Abstract
Background
In the literature, there have been scant studies that compare the effects of totally extraperitoneal (TEP) and Lichtenstein hernia (LH) repairs on men’s sexual function and quality of life. Our aim in this study was to study the sexual function of men after TEP and LH repair according to SF 36 (Health Survey Scoring Demonstration) and IIEF (The International Index of Erectile Function).
Methods
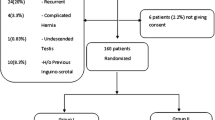
A total of 176 men with unilateral inguinal hernia were randomized into two groups. Group T (n = 88) received TEP hernia repair, and Group L (n:88) received LH repair. Patients’ demographics and perioperative findings were recorded. For all patients, the preoperative as well as postoperative 7th, 30th and 90th day SF 36 and IIEF were recorded.
Results
A total of 176 operations consisting of 88 TEP and 88 LH repairs were evaluated. There were no differences in demographics, hernia type, and complications except for body mass index (BMI). The operative time was higher in Group T (29.6 ± 5.8 vs. 43.5 ± 5.7 min; p = 0.001). The averages of the SF 36-Vitality and Social Function for Postoperative (PO) 30th day scores were higher in Group T. The averages of the SF 36-Bodily Pain, General Health, Physical Role, Emotional Role for PO 7–30th days SF36- Mental Health for PO 7th day and SF 36 Physical Function for PO 30–90th days scores were statistically higher in Group T. The averages of the IIEF- Erectile Function for PO 30th day, IIEF- Orgasmic Function, Sexual Desire, Intercourse Satisfaction, and Intercourse Satisfaction for PO 7th and 30th days scores were higher in Group T.
Conclusions
TEP and LH repairs have similar results for recurrence, complications, and hospital stay; otherwise, TEP repair yields better results than the LH repair in the postoperative course at the 7th and 30th day evaluation, concerning sexual function and quality of life, but this benefit is no longer apparent at the 90th day. Although the short-term differences were statistically significant, they were moderate and might have a limited impact from the clinical point of view.




Similar content being viewed by others
References
Rutkow IM (2003) Demographic and socioeconomic aspects of hernia repair in the United States in 2003. Surg Clin North Am 83:1045–1051
Neumayer L, Hurdcr AG, Jonasson O et al (2004) Open mesh versus laparoscopic mesh repair of inguinal hernia. N Engl J Med 350:1819–1827
Kartal A, Yalcın M, Citgez B, Uzunkoy A (2017) The effect of chronic constipation on the development of inguinal herniation. Hernia 21:531–535
Langeveld HR, Van’t Riet M, Weidema WF et al (2010) Total extraperitoneal inguinal hernia repair compared with Lichtenstein (the LEVEL-Trial): a randomized controlled trial. Ann Surg 251(5):819–824
Eker HH, Langeveld HR, Klitsie PJ et al (2012) Randomized clinical trial of total extraperitoneal inguinal hernioplasty vs Lichtenstein repair: a long-term follow-up study. Arch Surg 147(3):256–260
Eklund A, Montgomery A, Bergkvist L et al (2010) Chronic pain 5 years after randomized comparison of laparoscopic and Lichtenstein inguinal hernia repair. Br J Surg 97(4):600–608
Verhagen T, Loos MJ, Scheltinga MR, Roumen RM (2016) Surgery for chronic inguinodynia following routine herniorrhaphy: beneficial effects on dysejaculation. Hernia 20(1):63–68
Bansal VK, Krishna A, Manek P et al (2017) A prospective randomized comparison of testicular functions, sexual functions and quality of life following laparoscopic totally extra-peritoneal (TEP) and trans-abdominal pre-peritoneal (TAPP) inguinal hernia repairs. Surg Endosc 31:1478–1486
Gürbulak EK, Gürbulak B, Akgün İE, Özel A, Akan D, Ömeroğlu S, Öz A, Mihmanlı M, Bektaş H (2015) Effects of totally extraperitoneal (TEP) and Lichtenstein hernia repair on testicular blood flow and volume. Surgery 158:1297–1303
Tadaki C, Lomelin D, Simorov A, Jones R, Humphreys M, daSilva M et al (2016) Perioperative outcomes and costs of laparoscopic versus open inguinal hernia repair. Hernia 20:399–404
Hedberg HM, Hall T, Gitelis M, Lapin B, Butt Z, Linn JG et al (2018) Quality of life after laparoscopic totally extraperitoneal repair of an asymptomatic inguinal hernia. Surg Endosc 32:813–819
Simons MP, Aufenacker T, Bay-Nielsen M et al (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13:343–403
Aasvang EK, Mohl B, Bay-Nielsen M, Kehlet H (2006) Pain related sexual dysfunction after inguinal herniorrhaphy. Pain 122:258–263
Bischoff JM, Linderoth G, Aasvang EK, Werner MU, Kehlet H (2012) Dysejaculation after laparoscopic inguinal herniorrhaphy: a nationwide questionnaire study. Surg Endosc 26:979–983
Andresen K, Burcharth J, Fonnes S, Hupfeld L, Rothman JP, Deigaard S et al (2017) Sexual dysfunction after inguinal hernia repair with the Onstep versus Lichtenstein technique: a randomized clinical trial. Surgery 161(6):1690–1695
Lawrence K, McWhinnie D, Jenkinson C et al (1997) Quality of life in patients undergoing inguinal hernia repair. Ann R Coll Surg Engl 79:40–45
Funding
This research was funded from departmental sources.
Author information
Authors and Affiliations
Contributions
Riza Gurhan ISIL and Omer AVLANMIS were the primary surgeons and designed the study. Riza Gurhan ISIL wrote the manuscript.
Corresponding author
Ethics declarations
Disclosures
Riza Gurhan ISIL and Omer AVLANMIS have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Isil, R.G., Avlanmis, O. Effects of totally extraperitoneal and lichtenstein hernia repair on men’s sexual function and quality of life. Surg Endosc 34, 1103–1111 (2020). https://doi.org/10.1007/s00464-019-06857-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-06857-0