Abstract
Background
Although isolated caudate lobe (CL) liver resection is not a contraindication for minimally invasive liver surgery (MILS), feasibility and safety of the procedure are still poorly investigated. To address this gap, we evaluate data on the Italian prospective maintained database on laparoscopic liver surgery (IgoMILS) and compare outcomes between MILS and open group.
Methods
Perioperative data of patients with malignancies, as colorectal liver metastases (CRLM), hepatocellular carcinoma (HCC), intrahepatic cholangiocarcinoma (ICC), non-colorectal liver metastases (NCRLM) and benign liver disease, were retrospectively analyzed. A propensity score matching (PSM) analysis was performed to balance the potential selection bias for MILS and open group.
Results
A total of 224 patients were included in the study, 47 and 177 patients underwent MILS and open isolated CL resection, respectively. The overall complication rate was comparable between the two groups; however, severe complication rate (Dindo–Clavien grade ≥ 3) was lower in the MILS group (0% versus 6.8%, P = ns). In-hospital mortality was 0% in both groups and mean hospital stay was significantly shorter in the MILS group (P = 0.01). After selection of 42 MILS and 43 open CL resections by PSM analysis, intraoperative and postoperative outcomes remained similar except for the hospital stay which was not significantly shorter in MILS group.
Conclusions
This multi-institutional cohort study shows that MILS CL resection is feasible and safe. The surgical procedure can be technically demanding compared to open resection, whereas good perioperative outcomes can be achieved in highly selected patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Isolated caudate lobe (CL) resection, originally described in 1990 by Lerut et al. [1], is an uncommon and technically challenging liver surgery procedure. Conversely, the association of CL resection and major hepatectomy (i.e., left or right hepatectomy) is more frequently performed.
CL is an autonomous segment which is located anterior to the inferior vena cava (IVC) and posterior to the liver hilum. Therefore, the surgical approach of this area can be technically difficult.
This segment can be divided into three regions according to Kumon et al. [2] classification: the Spiegel’s lobe, the paracaval portion and the caudate process. The Spiegel lobe is located behind the lesser omentum, on the left side of the intrahepatic IVC. The paracaval portion is located ventrally to the hepatic IVC, between the Spiegel lobe and the right lobe and below the hepatic veins. The caudate process is a projection of the liver between the IVC and the right hepatic lobe, close to the paracaval portion [3].
Minimally invasive liver surgery (MILS) largely increased after the first international consensus conference in Louisville in 2008 [4, 5] and it is nowadays the standard procedure for anteroinferior segments. MILS for posterior and superior segments is technically more challenging and is reserved to experienced surgeons in tertiary centers [6].
The safety and feasibility of MILS have been widely described, demonstrating shorter hospital stay, lower blood loss with comparable oncological outcomes when compared with the open approach.
MILS approaches to the CL have specific technical challenges: proximity to the IVC, major hepatic veins and the hepatic hilum [7]. Surgical series of MILS for the caudate lobe in the literature are limited and only a few reports describing more than 5 cases have been published [5, 8,9,10,11,12,13,14,15,16].
The aim of our study was to evaluate the safety and feasibility of MILS for caudate lobe resections in the Italian prospective maintained database on laparoscopic liver surgery (IgoMILS) through comparison with a cohort of patients submitted to open CL resection.
Patients and methods
Patients who underwent MILS CL resection from March 2015 to December 2018 were identified from the IgoMILS registry, a prospective multi-institutional Italian database of patients undergoing laparoscopic liver resections. Specifically, data from 16 centers that performed at least 1 laparoscopic isolated CL resection were collected. Each center performed a variable number (1–13 cases) of MILS CL resections. Characteristics of the IgoMILS registry have been published previously [17]. In short, it is a prospective intention-to-treat registry open to any Italian center performing MILS, without restriction criteria based on number of procedures performed. The registry has been developed through eClinical, an electronic platform for the management of clinical trials. Any center willing to register patients in the registry was given access through the web page, https://www.cr-technology.com/igomils/.
Encryption data for identification of patients were held by the centers. Ethical approval for the registry was granted by the Ethics Committee of San Raffaele Hospital, Milan. The informed consent and study documents were evaluated and approved by the center where the subject was enrolled. Investigators belonging to the IgoMILS association undertake data auditing periodically. An external audit was performed in April 2018 to check the quality and reliability of the data. A random sample of 10% of patients enrolled in each center was selected. The registered data for each patient were verified; data accuracy was 96% and was similar in all centers.
Perioperative data of patients who underwent open isolated CL resection from November 2000 to December 2018 in the same surgical centers of the IgoMILS registry were also included in the study.
Our study population included both patients with malignancies, such as colorectal liver metastases (CRLM), hepatocellular carcinoma (HCC), intrahepatic cholangiocarcinoma (ICC), non-colorectal liver metastases (NCRLM) and benign liver disease.
The following preoperative data were collected for each patient: demographics, comorbidities, liver parenchyma characteristics, indication for resection and previous surgery. Operative details included the type of caudate lobe liver resection, the rate of conversion to open surgery, the use and type of pedicle clamping, surgical radicality, associated resections (hepatic or of other organs), intraoperative blood transfusions and blood losses. Early results included overall and severe complications, in-hospital mortality, postoperative blood transfusions, and length of stay. Pathological reports were available for all specimens. R0 resection was defined as a tumor-free surgical margin greater than 1 mm.
Caudate lobe anatomy was defined according to Kumon’s classification; for data collection and analysis we defined two different types of caudate lobe resection: isolated Spiegel’s lobe resection (S1-S) or combined resection of Spiegel’s lobe with paracaval portion and complete/partial resection of caudate process (S1-S + P).
Patients who underwent major liver resection with en-bloc CL resection or CL resection en-bloc with other hepatectomies were excluded from the study.
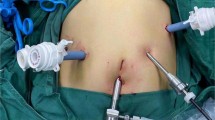
Figure 1 illustrates a surgical case of isolated MILS caudate lobe resection for HCC.
Morbidity included all postoperative complications and was graded according to the Clavien–Dindo classification, and complications of grade 3 or higher were defined as severe complications [18]. Cumulative morbidity was measured using the Comprehensive Complication Index (CCI) [19].
Statistical analysis
Categorical variables were compared using the χ2 test, Fisher’s exact test or Pearson’s test, as appropriate. The Student t test or 1-way ANOVA was used for continuous variables where appropriate. The results were expressed as mean and standard deviation (SD) or median and range.
To account for potential residual confounders regarding the effect of surgical approach on outcomes, propensity scores were estimated using a logistic regression model with the type of surgical approach as a dependent variable specified as MILS versus Open approach. Tumor size, liver histology, type of surgical procedure and tumor histology were independent variables in the logistic regression model. An exact propensity-score value was used for matching. The degrees of covariate imbalance were measured using the standardized (mean and proportion) differences, as proposed by Austin et al. [20]. A P value of < 0.05 (two-tailed) was considered statistically significant. All statistical analyses were performed with SPSS® version 25 (IBM) and XLSTAT (Addinsoft).
Results
A total of 224 patients were included in the study, 47 (21%) patients underwent MILS and 177 (79%) patients underwent open approach.
The two groups were similar for demographic characteristics, but HBV infection rate was higher in the MILS group than in the open group (P = 0.034). Moreover, liver cirrhosis and fibrosis were more frequent in the MILS group than in the open group (P < 0.001). Regarding histological diagnosis, the frequency of benign disease was similar between the two groups. On the contrary, in the open group more CRLM were observed and in the MILS group more HCC were observed (P = 0.020). Demographic and preoperative characteristics of the two groups are reported in Table 1.
Limited Spiegel’s lobe resections in the MILS and open group were 63.8% (30 patients) and 48.6% (86 patients), respectively. Instead, resection rate of Spiegel’s lobe extended at the paracaval portion and complete/partial resections of caudate process were 31.9% (15 patients) in the MILS group and 51.4% (85 patients) in the open group.
Pringle maneuver was performed in 29.8% (n = 14) of patients in the MILS group and 67.0% (n = 118) of patients in the open group (P < 0.001). Of note, the conversion rate from MILS approach to open surgery was 6.4% (n = 3) because of bleeding (1 case), intraperitoneal adhesions (1 case) and oncological radicality (1 case).
Mean intraoperative blood loss was lower in the MILS group compared to the open group (P < 0.001). No case of the MILS group required intraoperative blood transfusions, while 17 (10.0%) patients in the open group were transfused intraoperatively (P = 0.013). The use of abdominal drainage was less frequent in the MILS group than in the open group (P < 0.001).
Mean operation time in the MILS and open group was 309 min and 235 min, respectively (P = 0.001).
MILS and open group had similar mean size of the lesions and rate of positive resection margins for malignant tumors.
Overall complication rate was comparable between the two groups, but severe complication rate (Dindo–Clavien grade ≥ 3) was higher in the open group (6.8%, n = 12) compared to the MILS group (0%). Nevertheless, this difference was not statistically significant. On the contrary, mean CCI was 13.7 (SD ± 6.1) in the MILS group and 23.4 (SD ± 11.4) in the open group (P = 0.03). MILS group had a significantly shorter hospital stay (P = 0.01) and there were no in-hospital mortality in both groups. Intraoperative and postoperative data of both groups are summarized in Table 2.
To balance the potential selection bias, a PSM analysis was performed selecting 42 patients in the MILS and 43 patients in the open group. After the PSM analysis, demographics and preoperative data did not show significant differences between the two groups except for arterial hypertension that was more frequent in the MILS group (P = 0.03) (Table 1).
Most of the intraoperative and postoperative data also did not show significant differences (Table 2). However, MILS compared to open group had lower mean intraoperative blood losses [173 mL (SD ± 154 mL) versus 290 mL (SD ± 186 mL), P = 0.003], reduced use of abdominal drainage (71.4% vs 97.7%, P = 0.001), longer mean operation time (298 min vs 238 min, P = 0.038) and lower CCI [13.3 (SD ± 6.0) vs 19.8 (SD ± 6.3), P = 0.006].
Subgroup analysis according to S1 type of resection
A subgroup analysis based on the type of surgical procedure in the MILS and open group was performed. In particular, we analyzed perioperative data of resections limited to Spiegel lobe (S1-S) and extended to the paracaval portion and complete/partial resection of caudate process (S1-S + P). Intraoperative and postoperative data of the subgroup analysis are reported in Table 3.
Among the intraoperative variables, the MILS group showed lower blood loss compared to the open group for both S1-S (197.7 mL vs 346.2 mL, P = 0.014) and S1-S + P (134 mL vs 340 mL, P = n.s). Instead, mean operation time was significantly longer in the MILS group compared to the open group for S1-S (294 min vs 240 min, P = 0.044) and S1-S + P (327 min vs 216 min, P = 0.003). Other postoperative variables, such as rate and severity of surgical complications and length of hospital stay, were comparable between the MILS and open group in both S1-S and S1-S + P.
Discussion
In the last decades, MILS steadily increased. The spreading of MILS approach is supported by the improvements of surgical techniques, the implementation of new surgical tools and the growing MILS hepatobiliary surgeon’s skills that contribute to face more complex MILS procedures [21].
CL resection is a minor but complex surgical intervention, even with an open approach, due to its location deep into the liver. Anatomically, caudate lobe can be classified into three different parts: the Spiegel’s lobe that is located on the left side of the IVC, the paracaval portion in front of the IVC and the caudate process on the right side of the IVC [2].
Although the Spigelian lobe is relatively easy to manage, the resection of the caudate process and paracaval portion may be very demanding due to the relationship with the hepato-caval confluence, the main biliary ducts and the main portal vein bifurcation. MILS CL resection is a double-edged sword; indeed, MILS could improve short-term outcomes decreasing postoperative pain and shortening in-hospital stay, but is also true that surgeon should be aware of the potential intraoperative life-threatening massive bleeding caused by injury of IVC [22, 23].
In our experience, the main advantages of MILS are the magnification of surgical field that is very helpful during the dissection of small CL collaterals coming from IVC and the caudal view of segment 1 [26, 27]. Moreover, the balance between intra-abdominal pressure and central venous pressure can reduce venous bleeding (Fig. 1).
A surgical case of isolated MILS caudate lobe resection for HCC. Surgical case of isolated caudate lobe resection for 3 cm HCC (A), patient was positioned in French position with operating surgeon standing between patients’ legs, the scheme illustrating the position of the of trocars (B). Mobilization of caudate lobe from inferior vena cava, short hepatic veins secured with clips (C). Liver transection with ultrasonic aspirator (D)
From a technical point of view, three approaches to the caudate lobe have been described: from the left side, from the right side and trans-parenchymal [28, 29]. The most common approach for the Spiegel’s lobe is from the left side because it exposes the anterior surface of IVC. Right side approach is more commonly used for lesions of the paracaval portion or the caudate process. The trans-parenchymal approach is more suitable for larger lesions but is rarely applied for its complexity also in open approach [30].
The oncological safety of CL resection can be a matter of debate since the size and location of the tumor and its relationship with major hilar structures and IVC may affect the ability to achieve negative resection margins.
Our multi-institutional study confirmed the feasibility and safety of MILS CL resection and showed that MILS approach had lower intraoperative blood loss, lower severe postoperative complication rate and shorter hospital stay compare to open approach. Furthermore, the MILS and open group had similar good oncologic outcomes in terms of negative resection margin rate.
Our conversion rate of 6.4% (n = 3) is comparable to other series reported in the literature. The reasons for the conversion to open surgery were major bleeding, the need to achieve oncological radicality and strong adhesions. No massive intraoperative bleedings and in-hospital mortality were observed.
The complexity of the surgical procedures of CL resection varies depending on the portions to be resected. In particular, the resection of the paracaval portion and/or caudate process is more challenging than isolated Spiegel’s lobe resection. In order to clearly elucidate the short-term outcomes of open and laparoscopic surgery of S1-S and S1-S-P resection, we performed a subgroup analysis. Limited S1-S resection by MILS approach showed lower blood loss, but longer operative time compared to open approach. Instead, in more complex operation, as S1-S-P resection, we found that only mean operative time was significantly longer by MILS approach. Current literature is very limited about this topic. Wang et al. [24] reported that patients who underwent open caudate lobectomy for tumors located at the paracaval portion or the caudate process had longer operative time, vascular occlusion time, hospital stay and higher blood loss compared to Spiegel’s lobe resection. Conversely, Zhao et al. [25] described similar short-term outcomes in patients submitted to different types of robotic-assisted CL resections (Spiegel’s lobe, paracaval portion and/or caudate process).
Few articles concerning the laparoscopic approach to CL are published in literature. Moreover, the majority of these studies are limited to case reports or small surgical series [5, 8,9,10,11,12,13,14,15,16]. Table 4 provides a literature review and demonstrates that morbidity rate of MILS CL resections ranged from 0 to 33% with no postoperative mortality.
Only a few studies aimed to assess robotic approach to CL. One series of 10 cases describes the safety and feasibility of the robotic approach emphasizing the importance of the fully wristed dexterity, ergonomics and the full 3D vision [31]. Nevertheless, the authors reported equivalent short-term results with the laparoscopic approach, but with lower costs and shorter operative time. In our study, only 1 patient was treated with robotic approach.
The only comparative study between MILS and open approach was presented by Xu et al.[9] and demonstrated the benefits of the laparoscopic technique in reducing blood loss and transfusion rate. The reported morbidity and severe complication rate was similar to our study. In addition, the authors demonstrated a shorter time for ambulation, oral intake, first flatus and drainage tube removal in the MILS group [32, 33].
The present study has several limitations that should be considered. Despite the IgoMILS registry enrolls patients prospectively from several Italian centers, this is a retrospective study with a limited number of patients in the MILS group. Besides, we included lesions with different histologies. The PSM analysis was performed to mitigate the risk of selection bias; however, further studies are expected. Finally, MILS has been recently developed and the experience with difficult liver segments is improving. Therefore, short- and long-term outcomes should be reassessed in the future.
Conclusions
This multi-institutional cohort study shows that MILS CL resection is feasible and safe. The surgical procedure can be technically demanding compared to open resection, whereas good perioperative outcomes can be achieved in selected cases.
References
Lerut J, Gruwez JA, Blumgart LH (1990) Resection of the caudate lobe of the liver. Surg Gynecol Obstet 171:160–162
Kumon M (2017) Anatomical study of the caudate lobe with special reference to portal venous and biliary branches using corrosion liver casts and clinical application. Liver Cancer 6:161–170. https://doi.org/10.1159/000454682
Murakami G, Hata F (2002) Human liver caudate lobe and liver segment. Anat Sci Int 77:211–224. https://doi.org/10.1046/j.0022-7722.2002.00033.x
Buell JF, Cherqui D, Geller DA, O’Rourke N, Iannitti D, Dagher I, Koffron AJ, Thomas M, Gayet B, Han HS, Wakabayashi G, Belli G, Kaneko H, Ker C-G, Scatton O, Laurent A, Abdalla EK, Chaudhury P, Dutson E, Gamblin C, D’Angelica M, Nagorney D, Testa G, Labow D, Manas D, Poon RT, Nelson H, Martin R, Clary B, Pinson WC, Martinie J, Vauthey J-N, Goldstein R, Roayaie S, Barlet D, Espat J, Abecassis M, Rees M, Fong Y, McMasters KM, Broelsch C, Busuttil R, Belghiti J, Strasberg S, Chari RS (2009) The international position on laparoscopic liver surgery: the Louisville Statement, 2008. Ann Surg 250:825–830. https://doi.org/10.1097/sla.0b013e3181b3b2d8
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection—2,804 patients. Ann Surg 250(5):831–841
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, O’Rourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CHD, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen K-H, Schön MR, Sugioka A, Tang C-N, Herman P, Pekolj J, Chen X-P, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo C-M, Clavien P-A, Kokudo N, Barkun J, Strasberg SM (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629. https://doi.org/10.1097/SLA.0000000000001184
Kosuge T, Yamamoto J, Takayama T, Shimada K, Yamasaki S, Makuuchi M, Hasegawa H (1994) An isolated, complete resection of the caudate lobe, including the paracaval portion, for hepatocellular carcinoma. Arch Surg 129:280–284. https://doi.org/10.1001/archsurg.1994.01420270056013
Cappelle M, Aghayan DL, van der Poel MJ, Besselink MG, Sergeant G, Edwin B, Parmentier I, De Meyere C, Vansteenkiste F, D’Hondt M (2020) A multicenter cohort analysis of laparoscopic hepatic caudate lobe resection. Langenbeck’s Arch Surg. https://doi.org/10.1007/s00423-020-01867-2
Xu G, Tong J, Ji J, Wang H, Wu X, Jin B, Xu H, Lu X, Sang X, Mao Y, Du S, Hong Z (2020) Laparoscopic caudate lobectomy: a multicenter, propensity score-matched report of safety, feasibility, and early outcomes. Surg Endosc. https://doi.org/10.1007/s00464-020-07478-8
Koffron AJ, Auffenberg G, Kung R, Abecassis M (2007) Evaluation of 300 minimally invasive liver resections at a single institution: less is more. Ann Surg 246:384–385. https://doi.org/10.1097/SLA.0b013e318146996c
Chen K-H, Jeng K-S, Huang S-H, Chu S-H (2013) Laparoscopic caudate hepatectomy for cancer—An innovative approach to the no-man’s land. J Gastrointest Surg 17:522–526. https://doi.org/10.1007/s11605-012-2115-z
Araki K, Fuks D, Nomi T, Ogiso S, Lozano RR, Kuwano H, Gayet B (2016) Feasibility of laparoscopic liver resection for caudate lobe: technical strategy and comparative analysis with anteroinferior and posterosuperior segments. Surg Endosc 30:4300–4306. https://doi.org/10.1007/s00464-016-4747-7
Ho K-M, Han H-S, Yoon Y-S, Cho JY, Choi YR, Jang JS, Kwon SU, Kim S, Choi JK (2017) Laparoscopic total caudate lobectomy for hepatocellular carcinoma. J Laparoendosc Adv Surg Tech A 27:1074–1078. https://doi.org/10.1089/lap.2016.0459
Salloum C, Lahat E, Lim C, Doussot A, Osseis M, Compagnon P, Azoulay D (2016) Laparoscopic isolated resection of caudate lobe (segment 1): a safe and versatile technique. J Am Coll Surg. https://doi.org/10.1016/j.jamcollsurg.2016.01.047
Chai S, Zhao J, Zhang Y, Xiang S, Zhang W (2018) Arantius ligament suspension: a novel technique for retraction of the left lateral lobe liver during laparoscopic isolated caudate lobectomy. J Laparoendosc Adv Surg Tech A 28:740–744. https://doi.org/10.1089/lap.2017.0572
Jin B, Jiang Z, Hu S, Du G, Shi B, Kong D, Yang J (2018) Surgical technique and clinical analysis of twelve cases of isolated laparoscopic resection of the hepatic caudate lobe. Biomed Res Int. https://doi.org/10.1155/2018/5848309
Aldrighetti L, Ratti F, Cillo U, Ferrero A, Ettorre GM, Guglielmi A, Giuliante F, Calise F, Dalla Valle R, Mazzaferro V, Jovine E, De Carlis LG, Boggi U, Gruttadauria S, Di Benedetto F, Reggiani P, Berti S, Ceccarelli G, Vincenti L, Belli G, Torzilli G, Zamboni F, Coratti A, Mezzatesta P, Santambrogio R, Navarra G, Giuliani A, Pinna AD, Parisi A, Colledan M, Slim A, Antonucci A, Grazi GL, Frena A, Sgroi G, Brolese A, Morelli L, Floridi A, Patriti A, Veneroni L, Ercolani G, Boni L, Maida P, Griseri G, Percivale A, Filauro M, Guerriero S, Tisone G, Romito R, Tedeschi U, Zimmitti G, MILS) O behalf of the IG of MILS (I GO (2017) Diffusion, outcomes and implementation of minimally invasive liver surgery: a snapshot from the I Go MILS (Italian Group of Minimally Invasive Liver Surgery) Registry. Updates Surg 69:271–283. https://doi.org/10.1007/s13304-017-0489-x
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications. Ann Surg 240:205–213. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Slankamenac K, Graf R, Barkun J, Puhan MA, Clavien P-A (2013) The comprehensive complication index: a novel continuous scale to measure surgical morbidity. Ann Surg 258:1–7. https://doi.org/10.1097/SLA.0b013e318296c732
Austin PC (2009) Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med 28:3083–3107. https://doi.org/10.1002/sim.3697
Wabitsch S, Kästner A, Haber PK, Feldbrügge L, Winklmann T, Werner S, Pratschke J, Schmelzle M (2019) Laparoscopic versus open hemihepatectomy—A cost analysis after propensity score matching. Langenbeck’s Arch Surg 404:469–475. https://doi.org/10.1007/s00423-019-01790-1
Rowe AJ, Meneghetti AT, Schumacher PA, Buczkowski AK, Scudamore CH, Panton ONM, Chung SW (2009) Perioperative analysis of laparoscopic versus open liver resection. Surg Endosc 23:1198–1203. https://doi.org/10.1007/s00464-009-0372-z
Tsinberg M, Tellioglu G, Simpfendorfer C, Walsh R, Walsh M, Vogt D, Fung J, Berber E (2009) Comparison of laparoscopic versus open liver tumor resection: a case-controlled study. Surg Endosc 23:847–853. https://doi.org/10.1007/s00464-008-0262-9
Wang Y, Zhang LY, Yuan L, Sun FY, Wei TG (2010) Isolated caudate lobe resection for hepatic tumor: surgical approaches and perioperative outcomes. Am J Surg 200:346–351. https://doi.org/10.1016/j.amjsurg.2009.10.018
Zhao ZM, Yin ZZ, Pan LC, Hu MG, Tan XL, Liu R (2020) Robotic isolated partial and complete hepatic caudate lobectomy: a single institution experience. Hepatobiliary Pancreat Dis Int 19:435–439. https://doi.org/10.1016/j.hbpd.2020.05.003
Soubrane O, Schwarz L, Cauchy F, Perotto LO, Brustia R, Bernard D, Scatton O (2015) A conceptual technique for laparoscopic right hepatectomy based on facts and oncologic principles: the caudal approach. Ann Surg 261:1226–1231. https://doi.org/10.1097/SLA.0000000000000737
Ogiso S, Nomi T, Araki K, Conrad C, Hatano E, Uemoto S, Fuks D, Gayet B (2015) Laparoscopy-specific surgical concepts for hepatectomy based on the laparoscopic caudal view: a key to reboot surgeons’ minds. Ann Surg Oncol 22(Suppl 3):S327–S333. https://doi.org/10.1245/s10434-015-4661-6
Chaib E, Ribeiro MAF, de Silva SCF, Saad WA, Cecconello I (2008) Caudate lobectomy: tumor location, topographic classification, and technique using right- and left-sided approaches to the liver. Am J Surg 196:245–251. https://doi.org/10.1016/j.amjsurg.2007.11.020
Sasada A, Ataka K, Tsuchiya K, Yamagishi H, Maeda H, Okada M (1998) Complete caudate lobectomy: its definition, indications, and surgical approaches. HPB Surg 11:85–87. https://doi.org/10.1155/1998/92312
Asahara T, Dohi K, Hino H, Nakahara H, Katayama K, Itamoto T, Ono E, Moriwaki K, Yuge O, Nakanishi T, Kitamoto M (1998) Isolated caudate lobectomy by anterior approach for hepatocellular carcinoma originating in the paracaval portion of the caudate lobe. J Hepatobiliary Pancreat Surg 5:416–421. https://doi.org/10.1007/s005340050066
Marino MV, Glagolieva A, Guarrasi D (2018) Robotic resection of the liver caudate lobe: technical description and initial consideration. Circ Esp 96:162–168. https://doi.org/10.1016/j.ciresp.2018.01.001
Polignano FM, Quyn AJ, de Figueiredo RSM, Henderson NA, Kulli C, Tait IS (2008) Laparoscopic versus open liver segmentectomy: prospective, case-matched, intention-to-treat analysis of clinical outcomes and cost effectiveness. Surg Endosc 22:2564–2570. https://doi.org/10.1007/s00464-008-0110-y
Jia C, Li H, Wen N, Chen J, Wei Y, Li B (2018) Laparoscopic liver resection: a review of current indications and surgical techniques. Hepatobiliary Surg Nutr 7(277):288. https://doi.org/10.21037/hbsn.2018.03.01
Collaborators
Co-authors of this IgoMILS study are Francesca Ratti (Ospedale San Raffaele, Milan); Enrico Gringeri (Policlinico Universitario, Padua); Nadia Russolillo (Ospedale Mauriziano, Turin); Tommaso Campagnaro (AOU Integrata Verona, Verona); Simone Conci (AOU Integrata Verona, Verona); Giovanni Battista Levi Sandri (Ospedale San Camillo Forlanini, Rome); Francesco Ardito (Policlinico Gemelli, Rome); Ugo Boggi (Azienda Ospedaliero Universitaria (AOU) Pisana, Pisa); Salvatore Gruttadauria (Istituto Mediterraneo per i Trapianti e Terapie ad Alta Specializzazione, Palermo); Luca Viganò (Humanitas University, Rozzano); Fabrizio Di Benedetto (AOU Policlinico di Modena, Modena); Giogio Ettore Rossi (Ospedale Maggiore Policlinico, Milan); Stefano Berti (Ospedale Civile S. Andrea, La Spezia); Graziano Ceccarelli (Ospedale San Donato, Arezzo); Leonardo Vincenti (AOU Consorziale Policlinico, Bari); Umberto Cillo (University of Padua, Padua); Felice Giuliante (Policlinico Gemelli, Rome); Vincenzo Mazzaferro (Fondazione IRCCS Istituto Nazionale Tumori, Milan); Elio Jovine (Maggiore Hospital, Bologna); Fulvio Calise (Pinetagrande Hospital, Castelvolturno); Giulio Belli (Ospedale Santa Maria di Loreto Nuovo, Naples); Fausto Zamboni (Ospedale Brotzu, Cagliari); Andrea Coratti (AOU Careggi, Florence); Pietro Mezzatesta (Casa di Cura La Maddalena, Palermo); Roberto Santambrogio (Azienda Ospedaliera (AO) San Paolo, Milan); Giuseppe Navarra (AOU Policlinico G. Martino, Messina); Antonio Giuliani (AO R. N. Cardarelli, Naples); Fabio Ferla (ASST Grande Ospedale Metropolitano Niguarda, Milan); Antonio Domenico Pinna (Policlinico Sant’Orsola Malpighi, Bologne); Amilcare Parisi (AO Santa Maria di Terni, Terni); Michele Colledan (AO Papa Giovanni XXIII, Bergamo); Abdallah Slim (AO Desio e Vimercate, Vimercate); Adelmo Antonucci (Policlinico di Monza, Monza); Gian Luca Grazi (Istituto Nazionale Tumori Regina Elena, Rome); Antonio Frena (Ospedale Centrale, Bolzano); Giovanni Sgroi (AO Treviglio-Caravaggio, Treviglio); Alberto Brolese (Ospedale S. Chiara, Trento); Luca Morelli (AOU Pisana, Pisa); Antonio Floridi (AO Ospedale Maggiore, Crema); Alberto Patriti (Ospedale San Matteo degli Infermi, Spoleto); Luigi Veneroni (Ospedale Infermi AUSL Romagna, Rimini); Luigi Boni (AOU Fondazione Macchi, Varese); Piero Maida (Ospedale Villa Betania, Naples); Guido Griseri (Ospedale San Paolo, Savona); Marco Filauro (AO Galliera, Genoa); Silvio Guerriero (Ospedale San Martino, Belluno); Raffaele Romito (AOU Maggiore della Carità, Novara); Umberto Tedeschi (AOU Integrata Verona, Verona); Giuseppe Zimmitti (Fondazione Poliambulanza, Brescia).
Funding
Open access funding provided by Università degli Studi di Verona within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Disclosures
Doctors Andrea Ruzzenente, Andrea Ciangherotti, Luca Aldrighetti, Giuseppe Maria Ettorre, Luciano De Carlis, Alessandro Ferrero, Raffaele Dalla Valle, Giuseppe Tisone and Alfredo Guglielmi have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members of the Italian Group of Minimally Invasive Liver Surgery are co-authors of this study and can be found under the heading Collaborators.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ruzzenente, A., Ciangherotti, A., Aldrighetti, L. et al. Technical feasibility and short-term outcomes of laparoscopic isolated caudate lobe resection: an IgoMILS (Italian Group of Minimally Invasive Liver Surgery) registry-based study. Surg Endosc 36, 1490–1499 (2022). https://doi.org/10.1007/s00464-021-08434-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08434-w