed facial and leg edema with ascites and he looked uncomfortable. Vital signs: heart rate 75/min, respiratory rate 24/min, BP 138/76 with no orthostatic hypotension. Work up showed: serum albumin 2.2 g/dl, serum Cr 0.5 mg/dl, urine protein > 300 mg/dl and negative for blood.
Of the following, the most likely pathophysiologic mechanism of edema in this child:
-
a)
Lack of hematuria makes overfill more likely than underfill as the dominant mechanism
-
b)
Underfill is the most likely mechanism with his serum albumin > 2 g/dl
-
c)
The absence of hypotension makes overfill the more likely dominant mechanism
-
d)
We cannot determine his most likely mechanism since we do not have the urine Na measured.
-
a)
-
2-
In the previous case, the best initial plan to treat his edema is:
-
a)
Furosemide
-
b)
Albumin 25% followed by Furosemide
-
c)
Amiloride
-
d)
Hydrochlorothiazide.
-
a)
-
3-
A 9-year-old male with SRNS presented for a routine clinic visit. You noticed that he gained 12 lbs. since his last clinic visit six weeks ago and he complains of discomfort with his feet. He appeared comfortable otherwise and denied any pain. His physical examination showed pitting edema in his feet and legs and mild abdominal distention. His BP was 90/55, heart rate 90 /min. When approaching edema management in this child, of the following options, the best one to pursue is to:
-
a)
Avoid the outpatient use of loop diuretics as these agents are associated with increased risk of acute kidney injury
-
b)
Initiate diuretics since reducing edema has been shown to improve quality of life in subjects with NS
-
c)
Initiate a small dose of Lisinopril and follow up his weight in 1 week
-
d)
There is no indication to initiate diuretics since he has minimal symptoms.
-
a)
-
4-
A 7-year-old female with NS was admitted to the hospital for management of severe edema. Physical examination showed significant edema overall, abdominal distention and mild abdominal pain with palpation. Her BP was 132/85 and heart rate 90/min. Serum albumin was 2.3 g/dl. After 36 h of diuresis with furosemide, her fluid balance was negative for 560 ml and she continued to complain of abdominal discomfort. Of the following factors, this poor response to diuretics may best be explained by:
-
a)
Decreased kidney function
-
b)
Decreased distribution of furosemide in extracellular space with edema
-
c)
Increased excretion of furosemide into the urinary filtrate in NS
-
d)
Lack of binding of furosemide to albumin in the intratubular space
-
a)
Rights and permissions
About this article
Cite this article
Kallash, M., Mahan, J.D. Mechanisms and management of edema in pediatric nephrotic syndrome. Pediatr Nephrol 36, 1719–1730 (2021). https://doi.org/10.1007/s00467-020-04779-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-020-04779-x