Abstract
Background
Patients with hepatocellular adenomas are, in selected cases, candidates for liver resection, which can be approached via laparoscopy or laparotomy. The present study aimed to investigate the effects of the surgical approach on the postoperative morbidities of both minor and major liver resections.
Methods
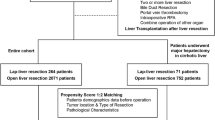
In this multi-institutional study, all patients who underwent open or laparoscopic hepatectomies for hepatocellular adenomas between 1989 and 2013 in 27 European centers were retrospectively reviewed. A multiple imputation model was constructed to manage missing variables. Comparisons of both the overall rate and the types of complications between open and laparoscopic hepatectomy were performed after propensity score adjustment (via the standardized mortality ratio weighting method) on the factors that influenced the choice of the surgical approach.
Results
The laparoscopic approach was selected in 208 (38%) of the 533 included patients. There were 194 (93%) women. The median age was 38.9 years. After the application of multiple imputation, 208 patients who underwent laparoscopic operations were compared with 216 patients who underwent laparotomic operations. After adjustment, there were 20 (9.6%) major liver resections in the laparoscopy group and 17 (7.9%) in the open group. The conversion rate was 6.3%. The two surgical approaches exhibited similar postoperative morbidity rates and severities. Laparoscopic resection was associated with significantly less blood loss (93 vs. 196 ml, p < 0.001), a less frequent need for pedicle clamping (21 vs. 40%, p = 0.002), a reduced need for transfusion (8 vs. 24 red blood cells units, p < 0.001), and a shorter hospital stay (5 vs. 7 days, p < 0.001). The mortality was nil.
Conclusions
Laparoscopy can achieve short-term outcomes similar to those of open surgery for hepatocellular adenomas and has the additional benefits of a reduced blood loss, need for transfusion, and a shorter hospital stay.
Similar content being viewed by others
References
Zucman-Rossi J, Jeannot E, Nhieu JT, Scoazec JY, Guettier C, Rebouissou S, Bacq Y, Leteurtre E, Paradis V, Michalak S, Wendum D, Chiche L, Fabre M, Mellottee L, Laurent C, Partensky C, Castaing D, Zafrani ES, Laurent-Puig P, Balabaud C, Bioulac-Sage P (2006) Genotype-phenotype correlation in hepatocellular adenoma: new classification and relationship with HCC. Hepatology 43:515–524
Marrero JA, Ahn J, Rajender Reddy K, Americal College of Gastroenterologists (2014) ACG clinical guideline: the diagnosis and management of focal liver lesions. Am J Gastroenterol 109:1328–1347
Rooks JB, Ory HW, Ishak KG, Strauss LT, Greenspan JR, Hill AP, Tyler CW Jr (1979) Epidemiology of hepatocellular adenoma. The role of oral contraceptive use. JAMA 242:644–648
Bioulac-Sage P, Taouji S, Possenti L, Balabaud C (2012) Hepatocellular adenoma subtypes: the impact of overweight and obesity. Liver Int 32:1217–1221
Paradis V, Champault A, Ronot M, Deschamps L, Valla DC, Vidaud D, Vilgrain V, Belghiti J, Bedossa P (2007) Telangiectatic adenoma: an entity associated with increased body mass index and inflammation. Hepatology 46:140–146
Barthelmes L, Tait IS (2005) Liver cell adenoma and liver cell adenomatosis. HPB 7:186–196
Kim Y, Amini N, He J, Margonis GA, Weiss M, Wolfgang CL, Makary M, Hirose K, Spolverato G, Pawlik TM (2015) National trends in the use of surgery for benign hepatic tumors in the United States. Surgery 157:1055–1064
van Aalten SM, de Man RA, JN IJ, Terkivatan T (2012) Systematic review of haemorrhage and rupture of hepatocellular adenomas. Br J Surg 99:911–916
Stoot JH, Coelen RJ, De Jong MC, Dejong CH (2010) Malignant transformation of hepatocellular adenomas into hepatocellular carcinomas: a systematic review including more than 1600 adenoma cases. HPB 12:509–522
Bioulac-Sage P, Laumonier H, Couchy G, Le Bail B, Sa Cunha A, Rullier A, Laurent C, Blanc JF, Cubel G, Trillaud H, Zucman-Rossi J, Balabaud C, Saric J (2009) Hepatocellular adenoma management and phenotypic classification: the Bordeaux experience. Hepatology 50:481–489
Ronot M, Bahrami S, Calderaro J, Valla DC, Bedossa P, Belghiti J, Vilgrain V, Paradis V (2011) Hepatocellular adenomas: accuracy of magnetic resonance imaging and liver biopsy in subtype classification. Hepatology 53:1182–1191
Dokmak S, Paradis V, Vilgrain V, Sauvanet A, Farges O, Valla D, Bedossa P, Belghiti J (2009) A single-center surgical experience of 122 patients with single and multiple hepatocellular adenomas. Gastroenterology 137:1698–1705
Karkar AM, Tang LH, Kashikar ND, Gonen M, Solomon SB, Dematteo RP, MI DA, Correa-Gallego C, Jarnagin WR, Fong Y, Getrajdman GI, Allen P, Kingham TP (2013) Management of hepatocellular adenoma: comparison of resection, embolization and observation. HPB 15:235–243
Bieze M, Phoa SS, Verheij J, van Lienden KP, van Gulik TM (2014) Risk factors for bleeding in hepatocellular adenoma. Br J Surg 101:847–855
Laurent A, Dokmak S, Nault JC, Pruvot FR, Fabre JM, Letoublon C, Bachellier P, Capussotti L, Farges O, Mabrut JY, Le Treut YP, Ayav A, Suc B, Soubrane O, Mentha G, Popescu I, Montorsi M, Demartines N, Belghiti J, Torzilli G, Cherqui D, Hardwigsen J (2016) European experience of 573 liver resections for hepatocellular adenoma: a cross-sectional study by the AFC-HCA-2013 study group. HPB 18:748–755
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative Short-term Benefits of Laparoscopic Liver Resection: 9000 Cases and Climbing. Ann Surg 263:761–777
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection-2804 patients. Ann Surg 250:831–841
Bryant R, Laurent A, Tayar C, Cherqui D (2009) Laparoscopic liver resection-understanding its role in current practice: the Henri Mondor Hospital experience. Ann Surg 250:103–111
Buell JF, Cherqui D, Geller DA, O’Rourke N, Iannitti D, Dagher I, Koffron AJ, Thomas M, Gayet B, Han HS, Wakabayashi G, Belli G, Kaneko H, Ker C-G, Scatton O, Laurent A, Abdalla EK, Chaudhury P, Dutson E, Gamblin C, D’Angelica M, Nagorney D, Testa G, Labow D, Manas D, Poon RT, Nelson H, Martin R, Clary B, Pinson WC, Martinie J, Vauthey J-N, Goldstein R, Roayaie S, Barlet D, Espat J, Abecassis M, Rees M, Fong Y, McMasters KM, Broelsch C, Busuttil R, Belghiti J, Strasberg S, Chari RS (2009) The International Position on Laparoscopic Liver Surgery. Ann Surg 250:825–830
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, O’Rourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CH, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen KH, Schon MR, Sugioka A, Tang CN, Herman P, Pekolj J, Chen XP, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo CM, Clavien PA, Kokudo N, Barkun J, Strasberg SM (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Bieze M, Busch OR, Tanis PJ, Verheij J, Phoa SS, Gouma DJ, van Gulik TM (2014) Outcomes of liver resection in hepatocellular adenoma and focal nodular hyperplasia. HPB (Oxford) 16:140–149
Abu Hilal M, Di Fabio F, Wiltshire RD, Hamdan M, Layfield DM, Pearce NW (2011) Laparoscopic liver resection for hepatocellular adenoma. World. J Gastrointest Surg 3:101–105
Cho SW, Marsh JW, Steel J, Holloway SE, Heckman JT, Ochoa ER, Geller DA, Gamblin TC (2008) Surgical management of hepatocellular adenoma: take it or leave it? Ann Surg Oncol 15:2795–2803
de’Angelis N, Memeo R, Calderaro J, Felli E, Salloum C, Compagnon P, Luciani A, Laurent A, Cherqui D, Azoulay D (2014) Open and laparoscopic resection of hepatocellular adenoma: trends over 23 years at a specialist hepatobiliary unit. HPB (Oxford) 16:783–788
Herman P, Coelho FF, Perini MV, Lupinacci RM, D’Albuquerque LA, Cecconello I (2012) Hepatocellular adenoma: an excellent indication for laparoscopic liver resection. HPB (Oxford) 14:390–395
Belghiti J, Clavien PA, Gadzijev E, Garden OJ, Lau WY, Makuuchi M, Strong RW (2000) The Brisbane 2000 Terminology of Liver Anatomy and Resections. HPB (Oxford) 2:333–339
de’Angelis N, Pascal G, Salloum C, Lahat E, Ichai P, Saliba F, Adam R, Castaing D, Azoulay D (2016) Central hepatectomy versus extended hepatectomy for malignant tumors: a propensity score analysis of postoperative complications. World J Surg 40:2745–2757
Goumard C, Farges O, Laurent A, Cherqui D, Soubrane O, Gayet B, Pessaux P, Pruvot FR, Scatton O (2015) An update on laparoscopic liver resection: The French Hepato-Bilio-Pancreatic Surgery Association statement. J Visc Surg 152:107–112
Cherqui D, Husson E, Hammoud R, Malassagne B, Stephan F, Bensaid S, Rotman N, Fagniez PL (2000) Laparoscopic liver resections: a feasibility study in 30 patients. Ann Surg 232:753–762
Chang S, Laurent A, Tayar C, Karoui M, Cherqui D (2007) Laparoscopy as a routine approach for left lateral sectionectomy. Br J Surg 94:58–63
Dokmak S, Raut V, Aussilhou B, Fteriche FS, Farges O, Sauvanet A, Belghiti J (2014) Laparoscopic left lateral resection is the gold standard for benign liver lesions: a case-control study. HPB 16:183–187
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Balzan S, Belghiti J, Farges O, Ogata S, Sauvanet A, Delefosse D, Durand F (2005) The “50–50 Criteria” on Postoperative Day 5. Ann Surg 242:824–829
van Buuren S (2007) Multiple imputation of discrete and continuous data by fully conditional specification. Stat Methods Med Res 16:219–242
Sato T, Matsuyama Y (2003) Marginal structural models as a tool for standardization. Epidemiology 14:680–686
de’Angelis N, Eshkenazy R, Brunetti F, Valente R, Costa M, Disabato M, Salloum C, Compagnon P, Laurent A, Azoulay D (2015) Laparoscopic versus open resection for colorectal liver metastases: a single-center study with propensity score analysis. J Laparoendosc Adv Surg Tech 25:12–20
Morino M, Morra I, Rosso E, Miglietta C, Garrone C (2003) Laparoscopic vs open hepatic resection: a comparative study. Surg Endosc 17:1914–1918
Polignano FM, Quyn AJ, de Figueiredo RS, Henderson NA, Kulli C, Tait IS (2008) Laparoscopic versus open liver segmentectomy: prospective, case-matched, intention-to-treat analysis of clinical outcomes and cost effectiveness. Surg Endosc 22:2564–2570
Koffron AJ, Auffenberg G, Kung R, Abecassis M (2007) Evaluation of 300 minimally invasive liver resections at a single institution: less is more. Ann Surg 246:385–394
Topal B, Fieuws S, Aerts R, Vandeweyer H, Penninckx F (2008) Laparoscopic versus open liver resection of hepatic neoplasms: comparative analysis of short-term results. Surg Endosc 22:2208–2213
Meguro M, Mizuguchi T, Kawamoto M, Ota S, Ishii M, Nishidate T, Okita K, Kimura Y, Hirata K (2015) Clinical comparison of laparoscopic and open liver resection after propensity matching selection. Surgery 158:573–587
Toro A, Gagner M, Di Carlo I (2013) Has laparoscopy increased surgical indications for benign tumors of the liver? Langenbecks Arch Surg 398:195–210
Collaborators of the AFC-HCA-2013 Study Group
François-René Pruvot Department of Digestive Surgery and Transplantation, Lille University Hospital, Nord de France University, Lille, France. Jean-Michel Fabre Department of Digestive Surgery and Transplantation, St Eloi Hospital, Montpellier, France. Christian Letoublon Clinique d’ Hépatogastroentérologie, pôle DigiDune, Grenoble University Hospital, France. Philippe Bachellier Department of Surgery, University Hospital of Hautepierre, Strasbourg, France. Olivier Farges, Department of Hepatopancreatobiliary Surgery and Liver Transplantation, Beaujon Hospital, Clichy, France. Jean-Yves Mabrut Department of Surgery, Croix Rousse Hospital, Lyon. Yves-Patrice Le Treut Department of Surgery, la Timone Hospital, Marseille, France. Bertrand Suc Department of Digestive Surgery and Transplantation, Rangueil University Hospital, Toulouse, France. Irinel Popescu Center of Gastrointestinal Disease and Liver Transplantation, Fundeni Clinical Institute, Bucharest, Romania. Marco Montorsi Department of General Surgery, Humanitas University and Research Hospital, Milano, Italy. Jacques Belghiti, Department of Hepatopancreatobiliary Surgery and Liver Transplantation, Beaujon Hospital, Clichy, France. Jean-Marc Régimbaud – CHU Amiens-Picardie, France. Romain Riboud – CHU Grenoble, France. Alexandra Dili – La Louvière, Hôpital de Jolimont, Belgium. Pierre Allemann – (CHUV), Lausanne, Switzerland. Emmanuel Boleslawski - CHRU Lille, France. Benjamin Darnis – CHU Lyon, France. Mustapha Adham, CHU Lyon, France. Emilie Bollon – CHU Marseille, France. Bernard Pol – Hôpital Saint-Joseph, Marseille, France. Jean-Robert Delpero – Institut Paoli-Calmettes, Marseille, France. Olivier Turrini – Institut Paoli-Calmettes, Marseille, France. Frédéric Borie – CHU-Nimes, France. Mathieu Gonot-Gachard – CHU-Nimes, France. Laura Ornella Perotto – CHU Pitié-Salpétrière, Paris, France. Riccardo Gauzolino – CHU-Poitier, France. Marie Castagnet – CHU-Poitier, France. Reza Kianmanesh – CHU-Reims, France. Daniele Sommacale – CHU-Reims, France. Mikael Chetboun – CHU-Reims, France. Jean-Luc Porcheron – CHU-St-Etienne, France. Alexandre Filippello – CHU-St-Etienne, France. Patrick Pessaux – CHU-Strasbourg, France. Pietro Addeo – CHU-Strasbourg, France. Manuela Cesaretti – CHU-Strasbourg, France.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Filippo Landi, Nicola de’Angelis, Olivier Scatton, Xavier Vidal, Ahmet Ayav, Fabrice Muscari, Safi Dokmak, Guido Torzilli, Nicolas Demartines, Olivier Soubrane, Daniel Cherqui, Jean Hardwigsen, and Alexis Laurent have no conflicts of interest or financial ties to disclose in relation to the results of the present study.
Additional information
Filippo Landi and Nicola de Angelis have contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Landi, F., de’ Angelis, N., Scatton, O. et al. Short-term outcomes of laparoscopic vs. open liver resection for hepatocellular adenoma: a multicenter propensity score adjustment analysis by the AFC-HCA-2013 study group. Surg Endosc 31, 4136–4144 (2017). https://doi.org/10.1007/s00464-017-5466-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5466-4