Abstract
Background
The advantages of reduced-port laparoscopic surgery (RPLS) for rectosigmoid cancer treatment have been disputed. This study evaluated the outcomes of RPLS compared to conventional laparoscopic surgery (CLS) for rectosigmoid cancer.
Methods
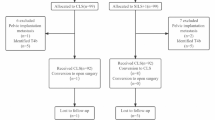
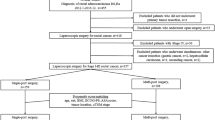
Data from 211 patients who underwent a selective sigmoidectomy or anterior resection from August 2011 to June 2014 at a single institution were collected and analyzed via propensity score matching. Operative outcomes, inflammatory responses, pain intensity, oncologic outcomes, quality of life, and cosmetic results were compared between groups.
Results
After matching, 96 patients (48 CLS and 48 RPLS) were evaluated. Sixteen RPLS cases underwent single-incision laparoscopic surgery (SILS), and 32 underwent single-incision plus one port laparoscopic surgery (SILS + 1). Baseline clinical characteristics were comparable between the RPLS and the CLS groups. Morbidity, pathologic outcomes, and 3-year disease-free survival and overall survival rates were also comparable between the 2 groups. Compared with the CLS group, the RPLS group had a shorter total incision length (p < 0.001); shorter time to liquid diet (p = 0.027), ambulation (p = 0.026), and discharge (p < 0.001); and lower visual analogue scale scores during mobilization at postoperative days 3–5 (p < 0.05). The total operation times, C-reactive protein levels at 24 h and 96 h, and interleukin-6 levels at 24 h postoperatively were significantly lower in the SILS + 1 group than those in the CLS and SILS groups (p < 0.05). Compared with the CLS group, the RPLS group showed better social functioning at 6 months postoperatively (p = 0.011). The SILS and SILS + 1 groups showed similar cosmetic results, and both groups showed better results than the CLS group (p < 0.001).
Conclusions
RPLS for rectosigmoid cancer is feasible, with short-term safety and long-term oncological safety comparable to that of CLS. Better cosmesis and accelerated recovery can be expected. SILS + 1 is a better choice than CLS or SILS for rectosigmoid cancer because it minimizes invasiveness and reduces technical difficulties.







Similar content being viewed by others
Abbreviations
- CLS:
-
Conventional laparoscopic surgery
- RPLS:
-
Reduced-port laparoscopic surgery
- SILS:
-
Single-incision laparoscopic surgery
- SILS + 1:
-
Single-incision plus one port laparoscopic surgery
- QOL:
-
Quality of life
- BMI:
-
Body mass index
- EORTC:
-
European Organization for Research and Treatment of Cancer
- PCIA:
-
Patient-controlled opioid-based intravenous analgesia
- POD:
-
Postoperative day
- WBC:
-
White blood cell
- CRP:
-
C-reactive protein
- IL-6:
-
Interleukin-6
- TNF-α:
-
Tumor necrosis factor-α
- DFS:
-
Disease-free survival
- OS:
-
Overall survival
- VAS:
-
Visual analogue scale
References
Bonjer HJ (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 10:44–52
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AMH, Heath RM, Brown JM (2005) Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet 365:1718–1726
Curcillo PG 2nd, Podolsky ER, King SA (2011) The road to reduced port surgery: from single big incisions to single small incisions, and beyond. World J Surg 35:1526–1531
Takemasa I, Uemura M, Nishimura J, Mizushima T, Yamamoto H, Ikeda M, Sekimoto M, Doki Y, Mori M (2014) Feasibility of single-site laparoscopic colectomy with complete mesocolic excision for colon cancer: a prospective case-control comparison. Surg Endosc 28:1110–1118
Kim SJ, Ryu GO, Choi BJ, Kim JG, Lee KJ, Lee SC, Oh ST (2011) The short-term outcomes of conventional and single-port laparoscopic surgery for colorectal cancer. Ann Surg 254:933–940
Kim CW, Cho MS, Baek SJ, Hur H, Min BS, Kang J, Baik SH, Lee KY, Kim NK (2015) Oncologic outcomes of single-incision versus conventional laparoscopic anterior resection for sigmoid colon cancer: a propensity-score matching analysis. Ann Surg Oncol 22:924–930
Yun JA, Yun SH, Park YA, Huh JW, Cho YB, Kim HC, Lee WY (2016) Oncologic outcomes of single-incision laparoscopic surgery compared with conventional laparoscopy for colon cancer. Ann Surg. 263:973–978
Lim SW, Kim HJ, Kim CH, Huh JW, Kim YJ, Kim HR (2013) Umbilical incision laparoscopic colectomy with one additional port for colorectal cancer. Tech Coloproctol 17:193–199
Gash K, Bicsak M, Dixon A (2015) Single incision laparoscopic surgery for rectal cancer: early results and medium term oncological outcome. Colorectal Dis 17:1071–1078
Hamabe A, Takemasa I, Uemura M, Nishimura J, Mizushima T, Ikeda M, Yamamoto H, Sekimoto M, Doki Y, Mori M (2014) Feasibility of single-port laparoscopic surgery for sigmoid colon and rectal cancers and preoperative assessment of operative difficulty. J Gastrointest Surg 18:977–985
Kawamata F, Homma S, Minagawa N, Kawamura H, Takahashi N, Taketomi A (2014) Comparison of single-incision plus one additional port laparoscopy-assisted anterior resection with conventional laparoscopy-assisted anterior resection for rectal cancer. World J Surg 38:2716–2723
Yu H, Shin JY (2016) Short-term outcomes following reduced-port, single-port, and multi-port laparoscopic surgery for colon cancer: tailored laparoscopic approaches based on tumor size and nodal status. Int J Colorectal Dis 31:115–122
Edge SBBD, Compton CC, Fritz AG, Greene FL, Trotti A (eds) (2010) AJCC cancer staging manual, 7th edn. Springer, New York
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, Duez NJ, Filiberti A, Flechtner H, Fleishman SB, de Haes JC (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85:365–376
Whistance RN, Conroy T, Chie W, Costantini A, Sezer O, Koller M, Johnson CD, Pilkington SA, Arraras J, Ben-Josef E, Pullyblank AM, Fayers P, Blazeby JM (2009) Clinical and psychometric validation of the EORTC QLQ-CR29 questionnaire module to assess health-related quality of life in patients with colorectal cancer. Eur J Cancer 45:3017–3026
Dunker MS, Stiggelbout AM, van Hogezand RA, Ringers J, Griffioen G, Bemelman WA (1998) Cosmesis and body image after laparoscopic-assisted and open ileocolic resection for Crohn’s disease. Surg Endosc 12:1334–1340
Fayers P, Aaronson N, Bjordal K, Groenvold M, Curran D, Bottomley A (2001) The EORTC QLQ-C30 scoring manual, 3rd edn. European Organisation for Research and Treatment of Cancer, Brussels
Bucher P, Pugin F, Morel P (2008) Single port access laparoscopic right hemicolectomy. Int J Colorectal Dis 23:1013–1016
Katsuno G, Fukunaga M, Nagakari K, Yoshikawa S, Azuma D, Kohama S (2016) Short-term and long-term outcomes of single-incision versus multi-incision laparoscopic resection for colorectal cancer: a propensity-score-matched analysis of 214 cases. Surg Endosc 30:1317–1325
Hiraki M, Takemasa I, Uemura M, Haraguchi N, Nishimura J, Hata T, Mizushima T, Yamamoto H, Doki Y, Mori M (2014) Evaluation of invasiveness in single-site laparoscopic colectomy, using “the PainVision system” for quantitative analysis of pain sensation. Surg Endosc 28:3216–3223
Moraca RJ, Sheldon DG, Thirlby RC (2003) The role of epidural anesthesia and analgesia in surgical practice. Ann Surg 238:663–673
Bulut O, Aslak KK, Levic K, Nielsen CB, Romer E, Sorensen S, Christensen IJ, Nielsen HJ (2015) A randomized pilot study on single-port versus conventional laparoscopic rectal surgery: effects on postoperative pain and the stress response to surgery. Tech Coloproctol 19:11–22
Jung IK, Kim MC, Kim KH, Kwak JY, Jung GJ, Kim HH (2008) Cellular and peritoneal immune response after radical laparoscopy-assisted and open gastrectomy for gastric cancer. J Surg Oncol 98:54–59
Nelson H, Petrelli N, Carlin A, Couture J, Fleshman J, Guillem J, Miedema B, Ota D, Sargent D (2001) Guidelines 2000 for colon and rectal cancer surgery. J Natl Cancer Inst 93:583–596
Acknowledgments
This study was supported by Major Program of Science and Technology Program of Guangzhou (No. 201300000087 and No. 201508020047), Research Fund of Public welfare in Health Industry of National Health and Family Planning Commission of China (No.201402015 and No. 201502039), National Key Technology R&D Program (No.2013BAI05B05), and Key Clinical Specialty Discipline Construction Program.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosure
Drs. Ruoyan Liu, Yanan Wang, Ze Zhang, Tingting Li, Hao Liu, Liying Zhao, Haijun Deng, and Guoxin Li have no conflicts of interest or financial ties to disclose.
Additional information
Ruoyan Liu and Yanan Wang have contributed equally to this work and should be considered co-first authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, R., Wang, Y., Zhang, Z. et al. Assessment of treatment options for rectosigmoid cancer: single-incision plus one port laparoscopic surgery, single-incision laparoscopic surgery, and conventional laparoscopic surgery. Surg Endosc 31, 2437–2450 (2017). https://doi.org/10.1007/s00464-016-5244-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5244-8