Abstract
Introduction
Ventral and incisional hernia repair (VIHR) is among the most frequently performed abdominal operations with significant incidence of postoperative complications and readmissions. Payers are targeting increased “value” of care through improved outcomes and reduced costs. Cost data in clinically relevant terms is still rare. This study aims to identify hospital costs associated with clinically relevant factors in order to facilitate strategies by surgeons to enhance the value of VIHR.
Methods
An IRB-approved retrospective review of VIHRs performed at the University of Kentucky from April 2009 through September 2013 was conducted. NSQIP clinical data and hospital cost data were matched. Operating room (ORC), total encounter (TEC), and 90-day postdischarge (90PDC) hospital costs were analyzed relative to clinical variables using non-parametric tests.
Results
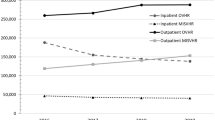
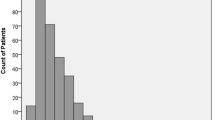
In total 385 patients that underwent VIHR during the time period were included in the analyses. Considering all VIHRs, median [interquartile range (IQR)] ORC was $6900 ($5600–$10,000); TEC was $10,700 ($7500–$18,600); and 90PDC was $0 ($0–$800). Compared to all VIHRs, ASA Class ≥ 3 was associated with increased ORC and TEC (p < .001), and 90PDC (p < .01). Preoperative open wound was associated with increased ORC and TEC (p < .001). Numerous operative variables were associated with both increased ORC and TEC. Wound Class > 1 was associated with increased ORC and TEC (p < .001) and 90PDC (p < .01). Inpatient occurrence of any complication was associated with increased TEC and 90PDC (p < .001).
Conclusions
ASA Class ≥ 3, Wound Class > 1, open abdominal wound, and postoperative complications significantly increase costs. Although the hospital encounter represents the majority of the cost associated with VIHR, additional costs are incurred during the 90-day postoperative period. An appreciation of global costs is essential in developing alternative payment models for hernia in order to provide the greatest value in hernia care.

Similar content being viewed by others
References
Merkow RP, Ju MH, Chung JW, Hall BL, Cohen ME, Williams MV, Tsai TC, Ko CY, Bilimoria KY (2015) Underlying reasons associated with hospital readmission following surgery in the United States. JAMA 313:483–495. doi:10.1001/jama.2014.18614
Lovecchio F, Farmer R, Souza J, Khavanin N, Dumanian GA, Kim JY (2014) Risk factors for 30-day readmission in patients undergoing ventral hernia repair. Surgery 155(4):702–710. doi:10.1016/j.surg.2013.12.021
Kassin MT, Owen RM, Perez SD, Leeds I, Cox JC, Schnier K, Sadiraj V, Sweeney JF (2012) Risk factors for 30-day hospital readmission among general surgery patients. J Am Coll Surg 215(3):322–330. doi:10.1016/j.jamcollsurg.2012.05.024
Baltodano PA, Webb-Vargas Y, Soares KC, Hicks CW, Cooney CM, Cornell P, Burce KK, Pawlik TM, Eckhauser FE (2016) A validated, risk assessment tool for predicting readmission after open ventral hernia repair. Hernia 20:119–129. doi:10.1007/s10029-015-1413-2
Brooke BS, Stone DH, Cronenwett JL, Nolan B, DeMartino RR, MacKenzie TA, Goodman DC, Goodney PP (2014) Early primary care provider follow-up and readmission after high-risk surgery. JAMA Surg 149:821–828. doi:10.1001/jamasurg.2014157
Nguyen MT, Li LT, Hicks SC, Davila JA, Suliburk JW, Leong M, Kao LS, Berger DH, Liang MK (2013) Readmission following open ventral hernia repair: incidence, indications, and predictors. Am J Surg 206:942–949. doi:10.1016/j.amjsurg.2013.08.022
Holihan JL, Alawadi Z, Martindale RG, Roth JS, Wray CJ, Ko TC, Kao L, Liang MK (2015) Adverse events after ventral hernia repair: the vicious cycle of complications. J Am Coll Surg 221:478–485. doi:10.1016/j.jamcollsurg.2015.04.026
Liang MK, Goodenough CJ, Martindale RG, Roth JS, Kao LS (2015) External validation of the ventral hernia risk score for prediction of surgical site infections. Surg Infect 16:36–40. doi:10.1089/sur.2014.115
Poulose BK, Shelton J, Phillips S, Moore D, Nealon W, Penson D, Holzman MD (2012) Epidemiology and cost of ventral hernia repair: making the case for hernia research. Hernia 16:179–183. doi:10.1007/s10029-011-0879-9
Hackbarth G, Reischauer R, Mutt A (2008) Collective accountability for medical care—toward bundled medicare payments. N Engl J Med 359:3–5. doi:10.1056/NEJMp0803749
Centers for Medicare and Medicaid Services (2016) The merit-based incentive payment system (MIPS) & alternative payment models (APMs). https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/Value-Based-Programs/MACRA-MIPS-and-APMs/MACRA-MIPS-and-APMs.html. Accessed 8 Feb 2016
Reynolds D, Davenport D, Korosec R, Roth JS (2013) Financial implications of ventral hernia repair: a hospital cost analysis. J Gastrointest Surg 17:159–167. doi:10.1007/s11605-012-1999-y
Davenport DL, Henderson WG, Khuri SF, Mentzer RM (2005) Preoperative risk factors and surgical complexity are more predictive of costs than postoperative complications: a case study using the National Surgical Quality Improvement Program (NSQIP) database. Ann Surg 242:463–471
Petro CC, O’Rourke CP, Posielski NM, Criss CN, Raigani S, Prabhu AS, Rosen MJ (2016) Designing a ventral hernia staging system. Hernia 20:111–117. doi:10.1007/s10029-015-1418-x
Fischer JP, Wes AM, Wink JD, Nelson JA, Rohrbach JI, Braslow BM, Kovach SJ (2014) Analysis of perioperative factors associated with increased cost following abdominal wall reconstruction (AWR). Hernia 18:617–624. doi:10.1007/s10029-014-1276-y
Berger RL, Li LT, Hicks SC, Davila JA, Kao LS, Liang MK (2013) Development and validation of a risk-stratification score for surgical site occurrence and surgical site infection after open ventral hernia repair. J Am Coll Surg 217:974–982. doi:10.1016/j.jamcollsurg.2013.08.003
Sorensen LT (2012) The clinical impact of smoking and smoking cessation: a systematic review and meta-analysis. Arch Surg 147:373–383
Goodenough CJ, Liang MK, Nguyen MT, Nguyen DH, Holihan JL, Awawadi ZM, Roth JS, Wray CJ, Ko TC, Kao LS (2015) Preoperative glycosylated hemoglobin and postoperative glucose together predict major complications after abdominal surgery. J Am Coll Surg 221:854–861
Stone AB, Grant MC, Pio Roda C, Hobson D, Pawlik T, Wu CL, Wick EC (2016) Implementation costs of an enhanced recovery after surgery program in the United States: a financial model and sensitivity analysis based on experiences at a quaternary academic medical center. J Am Coll Surg 222:113. doi:10.1016/j.jamcollsurg.2015.11.021
Thiele RH, Rea KM, Turrentine FE, Friel CM, Hassinger TE, Goudreau BJ, Umapathi BA, Kron IL, Sawyer RG, Hedrick TL, McMurry TL (2015) Standardization of care: impact of an enhanced recovery protocol on length of stay, complications and direct costs after colorectal surgery. J Am Coll Surg 220:430–443. doi:10.1016/j.jamcollsurg.2014.12.042
Fayezizadeh M, Petro CC, Rosen MJ, Novitsky YW (2014) Enhanced recovery after surgery pathway for abdominal wall reconstruction: pilot study and preliminary outcomes. Plast Reconstr Surg 134:151S–159S. doi:10.1097/prs.0000000000000674
Haynes AB, Weiser TG, Berry WR, Lipsitz SR, Breizat AH, Dellinger EP, Herbosa T, Joseph S, Kibatala PL, Lapitan MC, Merry AF, Moorthy K, Reznick RK, Taylor B, Gawande AA, Safe Surgery Saves Lives Study Group (2009) A surgical safety checklist to reduce morbidity and mortality in a global population. New Engl J Med 360:491–499
Scally CP, Thumma JR, Birkmeyer JD, Dimick JB (2015) Impact of surgical quality improvement on payments in medicare patients. Ann Surg 262:249–252
Hammermeister K (2009) The National Surgical Quality Improvement Program: learning from the past and moving to the future. Am J Surg 198:S69–S73
Hakko E, Guvenc S, Karaman I, Cakmak A, Erdem T, Cakmakci M (2015) Long-term sustainability of zero central-line associated bloodstream infections is possible with high compliance with care bundle elements. East Mediterr Health J 21:293–298
Pavia M, Mazza M (2016) Adding innovative practices and technology to central line bundle reduces bloodstream infection rate in challenging pediatric population. Am J Infect Control 44:112–114. doi:10.1016/j.ajic.2015.08.026
Eappen S, Lane BH, Rosenberg B, Lipsitz SA, Sadoff D, Matheson D, Berry WR, Lester M, Gawande AA (2013) Relationship between occurrence of surgical complications and hospital finances. JAMA 309:1599–1606. doi:10.1001/jama.2013.2773
Gani F, Hundt J, Makary MA, Haider AH, Zogg CK, Pawlik TM (2016) Financial impact of postoperative complication following hepato-pancreatico-biliary surgery for cancer. Ann Surg Oncol 23:1064–1070. doi:10.1245/s10434-015-5042-x
Colavita PD, Tsirline VB, Walters AL, Lincourt AE, Belyansky I, Heniford BT (2013) Laparoscopic versus open hernia repair: outcomes and sociodemographic utilization results from the nationwide inpatient sample. Surg Endosc 27:109–117. doi:10.1007/s00464-012-2432-z
Colavita PD, Tsirline VB, Belyansky I, Walters AL, Lincourt AE, Sing RF, Heniford T (2012) Prospective, long-term comparison of quality of life in laparoscopic versus open ventral hernia repair. Ann Surg 256:714–723
Liu Y, Pleasants RA, Croft JB, Wheaton AG, Khosrow H, Malarcher AM, Ohar JA, Kraft M, Mannino DM, Strange C (2015) Smoking duration, respiratory symptoms, and COPD in adults aged ≥ 45 years with a smoking history. Int J COPD 10:1409–1416. doi:10.2147/COPD.S82259
Acknowledgements
The authors acknowledge and express their gratitude for the expert work of the NSQIP nurses, Devauna Riley, RN, and Roseanna Adair, RN, and the financial analyst, Daniel Heidemann, MBA, in generating the data used in this study. This work was supported in part by a grant from Life Cell.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Margaret A. Plymale, Ranjan Ragulojan, and Dr. Dan Davenport have no conflicts of interest or financial ties to disclose. Dr. Roth is a speaker for Bard, has grants with Bard, Life Cell, Gore, and MTF, and is a consultant for LifeCell.
Rights and permissions
About this article
Cite this article
Plymale, M.A., Ragulojan, R., Davenport, D.L. et al. Ventral and incisional hernia: the cost of comorbidities and complications. Surg Endosc 31, 341–351 (2017). https://doi.org/10.1007/s00464-016-4977-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-4977-8