Abstract
Background
To create a suitable animal model for the training of laparoscopic anatomic liver resection, we performed left hepatectomy using a goat and found its suitability. We have since started using goats for wet-lab training and have gradually standardized the relevant procedures. Herein, we report our standardized training procedures using a goat and discuss its feasibility as a novel training model.
Methods
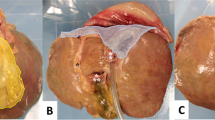
The standardized wet-lab training courses of laparoscopic liver resection conducted on 62 tables with a total of 70 goats were reviewed. The training course began by encircling the hepatoduodenal ligament for the Pringle maneuver, which was repeated during the parenchymal dissection. Following partial liver resection of the left lateral section, left hepatectomy was performed by a standardized procedure for humans in which the liver was split, exposing the entire length of the middle hepatic vein trunk from the dorsal side after extrahepatic transection of the left Glissonean pedicle. If a goat deceased before initiating left hepatectomy, the training was restarted with a new goat. The surgical procedures were performed by surgeons of varying skill levels.
Results
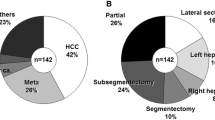
A total of 184 surgeons including 10 surgical residents participated in the training. Partial liver resection was initiated in 62 tables, with 8 (13%) dying during or after the procedure of partial liver resection. Subsequently, left hepatectomy was initiated in 61 and completed in 59 tables (98%), regardless of whether the goat survived or deceased, and was not completed in 2 tables (3%) due to time limitation. In 14 tables (23%), the goats deceased during the procedure, however, the procedure was completed. The causes of death were multifactorial, including massive bleeding, reperfusion injury after the Pringle maneuver, and carbon dioxide gas embolism.
Conclusions
Left hepatectomy in a goat is useful as a training model for laparoscopic anatomic liver resection.






Similar content being viewed by others
References
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, O’Rourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CH, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen KH, Schon MR, Sugioka A, Tang CN, Herman P, Pekolj J, Chen XP, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo CM, Clavien PA, Kokudo N, Barkun J, Strasberg SM (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Abu Hilal M, Aldrighetti L, Dagher I, Edwin B, Troisi RI, Alikhanov R, Aroori S, Belli G, Besselink M, Briceno J, Gayet B, D’Hondt M, Lesurtel M, Menon K, Lodge P, Rotellar F, Santoyo J, Scatton O, Soubrane O, Sutcliffe R, Van Dam R, White S, Halls MC, Cipriani F, Van der Poel M, Ciria R, Barkhatov L, Gomez-Luque Y, Ocana-Garcia S, Cook A, Buell J, Clavien PA, Dervenis C, Fusai G, Geller D, Lang H, Primrose J, Taylor M, Van Gulik T, Wakabayashi G, Asbun H, Cherqui D (2018) The Southampton consensus guidelines for laparoscopic liver surgery: from indication to implementation. Ann Surg 268:11–18
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative short-term benefits of laparoscopic liver resection: cases and climbing. Ann Surg 263:761–777
Komorowski AL, Mituś JW, Sanchez Hurtado MA, Sanchez Margallo FM (2015) Porcine model in the laparoscopic liver surgery training. Pol Przegl Chir 87:425–428
Popa C, Voicescu GT, Pestean C, Graur F, Momani TA, Al-Hajjar N, Liviu I (2020) An innovative approach for laparoscopic liver resections. Train protocol Ann Ital Chir 91:105–111
Lada E, Anna M, Patrik M, Zbynek T, Miroslav J, Hynek M, Richard P, Sarah L, Vaclav L (2020) Porcine liver anatomy applied to biomedicine. J Surg Res 250:70–79
Nykonenko A, Vávra P, Zonča P (2017) Anatomic peculiarities of pig and human liver. Exp Clin Transpl 15:21–26
Okuda Y, Honda G, Kurata M, Kobayashi S (2013) Useful and convenient procedure for intermittent vascular occlusion in laparoscopic hepatectomy. Asian J Endosc Surg 6:100–103
Honda G, Ome Y, Yoshida N, Kawamoto Y (2020) How to dissect the liver parenchyma: excavation with cavitron ultrasonic surgical aspirator. J Hepatobiliary Pancreat Sci 27:907–912
Ome Y, Honda G, Kawamoto Y (2020) Laparoscopic left hepatectomy by the Arantius-first approach: a video case report. J Gastrointest Surg 24:2180–2182
Honda G, Kurata M, Okuda Y, Kobayashi S, Tadano S, Yamaguchi T, Matsumoto H, Nakano D, Takahashi K (2013) Totally laparoscopic hepatectomy exposing the major vessels. J Hepatobiliary Pancreat Sci 20:435–440
Valdis M, Chu MW, Schlachta C, Kiaii B (2016) Evaluation of robotic cardiac surgery simulation training: a randomized controlled trial. J Thorac Cardiovasc Surg 151:1498–1505
Daly MK, Gonzalez E, Siracuse-Lee D, Legutko PA (2013) Efficacy of surgical simulator training versus traditional wet-lab training on operating room performance of ophthalmology residents during the capsulorhexis in cataract surgery. J Cataract Refract Surg 39:1734–1741
Huri G, Gülşen MR, Karmış EB, Karagüven D (2021) Cadaver versus simulator based arthroscopic training in shoulder surgery. Turk J Med Sci 51:1179–1190
Drosdeck J, Carraro E, Arnold M, Perry K, Harzman A, Nagel R, Sinclair L, Muscarella P (2013) Porcine wet lab improves surgical skills in third year medical students. J Surg Res 184:19–25
Machado MA, Galvão FH, Pompeu E, Ribeiro C, Bacchella T, Machado MC (2004) A canine model of laparoscopic segmental liver resection. J Laparoendosc Adv Surg Tech A 14:325–328
Cherqui D, Emond JC, Pietrabissa A, Michel M, Roncella M, Brown SB, Whitington PF, Broelsch CE (1990) Segmental liver transplantation from living donors. Report of the technique and preliminary results in dogs. HPB Surg 2:189–204
Gutt CN, Riemer V, Brier C, Berguer R, Paolucci V (1998) Standardized technique of laparoscopic surgery in the rat. Dig Surg 5:135–139
Teh SH, Hunter JG, Sheppard BC (2007) A suitable animal model for laparoscopic hepatic resection training. Surg Endosc 21:1738–1744
White SA, Satchidanand RY, French JJ, Tait IZ, Manas DM (2014) A cadaver lab training facility to facilitate laparoscopic liver resection. Surg Laparosc Endosc Percutan Tech 24:357–360
Rashidian N, Willaert W, Giglio MC, Scuderi V, Tozzi F, Vanlander A, D’Herde K, Alseidi A, Troisi RI (2019) Laparoscopic liver surgery training course on thiel-embalmed human cadavers: program evaluation, trainer’s long-term feedback and steps forward. World J Surg 43:2902–2908
Papadopoulos D, Siempis T, Theodorakou E, Tsoulfas G (2013) Hepatic ischemia and reperfusion injury and trauma: current concepts. Arch Trauma Res 2:63–70
Weigand K, Brost S, Steinebrunner N, Büchler M, Schemmer P, Müller M (2012) Ischemia/Reperfusion injury in liver surgery and transplantation: pathophysiology. HPB Surg 2012:176723
Kobayashi S, Honda G, Kurata M, Tadano S, Sakamoto K, Okuda Y, Abe K (2016) An experimental study on the relationship among airway pressure, pneumoperitoneum pressure, and central venous pressure in pure laparoscopic hepatectomy. Ann Surg 263:1159–1163
Acknowledgements
None.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Goro Honda reports receiving lecture fees from Johnson and Johnson, Medtronic, and Integra Japan. Yusuke Kawamoto and Yusuke Ome report receiving lecture fees from Integra Japan. Yutaro Matsunaga, Shuichiro Uemura, Naoki Yoshida, Yoshihito Kotera, and Shunichi Ariizumi have no conflicts of interest or financial ties.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 62048 KB)—Supplemental Digital Content 1 Encircling of the hepatoduodenal ligament
Supplementary file2 (MP4 203917 KB)—Supplemental Digital Content 2 Laparoscopic left hepatectomy in a goat
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kawamoto, Y., Honda, G., Ome, Y. et al. Laparoscopic left hepatectomy in a goat as a training model for laparoscopic anatomic liver resection: results of training courses with a total of 70 goats. Surg Endosc 37, 3634–3641 (2023). https://doi.org/10.1007/s00464-023-09864-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-09864-4