Abstract
Background
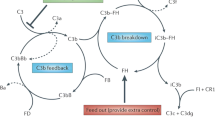
Anti-complement factor H (CFH) autoantibody-associated hemolytic uremic syndrome (HUS) is a severe sub-type of HUS.
Methods
We assessed the clinical and renal pathological features, circulating complement levels, and genetic background of Chinese pediatric patients with this sub-type of HUS. Thirty-three consecutive patients with acute kidney injury who tested positive for serum anti-CFH autoantibodies were enrolled in this study.
Results
All of the eight patients who underwent renal biopsies presented with changes typical of thrombotic microangiopathy, especially changes in chronic characteristics. Compared to patients in remission and normal control subjects, patients with acute disease had significantly lower plasma CFH levels and significantly higher plasma complement 3a (C3a), C5a, and terminal complement complex (SC5b-9) levels. The CFH–anti-CFH immunoglobin G (IgG) circulating immunocomplex (CFH-CIC) titers were more closely correlated with CFH plasma levels than anti-CFH IgG levels. Of the 22 patients, four (18%) were homozygous for CFHR3–1Δ and ten were heterozygous for CFHR1 or CFHR3 deletions. Most patients responded well to a combination of plasma and immunosuppressive therapies, with a remission rate of 87%. At the end of the follow-up, nine patients reached the combined end-points, including two with end-stage renal disease and seven with relapses.
Conclusion
Plasma C3a, C5a, and SC5b-9 levels predicted disease activity in anti-CFH autoantibody-associated HUS patients enrolled in this study. These patients responded well to plasma therapy combined with immunosuppression.




Similar content being viewed by others
References
Copelovitch L, Kaplan BS (2008) The thrombotic microangiopathies. Pediatr Nephrol 23:1761–1767
Westra D, Volokhina E, van der Heijden E, Vos A, Huigen M, Jansen J, van Kaauwen E, van der Velden T, van de Kar N, van den Heuvel L (2010) Genetic disorders in complement (regulating) genes in patients with atypical hemolytic uremic syndrome (aHUS). Nephrol Dial Transplant 25:2195–2202
Boyce TG, Swerdlow DL, Griffin PM (1995) Escherichia coli O157:H7 and the hemolytic-uremic syndrome. N Engl J Med 333(6):364–368
Bresin E, Rurali E, Caprioli J, Sanchez-Corral P, Fremeaux-Bacchi V, Rodriguez de Cordoba S, Pinto S, Goodship TH, Alberti M, Ribes D, Valoti E, Remuzzi G, Noris M, European Working Party on Complement Genetics in Renal Diseases (2013) Combined complement gene mutations in atypical hemolytic uremic syndrome influence clinical phenotype. J Am Soc Nephrol 24:475–486
George JN, Nester CM (2014) Syndromes of thrombotic microangiopathy. N Engl J Med 371:654–666
George JN, Nester CM (2014) Syndromes of thrombotic microangiopathy. N Engl J Med 371:1847–1848
Moore I, Strain L, Pappworth I (2010) Association of factor H autoantibodies with deletions of CFHR1, CFHR3, CFHR4, and with mutations in CFH, CFI, CD46, and C3 in patients with atypical hemolytic uremic syndrome. Blood 115:379–387
Geerdink LM, Westra D, van Wijk JA, Dorresteijn EM, Lilien MR, Davin JC, Kömhoff M, Van Hoeck K, van der Vlugt A, van den Heuvel LP, van de Kar NC (2012) Atypical hemolytic uremic syndrome in children: complement mutations and clinical characteristics. Pediatr Nephrol 27:1283–1291
Hofer J, Janecke AR, Zimmerhackl LB, Riedl M, Rosales A, Giner T, Cortina G, Haindl CJ, Petzelberger B, Pawlik M, Jeller V, Vester U, Gadner B, van Husen M, Moritz ML, Würzner R, Jungraithmayr T, German-Austrian HUS Study Group (2013) Complement factor H-related protein 1 deficiency and factor H antibodies in pediatric patients with atypical hemolytic uremic syndrome. Clin J Am Soc Nephrol 8:407–415
Dragon-Durey MA, Loirat C, Cloarec S, Macher MA, Blouin J, Nivet H, Weiss L, Fridman WH, Frémeaux-Bacchi V (2005) Anti-Factor H autoantibodies associated with atypical hemolytic uremic syndrome. J Am Soc Nephrol 16:555–563
Jozsi M, Licht C, Strobel S, Zipfel SL, Richter H, Heinen S, Zipfel PF, Skerka C (2008) Factor H autoantibodies in atypical hemolytic uremic syndrome correlate with CFHR1/CFHR3 deficiency. Blood 111:1512–1514
Strobel S, Hoyer PF, Mache CJ, Sulyok E, Liu WS, Richter H, Oppermann M, Zipfel PF, Józsi M (2010) Functional analyses indicate a pathogenic role of factor H autoantibodies in atypical haemolytic uraemic syndrome. Nephrol Dial Transplant 25:136–144
Lee BH, Kwak SH, Shin JI, Lee SH, Choi HJ, Kang HG, Ha IS, Lee JS, Dragon-Durey MA, Choi Y, Cheong H (2009) Atypical hemolytic uremic syndrome associated with complement factor H autoantibodies and CFHR1/CFHR3 deficiency. Pediatr Res 66:336–340
Dragon-Durey MA, Sethi SK, Bagga A, Blanc C, Blouin J, Ranchin B, André JL, Takagi N, Cheong HI, Hari P, Le Quintrec M, Niaudet P, Loirat C, Fridman WH, Frémeaux-Bacchi V (2010) Clinical features of anti-factor H autoantibody-associated hemolytic uremic syndrome. J Am Soc Nephrol 21:2180–2187
Blanc C, Roumenina LT, Ashraf Y, Hyvärinen S, Sethi SK, Ranchin B, Niaudet P, Loirat C, Gulati A, Bagga A, Fridman WH, Sautès-Fridman C, Jokiranta TS, Frémeaux-Bacchi V, Dragon-Durey MA (2012) Overall neutralization of complement factor H by autoantibodies in the acute phase of the autoimmune form of atypical hemolytic uremic syndrome. J Immunol 189:3528–3537
Rose M, Rowe JM, Eldor A (1993) The changing course of thrombotic thrombocytopenic purpura and modern therapy. Blood Rev 7:94–103
Wyllie BF, Garg AX, Macnab J, Rock GA, Clark WF (2006) Thrombotic thrombocytopenic purpura/haemolytic uraemic syndrome: a new index predicting response to plasma exchange. Br J Haematol 132:204–209
Yu XJ, Yu F, Song D, Wang SX, Song Y, Liu G, Zhao MH (2014) Clinical and renal biopsy findings predicting outcome in renal thrombotic microangiopathy: a large cohort study from a single institute in China. Sci World J 2014:680502. doi:10.1155/2014/680502
Wu LH, Yu F, Tan Y, Qu Z, Chen MH, Wang SX, Liu G, Zhao MH (2013) Inclusion of renal vascular lesions in the 2003 ISN/RPS system for classifying lupus nephritis improves renal outcome predictions. Kidney Int 83:715–723
Wang FM, Yu F, Tan Y, Song D, Zhao MH (2012) Serum complement factor H is associated with clinical and pathological activities of patients with lupus nephritis. Rheumatology 51(12):2269–2277
Gonzalez-Rubio C, Ferreira-Cerdan A, Ponce IM, Arpa J, Fontán G, López-Trascasa M (2001) Complement factor I deficiency associated with recurrent meningitis coinciding with menstruation. Arch Neurol 58:1923–1928
Watson R, Lindner S, Bordereau P, Hunze EM, Tak F, Ngo S, Zipfel PF, Skerka C, Dragon-Durey MA, Marchbank KJ (2014) Standardisation of the factor H autoantibody assay. Immunobiology 219:9–16
Zipfel PF, Edey M, Heinen S, Józsi M, Richter H, Misselwitz J, Hoppe B, Routledge D, Strain L, Hughes AE, Goodship JA, Licht C, Goodship TH, Skerka C (2007) Deletion of complement factor H-related genes CFHR1 and CFHR3 is associated with atypical hemolytic uremic syndrome. PLoS Genet 3:e41
Cofiell R, Kukreja A, Bedard K, Yan Y, Mickle AP, Ogawa M, Bedrosian CL, Faas SJ (2015) Eculizumab reduces complement activation, inflammation, endothelial damage, thrombosis, and renal injury markers in aHUS. Blood 125:3253–3262
Chua JS, Baelde HJ, Zandbergen M, Wilhelmus S, van Es LA, de Fijter JW, Bruijn JA, Bajema IM, Cohen D (2015) Complement Factor C4d Is a Common Denominator in Thrombotic Microangiopathy. J Am Soc Nephrol 26:2239–2247
Allford SL, Hunt BJ, Rose P, Machin SJ (2003) Guidelines on the diagnosis and management of the thrombotic microangiopathic haemolytic anaemias. Br J Haematol 120:556–573
Scully M, Hunt BJ, Benjamin S, Liesner R, Rose P, Peyvandi F, Cheung B, Machin SJ, British Committee for Standards in Haematology (2012) Guidelines on the diagnosis and management of thrombotic thrombocytopenic purpura and other thrombotic microangiopathies. Br J Haematol 158:323–335
Taylor CM, Machin S, Wigmore SJ, Goodship TH (2010) Clinical practice guidelines for the management of atypical haemolytic uraemic syndrome in the United Kingdom. Br J Haematol 148:37–47
Loirat C, Fakhouri F, Ariceta G, Besbas N, Bitzan M, Bjerre A, Coppo R, Emma F, Johnson S, Karpman D, Landau D, Langman CB, Lapeyraque AL, Licht C, Nester C, Pecoraro C, Riedl M, van de Kar NC, Van de Walle J, Vivarelli M, Frémeaux-Bacchi V, HUS International (2016) An international consensus approach to the management of atypical hemolytic uremic syndrome in children. Pediatr Nephrol 31:15–39
Khandelwal P, Gupta A, Sinha A, Saini S, Hari P, Dragon Durey MA, Bagga A (2015) Effect of plasma exchange and immunosuppressive medications on antibody titers and outcome in anti-complement factor H antibody-associated hemolytic uremic syndrome. Pediatr Nephrol 30:451–457
Sinha A, Gulati A, Saini S, Blanc C, Gupta A, Gurjar BS, Saini H, Kotresh ST, Ali U, Bhatia D, Ohri A, Kumar M, Agarwal I, Gulati S, Anand K, Vijayakumar M, Sinha R, Sethi S, Salmona M, George A, Bal V, Singh G, Dinda AK, Hari P, Rath S, Dragon-Durey MA, Bagga A, Indian HUS (2014) Registry Prompt plasma exchanges and immunosuppressive treatment improves the outcomes of anti-factor H autoantibody-associated hemolytic uremic syndrome in children. Kidney Int 85:1151–1160
Boyer O, Balzamo E, Charbit M, Biebuyck-Gougé N, Salomon R, Dragon-Durey MA, Frémeaux-Bacchi V, Niaudet P (2010) Pulse cyclophosphamide therapy and clinical remission in atypical hemolytic uremic syndrome with anti-complement factor H autoantibodies. Am J Kidney Dis 55:923–927
Lee JM, Park YS, Lee JH, Park SJ, Shin JI, Park YH, Yoo KH, Cho MH, Kim SY, Kim SH, Namgoong MK, Lee SJ, Lee JH, Cho HY, Han KH, Kang HG, Ha IS, Bae JS, Kim NK, Park WY, Cheong H (2014) Atypical hemolytic uremic syndrome: Korean pediatric series. Pediatr Int 57:431–438
Noris M, Caprioli J, Bresin E, Mossali C, Pianetti G, Gamba S, Daina E, Fenili C, Castelletti F, Sorosina A, Piras R, Donadelli R, Maranta R, van der Meer I, Conway EM, Zipfel PF, Goodship TH, Remuzzi G (2010) Relative role of genetic complement abnormalities in sporadic and familial aHUS and their impact on clinical phenotype. Clin J Am Soc Nephrol 5:1844–1859
Abarrategui-Garrido C, Martinez-Barricarte R, Lopez-Trascasa M, de Cordoba SR, Sanchez-Corral P (2009) Characterization of complement factor H-related (CFHR) proteins in plasma reveals novel genetic variations of CFHR1 associated with atypical hemolytic uremic syndrome. Blood 114:4261–4271
Acknowledgements
We gratefully acknowledge the contributions of Jie AO, Xin ZHENG and Lei QU of the Peking University First Hospital in our histopathological studies. This work was supported by grants from the National Natural Science Foundation of China to Innovation Research Group (No. 81321064), National Natural Science Foundation of China (No. 81470932, No.81500526, No, 81670639 and No. 81670640), The Capital Health Research and Development of Special Grant (No. 2016-2-2094) and the Research on the Application of Capital Clinical Characteristics Program of Beijing Municipal Science and Technology Commission (No. Z161100000516106).
Author information
Authors and Affiliations
Consortia
Corresponding authors
Ethics declarations
The research was in compliance with the Declaration of Helsinki Principles and approved by the local ethical committees. Informed consent of the participants or the parents of minor patients was obtained for blood sampling and renal biopsy
Disclosures
None
Additional information
Xiao-rong Liu and Feng Yu contributed equally to this work.
Rights and permissions
About this article
Cite this article
Song, D., Liu, Xr., Chen, Z. et al. The clinical and laboratory features of Chinese Han anti-factor H autoantibody-associated hemolytic uremic syndrome. Pediatr Nephrol 32, 811–822 (2017). https://doi.org/10.1007/s00467-016-3562-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-016-3562-7