Abstract
Background
Pancreatoduodenectomy (PD) and total pancreatectomy (TP) are two surgical methods to treat patients with pancreatic head adenocarcinoma (PHAC). However, the oncologic outcomes of TP for PHAC remain controversial. In this study, we compared early mortality and long-term survival patients undergoing TP and those with PD.
Methods
All patients diagnosed with non-metastatic PHAC who underwent PD or TP from 1988 to 2016 were retrieved from the Surveillance, Epidemiology, and End Results database. Propensity score matching (PSM) was used to balance the inter-group covariates. Cancer-specific survival (CSS) was the primary endpoint.
Results
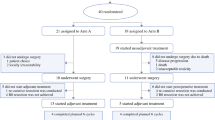
A total of 4748 patients (743 TP and 4005 PD) were included in the study. Some 740 patients who underwent TP were matched with 1479 who had PD. After PSM, there was no difference between TP and PD groups regarding 30-day mortality (3.5% vs. 2.7%, p = 0.290) and 90-day mortality (9.9% vs. 8%, p = 0.135). More importantly, TP showed comparable survival in comparison to PD, prior or after excluding patients who died within 30 and 90 days. Besides, multivariate analysis revealed that tumor size, tumor stage, N stage, chemotherapy, and radiation were significant prognostic factors.
Conclusion
PD and TP have similar early mortality and long-term survival for patients with PHAC. In selected patients, TP can be used when oncologically appropriate.
Graphical abstract





Similar content being viewed by others
References
Siegel RL, Miller KD, Fuchs HE et al (2021) Cancer statistics, 2021. CA Cancer J Clin 71:7–33
Sener SF, Fremgen A, Menck HR et al (1999) Pancreatic cancer: a report of treatment and survival trends for 100,313 patients diagnosed from 1985–1995, using the National Cancer Database. J Am Coll Surg 189:1–7
Conlon KC, Klimstra DS, Brennan MF (1996) Long-term survival after curative resection for pancreatic ductal adenocarcinoma. clinicopathologic analysis of 5-year survivors. Ann Surg 223:273–279
Mayo SC, Nathan H, Cameron JL et al (2012) Conditional survival in patients with pancreatic ductal adenocarcinoma resected with curative intent. Cancer 118:2674–2681
Satoi S, Murakami Y, Motoi F et al (2016) Reappraisal of total pancreatectomy in 45 patients with pancreatic ductal adenocarcinoma in the modern era using matched-pairs analysis: multicenter study group of pancreatobiliary surgery in Japan. Pancreas 45:1003–1009
Reddy S, Wolfgang CL, Cameron JL et al (2009) Total pancreatectomy for pancreatic adenocarcinoma: evaluation of morbidity and long-term survival. Ann Surg 250:282–287
Stoop TF, Ateeb Z, Ghorbani P et al (2021) Surgical outcomes after total pancreatectomy: a high-volume center experience. Ann Surg Oncol 28:1543–1551
Schmidt CM, Glant J, Winter JM et al (2007) Total pancreatectomy (R0 resection) improves survival over subtotal pancreatectomy in isolated neck margin positive pancreatic adenocarcinoma. Surgery 142:572–578
Simons JP, Shah SA, Ng SC et al (2009) National complication rates after pancreatectomy: beyond mere mortality. J Gastrointest Surg 13:1798–1805
Bhayani NH, Miller JL, Ortenzi G et al (2014) Perioperative outcomes of pancreaticoduodenectomy compared to total pancreatectomy for neoplasia. J Gastrointest Surg 18:549–554
Karpoff HM, Klimstra DS, Brennan MF et al (2001) Results of total pancreatectomy for adenocarcinoma of the pancreas. Arch Surg 136:44–47
Müller MW, Friess H, Kleeff J et al (2007) Is there still a role for total pancreatectomy? Ann Surg 246:966–974
Scholten L, Latenstein AEJ, van Eijck C et al (2019) Outcome and long-term quality of life after total pancreatectomy (PANORAMA): a nationwide cohort study. Surgery 166:1017–1026
Stoop TF, Ateeb Z, Ghorbani P et al (2020) Impact of endocrine and exocrine insufficiency on quality of life after total pancreatectomy. Ann Surg Oncol 27:587–596
Hartwig W, Gluth A, Hinz U et al (2015) Total pancreatectomy for primary pancreatic neoplasms: renaissance of an unpopular operation. Ann Surg 261:537–546
Pulvirenti A, Pea A, Rezaee N et al (2019) Perioperative outcomes and long-term quality of life after total pancreatectomy. Br J Surg 106:1819–1828
Billings BJ, Christein JD, Harmsen WS et al (2005) Quality-of-life after total pancreatectomy: is it really that bad on long-term follow-up? J Gastrointest Surg 9:1059–1066
Epelboym I, Winner M, DiNorcia J et al (2014) Quality of life in patients after total pancreatectomy is comparable with quality of life in patients who undergo a partial pancreatic resection. J Surg Res 187:189–196
Xiong J, Wei A, Ke N et al (2017) A case-matched comparison study of total pancreatectomy versus pancreaticoduodenectomy for patients with pancreatic ductal adenocarcinoma. Int J Surg 48:134–141
Govindarajan A, Tan JC, Baxter NN et al (2008) Variations in surgical treatment and outcomes of patients with pancreatic cancer: a population-based study. Ann Surg Oncol 15:175–185
Nathan H, Wolfgang CL, Edil BH et al (2009) Peri-operative mortality and long-term survival after total pancreatectomy for pancreatic adenocarcinoma: a population-based perspective. J Surg Oncol 99:87–92
Little RJ, Rubin DB (2000) Causal effects in clinical and epidemiological studies via potential outcomes: concepts and analytical approaches. Annu Rev Public Health 21:121–145
Austin PC (2008) A critical appraisal of propensity-score matching in the medical literature between 1996 and 2003. Stat Med 27:2037–2049
Rockey EW (1943) Total pancreatectomy for carcinoma: case report. Ann Surg 118:603–611
Tattersall RB (1997) Brittle diabetes revisited: the Third Arnold Bloom Memorial Lecture. Diabet Med 14:99–110
Coco D, Leanza S, Guerra F (2019) Total pancreatectomy: indications, advantages and disadvantages-a review. Maedica (Bucur) 14:391–396
Capretti G, Donisi G, Gavazzi F et al (2021) Total pancreatectomy as alternative to pancreatico-jejunal anastomosis in patients with high fistula risk score: the choice of the fearful or of the wise? Langenbecks Arch Surg 406:713–719
Marchegiani G, Perri G, Burelli A et al (2021) High-risk pancreatic anastomosis vs. total pancreatectomy after pancreatoduodenectomy: postoperative outcomes and quality of life analysis. Ann Surg. https://doi.org/10.1097/SLA.0000000000004840
Paik KY, Chung JC (2021) Reappraisal of clinical indication regarding total pancreatectomy: can we do it for the risky gland? Langenbecks Arch Surg. https://doi.org/10.1007/s00423-021-02208-7
Almond M, Roberts KJ, Hodson J et al (2015) Changing indications for a total pancreatectomy: perspectives over a quarter of a century. HPB (Oxford) 17:416–421
Johnston WC, Hoen HM, Cassera MA et al (2016) Total pancreatectomy for pancreatic ductal adenocarcinoma: review of the National Cancer Data Base. HPB (Oxford) 18:21–28
Schnelldorfer T, Ware AL, Sarr MG et al (2008) Long-term survival after pancreatoduodenectomy for pancreatic adenocarcinoma: is cure possible? Ann Surg 247:456–462
Hashimoto D, Mizuma M, Kumamaru H et al (2020) Risk model for severe postoperative complications after total pancreatectomy based on a nationwide clinical database. Br J Surg 107:734–742
Latenstein AEJ, Mackay TM, Beane JD et al (2021) The use and clinical outcome of total pancreatectomy in the United States, Germany, the Netherlands, and Sweden. Surgery 170:563–570
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Jisheng Zhu, Zhengying Jiang, Bin Xie, Chengchao Fu, Weidong Xiao, and Yong Li have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhu, J., Jiang, Z., Xie, B. et al. Comparison of oncologic outcomes between pancreaticoduodenectomy and total pancreatectomy for pancreatic adenocarcinoma. Surg Endosc 37, 109–119 (2023). https://doi.org/10.1007/s00464-022-09441-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09441-1