Abstract
Background
Studies find similar perioperative outcomes between single-incision laparoscopic surgery (SILS) and conventional laparoscopic surgery (CLS) for colon cancer. However, few have reported long-term outcomes of SILS versus CLS. We aimed to compare long-term postoperative and oncologic outcomes as well as perioperative outcomes between SILS and CLS for colon cancer.
Methods
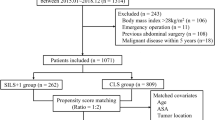
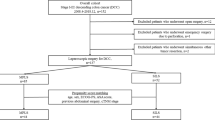
A total of 641 consecutive patients who underwent laparoscopic surgery for colon cancer from July 2009 to September 2014 were eligible for the study. Data from 300 of these patients were used for analysis after propensity score-matching (n = 150 per group). Variables associated with short- and long-term outcomes were analyzed.
Results
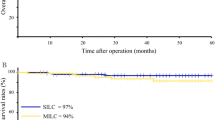
The SILS group had a shorter mean total incision length, less postoperative pain, and a similar mean rate of incisional hernia (2.7% versus 3.3%) compared with the CLS group. The 7-year overall and disease-free survival rates were 92.7% versus 94% (p = 0.673) and 85.3% versus 84.7% (p = 0.688) in the SILS and CLS groups, respectively.
Conclusions
Compared with CLS, SILS for colon cancer appeared to be safe in terms of perioperative and long-term postoperative and oncologic outcomes. The results suggested that SILS is a reasonable treatment option for colon cancer for a selected group of patients.




Similar content being viewed by others
References
Kim CW, Kim CH, Baik SH (2014) Outcomes of robotic-assisted colorectal surgery compared with laparoscopic and open surgery: a systematic review. J Gastrointest Surg 18(4):816–830
Lacy AM, Garcia-Valdecasas JC, Delgado S, Castells A, Taura P, Pique JM, Visa J (2002) Laparoscopy-assisted colectomy versus open colectomy for treatment of non-metastatic colon cancer: a randomised trial. Lancet 359(9325):2224–2229
Group TCOoSTS (2004) A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 350(20):2050–2059
Hoyuela C, Juvany M, Carvajal F (2017) Single-incision laparoscopy versus standard laparoscopy for colorectal surgery: a systematic review and meta-analysis. Am J Surg 214(1):127–140
Dong B, Luo Z, Lu J, Yang Y, Song Y, Cao J, Li W (2018) Single-incision laparoscopic versus conventional laparoscopic right colectomy: a systematic review and meta-analysis. Int J Surg 55:31–38
Bucher P, Pugin F, Morel P (2008) Single port access laparoscopic right hemicolectomy. Int J Colorectal Dis 23(10):1013–1016
Remzi FH, Kirat HT, Kaouk JH, Geisler DP (2008) Single-port laparoscopy in colorectal surgery. Colorectal Dis 10(8):823–826
Rink AD, Vestweber B, Paul C, Vestweber KH (2015) Single-incision laparoscopic surgery for colorectal malignancy–results of a matched-pair comparison to conventional surgery. Int J Colorectal Dis 30(1):79–85
Katsuno G, Fukunaga M, Nagakari K, Yoshikawa S, Azuma D, Kohama S (2016) Short-term and long-term outcomes of single-incision versus multi-incision laparoscopic resection for colorectal cancer: a propensity-score-matched analysis of 214 cases. Surg Endosc 30(4):1317–1325
Kim CW, Cho MS, Baek SJ, Hur H, Min BS, Kang J, Baik SH, Lee KY, Kim NK (2015) Oncologic outcomes of single-incision versus conventional laparoscopic anterior resection for sigmoid colon cancer: a propensity-score matching analysis. Ann Surg Oncol 22(3):924–930
Yun JA, Yun SH, Park YA, Huh JW, Cho YB, Kim HC, Lee WY (2016) Oncologic outcomes of single-incision laparoscopic surgery compared with conventional laparoscopy for colon cancer. Ann Surg 263(5):973–978
Song Z, Li Y, Liu K, Jiang Y, Shi Y, Ji X, Zhang T, Wu H, Shi Y, Zhao R (2019) Clinical and oncologic outcomes of single-incision laparoscopic surgery for right colon cancer: a propensity score matching analysis. Surg Endosc 33(4):1117–1123
Watanabe J, Ota M, Fujii S, Suwa H, Ishibe A, Endo I (2016) Randomized clinical trial of single-incision versus multiport laparoscopic colectomy. Br J Surg 103(10):1276–1281
Kang BM, Kim HJ, Kye BH, Lee SC, Lee KY, Park SJ, Lee SH, Lim SW, Lee YS, Kim JH, Lee J, Kim MK, Kim JG (2018) Multicenter, randomized single-port versus multiport laparoscopic surgery (SIMPLE) trial in colon cancer: an interim analysis. Surg Endosc 32(3):1540–1549
Maggiori L, Tuech JJ, Cotte E, Lelong B, Denost Q, Karoui M, Vicaut E, Panis Y (2018) Single-incision laparoscopy versus multiport laparoscopy for colonic surgery: a multicenter, double-blinded, randomized controlled trial. Ann Surg 268(5):740–746
Kim CW, Hur H, Min BS, Baik SH, Lee KY, Kim NK (2017) Oncologic outcomes of single-incision laparoscopic surgery for right colon cancer: a propensity score-matching analysis. Int J Surg 45:125–130
Shawki S, Bashankaev B, Denoya P, Seo C, Weiss EG, Wexner SD (2009) What is the definition of “conversion” in laparoscopic colorectal surgery? Surg Endosc 23(10):2321–2326
Kim CW, Kim WR, Kim HY, Kang J, Hur H, Min BS, Baik SH, Lee KY, Kim NK (2015) Learning curve for single-incision laparoscopic anterior resection for sigmoid colon cancer. J Am Coll Surg 221(2):397–403
Kim CW, Han YD, Kim HY, Hur H, Min BS, Lee KY, Kim NK (2016) Learning curve for single-incision laparoscopic resection of right-sided colon cancer by complete mesocolic excision. Medicine (Baltimore) 95(26):e3982
Kim CW, Lee KY, Lee SC, Lee SH, Lee YS, Lim SW, Kim JG (2017) Learning curve for single-port laparoscopic colon cancer resection: a multicenter observational study. Surg Endosc 31(4):1828–1835
Kim CW, Park YY, Hur H, Min BS, Lee KY, Kim NK (2020) Cost analysis of single-incision versus conventional laparoscopic surgery for colon cancer: a propensity score-matching analysis. Asian J Surg 43(4):557–563
Tsimoyiannis EC, Tsimogiannis KE, Pappas-Gogos G, Farantos C, Benetatos N, Mavridou P, Manataki A (2010) Different pain scores in single transumbilical incision laparoscopic cholecystectomy versus classic laparoscopic cholecystectomy: a randomized controlled trial. Surg Endosc 24(8):1842–1848
Maggiori L, Gaujoux S, Tribillon E, Bretagnol F, Panis Y (2012) Single-incision laparoscopy for colorectal resection: a systematic review and meta-analysis of more than a thousand procedures. Colorectal Dis 14(10):e643-654
Poulose BK, Shelton J, Phillips S, Moore D, Nealon W, Penson D, Beck W, Holzman MD (2012) Epidemiology and cost of ventral hernia repair: making the case for hernia research. Hernia 16(2):179–183
Sanders DL, Kingsnorth AN (2012) The modern management of incisional hernias. Bmj 344:e2843
Antoniou SA, Morales-Conde S, Antoniou GA, Granderath FA, Berrevoet F, Muysoms FE (2016) Single-incision laparoscopic surgery through the umbilicus is associated with a higher incidence of trocar-site hernia than conventional laparoscopy: a meta-analysis of randomized controlled trials. Hernia 20(1):1–10
Vestweber B, Vestweber KH, Paul C, Rink AD (2016) Single-port laparoscopic resection for diverticular disease: experiences with more than 300 consecutive patients. Surg Endosc 30(1):50–58
Kossler-Ebs JB, Grummich K, Jensen K, Huttner FJ, Muller-Stich B, Seiler CM, Knebel P, Buchler MW, Diener MK (2016) Incisional hernia rates after laparoscopic or open abdominal surgery—a systematic review and meta-analysis. World J Surg 40(10):2319–2330
Gash K, Bicsak M, Dixon A (2015) Single-incision laparoscopic surgery for rectal cancer: early results and medium-term oncological outcome. Colorectal Dis 17(12):1071–1078
Acknowledgements
This work was supported by a National Research Foundation of Korea grant funded by the Korea government Ministry of Science and ICT (No. 2020R1C1C1008212).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Chang Woo Kim, Seung Yoon Yang, and Hyuk Hur have no conflicts of interests or additional financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Meeting presentations: This work was presented as an E-poster at the 27th International Congress of the European Association of Endoscopic Surgery, June 12–15, 2019, Seville, Spain.
Rights and permissions
About this article
Cite this article
Kim, C.W., Yang, S.Y. & Hur, H. Long-term oncologic outcomes of single-incision laparoscopic surgery for colon cancer. Surg Endosc 36, 3200–3208 (2022). https://doi.org/10.1007/s00464-021-08629-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08629-1