Abstract
Background
Despite patient risk factors such as diabetes and obesity, contamination during surgery remains a significant cause of infections and subsequent wound morbidity. Pressurized pulse lavage (PPL) has been utilized as a method to reduce bacterial bioburden with promising results in many fields. Although existing methods of lavage have been utilized during abdominal operations, no studies have examined the use of PPL during complex hernia repair.
Methods
Patients undergoing abdominal wall reconstruction (AWR) in clean-contaminated or contaminated fields with antibiotic PPL, from January 2012 to May 2013, were prospectively evaluated. Primary outcome measures studied were conversion of retrorectus space culture from positive to negative after PPL and 30-day surgical site infection (SSI) rate.
Results
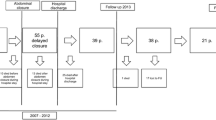
A total of 56 patients underwent AWR, with 44 patients (78.6 %) having clean-contaminated fields and 12 patients (21.4 %) having contaminated ones. Twenty-two patients (39.3 %) had positive pre-PPL cultures, 18 of which (81.8 %) converted to negative cultures after PPL. Eleven patients (19.6 %) developed SSIs. Those with persistently positive cultures after PPL had the highest rate of SSI, where two out of four patients (50.0 %) developed an SSI. Contrastingly, only 5 of 18 patients (27.8 %) who converted from a positive to negative culture after PPL developed an SSI.
Conclusion
Our findings demonstrate that antibiotic PPL is an effective method to reduce bacterial bioburden during AWR in clean-contaminated and contaminated fields. While complete conversion and eradication of SSI were not achieved, we believe that PPL may be a useful adjunct to standard operative asepsis in preventing prosthetic contamination during contaminated AWR.
Similar content being viewed by others
References
Breuing K, Butler CE, Ferzoco S, Franz M, Hultman CS, Kilbridge JF, Rosen M, Silverman RP, Vargo D (2010) Incisional ventral hernias: review of the literature and recommendations regarding the grading and technique of repair. Surgery 148:544–558. doi:10.1016/j.surg.2010.01.008
Koltz PF, Frey JD, Bell DE, Girotto JA, Christiano JG, Langstein HN (2013) Evolution of abdominal wall reconstruction: development of a unified algorithm with improved outcomes. Ann Plast Surg 71:554–560. doi:10.1097/SAP.0b013e3182a6367f
Lowe JB, Lowe JB, Baty JD, Garza JR (2003) Risks associated with “components separation” for closure of complex abdominal wall defects. Plast Reconstr Surg 111:1276–1283. doi:10.1097/01.PRS.0000047021.36879.FD (quiz 1284–5; discussion 1286–8)
Awad ZT, Puri V, LeBlanc K, Stoppa R, Fitzgibbons RJ, Iqbal A, Filipi CJ (2005) Mechanisms of ventral hernia recurrence after mesh repair and a new proposed classification. J Am Coll Surg 201:132–140. doi:10.1016/j.jamcollsurg.2005.02.035
Luijendijk RW, Hop WC, van den Tol MP, de Lange DC, Braaksma MM, IJzermans JN, Boelhouwer RU, de Vries BC, Salu MK, Wereldsma JC, Bruijninckx CM, Jeekel J (2000) A comparison of suture repair with mesh repair for incisional hernia. N Engl J Med 343:392–398. doi:10.1056/NEJM200008103430603
Iqbal CW, Pham TH, Joseph A, Mai J, Thompson GB, Sarr MG (2007) Long-term outcome of 254 complex incisional hernia repairs using the modified Rives–Stoppa technique. World J Surg 31:2398–2404. doi:10.1007/s00268-007-9260-7
Colavita PD, Zemlya AY, Tsirline VB et al (2013) The expansive cost of wound complications following ventral hernia repair. In: American College of Surgeons meeting in Washington, DC
Darouiche RO (2004) Treatment of infections associated with surgical implants. N Engl J Med 350:1422–1429. doi:10.1056/NEJMra035415
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol 20:250–278. doi:10.1086/501620 (quiz 279–80)
Rodeheaver GT, Pettry D, Thacker JG, Edgerton MT, Edlich RF (1975) Wound cleansing by high pressure irrigation. Surg Gynecol Obstet 141:357–362
Brown LL, Shelton HT, Bornside GH, Cohn I (1978) Evaluation of wound irrigation by pulsatile jet and conventional methods. Ann Surg 187:170–173
Svoboda SJ, Bice TG, Gooden HA, Brooks DE, Thomas DB, Wenke JC (2006) Comparison of bulb syringe and pulsed lavage irrigation with use of a bioluminescent musculoskeletal wound model. J Bone Joint Surg Am 88:2167–2174. doi:10.2106/JBJS.E.00248
Muñoz-Mahamud E, García S, Bori G, Martínez-Pastor JC, Zumbado JA, Riba J, Mensa J, Soriano A (2011) Comparison of a low-pressure and a high-pressure pulsatile lavage during debridement for orthopaedic implant infection. Arch Orthop Trauma Surg 131:1233–1238. doi:10.1007/s00402-011-1291-8
Mote GA, Malay DS (2010) Efficacy of power-pulsed lavage in lower extremity wound infections: a prospective observational study. J Foot Ankle Surg 49:135–142. doi:10.1053/j.jfas.2009.10.004
Fry DE (2013) The prevention of surgical site infection in elective colon surgery. Scientifica 2013:896297. doi:10.1155/2013/896297
Cervantes-Sánchez CR, Gutiérrez-Vega R, Vázquez-Carpizo JA, Clark P, Athié-Gutiérrez C (2000) Syringe pressure irrigation of subdermic tissue after appendectomy to decrease the incidence of postoperative wound infection. World J Surg 24:38–41
Novitsky YW, Elliott HL, Orenstein SB, Rosen MJ (2012) Transversus abdominis muscle release: a novel approach to posterior component separation during complex abdominal wall reconstruction. Am J Surg 204:709–716. doi:10.1016/j.amjsurg.2012.02.008
Carbonell AM, Criss CN, Cobb WS, Novitsky YW, Rosen MJ (2013) Outcomes of synthetic mesh in contaminated ventral hernia repairs. J Am Coll Surg 217:991–998. doi:10.1016/j.jamcollsurg.2013.07.382
Hargrove R, Ridgeway S, Russell R, Norris M, Packham I, Levy B (2006) Does pulse lavage reduce hip hemiarthroplasty infection rates? J Hosp Infect 62:446–449. doi:10.1016/j.jhin.2005.07.012
Luedtke-Hoffmann KA, Schafer DS (2000) Pulsed lavage in wound cleansing. Phys Ther 80:292–300
Nikfarjam M, Weinberg L, Fink MA, Muralidharan V, Starkey G, Jones R, Staveley-O’Carroll K, Christophi C (2014) Pressurized pulse irrigation with saline reduces surgical-site infections following major hepatobiliary and pancreatic surgery: randomized controlled trial. World J Surg 38:447–455. doi:10.1007/s00268-013-2309-x
Wheeler CB, Rodeheaver GT, Thacker JG, Edgerton MT, Edilich RF (1976) Side-effects of high pressure irrigation. Surg Gynecol Obstet 143:775–778
Platell C, Papadimitriou JM, Hall JC (2000) The influence of lavage on peritonitis. J Am Coll Surg 191:672–680
Primus FE, Harris HW (2013) A critical review of biologic mesh use in ventral hernia repairs under contaminated conditions. Hernia 17:21–30. doi:10.1007/s10029-012-1037-8
Bahrs C, Schnabel M, Frank T, Zapf C, Mutters R, von Garrel T (2003) Lavage of contaminated surfaces: an in vitro evaluation of the effectiveness of different systems. J Surg Res 112:26–30
Anglen JO, Apostoles S, Christensen G, Gainor B (1994) The efficacy of various irrigation solutions in removing slime-producing Staphylococcus. J Orthop Trauma 8:390–396
Parcells JP, Mileski JP, Gnagy FT, Haragan AF, Mileski WJ (2009) Using antimicrobial solution for irrigation in appendicitis to lower surgical site infection rates. Am J Surg 198:875–880. doi:10.1016/j.amjsurg.2009.09.002
Owens BD, White DW, Wenke JC (2009) Comparison of irrigation solutions and devices in a contaminated musculoskeletal wound survival model. J Bone Joint Surg Am 91:92–98. doi:10.2106/JBJS.G.01566
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Arnab Majumder, Heidi J. Miller, Parita Patel, Yuhsin V. Wu, and Heidi L. Elliott have no conflicts of interest or financial ties to disclose. Yuri W. Novitsky declares conflicts of interest [consultant for C.R. Bard (Davol) and Cooper Surgical, prior research support from C.R. Bard (Davol)] not directly related to the submitted work.
Rights and permissions
About this article
Cite this article
Majumder, A., Miller, H.J., Patel, P. et al. Evaluation of antibiotic pressurized pulse lavage for contaminated retromuscular abdominal wall reconstruction. Surg Endosc 31, 2763–2770 (2017). https://doi.org/10.1007/s00464-016-5283-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5283-1