Abstract
Purpose
There is a significant morbidity associated with abdominal wall reconstruction (AWR) with a need for overall improvement during the post-operative management. Scientific literature has proven the use of negative pressure therapy (NPT) in wound healing for orthopedic and cardiac surgery with limited data present on its role in AWR. The goal of this study was to examine whether primary wound events were different between patients who had primary closure with NPT versus patients who only had primary closure after AWR.
Methods
This retrospective study examined the rate of post-operative complications in all open-complex AWR that were done in a similar fashion between May 2008 and July 2011 at two large university teaching hospitals. Wound closure was stringent upon attending surgeon preference without randomization.
Results
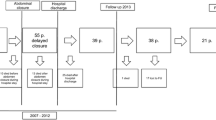
There were a total of 61 patients who met inclusion criteria with an average age of 54 and 60 % were women. Thirty-two patients had primary closure and 29 patients had primary closure with NPT. The mean length of follow-up was 167 days for both groups. The type of wound closure had an effect on the rate of hernia recurrence and surgical site infections. The application of NPT leads to lower hernia recurrence rate of 25 versus 3 % and the type of wound closure had a profound effect on the rate and type of SSI.
Conclusions
The data presented in this study demonstrates a potential advantage for adjunctive NPT in patients undergoing AWR. There is an associated decreased incidence in the overall rate of SSI and hernia recurrence with the use of NPT in those patients undergoing AWR. These results show an advantage for adjunctive NPT.

Similar content being viewed by others
References
Korenkov M, Paul A, Sauerland S, Neugebauer E, Arndt M, Chevrel JP, Corcione F, Fingerhut A, Flament JB, Kux M, Matzinger A, Myrvold HE, Rath AM, Simmermacher RK (2001) Classification and surgical treatment of incisional hernia. Results of an experts’ meeting. Langenbecks Arch Surg 386:65–73
Bachman SL, Ramaswamy A, Ramshaw BJ (2009) Early results of midline hernia repair using a minimally invasive component separation technique. Am Surg 75:572–577 (discussion 577–578)
Barbaros U, Asoglu O, Seven R, Erbil Y, Dinccag A, Deveci U, Ozarmagan S, Mercan S (2007) The comparison of laparoscopic and open ventral hernia repairs: a prospective randomized study. Hernia 11:51–56
Breuing K, Butler CE, Ferzoco S, Franz M, Hultman CS, Kilbridge JF, Rosen M, Silverman RP, Vargo D (2010) Incisional ventral hernias: review of the literature and recommendations regarding the grading and technique of repair. Surgery 148:544–558
Candage R, Jones K, Luchette FA, Sinacore JM, Vandevender D, Reed RL 2nd (2008) Use of human acellular dermal matrix for hernia repair: friend or foe? Surgery 144:703–709 (discussion 709–711)
de Vries Reilingh TS, van Goor H, Rosman C, Bemelmans MH, de Jong D, van Nieuwenhoven EJ, van Engeland MI, Bleichrodt RP (2003) “Components separation technique” for the repair of large abdominal wall hernias. J Am Coll Surg 196:32–37
Diaz JJ, Jr, Guy J, Berkes MB, Guillamondegui O, Miller RS (2006) Acellular dermal allograft for ventral hernia repair in the compromised surgical field. Am Surg 72:1181–1187 (discussion 1187–1188)
Eriksen JR, Gogenur I, Rosenberg J (2007) Choice of mesh for laparoscopic ventral hernia repair. Hernia 11:481–492
Goodney PP, Birkmeyer CM, Birkmeyer JD (2002) Short-term outcomes of laparoscopic and open ventral hernia repair: a meta-analysis. Arch Surg 137:1161–1165
Ko JH, Wang EC, Salvay DM, Paul BC, Dumanian GA (2009) Abdominal wall reconstruction: lessons learned from 200 “components separation” procedures. Arch Surg 144:1047–1055
Larson GM (2000) Ventral hernia repair by the laparoscopic approach. Surg Clin North Am 80:1329–1340
Lowham AS, Filipi CJ, Fitzgibbons RJ Jr, Stoppa R, Wantz GE, Felix EL, Crafton WB (1997) Mechanisms of hernia recurrence after preperitoneal mesh repair. Traditional and laparoscopic. Ann Surg 225:422–431
Meeker J, Weinhold P, Dahners L (2011) Negative pressure therapy on primarily closed wounds improves wound healing parameters at 3 days in a porcine model. J Orthop Trauma 25:756–761
Pachowsky M, Gusinde J, Klein A, Lehrl S, Schulz-Drost S, Schlechtweg P, Pauser J, Gelse K, Brem MH (2012) Negative pressure wound therapy to prevent seromas and treat surgical incisions after total hip arthroplasty. Int Orthop 36:719–722
Tocco MP, Costantino A, Ballardini M, D’Andrea C, Masala M, Merico E, Mosillo L, Sordini P (2009) Improved results of the vacuum assisted closure and nitinol clips sternal closure after postoperative deep sternal wound infection. Eur J Cardiothorac Surg 35:833–838
Blackham AU, Farrah JP, McCoy TP, Schmidt BS, Shen P (2013) Prevention of surgical site infections in high-risk patients with laparotomy incisions using negative-pressure therapy. Am J Surg 205:647–654
Lee SY, Niikura T, Miwa M, Sakai Y, Oe K, Fukazawa T, Kawakami Y, Kurosaka M (2011) Negative pressure wound therapy for the treatment of infected wounds with exposed knee joint after patellar fracture. Orthopedics 34:211
Satterwhite TS, Miri S, Chung C, Spain D, Lorenz HP, Lee GK (2012) Outcomes of complex abdominal herniorrhaphy: experience with 106 cases. Ann Plast Surg 68:382–388
Ramirez OM, Ruas E, Dellon AL (1990) “Components separation” method for closure of abdominal-wall defects: an anatomic and clinical study. Plast Reconstr Surg 86:519–526
Boltz MM, Hollenbeak CS, Julian KG, Ortenzi G, Dillon PW (2011) Hospital costs associated with surgical site infections in general and vascular surgery patients. Surgery 150:934–942
Conde-Green A, Chung TL, Holton LH 3rd, Hui-Chou HG, Zhu Y, Wang H, Zahiri H, Singh DP (2013) Incisional negative-pressure wound therapy versus conventional dressings following abdominal wall reconstruction: A comparative study. Ann Plast Surg 71:394–397
Pauli EM, Krpata DM, Novitsky YW, Rosen MJ (2013) Negative pressure therapy for high-risk abdominal wall reconstruction incisions. Surg Infect 14:270–274
Conflict of interest
AG declares no conflict of interest.
AM declares no conflict of interest.
EB declares no conflict of interest.
AA declares no conflict of interest.
OG declares no conflict of interest.
MM declares no conflict of interest.
TE declares no conflict of interest.
CT declares no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gassman, A., Mehta, A., Bucholdz, E. et al. Positive outcomes with negative pressure therapy over primarily closed large abdominal wall reconstruction reduces surgical site infection rates. Hernia 19, 273–278 (2015). https://doi.org/10.1007/s10029-014-1312-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-014-1312-y