Abstract
Background
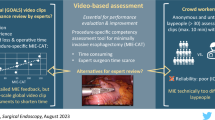
Previous studies of video-based operative assessments using crowd sourcing have established the efficacy of non-expert evaluations. Our group sought to establish the equivalence of abbreviating video content for operative assessment.
Methods
A single institution video repository of six core general surgery operations was submitted for evaluation. Each core surgery included three unique surgical performances, totaling 18 unique operative videos. Each video was edited using four different protocols based on the critical portion of the operation: (1) custom edited critical portion (2) condensed critical portion (3) first 20 s of every minute of the critical portion, and (4) first 10 s of every minute of the critical portion. In total, 72 individually edited operative videos were submitted to the C-SATS (Crowd-Sourced Assessment of Technical Skills) platform (C-SATS) for evaluation. Aggregate score for study protocol was compared using the Kruskal–Wallis test. A multivariable, multilevel mixed-effects model was constructed to predict total skill assessment scores.
Results
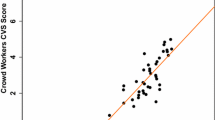
Median video lengths for each protocol were: custom, 6:20 (IQR 5:27–7:28); condensed, 10:35 (8:50–12:06); 10 s, 4:35 (2:11–6:09); and 20 s, 9:09 (4:20–12:14). There was no difference in aggregate median score among the four study protocols: custom, 15.7 (14.4–16.2); condensed, 15.8 (15.2–16.4); 10 s, 15.8 (15.3–16.1); 20 s, 16.0 (15.1–16.3); χ2 = 1.661, p = 0.65. Regression modeling demonstrated a significant, but minimal effect of the 10 s and 20 s editing protocols compared to the custom method on individual video score: condensed, + 0.33 (− 0.05–0.70), p = 0.09; 10 s, + 0.29 (0.04–0.55), p = 0.03; 20 s, + 0.40 (0.15–0.66), p = 0.002.
Conclusion
A standardized protocol for video editing abbreviated surgical performances yields reproducible assessment of surgical aptitude when assessed by non-experts.

Representation of varying edited formats of video submission of the four separate study protocols (VM1 Lap Chole 19:20)


Similar content being viewed by others
References
Garrett K, Kaups K (2014) The aging surgeon: when is it time to leave active practice? Bull Am Coll Surg 99:32–35
Mellinger J, Williams R, Sanfey H, Fryer J, DaRosa D, George B, Bohnen J, Schuller M, Sandhu G, Minter R, Gardner A, Scott D (2017) Teaching and assessing operative skills: from theory to practice. Curr Probl Surg 54:44–81
Bieliauskaus L, Langenecker S, Graver C, Lee H, O’Neill J, Greenfield L (2008) Cognitive changes and retirement among senior surgeons (CCRASS): Results from the CCRASS study. J Am Coll Surg 207:69–78
Deal S, Lendvay T, Haque M, Brand T, Comstock B, Warren J, Alseidi A (2016) Crowd-sourced assessment of technical skills: an opportunity for improvement in the assessment of laparoscopic surgical skills. Am J Surg 211:398–404
Scully R, Deal S, Clark M, Yang K, Wnuk G, Smink D, Fryer J, Bohnen J, Teitelbaum E, Meyerson S, Meier A, Gauger P, Reddy R, Kendrick D, Stern M, Hughes D, Chipman J, Patel J, Alseidi A, George B (2020) Concordance between expert and nonexpert ratings of condensed video-based trainee operative performance assessment. J Surg Ed 77:627–634
McQueen S, McKinnon V, Vanderbeek L, McCarthy C, Sonnadara R (2019) Video-based assessment in surgical education: a scoping review. J Surg Ed 76:1645–1654
Greenberg C, Dombrowski J, Dimick J (2016) Video-Based Surgical Coaching. JAMA Surg 151:282–283
Acknowledgements
Funding for this project was made possible through the generosity of the Virginia Mason Digestive Disease Institute Research Grant (#0920801) and the Honoraria Fund for Surgical Education.
Funding
Virginia Mason Digestive Disease Institute Grant #0920801.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Doctors Barnhill, Kaplan, Alseidi and Deal have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Barnhill, C.W., Kaplan, S.J., Alseidi, A.A. et al. A comparative analysis of video-based surgical assessment: is evaluation of the entire critical portion of the operation necessary?. Surg Endosc 36, 6719–6723 (2022). https://doi.org/10.1007/s00464-021-08945-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08945-6